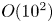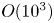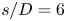175 results
An unhealthful plant-based diet and circulating hsCRP levels are independently associated with lower physical well-being in older adults
-
- Journal:
- Proceedings of the Nutrition Society / Volume 82 / Issue OCE5 / 2023
- Published online by Cambridge University Press:
- 08 January 2024, E355
-
- Article
-
- You have access
- HTML
- Export citation
Features of immunometabolic depression as predictors of antidepressant treatment outcomes: pooled analysis of four clinical trials
-
- Journal:
- The British Journal of Psychiatry / Volume 224 / Issue 3 / March 2024
- Published online by Cambridge University Press:
- 22 December 2023, pp. 89-97
- Print publication:
- March 2024
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Accelerated brain aging as a biomarker for staging in bipolar disorder: an exploratory study
-
- Journal:
- Psychological Medicine / Volume 54 / Issue 5 / April 2024
- Published online by Cambridge University Press:
- 26 September 2023, pp. 1016-1025
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
The MooDFOOD randomized controlled trial: the data and its implications for the theory – Authors’ reply
-
- Journal:
- Psychological Medicine / Volume 53 / Issue 12 / September 2023
- Published online by Cambridge University Press:
- 02 June 2023, pp. 5884-5885
-
- Article
-
- You have access
- HTML
- Export citation
Steady and unsteady coupling in twin weakly underexpanded round jets
-
- Journal:
- Journal of Fluid Mechanics / Volume 964 / 10 June 2023
- Published online by Cambridge University Press:
- 23 May 2023, A2
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Killing day-old chicks? Public opinion regarding potential alternatives
-
- Journal:
- Animal Welfare / Volume 20 / Issue 1 / February 2011
- Published online by Cambridge University Press:
- 01 January 2023, pp. 37-45
-
- Article
- Export citation
The prescriber’s guide to classic MAO inhibitors (phenelzine, tranylcypromine, isocarboxazid) for treatment-resistant depression
-
- Journal:
- CNS Spectrums / Volume 28 / Issue 4 / August 2023
- Published online by Cambridge University Press:
- 15 July 2022, pp. 427-440
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Religious delusions in Dutch older adults in treatment for psychosis: a follow-up study
-
- Journal:
- International Psychogeriatrics / Volume 36 / Issue 1 / January 2024
- Published online by Cambridge University Press:
- 14 March 2022, pp. 51-63
-
- Article
- Export citation
Rising co-payments and continuity of healthcare for Dutch patients with bipolar disorder: retrospective longitudinal cohort study
-
- Journal:
- BJPsych Open / Volume 7 / Issue 5 / September 2021
- Published online by Cambridge University Press:
- 31 August 2021, e155
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
The Montreal Cognitive Assessment (MoCA) with a double threshold: improving the MoCA for triaging patients in need of a neuropsychological assessment.
-
- Journal:
- International Psychogeriatrics / Volume 34 / Issue 6 / June 2022
- Published online by Cambridge University Press:
- 31 August 2021, pp. 571-583
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Intensive home treatment in comparison with care as usual: Cost-utility analysis from a pre-randomized controlled trial in the netherlands
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, pp. S117-S118
-
- Article
-
- You have access
- Open access
- Export citation
Ancient West Mexico in the Mesoamerican Ecumene. EDUARDO WILLIAMS. 2020. Archaeopress Pre-Columbian Archaeology 12. Archaeopress, Summertown, Oxford. xviii + 468 pp. $84.00 (paper), ISBN 978-1-78969-353-9.
-
- Journal:
- Latin American Antiquity / Volume 32 / Issue 3 / September 2021
- Published online by Cambridge University Press:
- 28 July 2021, pp. 667-669
- Print publication:
- September 2021
-
- Article
- Export citation
Effects of dietary interventions on depressive symptom profiles: results from the MooDFOOD depression prevention study
-
- Journal:
- Psychological Medicine / Volume 52 / Issue 15 / November 2022
- Published online by Cambridge University Press:
- 07 April 2021, pp. 3580-3589
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
424 - Using the Montreal cognitive assessment in a memory clinic setting for triaging after initial assessment
-
- Journal:
- International Psychogeriatrics / Volume 32 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 04 November 2020, p. 140
-
- Article
-
- You have access
- Export citation
333 - The advantages of a double threshold MoCA (Montreal Cognitive Assessment) for triaging patients to a memory clinic
-
- Journal:
- International Psychogeriatrics / Volume 32 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 04 November 2020, p. 92
-
- Article
-
- You have access
- Export citation
Using an adoption design to test genetically based differences in risk for child behavior problems in response to home environmental influences
-
- Journal:
- Development and Psychopathology / Volume 33 / Issue 4 / October 2021
- Published online by Cambridge University Press:
- 13 July 2020, pp. 1229-1247
-
- Article
- Export citation
Genetics and Not Shared Environment Explains Familial Resemblance in Adult Metabolomics Data
-
- Journal:
- Twin Research and Human Genetics / Volume 23 / Issue 3 / June 2020
- Published online by Cambridge University Press:
- 08 July 2020, pp. 145-155
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Familial risk for depressive and anxiety disorders: associations with genetic, clinical, and psychosocial vulnerabilities
-
- Journal:
- Psychological Medicine / Volume 52 / Issue 4 / March 2022
- Published online by Cambridge University Press:
- 06 July 2020, pp. 696-706
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Combined impact of ADHD and insomnia symptoms on quality of life, productivity, and health care use in the general population
-
- Journal:
- Psychological Medicine / Volume 52 / Issue 1 / January 2022
- Published online by Cambridge University Press:
- 29 June 2020, pp. 36-47
-
- Article
- Export citation
PW01-200 - Ethnic Differences And Similarities In Treatment Of Common Mental Disorders In Primary And Outpatient Mental Health Care In The Netherlands
-
- Journal:
- European Psychiatry / Volume 25 / Issue S1 / 2010
- Published online by Cambridge University Press:
- 17 April 2020, 25-E1607
-
- Article
-
- You have access
- Export citation