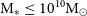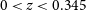352 results
302 Diagnostic Evidence Gauge of Spatial Transcriptomics (DEGAS-ST): Using transfer learning to map clinical data to spatial transcriptomics in prostate cancer
- Part of
-
- Journal:
- Journal of Clinical and Translational Science / Volume 8 / Issue s1 / April 2024
- Published online by Cambridge University Press:
- 03 April 2024, p. 93
-
- Article
-
- You have access
- Open access
- Export citation
370 Point-of-Service Salivary Microbiome Analysis in the Prevention and Detection of Oral Premalignant Lesions
- Part of
-
- Journal:
- Journal of Clinical and Translational Science / Volume 8 / Issue s1 / April 2024
- Published online by Cambridge University Press:
- 03 April 2024, p. 111
-
- Article
-
- You have access
- Open access
- Export citation
Evaluation of indigenous and exotic fodder sorghum accessions for fodder-related traits and host resistance to zonate leaf spot disease
-
- Journal:
- Plant Genetic Resources , First View
- Published online by Cambridge University Press:
- 20 March 2024, pp. 1-8
-
- Article
- Export citation
Annual risk of hepatitis E virus infection and seroreversion: Insights from a serological cohort in Sitakunda, Bangladesh
-
- Journal:
- Epidemiology & Infection / Volume 152 / 2024
- Published online by Cambridge University Press:
- 18 March 2024, e52
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
EMU/GAMA: A technique for detecting active galactic nuclei in low mass systems
-
- Journal:
- Publications of the Astronomical Society of Australia / Volume 41 / 2024
- Published online by Cambridge University Press:
- 21 February 2024, e016
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Jurassic Trigoniida (Bivalvia) from Gebel Maghara, northern Sinai, Egypt
-
- Journal:
- Journal of Paleontology / Volume 97 / Issue 6 / November 2023
- Published online by Cambridge University Press:
- 25 January 2024, pp. 1206-1232
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Somatic multicomorbidity and disability in patients with psychiatric disorders in comparison to the general population: a quasi-epidemiological investigation in 54,826 subjects from 40 countries (COMET-G study)
-
- Journal:
- CNS Spectrums / Volume 29 / Issue 2 / April 2024
- Published online by Cambridge University Press:
- 25 January 2024, pp. 126-149
-
- Article
-
- You have access
- HTML
- Export citation
EMU/GAMA: Radio-detected galaxies are more obscured than optically selected galaxies
-
- Journal:
- Publications of the Astronomical Society of Australia / Volume 41 / 2024
- Published online by Cambridge University Press:
- 17 January 2024, e021
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
72 Dietary Fat and Measures of Attention and Learning in Middle-Aged Adults
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 376-377
-
- Article
-
- You have access
- Export citation
71 Sleep Quality and Measures of Attention and Learning in Middle-Aged Adults
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 580-581
-
- Article
-
- You have access
- Export citation
50 Sex differences in psychological features in adolescents after concussion
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 155-156
-
- Article
-
- You have access
- Export citation
Risk factors associated with overweight and obesity in people with severe mental illness in South Asia: cross-sectional study in Bangladesh, India, and Pakistan
-
- Journal:
- Journal of Nutritional Science / Volume 12 / 2023
- Published online by Cambridge University Press:
- 21 November 2023, e116
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Wake bi-modality: the effect of upstream boundary layer dynamics
-
- Journal:
- Journal of Fluid Mechanics / Volume 975 / 25 November 2023
- Published online by Cambridge University Press:
- 10 November 2023, A7
-
- Article
- Export citation
Revision of Jurassic Protobranch Bivalves from Gebel Maghara, northern Sinai, Egypt
-
- Journal:
- Journal of Paleontology / Volume 97 / Issue S93 / June 2023
- Published online by Cambridge University Press:
- 27 June 2023, pp. 1-45
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
P.098 Antibacterial envelopes prevent post-operative infections in neuromodulation surgery
-
- Journal:
- Canadian Journal of Neurological Sciences / Volume 50 / Issue s2 / June 2023
- Published online by Cambridge University Press:
- 05 June 2023, p. S84
-
- Article
-
- You have access
- Export citation
Versatile tape-drive target for high-repetition-rate laser-driven proton acceleration – CORRIGENDUM
-
- Journal:
- High Power Laser Science and Engineering / Volume 11 / 2023
- Published online by Cambridge University Press:
- 05 June 2023, e43
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Characterisation of infection-induced SARS-CoV-2 seroprevalence amongst children and adolescents in North Carolina
-
- Journal:
- Epidemiology & Infection / Volume 151 / 2023
- Published online by Cambridge University Press:
- 03 April 2023, e63
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Automated control and optimization of laser-driven ion acceleration
- Part of
-
- Journal:
- High Power Laser Science and Engineering / Volume 11 / 2023
- Published online by Cambridge University Press:
- 27 March 2023, e35
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Versatile tape-drive target for high-repetition-rate laser-driven proton acceleration
- Part of
-
- Journal:
- High Power Laser Science and Engineering / Volume 11 / 2023
- Published online by Cambridge University Press:
- 21 March 2023, e23
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Development and genomic characterization of EMS induced mutant population of Zea mays L.
-
- Journal:
- Plant Genetic Resources / Volume 20 / Issue 3 / June 2022
- Published online by Cambridge University Press:
- 28 February 2023, pp. 188-193
-
- Article
- Export citation