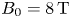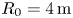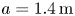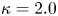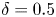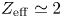82 results
Genomic investigation of multispecies and multivariant blaNDM outbreak reveals key role of horizontal plasmid transmission
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 45 / Issue 6 / June 2024
- Published online by Cambridge University Press:
- 12 February 2024, pp. 709-716
- Print publication:
- June 2024
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Development of compact tokamak fusion reactor use cases to inform future transport studies
- Part of
-
- Journal:
- Journal of Plasma Physics / Volume 89 / Issue 4 / August 2023
- Published online by Cambridge University Press:
- 30 August 2023, 905890418
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
21 - Bangladesh, 1971
- from Part III - The Nation-State System during the Cold War
-
-
- Book:
- The Cambridge World History of Genocide
- Published online:
- 23 June 2023
- Print publication:
- 04 May 2023, pp 497-517
-
- Chapter
- Export citation
Current Evidence for Infection Prevention and Control Interventions in Emergency Medical Services: A Scoping Review
-
- Journal:
- Prehospital and Disaster Medicine / Volume 38 / Issue 3 / June 2023
- Published online by Cambridge University Press:
- 29 March 2023, pp. 371-377
- Print publication:
- June 2023
-
- Article
- Export citation
Expanding mental health services in low- and middle-income countries: A task-shifting framework for delivery of comprehensive, collaborative, and community-based care
-
- Journal:
- Cambridge Prisms: Global Mental Health / Volume 10 / 2023
- Published online by Cambridge University Press:
- 27 February 2023, e16
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Introduction and overview
-
- Journal:
- Animal Welfare / Volume 22 / Issue 1 / February 2013
- Published online by Cambridge University Press:
- 01 January 2023, p. 107
-
- Article
- Export citation
Cost-effectiveness of psychological intervention within services for depression delivered by primary care workers in Nepal: economic evaluation of a randomized control trial
-
- Journal:
- Global Mental Health / Volume 9 / 2022
- Published online by Cambridge University Press:
- 31 October 2022, pp. 499-507
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
A latent class approach to understanding patterns of emotional and behavioral problems among early adolescents across four low- and middle-income countries
-
- Journal:
- Development and Psychopathology / Volume 35 / Issue 4 / October 2023
- Published online by Cambridge University Press:
- 30 May 2022, pp. 1684-1700
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Characterisation of age and polarity at onset in bipolar disorder
-
- Journal:
- The British Journal of Psychiatry / Volume 219 / Issue 6 / December 2021
- Published online by Cambridge University Press:
- 25 August 2021, pp. 659-669
- Print publication:
- December 2021
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Diagnosis and prevalence of two new species of haplosporidians infecting shore crabs Carcinus maenas: Haplosporidium carcini n. sp., and H. cranc n. sp.
-
- Journal:
- Parasitology / Volume 147 / Issue 11 / September 2020
- Published online by Cambridge University Press:
- 16 June 2020, pp. 1229-1237
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
When less is more: reducing redundancy in mental health and psychosocial instruments using Item Response Theory
-
- Journal:
- Global Mental Health / Volume 7 / 2020
- Published online by Cambridge University Press:
- 09 January 2020, e3
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Encompassing a global mental health perspective into psychotherapy research: a critique of approaches to measuring the efficacy of psychotherapy for depression
-
- Journal:
- Epidemiology and Psychiatric Sciences / Volume 28 / Issue 3 / June 2019
- Published online by Cambridge University Press:
- 15 January 2019, pp. 275-277
-
- Article
- Export citation
Mental Health and Psychosocial Problems and Needs of Violence Survivors in the Colombian Pacific Coast: A Qualitative Study in Buenaventura and Quibdó
-
- Journal:
- Prehospital and Disaster Medicine / Volume 33 / Issue 6 / December 2018
- Published online by Cambridge University Press:
- 26 July 2018, pp. 567-574
- Print publication:
- December 2018
-
- Article
- Export citation
P.027 Efficacy of a fourth alemtuzumab course in RRMS patients from CARE-MS II who experienced disease activity after three prior courses
-
- Journal:
- Canadian Journal of Neurological Sciences / Volume 45 / Issue s2 / June 2018
- Published online by Cambridge University Press:
- 27 June 2018, p. S23
-
- Article
-
- You have access
- Export citation
Marteilia refringens and Marteilia pararefringens sp. nov. are distinct parasites of bivalves and have different European distributions
-
- Journal:
- Parasitology / Volume 145 / Issue 11 / September 2018
- Published online by Cambridge University Press:
- 11 June 2018, pp. 1483-1492
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
An evaluation of a common elements treatment approach for youth in Somali refugee camps
-
- Journal:
- Global Mental Health / Volume 5 / 2018
- Published online by Cambridge University Press:
- 25 April 2018, e16
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Development and cross-cultural testing of the International Depression Symptom Scale (IDSS): a measurement instrument designed to represent global presentations of depression
-
- Journal:
- Global Mental Health / Volume 4 / 2017
- Published online by Cambridge University Press:
- 11 September 2017, e17
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
An ecological model for refugee mental health: implications for research
-
- Journal:
- Epidemiology and Psychiatric Sciences / Volume 26 / Issue 2 / April 2017
- Published online by Cambridge University Press:
- 19 September 2016, pp. 139-141
-
- Article
- Export citation
Local perceptions of the impact of group interpersonal psychotherapy in rural Uganda
-
- Journal:
- Global Mental Health / Volume 3 / 2016
- Published online by Cambridge University Press:
- 27 July 2016, e23
-
- Article
-
- You have access
- Open access
- HTML
- Export citation