23 results
Impact of discontinuation of contact precautions on surveillance- and whole genome sequencing-defined methicillin-resistant Staphylococcus aureus healthcare-associated infections
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue 1 / 2024
- Published online by Cambridge University Press:
- 04 June 2024, e97
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
P.023 Review of imaging changes, cognitive decline, and dementia risk in cancer survivors after chemotherapy
-
- Journal:
- Canadian Journal of Neurological Sciences / Volume 51 / Issue s1 / June 2024
- Published online by Cambridge University Press:
- 24 May 2024, p. S21
-
- Article
-
- You have access
- Export citation
Incidence and transmission associated with respiratory viruses in an acute care facility: An observational study
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 45 / Issue 6 / June 2024
- Published online by Cambridge University Press:
- 14 February 2024, pp. 774-776
- Print publication:
- June 2024
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Prolonged bacterial carriage and hospital transmission detected by whole genome sequencing surveillance
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue 1 / 2024
- Published online by Cambridge University Press:
- 30 January 2024, e11
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
The utility of whole-genome sequencing to inform epidemiologic investigations of SARS-CoV-2 clusters in acute-care hospitals
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 45 / Issue 2 / February 2024
- Published online by Cambridge University Press:
- 22 December 2023, pp. 144-149
- Print publication:
- February 2024
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Environmental contamination of postmortem blood cultures detected by whole-genome sequencing surveillance
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 12 / December 2023
- Published online by Cambridge University Press:
- 24 August 2023, pp. 2103-2105
- Print publication:
- December 2023
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Sensitivity of National Healthcare Safety Network definitions to capture healthcare-associated transmission identified by whole-genome sequencing surveillance
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 10 / October 2023
- Published online by Cambridge University Press:
- 28 March 2023, pp. 1663-1665
- Print publication:
- October 2023
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Whole-genome sequencing surveillance and machine learning for healthcare outbreak detection and investigation: A systematic review and summary
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue 1 / 2022
- Published online by Cambridge University Press:
- 13 June 2022, e91
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
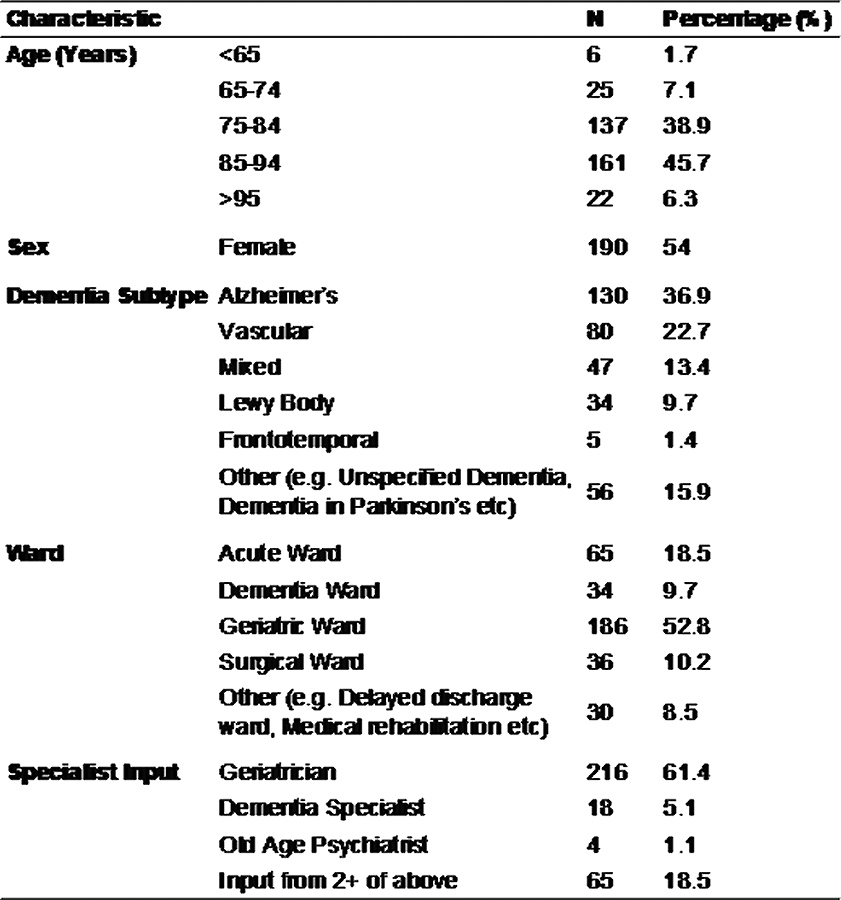
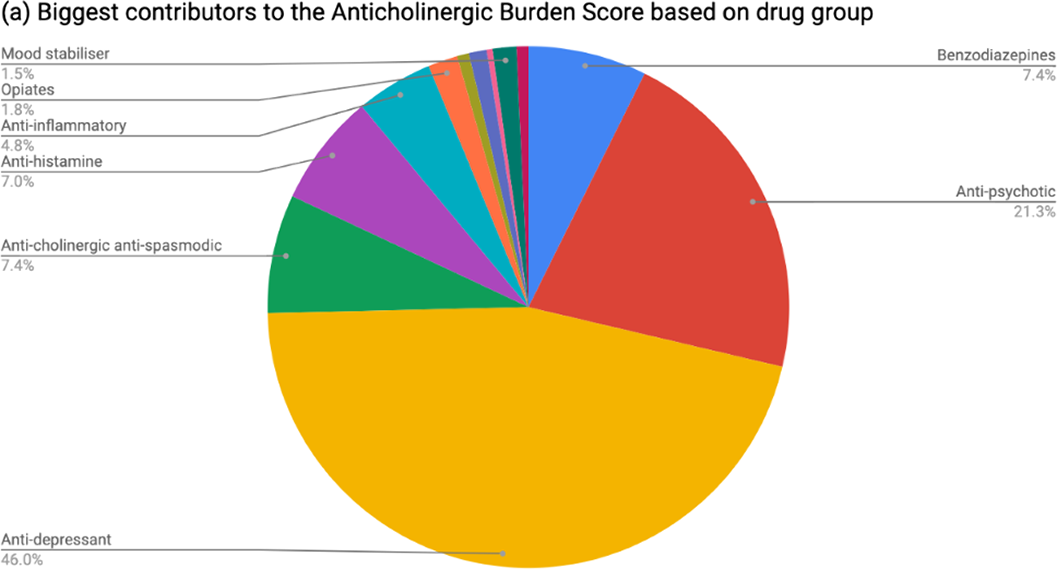
Dementia patients have greater anti-cholinergic drug burden on discharge from hospital: A multicentre cross-sectional study
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, pp. S422-S423
-
- Article
-
- You have access
- Open access
- Export citation
Automated data mining of the electronic health record for investigation of healthcare-associated outbreaks
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 40 / Issue 3 / March 2019
- Published online by Cambridge University Press:
- 18 February 2019, pp. 314-319
- Print publication:
- March 2019
-
- Article
- Export citation
Bronchoscope-associated clusters of multidrug-resistant Pseudomonas aeruginosa and carbapenem-resistant Klebsiella pneumoniae
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 40 / Issue 1 / January 2019
- Published online by Cambridge University Press:
- 19 November 2018, pp. 40-46
- Print publication:
- January 2019
-
- Article
- Export citation
Completeness of Methicillin-Resistant Staphylococcus aureus Bloodstream Infection Reporting From Outpatient Hemodialysis Facilities to the National Healthcare Safety Network, 2013
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 37 / Issue 2 / February 2016
- Published online by Cambridge University Press:
- 11 November 2015, pp. 205-207
- Print publication:
- February 2016
-
- Article
- Export citation
Notes on contributors
-
-
- Book:
- The Cambridge Companion to Latin Love Elegy
- Published online:
- 18 December 2013
- Print publication:
- 21 November 2013, pp viii-xii
-
- Chapter
- Export citation
Contributors
-
-
- Book:
- Maternal Critical Care
- Published online:
- 05 July 2013
- Print publication:
- 04 July 2013, pp ix-xiv
-
- Chapter
- Export citation
Natural History of Multidrug-Resistant Acinetobacter baumannii Carriage in Intensive Care Units
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 33 / Issue 6 / June 2012
- Published online by Cambridge University Press:
- 02 January 2015, pp. 642-643
- Print publication:
- June 2012
-
- Article
- Export citation
Patient-Associated Risk Factors for Acquisition of Methicillin-Resistant Staphylococcus aureus in a Tertiary Care Hospital
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 31 / Issue 11 / November 2010
- Published online by Cambridge University Press:
- 02 January 2015, pp. 1139-1147
- Print publication:
- November 2010
-
- Article
- Export citation
Economic Impact of Acinetobacter baumannii Infection in the Intensive Care Unit
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 31 / Issue 10 / October 2010
- Published online by Cambridge University Press:
- 02 January 2015, pp. 1087-1089
- Print publication:
- October 2010
-
- Article
- Export citation
Universal Methicillin-Resistant Staphylococcus aureus (MRSA) Surveillance for Adults at Hospital Admission: An Economic Model and Analysis
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 31 / Issue 6 / June 2010
- Published online by Cambridge University Press:
- 02 January 2015, pp. 598-606
- Print publication:
- June 2010
-
- Article
- Export citation
Should Vascular Surgery Patients Be Screened Preoperatively for Methicillin-Resistant Staphylococcus aureus?
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 30 / Issue 12 / December 2009
- Published online by Cambridge University Press:
- 02 January 2015, pp. 1158-1165
- Print publication:
- December 2009
-
- Article
- Export citation
Trends in stimulated Brillouin scattering and optical phase conjugation
-
- Journal:
- Laser and Particle Beams / Volume 26 / Issue 3 / September 2008
- Published online by Cambridge University Press:
- 09 June 2008, pp. 297-362
-
- Article
- Export citation