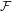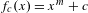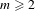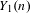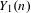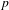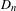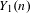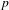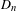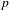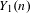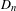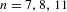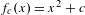350 results
Passive acoustic monitoring detects new records of globally threatened birds in a high elevation wetland (Free State, South Africa) – CORRIGENDUM
-
- Journal:
- Bird Conservation International / Volume 34 / 2024
- Published online by Cambridge University Press:
- 02 February 2024, e8
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
12 - Cornelia-Uitzoek: Paleoecology, Archeology, and Geochronology
- from Part II - Southern Africa
-
-
- Book:
- African Paleoecology and Human Evolution
- Published online:
- 19 May 2022
- Print publication:
- 09 June 2022, pp 120-134
-
- Chapter
- Export citation
The effect of the COVID-19 pandemic on mental health in individuals with pre-existing mental illness
-
- Journal:
- BJPsych Open / Volume 8 / Issue 2 / March 2022
- Published online by Cambridge University Press:
- 07 March 2022, e59
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Reductions in vancomycin and meropenem following the implementation of a febrile neutropenia management algorithm in hospitalized adults: An interrupted time series analysis
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 42 / Issue 9 / September 2021
- Published online by Cambridge University Press:
- 25 January 2021, pp. 1090-1097
- Print publication:
- September 2021
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Accuracy of dopaminergic imaging as a biomarker for mild cognitive impairment with Lewy bodies
-
- Journal:
- The British Journal of Psychiatry / Volume 218 / Issue 5 / May 2021
- Published online by Cambridge University Press:
- 23 December 2020, pp. 276-282
- Print publication:
- May 2021
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Impact of schizophrenia genetic liability on the association between schizophrenia and physical illness: data-linkage study
-
- Journal:
- BJPsych Open / Volume 6 / Issue 6 / November 2020
- Published online by Cambridge University Press:
- 10 November 2020, e139
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Mild cognitive impairment with Lewy bodies: neuropsychiatric supportive symptoms and cognitive profile
-
- Journal:
- Psychological Medicine / Volume 52 / Issue 6 / April 2022
- Published online by Cambridge University Press:
- 25 August 2020, pp. 1147-1155
-
- Article
- Export citation
Contacts with primary and secondary healthcare prior to suicide: case–control whole-population-based study using person-level linked routine data in Wales, UK, 2000–2017
-
- Journal:
- The British Journal of Psychiatry / Volume 217 / Issue 6 / December 2020
- Published online by Cambridge University Press:
- 03 August 2020, pp. 717-724
- Print publication:
- December 2020
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Developing community-based urine sampling methods to deploy biomarker technology for the assessment of dietary exposure
-
- Journal:
- Public Health Nutrition / Volume 23 / Issue 17 / December 2020
- Published online by Cambridge University Press:
- 11 June 2020, pp. 3081-3092
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Understanding the use and impact of allied health services for people with chronic health conditions in Central and Eastern Sydney, Australia: a five-year longitudinal analysis
-
- Journal:
- Primary Health Care Research & Development / Volume 20 / 2019
- Published online by Cambridge University Press:
- 23 October 2019, e141
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
2111: Insulin resistance patterns over 25-years of adulthood and nonalcoholic fatty liver disease in middle age: The Coronary Artery Risk Development in Young Adults (CARDIA) Study
-
- Journal:
- Journal of Clinical and Translational Science / Volume 1 / Issue S1 / September 2017
- Published online by Cambridge University Press:
- 10 May 2018, pp. 23-24
-
- Article
-
- You have access
- Open access
- Export citation
Diagnostic accuracy of dopaminergic imaging in prodromal dementia with Lewy bodies
-
- Journal:
- Psychological Medicine / Volume 49 / Issue 3 / February 2019
- Published online by Cambridge University Press:
- 25 April 2018, pp. 396-402
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Neuroticism and suicide in a general population cohort: results from the UK Biobank Project
- Part of
-
- Journal:
- BJPsych Open / Volume 4 / Issue 2 / March 2018
- Published online by Cambridge University Press:
- 16 March 2018, pp. 62-68
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Reduction of dynatomic curves
-
- Journal:
- Ergodic Theory and Dynamical Systems / Volume 39 / Issue 10 / October 2019
- Published online by Cambridge University Press:
- 25 January 2018, pp. 2717-2768
- Print publication:
- October 2019
-
- Article
- Export citation
Neuropsychiatric symptoms and cognitive profile in mild cognitive impairment with Lewy bodies
-
- Journal:
- Psychological Medicine / Volume 48 / Issue 14 / October 2018
- Published online by Cambridge University Press:
- 24 January 2018, pp. 2384-2390
-
- Article
- Export citation
6.6 (34) - On Numbers
- from 6.6 (34) - On Numbers
-
- Book:
- Plotinus: The <I>Enneads</I>
- Published online:
- 16 December 2017
- Print publication:
- 28 December 2017, pp 775-797
-
- Chapter
- Export citation
3.6 (26) - On the Impassibility of Things without Bodies
- from 3.6 (26) - On the Impassibility of Things without Bodies
-
- Book:
- Plotinus: The <I>Enneads</I>
- Published online:
- 16 December 2017
- Print publication:
- 28 December 2017, pp 307-331
-
- Chapter
- Export citation
2.8 (35) - On Seeing, or On How It Is That Distant Things Appear Small
- from 2.8 (35) - On Seeing, or On How It Is That Distant Things Appear Small1
-
- Book:
- Plotinus: The <I>Enneads</I>
- Published online:
- 16 December 2017
- Print publication:
- 28 December 2017, pp 203-205
-
- Chapter
- Export citation
2.2 (14) - On the Motion of Heaven1
- from 2.2 (14) - On the Motion of Heaven
-
- Book:
- Plotinus: The <I>Enneads</I>
- Published online:
- 16 December 2017
- Print publication:
- 28 December 2017, pp 141-144
-
- Chapter
- Export citation
4.7 (2) - On the Immortality of the Soul
- from Ennead Four
-
- Book:
- Plotinus: The <I>Enneads</I>
- Published online:
- 16 December 2017
- Print publication:
- 28 December 2017, pp 487-509
-
- Chapter
- Export citation