59 results
Features of immunometabolic depression as predictors of antidepressant treatment outcomes: pooled analysis of four clinical trials
-
- Journal:
- The British Journal of Psychiatry / Volume 224 / Issue 3 / March 2024
- Published online by Cambridge University Press:
- 22 December 2023, pp. 89-97
- Print publication:
- March 2024
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
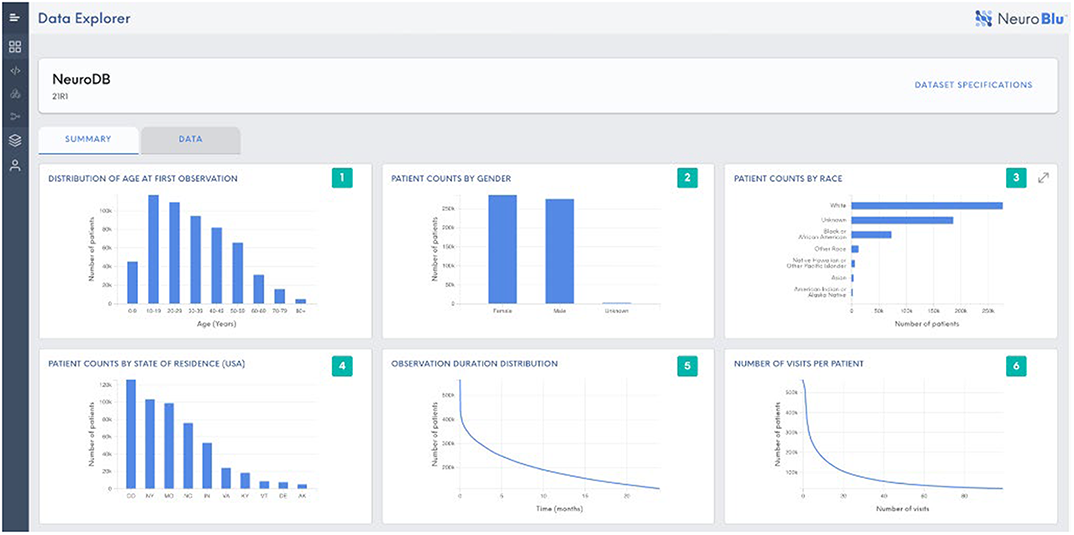
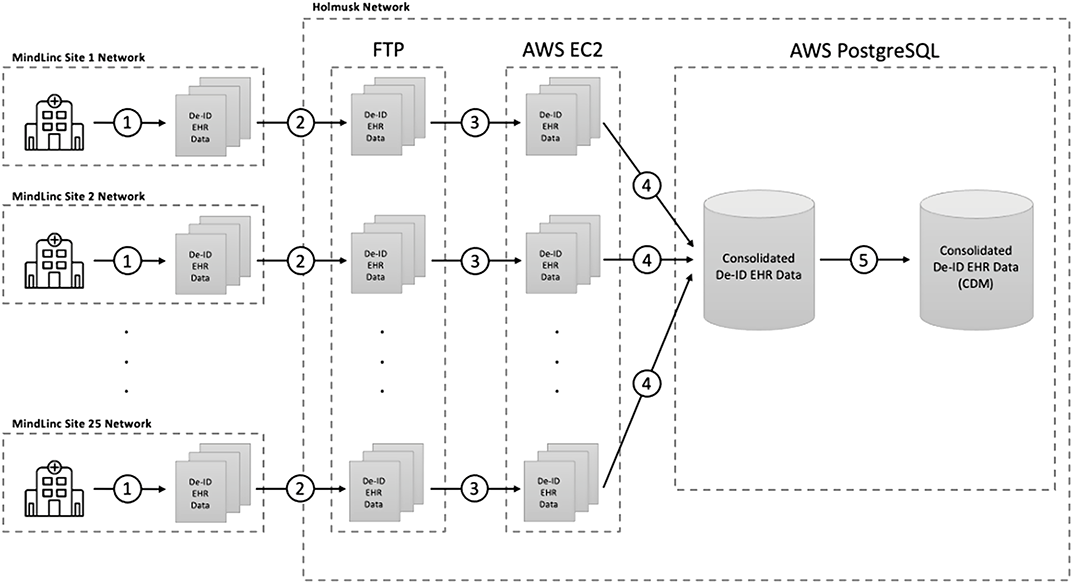
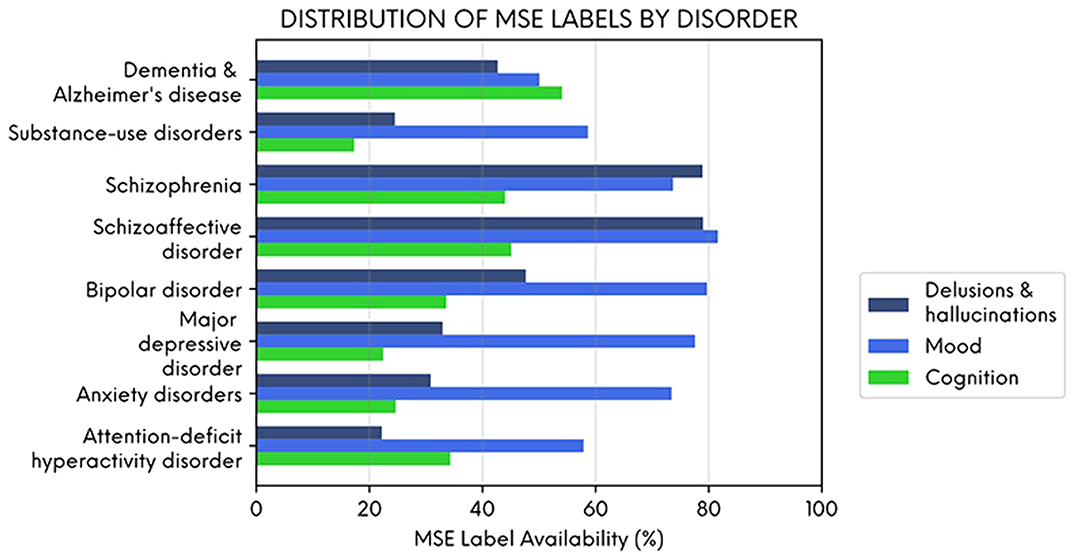
NeuroBlu: a natural language processing (NLP) electronic health record (EHR) data analytic tool to generate real-world evidence in mental healthcare
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S99-S100
-
- Article
-
- You have access
- Open access
- Export citation
The Qualitative Transparency Deliberations: Insights and Implications
-
- Journal:
- Perspectives on Politics / Volume 19 / Issue 1 / March 2021
- Published online by Cambridge University Press:
- 06 January 2021, pp. 171-208
- Print publication:
- March 2021
-
- Article
- Export citation
The role of the social vulnerability index in personal protective equipment shortages, number of cases, and associated mortality during the coronavirus disease 2019 (COVID-19) pandemic in Michigan skilled nursing facilities
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 42 / Issue 7 / July 2021
- Published online by Cambridge University Press:
- 13 November 2020, pp. 877-880
- Print publication:
- July 2021
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
P-479 - Visual Contrast Sensitivity in Depression
-
- Journal:
- European Psychiatry / Volume 27 / Issue S1 / 2012
- Published online by Cambridge University Press:
- 15 April 2020, p. 1
-
- Article
-
- You have access
- Export citation
Utility of published skinfold thickness equations for prediction of body composition in very young New Zealand children
-
- Journal:
- British Journal of Nutrition / Volume 124 / Issue 3 / 14 August 2020
- Published online by Cambridge University Press:
- 06 April 2020, pp. 349-360
- Print publication:
- 14 August 2020
-
- Article
-
- You have access
- HTML
- Export citation
Review: innovation through research in the North American pork industry
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Lack of Prognostic Significance of SPECT Abnormalities in Non-demented Elderly Subjects with Memory Loss
-
- Journal:
- Canadian Journal of Neurological Sciences / Volume 26 / Issue 1 / February 1999
- Published online by Cambridge University Press:
- 05 August 2019, pp. 23-28
-
- Article
-
- You have access
- Export citation
Delivery of the research participant perception survey through the patient portal
-
- Journal:
- Journal of Clinical and Translational Science / Volume 2 / Issue 3 / June 2018
- Published online by Cambridge University Press:
- 21 September 2018, pp. 163-168
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Improving Long-Term Care Facility Disaster Preparedness and Response: A Literature Review
-
- Journal:
- Disaster Medicine and Public Health Preparedness / Volume 11 / Issue 1 / February 2017
- Published online by Cambridge University Press:
- 11 August 2016, pp. 140-149
-
- Article
-
- You have access
- HTML
- Export citation
Rethinking funding priorities in mental health research
-
- Journal:
- The British Journal of Psychiatry / Volume 208 / Issue 6 / June 2016
- Published online by Cambridge University Press:
- 02 January 2018, pp. 507-509
- Print publication:
- June 2016
-
- Article
-
- You have access
- HTML
- Export citation
Management of hypoplastic left heart syndrome with intact atrial septum: a two-centre experience
-
- Journal:
- Cardiology in the Young / Volume 26 / Issue 6 / August 2016
- Published online by Cambridge University Press:
- 08 September 2015, pp. 1072-1081
-
- Article
- Export citation
Human anthrax outbreak associated with livestock exposure: Georgia, 2012
-
- Journal:
- Epidemiology & Infection / Volume 144 / Issue 1 / January 2016
- Published online by Cambridge University Press:
- 19 June 2015, pp. 76-87
-
- Article
-
- You have access
- HTML
- Export citation
Does early-onset chronic or recurrent major depression impact outcomes with antidepressant medications? A CO-MED Trial Report
-
- Journal:
- Psychological Medicine / Volume 43 / Issue 5 / May 2013
- Published online by Cambridge University Press:
- 11 December 2012, pp. 945-960
-
- Article
- Export citation
(Z)-11-HEXADECEN-1-OL: A BEHAVIORAL MODIFYING CHEMICAL PRESENT IN THE PHEROMONE GLAND OF FEMALE HELIOTHIS ZEA (LEPIDOPTERA: NOCTUIDAE)
-
- Journal:
- The Canadian Entomologist / Volume 116 / Issue 5 / May 1984
- Published online by Cambridge University Press:
- 31 May 2012, pp. 777-779
-
- Article
- Export citation
Is prior course of illness relevant to acute or longer-term outcomes in depressed out-patients? A STAR*D report
-
- Journal:
- Psychological Medicine / Volume 42 / Issue 6 / June 2012
- Published online by Cambridge University Press:
- 19 October 2011, pp. 1131-1149
-
- Article
- Export citation
A practical approach to the early identification of antidepressant medication non-responders
-
- Journal:
- Psychological Medicine / Volume 42 / Issue 2 / February 2012
- Published online by Cambridge University Press:
- 25 July 2011, pp. 309-316
-
- Article
- Export citation
Contributors
-
-
- Book:
- Intracerebral Hemorrhage
- Published online:
- 04 May 2010
- Print publication:
- 12 November 2009, pp ix-xi
-
- Chapter
- Export citation
Anticipated Benefits of Care (ABC): psychometrics and predictive value in psychiatric disorders
-
- Journal:
- Psychological Medicine / Volume 40 / Issue 6 / June 2010
- Published online by Cambridge University Press:
- 29 September 2009, pp. 955-965
-
- Article
- Export citation
Impact of persistent substance misuse on 1-year outcome in first-episode psychosis
-
- Journal:
- The British Journal of Psychiatry / Volume 195 / Issue 3 / September 2009
- Published online by Cambridge University Press:
- 02 January 2018, pp. 242-248
- Print publication:
- September 2009
-
- Article
-
- You have access
- HTML
- Export citation