88 results
The equitable impact of sugary drink taxation structures on sugary drink consumption among Canadians: a modelling study using the 2015 Canadian Community Health Survey-Nutrition
-
- Journal:
- Public Health Nutrition / Accepted manuscript
- Published online by Cambridge University Press:
- 15 April 2024, pp. 1-27
-
- Article
-
- You have access
- Open access
- Export citation
Comparative epidemiology of hospital-onset bloodstream infections (HOBSIs) and central line-associated bloodstream infections (CLABSIs) across a three-hospital health system
-
- Journal:
- Infection Control & Hospital Epidemiology , First View
- Published online by Cambridge University Press:
- 20 March 2024, pp. 1-7
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Identification of carbapenem-resistant organism (CRO) contamination of in-room sinks in intensive care units in a new hospital bed tower
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 45 / Issue 3 / March 2024
- Published online by Cambridge University Press:
- 19 January 2024, pp. 302-309
- Print publication:
- March 2024
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
4 Initial Application of Constraint-Induced Cognitive Therapy to Long COVID Brain Fog
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 598-599
-
- Article
-
- You have access
- Export citation
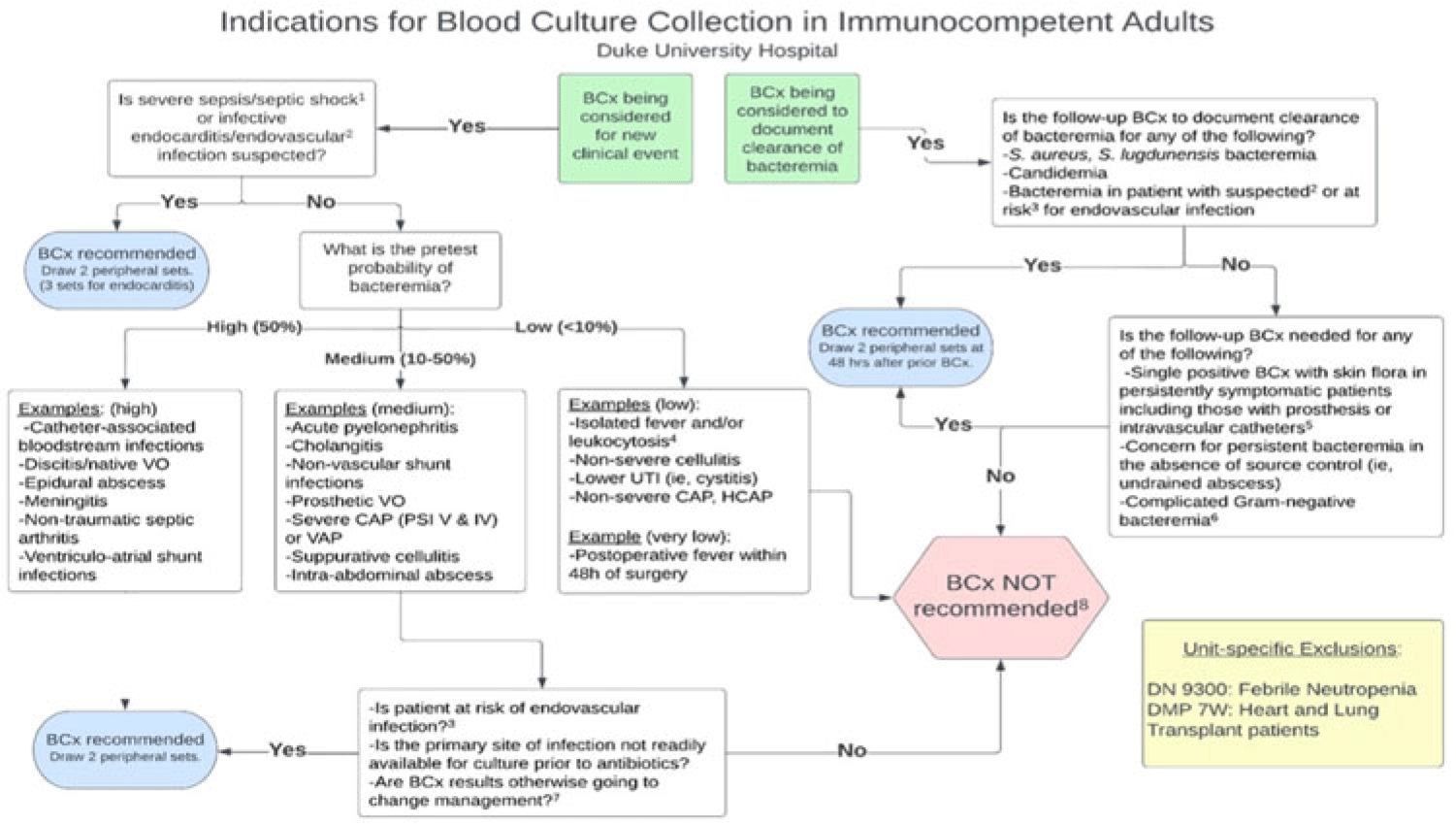
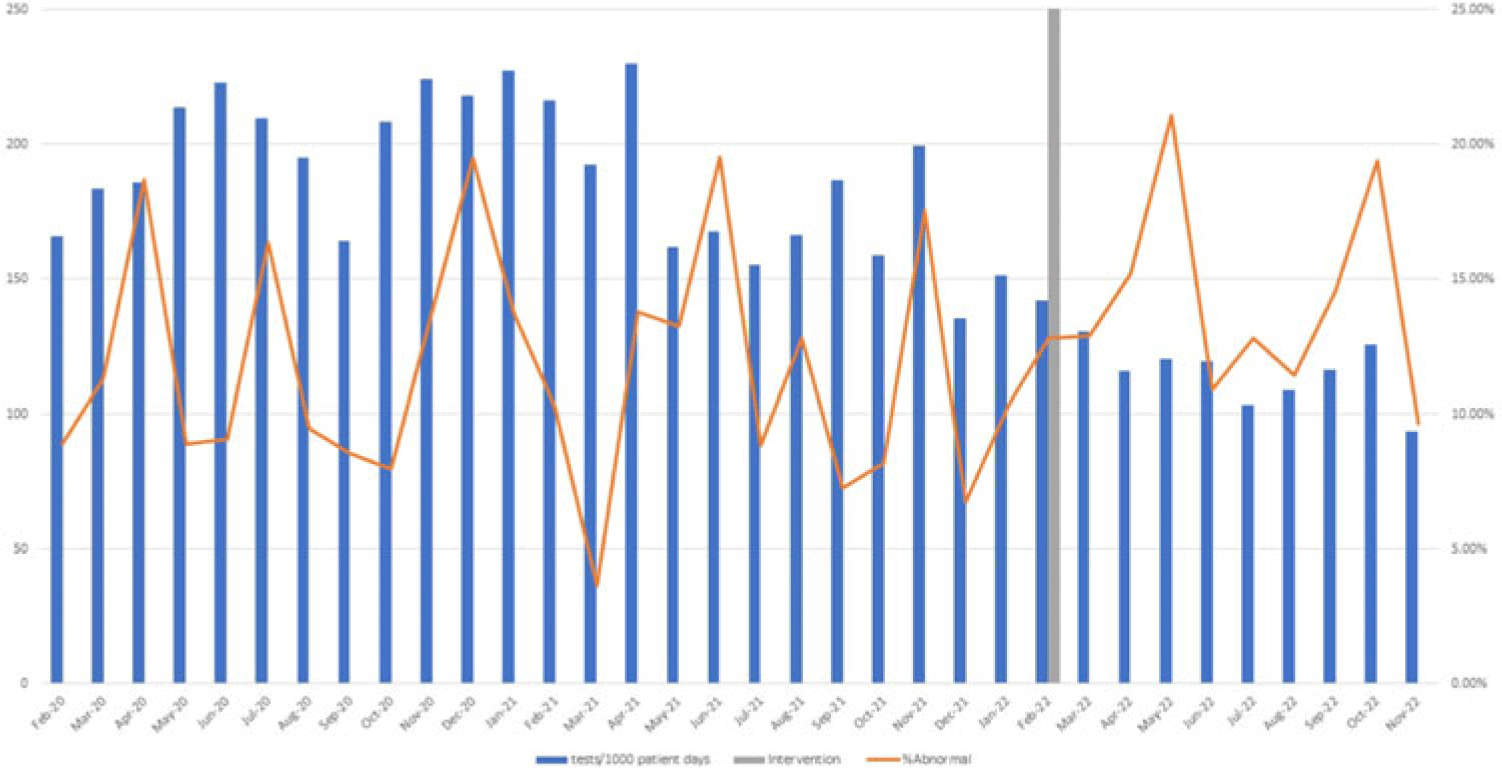
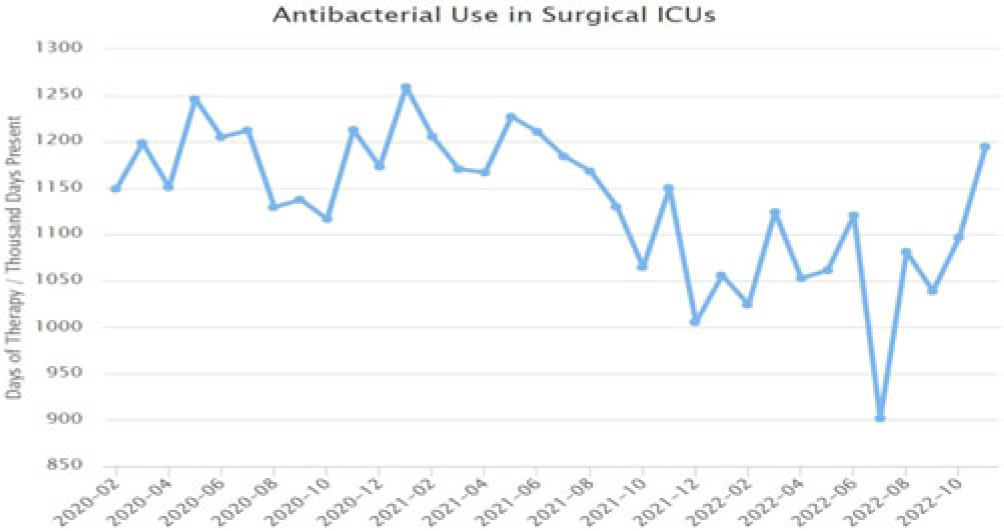
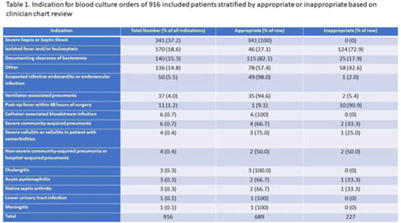
Implementation of a diagnostic stewardship intervention to improve blood-culture utilization in 2 surgical ICUs: Time for a blood-culture change
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 45 / Issue 4 / April 2024
- Published online by Cambridge University Press:
- 11 December 2023, pp. 452-458
- Print publication:
- April 2024
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Implementation of diagnostic stewardship in two surgical ICUs: Time for a blood-culture change
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s9-s10
-
- Article
-
- You have access
- Open access
- Export citation
Epidemiology of carbapenem-resistant and extended-spectrum beta-lactamase-producing Enterobacterales in US children, 2016–2020
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, p. s16
-
- Article
-
- You have access
- Open access
- Export citation
Investigation of the first cluster of Candida auris cases among pediatric patients in the United States―Nevada, May 2022
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s118-s119
-
- Article
-
- You have access
- Open access
- Export citation
Strategies to build a positive and inclusive Antarctic field work environment
-
- Journal:
- Annals of Glaciology / Volume 63 / Issue 87-89 / September 2022
- Published online by Cambridge University Press:
- 11 July 2023, pp. 125-131
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
The Social Determinants of Loneliness During COVID-19: Personal, Community, and Societal Predictors and Implications for Treatment – CORRIGENDUM
-
- Journal:
- Behaviour Change / Volume 40 / Issue 3 / September 2023
- Published online by Cambridge University Press:
- 02 June 2023, p. 251
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
A Case Study of Academic Facilitation of the Global Illicit Trade in Cultural Objects: Mary Slusser in Nepal
-
- Journal:
- International Journal of Cultural Property / Volume 30 / Issue 1 / February 2023
- Published online by Cambridge University Press:
- 12 May 2023, pp. 22-41
-
- Article
- Export citation
A New Model for Postgraduate and Continuing Education in Disaster and Terror Medicine
-
- Journal:
- Prehospital and Disaster Medicine / Volume 38 / Issue S1 / May 2023
- Published online by Cambridge University Press:
- 13 July 2023, p. s181
- Print publication:
- May 2023
-
- Article
-
- You have access
- Export citation
Disparities in central line-associated bloodstream infection and catheter-associated urinary tract infection rates: An exploratory analysis
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 11 / November 2023
- Published online by Cambridge University Press:
- 14 April 2023, pp. 1857-1860
- Print publication:
- November 2023
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
The Social Determinants of Loneliness During COVID-19: Personal, Community, and Societal Predictors and Implications for Treatment
-
- Journal:
- Behaviour Change / Volume 40 / Issue 1 / April 2023
- Published online by Cambridge University Press:
- 14 April 2023, pp. 1-10
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Developmental care pathway for hospitalised infants with CHD: on behalf of the Cardiac Newborn Neuroprotective Network, a Special Interest Group of the Cardiac Neurodevelopmental Outcome Collaborative
-
- Journal:
- Cardiology in the Young / Volume 33 / Issue 12 / December 2023
- Published online by Cambridge University Press:
- 30 March 2023, pp. 2521-2538
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Closing the Wearable Gap: Foot–ankle kinematic modeling via deep learning models based on a smart sock wearable
-
- Journal:
- Wearable Technologies / Volume 4 / 2023
- Published online by Cambridge University Press:
- 20 February 2023, e4
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Reducing burden and building goodwill for practice-embedded trials: Results of rapid qualitative methods in the preimplementation phase of a community paramedic trial to reduce hospitalizations
-
- Journal:
- Journal of Clinical and Translational Science / Volume 7 / Issue 1 / 2023
- Published online by Cambridge University Press:
- 08 February 2023, e61
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Open innovation: the key to advancing brain health
-
- Journal:
- CNS Spectrums / Volume 28 / Issue 4 / August 2023
- Published online by Cambridge University Press:
- 29 July 2022, pp. 392-394
-
- Article
-
- You have access
- HTML
- Export citation
Impacts of drought intensity and weed competition on drought-tolerant corn performance
-
- Journal:
- Weed Science / Volume 70 / Issue 4 / July 2022
- Published online by Cambridge University Press:
- 17 June 2022, pp. 455-462
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
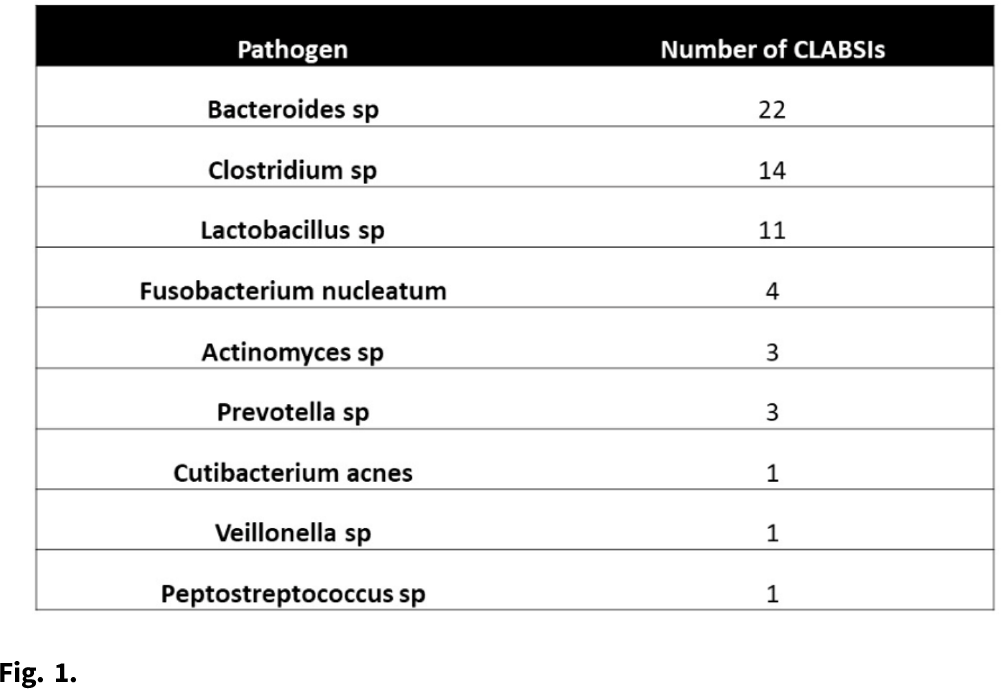
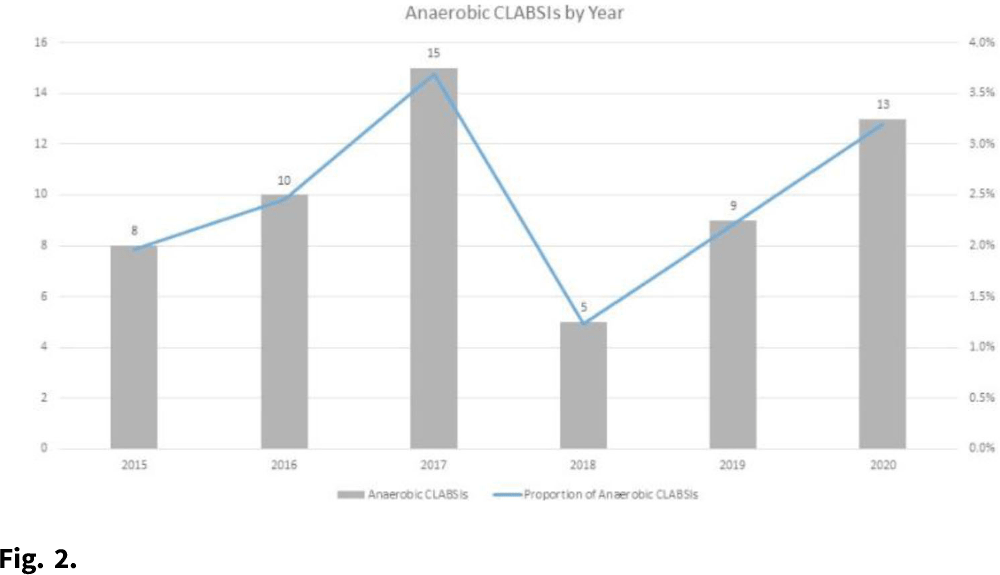
Central-line associated bloodstream infections secondary to strict anaerobes: Time for A definition change?
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, pp. s73-s74
-
- Article
-
- You have access
- Open access
- Export citation