136 results
P.104 Prognostic value of NIRS regional oxygen saturation based cerebrovascular reactivity in TBI: a Canadian high resolution traumatic brain injury (CAHR-TBI) cohort study
-
- Journal:
- Canadian Journal of Neurological Sciences / Volume 51 / Issue s1 / June 2024
- Published online by Cambridge University Press:
- 24 May 2024, p. S44
-
- Article
-
- You have access
- Export citation
4 Evaluating Plasma GFAP for the Detection of Alzheimer’s Disease Dementia
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 408-409
-
- Article
-
- You have access
- Export citation
6 Association Between American Football Play and Parkinson's Disease: Analysis of the Fox Insight Data Set
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 415-416
-
- Article
-
- You have access
- Export citation
64 Neuroimaging Evidence of Neurodegenerative Disease in Former Professional American Football Players Who “Fail” Validity Testing: A Case Series
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 574-575
-
- Article
-
- You have access
- Export citation
5 Antemortem Plasma GFAP Predicts Alzheimer’s Disease Neuropathological Changes
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 409-410
-
- Article
-
- You have access
- Export citation
Participation in the Georgia Food for Health programme and CVD risk factors: a longitudinal observational study
-
- Journal:
- Public Health Nutrition / Volume 26 / Issue 11 / November 2023
- Published online by Cambridge University Press:
- 07 August 2023, pp. 2470-2479
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
The use of a Subjective wellbeing scale as predictor of adherence to neuroleptic treatment to determine poor prognostic factor in African population with Schizophrenia
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S156
-
- Article
-
- You have access
- Open access
- Export citation
Random variation drives a critical bias in the comparison of healthcare-associated infections
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 9 / September 2023
- Published online by Cambridge University Press:
- 10 March 2023, pp. 1396-1402
- Print publication:
- September 2023
-
- Article
- Export citation
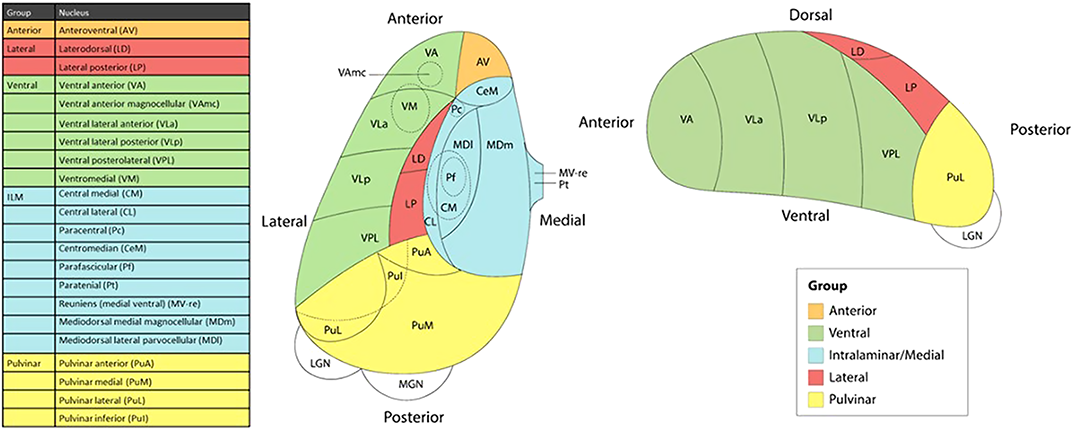
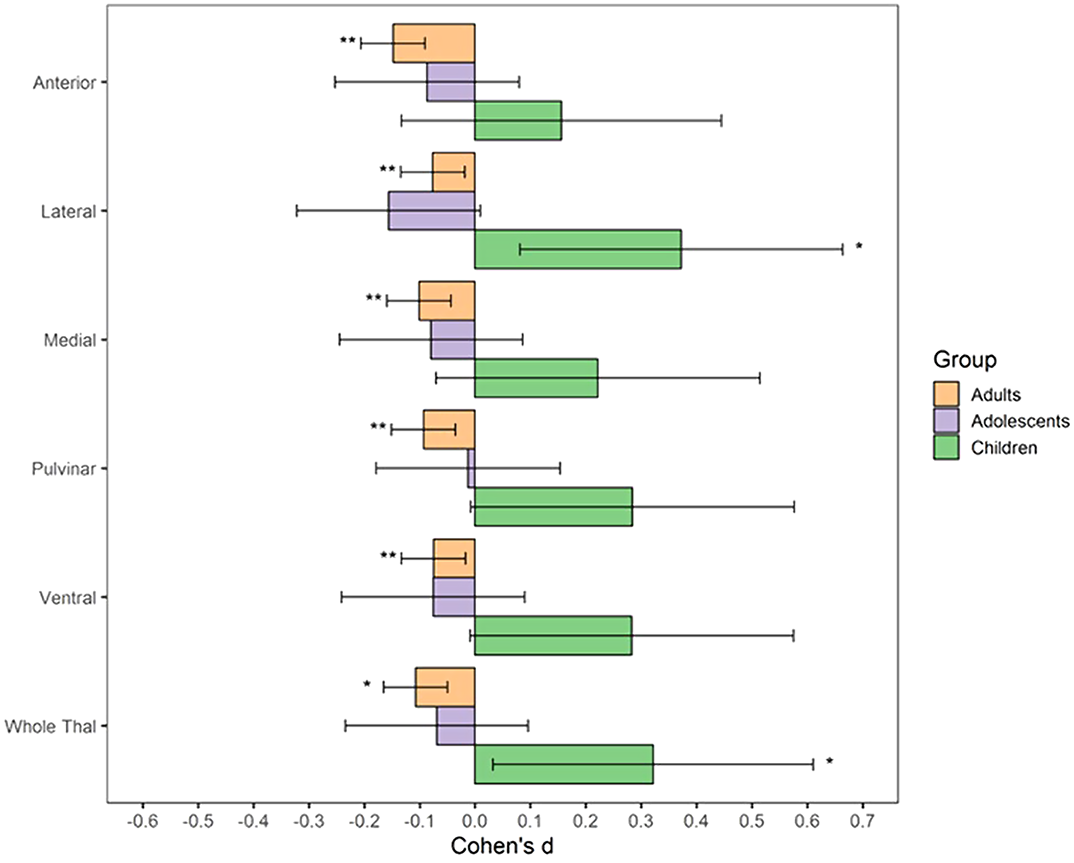
The thalamus and its subregions – a gateway to obsessive-compulsive disorder
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S77-S78
-
- Article
-
- You have access
- Open access
- Export citation
Risk of bacterial bloodstream infection does not vary by central-line type during neutropenic periods in pediatric acute myeloid leukemia
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 2 / February 2023
- Published online by Cambridge University Press:
- 25 April 2022, pp. 222-229
- Print publication:
- February 2023
-
- Article
- Export citation
Pain perception and physiological correlates in body-focused repetitive behavior disorders
-
- Journal:
- CNS Spectrums / Volume 28 / Issue 2 / April 2023
- Published online by Cambridge University Press:
- 22 March 2022, pp. 197-204
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Childhood adversities and mental disorders in first-year college students: results from the World Mental Health International College Student Initiative
-
- Journal:
- Psychological Medicine / Volume 53 / Issue 7 / May 2023
- Published online by Cambridge University Press:
- 11 January 2022, pp. 2963-2973
-
- Article
- Export citation
Effects of prior deployments and perceived resilience on anger trajectories of combat-deployed soldiers
-
- Journal:
- Psychological Medicine / Volume 53 / Issue 5 / April 2023
- Published online by Cambridge University Press:
- 22 November 2021, pp. 2031-2040
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Neurobiology of subtypes of trichotillomania and skin picking disorder
-
- Journal:
- CNS Spectrums / Volume 28 / Issue 1 / February 2023
- Published online by Cambridge University Press:
- 03 November 2021, pp. 98-103
-
- Article
- Export citation
Antidepressant use in low- middle- and high-income countries: a World Mental Health Surveys report
-
- Journal:
- Psychological Medicine / Volume 53 / Issue 4 / March 2023
- Published online by Cambridge University Press:
- 23 September 2021, pp. 1583-1591
-
- Article
- Export citation
Direct maxillary irrigation therapy in non-operated chronic sinusitis: a prospective randomised controlled trial
-
- Journal:
- The Journal of Laryngology & Otology / Volume 136 / Issue 3 / March 2022
- Published online by Cambridge University Press:
- 01 September 2021, pp. 229-236
- Print publication:
- March 2022
-
- Article
- Export citation
Non-suicidal self-injury among first-year college students and its association with mental disorders: results from the World Mental Health International College Student (WMH-ICS) initiative
-
- Journal:
- Psychological Medicine / Volume 53 / Issue 3 / February 2023
- Published online by Cambridge University Press:
- 18 June 2021, pp. 875-886
-
- Article
- Export citation
The prevalence of mental health problems in sub-Saharan adolescents living with HIV: a systematic review
-
- Journal:
- Global Mental Health / Volume 7 / 2020
- Published online by Cambridge University Press:
- 26 October 2020, e29
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Comorbidity within mental disorders: a comprehensive analysis based on 145 990 survey respondents from 27 countries
-
- Journal:
- Epidemiology and Psychiatric Sciences / Volume 29 / 2020
- Published online by Cambridge University Press:
- 12 August 2020, e153
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Intermittent explosive disorder subtypes in the general population: association with comorbidity, impairment and suicidality
-
- Journal:
- Epidemiology and Psychiatric Sciences / Volume 29 / 2020
- Published online by Cambridge University Press:
- 23 June 2020, e138
-
- Article
-
- You have access
- Open access
- HTML
- Export citation