40 results
Idiopathic Extracranial Internal Carotid Artery Vasospasm
-
- Journal:
- Canadian Journal of Neurological Sciences , First View
- Published online by Cambridge University Press:
- 12 February 2024, pp. 1-2
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
21 - Valvular Diseases
- from Section 4 - Cardiovascular Emergencies
-
-
- Book:
- Practical Emergency Resuscitation and Critical Care
- Published online:
- 02 November 2023
- Print publication:
- 23 November 2023, pp 187-196
-
- Chapter
- Export citation
Frontal sinus stenting in endoscopic sinus surgery: the 10-year Oxford experience
-
- Journal:
- The Journal of Laryngology & Otology / Volume 138 / Issue 1 / January 2024
- Published online by Cambridge University Press:
- 05 April 2023, pp. 60-66
- Print publication:
- January 2024
-
- Article
- Export citation
The use of modified Montgomery T-tubes as frontal sinus stents: how I do it
-
- Journal:
- The Journal of Laryngology & Otology / Volume 136 / Issue 12 / December 2022
- Published online by Cambridge University Press:
- 31 January 2022, pp. 1328-1329
- Print publication:
- December 2022
-
- Article
- Export citation
Duration of stenting with Montgomery T-tubes in severe laryngotracheal stenosis: does it matter?
-
- Journal:
- The Journal of Laryngology & Otology / Volume 136 / Issue 4 / April 2022
- Published online by Cambridge University Press:
- 19 November 2021, pp. 354-359
- Print publication:
- April 2022
-
- Article
- Export citation
Severe conduit stenosis in a patient with Fontan circulation with a Y-shaped Dacron conduit
- Part of
-
- Journal:
- Cardiology in the Young / Volume 31 / Issue 10 / October 2021
- Published online by Cambridge University Press:
- 08 April 2021, pp. 1693-1695
-
- Article
- Export citation
Revision cricotracheal resection: our experience
-
- Journal:
- The Journal of Laryngology & Otology / Volume 135 / Issue 1 / January 2021
- Published online by Cambridge University Press:
- 25 January 2021, pp. 57-63
- Print publication:
- January 2021
-
- Article
- Export citation
Balloon angioplasty of bidirectional Glenn anastomosis
-
- Journal:
- Cardiology in the Young / Volume 30 / Issue 10 / October 2020
- Published online by Cambridge University Press:
- 11 August 2020, pp. 1452-1457
-
- Article
- Export citation
Cochlear nerve canal stenosis and associated semicircular canal abnormalities in paediatric sensorineural hearing loss: a single centre study
-
- Journal:
- The Journal of Laryngology & Otology / Volume 134 / Issue 7 / July 2020
- Published online by Cambridge University Press:
- 27 July 2020, pp. 603-609
- Print publication:
- July 2020
-
- Article
- Export citation
Kawasaki disease with giant aneurysm of left coronary artery and complete occlusion of right coronary artery
-
- Journal:
- Cardiology in the Young / Volume 30 / Issue 4 / April 2020
- Published online by Cambridge University Press:
- 04 March 2020, pp. 580-581
-
- Article
- Export citation
Reduction of cicatricial stenosis after canalplasty for auditory exostoses
-
- Journal:
- The Journal of Laryngology & Otology / Volume 133 / Issue 9 / September 2019
- Published online by Cambridge University Press:
- 22 August 2019, pp. 814-817
- Print publication:
- September 2019
-
- Article
- Export citation
The ancient practice of sutra neti leading to velopharyngeal stenosis: case report
-
- Journal:
- The Journal of Laryngology & Otology / Volume 133 / Issue 8 / August 2019
- Published online by Cambridge University Press:
- 07 June 2019, pp. 730-732
- Print publication:
- August 2019
-
- Article
- Export citation
Feasibility and potential of three-dimensional printing in laryngotracheal stenosis
-
- Journal:
- The Journal of Laryngology & Otology / Volume 133 / Issue 6 / June 2019
- Published online by Cambridge University Press:
- 24 June 2019, pp. 530-534
- Print publication:
- June 2019
-
- Article
- Export citation
Review of children with Takayasu’s arteritis at a Southern African tertiary care centre
-
- Journal:
- Cardiology in the Young / Volume 28 / Issue 9 / September 2018
- Published online by Cambridge University Press:
- 06 July 2018, pp. 1129-1135
-
- Article
- Export citation
Pyriform aperture enlargement in all aspects
-
- Journal:
- The Journal of Laryngology & Otology / Volume 131 / Issue 6 / June 2017
- Published online by Cambridge University Press:
- 27 February 2017, pp. 476-479
- Print publication:
- June 2017
-
- Article
- Export citation
Surgical management of nasal stenosis following chemoradiation for nasopharyngeal carcinoma
-
- Journal:
- The Journal of Laryngology & Otology / Volume 131 / Issue 5 / May 2017
- Published online by Cambridge University Press:
- 15 February 2017, pp. 429-432
- Print publication:
- May 2017
-
- Article
- Export citation
UNSTEADY TWO-LAYERED BLOOD FLOW THROUGH A
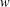 $w$-SHAPED STENOSED ARTERY USING THE GENERALIZED OLDROYD-B FLUID MODEL
$w$-SHAPED STENOSED ARTERY USING THE GENERALIZED OLDROYD-B FLUID MODEL
- Part of
-
- Journal:
- The ANZIAM Journal / Volume 58 / Issue 1 / July 2016
- Published online by Cambridge University Press:
- 21 July 2016, pp. 96-118
-
- Article
-
- You have access
- Export citation
Repair techniques for anomalous aortic origins of the coronary arteries*
-
- Journal:
- Cardiology in the Young / Volume 25 / Issue 8 / December 2015
- Published online by Cambridge University Press:
- 16 December 2015, pp. 1546-1560
-
- Article
- Export citation
MODELLING OF ATHEROSCLEROTIC PLAQUE GROWTH USING FLUID–STRUCTURE INTERACTION
- Part of
-
- Journal:
- Bulletin of the Australian Mathematical Society / Volume 93 / Issue 1 / February 2016
- Published online by Cambridge University Press:
- 02 October 2015, pp. 170-172
- Print publication:
- February 2016
-
- Article
-
- You have access
- Export citation
Primary cardiovascular care for patients with valvar cardiac disease*
-
- Journal:
- Cardiology in the Young / Volume 24 / Issue 6 / December 2014
- Published online by Cambridge University Press:
- 29 December 2014, pp. 1057-1063
-
- Article
- Export citation