75 results
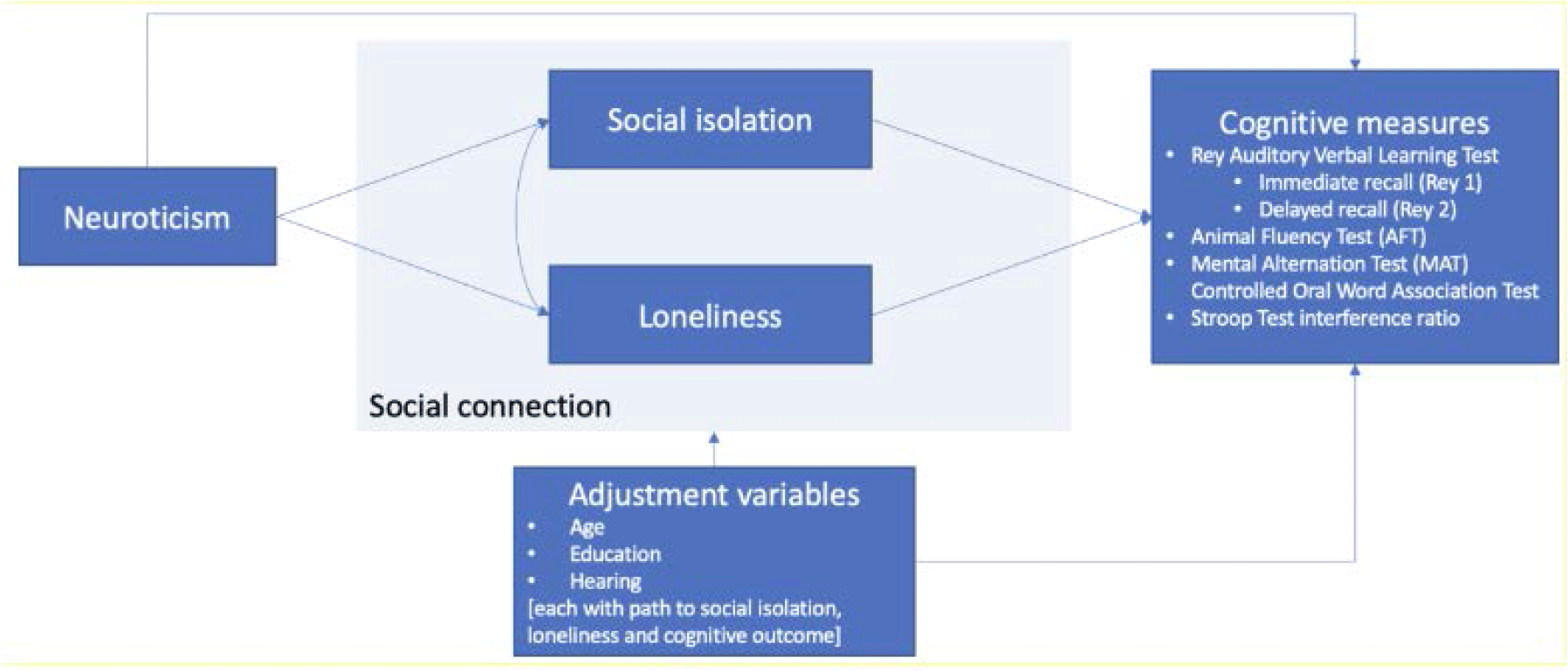
FC30: The relationships between neuroticism, social connection and cognition
-
- Journal:
- International Psychogeriatrics / Volume 35 / Issue S1 / December 2023
- Published online by Cambridge University Press:
- 02 February 2024, pp. 92-94
-
- Article
-
- You have access
- Export citation
Clinicians who primarily practice in nursing homes and outcomes among residents with urinary tract infection or pneumonia
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue 1 / 2023
- Published online by Cambridge University Press:
- 03 January 2024, e253
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Validation of a brief screener for broad-spectrum mental and substance-use disorders in South Africa
-
- Journal:
- Cambridge Prisms: Global Mental Health / Volume 11 / 2024
- Published online by Cambridge University Press:
- 21 December 2023, e4
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
A Data-Driven Approach to Optimizing Medical-Legal Partnership Performance and Joint Advocacy
-
- Journal:
- Journal of Law, Medicine & Ethics / Volume 51 / Issue 4 / Winter 2023
- Published online by Cambridge University Press:
- 13 March 2024, pp. 880-888
- Print publication:
- Winter 2023
-
- Article
- Export citation
Agricultural Research Service Weed Science Research: Past, Present, and Future
-
- Journal:
- Weed Science / Volume 71 / Issue 4 / July 2023
- Published online by Cambridge University Press:
- 16 August 2023, pp. 312-327
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
A review of the conservation status of Black Stork Ciconia nigra in South Africa, Lesotho, and Eswatini
-
- Journal:
- Bird Conservation International / Volume 33 / 2023
- Published online by Cambridge University Press:
- 11 April 2023, e56
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Developmental care pathway for hospitalised infants with CHD: on behalf of the Cardiac Newborn Neuroprotective Network, a Special Interest Group of the Cardiac Neurodevelopmental Outcome Collaborative
-
- Journal:
- Cardiology in the Young / Volume 33 / Issue 12 / December 2023
- Published online by Cambridge University Press:
- 30 March 2023, pp. 2521-2538
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Paediatric cardiology training: burnout, fulfilment, and fears
-
- Journal:
- Cardiology in the Young / Volume 33 / Issue 11 / November 2023
- Published online by Cambridge University Press:
- 24 January 2023, pp. 2274-2281
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Going local: Evaluating guideline adherence and appropriateness of antibiotic prescribing in patients with febrile neutropenia at an academic teaching hospital
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue 1 / 2023
- Published online by Cambridge University Press:
- 09 January 2023, e3
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Using framework analysis to understand multiple stakeholders’ views of vocational rehabilitation following acquired brain injury
-
- Journal:
- Brain Impairment / Volume 24 / Issue 2 / September 2023
- Published online by Cambridge University Press:
- 23 November 2022, pp. 347-370
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Enhancing Artificial Intelligence for Twitter-based Public Discourse on Food Security During the COVID-19 Pandemic
-
- Journal:
- Disaster Medicine and Public Health Preparedness / Accepted manuscript
- Published online by Cambridge University Press:
- 04 August 2022, pp. 1-25
-
- Article
- Export citation
Life Satisfaction and Influenza Vaccination Among Older Adults in Canada
-
- Journal:
- Canadian Journal on Aging / La Revue canadienne du vieillissement / Volume 41 / Issue 4 / December 2022
- Published online by Cambridge University Press:
- 28 July 2022, pp. 514-522
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
A rational explanation for links between the ANS and math
-
- Journal:
- Behavioral and Brain Sciences / Volume 44 / 2021
- Published online by Cambridge University Press:
- 15 December 2021, e194
-
- Article
- Export citation
Deep Learning-Based Point-Scanning Super-Resolution Microscopy
-
- Journal:
- Microscopy and Microanalysis / Volume 27 / Issue S1 / August 2021
- Published online by Cambridge University Press:
- 30 July 2021, pp. 2516-2517
- Print publication:
- August 2021
-
- Article
-
- You have access
- Export citation
Low Back Pain in a Nova Scotian Emergency Department: Prevalence and Patient Characteristics in the Older Adult Patient Population
-
- Journal:
- Canadian Journal on Aging / La Revue canadienne du vieillissement / Volume 41 / Issue 2 / June 2022
- Published online by Cambridge University Press:
- 27 May 2021, pp. 145-153
-
- Article
-
- You have access
- HTML
- Export citation
Severe acute respiratory coronavirus virus 2 (SARS-CoV-2) seroprevalence in healthcare personnel in northern California early in the coronavirus disease 2019 (COVID-19) pandemic
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 42 / Issue 9 / September 2021
- Published online by Cambridge University Press:
- 09 December 2020, pp. 1053-1059
- Print publication:
- September 2021
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Midlife improvements in financial situation and dementia risk: considerations for research, policy, and practice
-
- Journal:
- International Psychogeriatrics / Volume 32 / Issue 11 / November 2020
- Published online by Cambridge University Press:
- 09 December 2020, pp. 1271-1273
-
- Article
- Export citation
Mental practice as a novel learning strategy for donning and doffing personal protective equipment during the COVID-19 pandemic
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 22 / Issue 5 / September 2020
- Published online by Cambridge University Press:
- 24 June 2020, pp. 614-616
- Print publication:
- September 2020
-
- Article
-
- You have access
- HTML
- Export citation
Influenza surveillance case definitions miss a substantial proportion of older adults hospitalized with laboratory-confirmed influenza: A report from the Canadian Immunization Research Network (CIRN) Serious Outcomes Surveillance (SOS) Network
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue 5 / May 2020
- Published online by Cambridge University Press:
- 09 March 2020, pp. 499-504
- Print publication:
- May 2020
-
- Article
- Export citation
An Active Shooter in Your Hospital: A Novel Method to Develop a Response Policy Using In Situ Simulation and Video Framework Analysis
-
- Journal:
- Disaster Medicine and Public Health Preparedness / Volume 15 / Issue 2 / April 2021
- Published online by Cambridge University Press:
- 09 March 2020, pp. 223-231
-
- Article
- Export citation