25 results
Determining cut-off values and predictors for the Snaith–Hamilton Pleasure Scale: comparison between clinical and school settings
-
- Journal:
- BJPsych Open / Volume 10 / Issue 3 / May 2024
- Published online by Cambridge University Press:
- 09 May 2024, e106
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
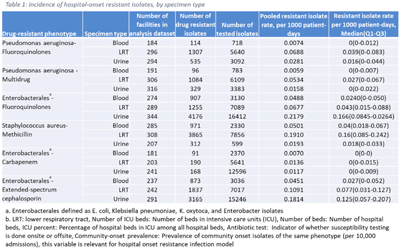
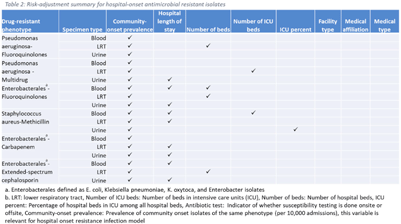
Developing national benchmarks for antimicrobial resistance–NHSN, 2019
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, p. s65
-
- Article
-
- You have access
- Open access
- Export citation
Depression in nursing home residents and its correlation with meaning of family involvement and depression of family
-
- Journal:
- International Psychogeriatrics / Volume 35 / Issue 2 / February 2023
- Published online by Cambridge University Press:
- 11 March 2022, pp. 67-75
-
- Article
- Export citation
Pathogens attributed to central-line–associated bloodstream infections in US acute-care hospitals during the first year of the coronavirus disease 2019 (COVID-19) pandemic
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 4 / April 2023
- Published online by Cambridge University Press:
- 08 February 2022, pp. 651-654
- Print publication:
- April 2023
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Association between prevalence of laboratory-identified Clostridioides difficile infection (CDI) and antibiotic treatment for CDI in US acute-care hospitals, 2019
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 43 / Issue 12 / December 2022
- Published online by Cambridge University Press:
- 24 January 2022, pp. 1847-1852
- Print publication:
- December 2022
-
- Article
- Export citation
Hospital capacities and shortages of healthcare resources among US hospitals during the coronavirus disease 2019 (COVID-19) pandemic, National Healthcare Safety Network (NHSN), March 27–July 14, 2020
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 43 / Issue 10 / October 2022
- Published online by Cambridge University Press:
- 24 June 2021, pp. 1473-1476
- Print publication:
- October 2022
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Impact of coronavirus disease 2019 (COVID-19) on US Hospitals and Patients, April–July 2020
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 43 / Issue 1 / January 2022
- Published online by Cambridge University Press:
- 19 February 2021, pp. 32-39
- Print publication:
- January 2022
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Hospital Microbiologic Culture Results to Predict the Use of Anti–methicillin-Resistant Staphylococcus aureus (MRSA)
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, p. s40
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Risk Factors Associated With Hospital-Onset MRSA Proportion—National Healthcare Safety Network, 2017–2018
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s375-s376
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
The role of basement-involved normal faults in the recent tectonics of western Taiwan
-
- Journal:
- Geological Magazine / Volume 153 / Issue 5-6 / September 2016
- Published online by Cambridge University Press:
- 05 August 2016, pp. 1166-1191
-
- Article
-
- You have access
- HTML
- Export citation
Intractable Hiccup Due to Multiple Sclerosis: MR Imaging of Medullary Plaque
-
- Journal:
- Canadian Journal of Neurological Sciences / Volume 21 / Issue 3 / August 1994
- Published online by Cambridge University Press:
- 18 September 2015, pp. 271-272
-
- Article
-
- You have access
- Export citation
Reassessment of the conservation status and protected area coverage of Taiwanese birds: How distribution modelling can help species conservation
-
- Journal:
- Bird Conservation International / Volume 24 / Issue 2 / June 2014
- Published online by Cambridge University Press:
- 21 June 2013, pp. 223-238
-
- Article
-
- You have access
- HTML
- Export citation
Nosocomial Transmission of Undetected, Imported Measles in Taiwan, 2008
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 30 / Issue 10 / October 2009
- Published online by Cambridge University Press:
- 02 January 2015, pp. 1026-1028
- Print publication:
- October 2009
-
- Article
- Export citation
Influence of DSS-8 on the remineralisation of Dentine
-
- Journal:
- MRS Online Proceedings Library Archive / Volume 1187 / 2009
- Published online by Cambridge University Press:
- 31 January 2011, 1187-KK05-34
- Print publication:
- 2009
-
- Article
- Export citation
Impact of chewing betel-nut (Areca catechu) on liver cirrhosis and hepatocellular carcinoma†: a population-based study from an area with a high prevalence of hepatitis B and C infections
-
- Journal:
- Public Health Nutrition / Volume 12 / Issue 1 / January 2009
- Published online by Cambridge University Press:
- 01 January 2009, pp. 129-135
-
- Article
-
- You have access
- HTML
- Export citation
Effects on Hardness and Elastic Modulus for DSS-8 Peptide Treatment on Remineralization of Human Dental Tissues
-
- Journal:
- MRS Online Proceedings Library Archive / Volume 1132 / 2008
- Published online by Cambridge University Press:
- 15 March 2011, 1132-Z09-05
- Print publication:
- 2008
-
- Article
- Export citation
Modeling of Effect of Stress on C Diffusion/Clustering in Si
-
- Journal:
- MRS Online Proceedings Library Archive / Volume 1070 / 2008
- Published online by Cambridge University Press:
- 01 February 2011, 1070-E03-07
- Print publication:
- 2008
-
- Article
- Export citation
Modeling of Cu Surface Precipitation and Out-Diffusion from Silicon Wafers
-
- Journal:
- MRS Online Proceedings Library Archive / Volume 994 / 2007
- Published online by Cambridge University Press:
- 01 February 2011, 0994-F09-01
- Print publication:
- 2007
-
- Article
- Export citation
Low Temperature Poly-Si Sputtering Deposition Through Metal-induced Crystallization and its Application
-
- Journal:
- MRS Online Proceedings Library Archive / Volume 910 / 2006
- Published online by Cambridge University Press:
- 01 February 2011, 0910-A21-05
- Print publication:
- 2006
-
- Article
- Export citation