312 results
Head and Neck Cancer: United Kingdom National Multidisciplinary Guidelines, Sixth Edition
-
- Journal:
- The Journal of Laryngology & Otology / Volume 138 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 14 March 2024, pp. S1-S224
- Print publication:
- April 2024
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Waka’ Stela 44 and the Early Classic Kaan hegemony
-
- Journal:
- Ancient Mesoamerica , First View
- Published online by Cambridge University Press:
- 04 March 2024, pp. 1-13
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
27 Assessing Differences in Academic Achievement Among a National Sample of Children with Epilepsy Before and During the COVID-19 Pandemic
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 28-29
-
- Article
-
- You have access
- Export citation
3 Latent Wechsler Profiles in Presurgical Pediatric Epilepsy
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 308-310
-
- Article
-
- You have access
- Export citation
26 The Importance of Executive Functioning for Academic Achievement Among a National Sample of Children with Epilepsy
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 26-27
-
- Article
-
- You have access
- Export citation
Investigating the association between characteristics of local crisis care systems and service use in an English national survey – CORRIGENDUM
-
- Journal:
- BJPsych Open / Volume 10 / Issue 1 / January 2024
- Published online by Cambridge University Press:
- 06 December 2023, e6
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Investigating the association between characteristics of local crisis care systems and service use in an English national survey
-
- Journal:
- BJPsych Open / Volume 9 / Issue 6 / November 2023
- Published online by Cambridge University Press:
- 03 November 2023, e209
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Radiofrequency ice dielectric measurements at Summit Station, Greenland
-
- Journal:
- Journal of Glaciology , First View
- Published online by Cambridge University Press:
- 09 October 2023, pp. 1-12
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
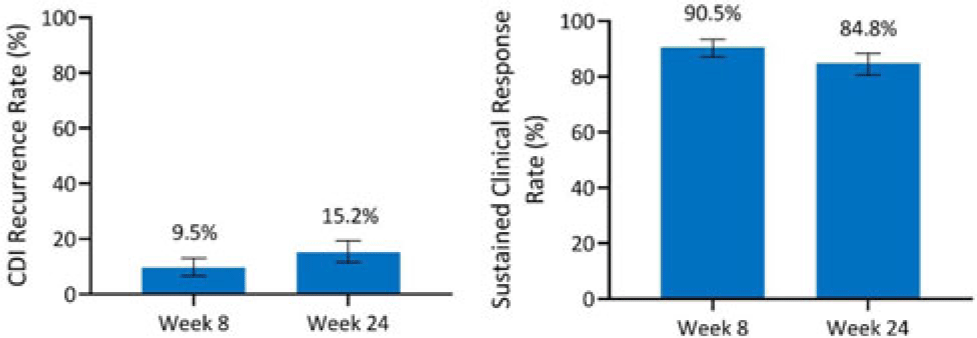
Integrated efficacy analysis from phase 3 studies of investigational microbiome therapeutic, SER-109, in recurrent Clostridioides difficile infection
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, p. s5
-
- Article
-
- You have access
- Open access
- Export citation
Integrated safety analysis of phase 3 studies for investigational microbiome therapeutic, SER-109, in recurrent CDI
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s44-s45
-
- Article
-
- You have access
- Open access
- Export citation
Classic Maya mirror conjurors of Waka', Guatemala
-
- Journal:
- Ancient Mesoamerica / Volume 35 / Issue 1 / Spring 2024
- Published online by Cambridge University Press:
- 14 September 2023, pp. 6-28
- Print publication:
- Spring 2024
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
What Do Beginning Students Think about Philosophy before Their First College Course?
-
- Journal:
- Journal of the American Philosophical Association , First View
- Published online by Cambridge University Press:
- 04 September 2023, pp. 1-11
-
- Article
- Export citation
The effects of advanced factor analysis approaches on outcomes in randomised trials for depression: protocol for secondary analysis of individual participant data
-
- Journal:
- BJPsych Open / Volume 9 / Issue 5 / September 2023
- Published online by Cambridge University Press:
- 11 August 2023, e157
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Ethics information retrieval in HTA: state of current practice
- Part of
-
- Journal:
- International Journal of Technology Assessment in Health Care / Volume 39 / Issue 1 / 2023
- Published online by Cambridge University Press:
- 19 July 2023, e43
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Chapter 4 - Overview of Offenders with Attention Deficit Hyperactivity Disorder
- from Section 1 - An Overview: Definitions, Epidemiology and Policy Issues
-
-
- Book:
- Forensic Aspects of Neurodevelopmental Disorders
- Published online:
- 18 May 2023
- Print publication:
- 01 June 2023, pp 34-47
-
- Chapter
- Export citation
Medics, Mercenaries and Miscreants — A review of Canadian Medical Assistance Teams' EMT Type 1 response to the conflict in Ukraine
-
- Journal:
- Prehospital and Disaster Medicine / Volume 38 / Issue S1 / May 2023
- Published online by Cambridge University Press:
- 13 July 2023, p. s37
- Print publication:
- May 2023
-
- Article
-
- You have access
- Export citation
Estimating the effect of active detection and isolation on Clostridioides difficile infections in a bone marrow transplant unit
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 10 / October 2023
- Published online by Cambridge University Press:
- 13 March 2023, pp. 1614-1619
- Print publication:
- October 2023
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Habitat severity characteristics structure soil communities at regional and local spatial scales along the Antarctica Peninsula
-
- Journal:
- Antarctic Science / Volume 35 / Issue 2 / April 2023
- Published online by Cambridge University Press:
- 01 March 2023, pp. 103-119
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Moderators of peak respiratory exchange ratio during exercise testing in children and adolescents with Fontan physiology
-
- Journal:
- Cardiology in the Young / Volume 33 / Issue 11 / November 2023
- Published online by Cambridge University Press:
- 13 February 2023, pp. 2334-2341
-
- Article
- Export citation
Baseline stool toxin concentration is associated with risk of recurrence in children with Clostridioides difficile infection
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 9 / September 2023
- Published online by Cambridge University Press:
- 10 January 2023, pp. 1403-1409
- Print publication:
- September 2023
-
- Article
- Export citation