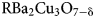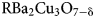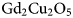51 results
Epidemiology and genomics of a slow outbreak of methicillin-resistant Staphyloccus aureus (MRSA) in a neonatal intensive care unit: Successful chronic decolonization of MRSA-positive healthcare personnel
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 4 / April 2023
- Published online by Cambridge University Press:
- 16 June 2022, pp. 589-596
- Print publication:
- April 2023
-
- Article
- Export citation
Laser-Assisted Field Evaporation of
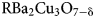 ${\rm RB}{\rm a}_ 2{\rm C}{\rm u}_ 3{\rm O}_{ 7-{\rm \delta }}$ (R = Gd, Sm) High-Temperature Superconducting Coated Conductors
${\rm RB}{\rm a}_ 2{\rm C}{\rm u}_ 3{\rm O}_{ 7-{\rm \delta }}$ (R = Gd, Sm) High-Temperature Superconducting Coated Conductors
-
- Journal:
- Microscopy and Microanalysis / Volume 27 / Issue 6 / December 2021
- Published online by Cambridge University Press:
- 01 October 2021, pp. 1338-1355
- Print publication:
- December 2021
-
- Article
- Export citation
LO39: Using an ambulatory zone to improve physician initial assessment times in a tertiary care hospital emergency department
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 22 / Issue S1 / May 2020
- Published online by Cambridge University Press:
- 13 May 2020, p. S21
- Print publication:
- May 2020
-
- Article
-
- You have access
- Export citation
MP35: Targeting the opioid crisis by influencing opioid prescribing in the emergency department
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 22 / Issue S1 / May 2020
- Published online by Cambridge University Press:
- 13 May 2020, p. S55
- Print publication:
- May 2020
-
- Article
-
- You have access
- Export citation
P030: Assessment of lab results on emergency department patients that leave without seeing a physician
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 22 / Issue S1 / May 2020
- Published online by Cambridge University Press:
- 13 May 2020, p. S75
- Print publication:
- May 2020
-
- Article
-
- You have access
- Export citation
L-methylfolate augmentation of selective serotonin reuptake inhibitors (SSRIS) for major depressive disorder: Results of two randomized, double-blind trials
-
- Journal:
- European Psychiatry / Volume 26 / Issue S2 / March 2011
- Published online by Cambridge University Press:
- 16 April 2020, p. 592
-
- Article
-
- You have access
- Export citation
LO88: Reducing urine culture testing in the emergency department
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 21 / Issue S1 / May 2019
- Published online by Cambridge University Press:
- 02 May 2019, pp. S39-S40
- Print publication:
- May 2019
-
- Article
-
- You have access
- Export citation
LO87: Impact of an evidence-based clinical pathway for suspected renal colic in low-risk patients with previous nephrolithiasis on CT utilization and emergency department throughput
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 21 / Issue S1 / May 2019
- Published online by Cambridge University Press:
- 02 May 2019, p. S39
- Print publication:
- May 2019
-
- Article
-
- You have access
- Export citation
P137: Automation of follow-up microbiology culture results in patients discharged from the emergency department
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 20 / Issue S1 / May 2018
- Published online by Cambridge University Press:
- 11 May 2018, pp. S105-S106
- Print publication:
- May 2018
-
- Article
-
- You have access
- Export citation
MP25: The quality improvement and patient safety curriculum for emergency medicine residents at the University of Toronto: results from the first cohort
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 20 / Issue S1 / May 2018
- Published online by Cambridge University Press:
- 11 May 2018, pp. S49-S50
- Print publication:
- May 2018
-
- Article
-
- You have access
- Export citation
LO26: Reduction of CT scan use in emergency department patients with recurrent renal colic
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 20 / Issue S1 / May 2018
- Published online by Cambridge University Press:
- 11 May 2018, pp. S15-S16
- Print publication:
- May 2018
-
- Article
-
- You have access
- Export citation
LO86: Overutilization of computed tomography as a first-line investigation for patients presenting with suspected recurrent nephrolithiasis in the emergency department: a retrospective cohort study
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 19 / Issue S1 / May 2017
- Published online by Cambridge University Press:
- 15 May 2017, pp. S57-S58
- Print publication:
- May 2017
-
- Article
-
- You have access
- Export citation
Lexicography in-your-face: The active semantics of Pastaza Quichua ideophones
-
- Journal:
- Canadian Journal of Linguistics/Revue canadienne de linguistique / Volume 62 / Issue 2 / June 2017
- Published online by Cambridge University Press:
- 03 April 2017, pp. 154-172
-
- Article
- Export citation
An Interdisciplinary Response to a Tobacco Cessation Case Vignette
-
- Journal:
- Journal of Smoking Cessation / Volume 12 / Issue 3 / September 2017
- Published online by Cambridge University Press:
- 28 March 2016, pp. 153-164
- Print publication:
- September 2017
-
- Article
- Export citation
Direct synthesis of ultra-thin large area transition metal dichalcogenides and their heterostructures on stretchable polymer surfaces
-
- Journal:
- Journal of Materials Research / Volume 31 / Issue 7 / 14 April 2016
- Published online by Cambridge University Press:
- 03 March 2016, pp. 967-974
- Print publication:
- 14 April 2016
-
- Article
- Export citation
Gains in employment status following antidepressant medication or cognitive therapy for depression
-
- Journal:
- The British Journal of Psychiatry / Volume 206 / Issue 4 / April 2015
- Published online by Cambridge University Press:
- 02 January 2018, pp. 332-338
- Print publication:
- April 2015
-
- Article
-
- You have access
- HTML
- Export citation
Factors Associated with Concomitant Psychotropic Drug Use in the Treatment of Major Depression: A STAR*D Report
-
- Journal:
- CNS Spectrums / Volume 14 / Issue 9 / September 2009
- Published online by Cambridge University Press:
- 07 November 2014, pp. 487-498
-
- Article
- Export citation
Contributors
-
-
- Book:
- Acute Care and Emergency Gynecology
- Published online:
- 05 November 2014
- Print publication:
- 30 October 2014, pp ix-xiv
-
- Chapter
- Export citation
Building Performance-Based Accountability With Limited Empirical Evidence: Performance Measurement for Public Health Preparedness
-
- Journal:
- Disaster Medicine and Public Health Preparedness / Volume 7 / Issue 4 / August 2013
- Published online by Cambridge University Press:
- 23 April 2013, pp. 373-379
-
- Article
- Export citation
Long bone histology indicates sympatric species of Dimetrodon (Lower Permian, Sphenacodontidae)
-
- Journal:
- Earth and Environmental Science Transactions of The Royal Society of Edinburgh / Volume 103 / Issue 3-4 / September 2012
- Published online by Cambridge University Press:
- 07 October 2013, pp. 217-236
- Print publication:
- September 2012
-
- Article
- Export citation