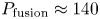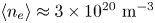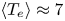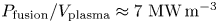75 results
Alcohol milestones and internalizing, externalizing, and executive function: longitudinal and polygenic score associations
-
- Journal:
- Psychological Medicine , First View
- Published online by Cambridge University Press:
- 09 May 2024, pp. 1-14
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
6 Remote Smartphone Cognitive and Motor Testing in Frontotemporal Dementia Research: Feasibility, Reliability, and Validity
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 604-605
-
- Article
-
- You have access
- Export citation
Systematic Review on the Mechanisms of Action of Psilocybin in the Treatment of Depression
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S416-S417
-
- Article
-
- You have access
- Open access
- Export citation
P.043 Long-term safety, tolerability, and efficacy of efgartigimod in patients with Generalized Myasthenia Gravis: concluding analyses from ADAPT+
-
- Journal:
- Canadian Journal of Neurological Sciences / Volume 50 / Issue s2 / June 2023
- Published online by Cambridge University Press:
- 05 June 2023, p. S69
-
- Article
-
- You have access
- Export citation
Examining associations between genetic and neural risk for externalizing behaviors in adolescence and early adulthood
-
- Journal:
- Psychological Medicine / Volume 54 / Issue 2 / January 2024
- Published online by Cambridge University Press:
- 19 May 2023, pp. 267-277
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Characterisation of age and polarity at onset in bipolar disorder
-
- Journal:
- The British Journal of Psychiatry / Volume 219 / Issue 6 / December 2021
- Published online by Cambridge University Press:
- 25 August 2021, pp. 659-669
- Print publication:
- December 2021
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Investigation of convergent and divergent genetic influences underlying schizophrenia and alcohol use disorder
-
- Journal:
- Psychological Medicine / Volume 53 / Issue 4 / March 2023
- Published online by Cambridge University Press:
- 07 July 2021, pp. 1196-1204
-
- Article
- Export citation
A distributed geospatial approach to describe community characteristics for multisite studies
-
- Journal:
- Journal of Clinical and Translational Science / Volume 5 / Issue 1 / 2021
- Published online by Cambridge University Press:
- 05 February 2021, e86
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Neutron Star Extreme Matter Observatory: A kilohertz-band gravitational-wave detector in the global network
- Part of
-
- Journal:
- Publications of the Astronomical Society of Australia / Volume 37 / 2020
- Published online by Cambridge University Press:
- 05 November 2020, e047
-
- Article
-
- You have access
- HTML
- Export citation
Overview of the SPARC tokamak
- Part of
-
- Journal:
- Journal of Plasma Physics / Volume 86 / Issue 5 / October 2020
- Published online by Cambridge University Press:
- 29 September 2020, 865860502
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Polygenic contributions to alcohol use and alcohol use disorders across population-based and clinically ascertained samples
-
- Journal:
- Psychological Medicine / Volume 51 / Issue 7 / May 2021
- Published online by Cambridge University Press:
- 20 January 2020, pp. 1147-1156
-
- Article
- Export citation
Amorphous and Nano-Crystalline Materials in Pristine Carbonaceous Chondrite Meteorites
-
- Journal:
- Microscopy and Microanalysis / Volume 25 / Issue S2 / August 2019
- Published online by Cambridge University Press:
- 05 August 2019, pp. 2452-2453
- Print publication:
- August 2019
-
- Article
-
- You have access
- Export citation
The Comprehensive Assessment of Neurodegeneration and Dementia: Canadian Cohort Study
-
- Journal:
- Canadian Journal of Neurological Sciences / Volume 46 / Issue 5 / September 2019
- Published online by Cambridge University Press:
- 16 July 2019, pp. 499-511
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Observed psychopathology in offspring of parents with major depressive disorder, bipolar disorder and schizophrenia
-
- Journal:
- Psychological Medicine / Volume 50 / Issue 6 / April 2020
- Published online by Cambridge University Press:
- 23 May 2019, pp. 1050-1056
-
- Article
- Export citation
16-Year Survival of the Canadian Collaborative Cohort of Related Dementias
- Part of
-
- Journal:
- Canadian Journal of Neurological Sciences / Volume 45 / Issue 4 / July 2018
- Published online by Cambridge University Press:
- 07 May 2018, pp. 367-374
-
- Article
-
- You have access
- HTML
- Export citation
Some Problems in Aeroplane Structural Design
-
- Journal:
- The Aeronautical Journal / Volume 30 / Issue 184 / April 1926
- Published online by Cambridge University Press:
- 24 August 2017, pp. 238-266
-
- Article
- Export citation
Impact of dysfunctional maternal personality traits on risk of offspring depression, anxiety and self-harm at age 18 years: a population-based longitudinal study
-
- Journal:
- Psychological Medicine / Volume 48 / Issue 1 / January 2018
- Published online by Cambridge University Press:
- 06 June 2017, pp. 50-60
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Tube of Least Weight for Given Torsional Stiffness
-
- Journal:
- The Aeronautical Journal / Volume 57 / Issue 505 / January 1953
- Published online by Cambridge University Press:
- 28 July 2016, pp. 45-46
-
- Article
- Export citation
Certificates of Airworthiness
-
- Journal:
- The Aeronautical Journal / Volume 34 / Issue 233 / May 1930
- Published online by Cambridge University Press:
- 28 July 2016, pp. 361-383
-
- Article
- Export citation
Tubes of Optimum Bending Stiffness: An Analogy
-
- Journal:
- The Aeronautical Journal / Volume 58 / Issue 520 / April 1954
- Published online by Cambridge University Press:
- 28 July 2016, pp. 296-299
-
- Article
- Export citation