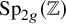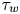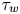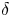886 results
Brain Injury Associated Shock: An Under-Recognized and Challenging Prehospital Phenomenon
-
- Journal:
- Prehospital and Disaster Medicine , First View
- Published online by Cambridge University Press:
- 29 April 2024, pp. 1-6
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Causal Agnosticism About Race: Variable Selection Problems in Causal Inference
-
- Journal:
- Philosophy of Science ,
- Published online by Cambridge University Press:
- 16 February 2024, pp. 1-11
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Protecting and promoting editorial independence
-
- Journal:
- The British Journal of Psychiatry , FirstView
- Published online by Cambridge University Press:
- 15 February 2024, pp. 1-3
-
- Article
-
- You have access
- HTML
- Export citation
Chapter 49 - Preparing Effectively for Emergencies, Incidents, Disasters, and Disease Outbreaks
- from Section 6 - Designing, Leading, and Managing Responses to Emergencies and Pandemics
-
-
- Book:
- Major Incidents, Pandemics and Mental Health
- Published online:
- 11 January 2024
- Print publication:
- 01 February 2024, pp 365-375
-
- Chapter
- Export citation
Chapter 50 - Leadership, Organisation, and Implementation of Emergency Preparedness
- from Section 6 - Designing, Leading, and Managing Responses to Emergencies and Pandemics
-
-
- Book:
- Major Incidents, Pandemics and Mental Health
- Published online:
- 11 January 2024
- Print publication:
- 01 February 2024, pp 376-387
-
- Chapter
- Export citation
Impact of primary care triage using the Head and Neck Cancer Risk Calculator version 2 on tertiary head and neck services in the post-coronavirus disease 2019 period
-
- Journal:
- The Journal of Laryngology & Otology , First View
- Published online by Cambridge University Press:
- 22 January 2024, pp. 1-6
-
- Article
-
- You have access
- HTML
- Export citation
4 Risk Factor and Biomarker Correlates of FLAIR White Matter Hyperintensities in Former American Football Players
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 608-610
-
- Article
-
- You have access
- Export citation
A Silurian (Homerian) pelmatozoan echinoderm fauna from west-central Ohio, USA
-
- Journal:
- Journal of Paleontology / Volume 97 / Issue 5 / September 2023
- Published online by Cambridge University Press:
- 13 December 2023, pp. 1070-1091
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Radiofrequency ice dielectric measurements at Summit Station, Greenland
-
- Journal:
- Journal of Glaciology , First View
- Published online by Cambridge University Press:
- 09 October 2023, pp. 1-12
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Sex differences in iron status during military training: a prospective cohort study of longitudinal changes and associations with endurance performance and musculoskeletal outcomes
-
- Journal:
- British Journal of Nutrition / Volume 131 / Issue 4 / 28 February 2024
- Published online by Cambridge University Press:
- 21 September 2023, pp. 581-592
- Print publication:
- 28 February 2024
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
At the Intersections of History: Collaborative, Public Archaeology of the Nineteenth-Century Tom Cook Blacksmith Shop along the Chisholm Trail in Bolivar, Texas
-
- Journal:
- Advances in Archaeological Practice / Volume 11 / Issue 3 / August 2023
- Published online by Cambridge University Press:
- 06 September 2023, pp. 328-340
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Why a group-level analysis is essential for effective public policy: The case for a g-frame
-
- Journal:
- Behavioral and Brain Sciences / Volume 46 / 2023
- Published online by Cambridge University Press:
- 30 August 2023, e148
-
- Article
- Export citation
Environmental contamination of postmortem blood cultures detected by whole-genome sequencing surveillance
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 12 / December 2023
- Published online by Cambridge University Press:
- 24 August 2023, pp. 2103-2105
- Print publication:
- December 2023
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
The psychological and social impact of the digital self-support system ‘Brain in Hand’ on autistic people: prospective cohort study in England and Wales
-
- Journal:
- BJPsych Open / Volume 9 / Issue 3 / May 2023
- Published online by Cambridge University Press:
- 26 May 2023, e96
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
266 Decoding the role of polyamine metabolism on anti-tumor immunity in head and neck cancer
- Part of
-
- Journal:
- Journal of Clinical and Translational Science / Volume 7 / Issue s1 / April 2023
- Published online by Cambridge University Press:
- 24 April 2023, p. 80
-
- Article
-
- You have access
- Open access
- Export citation
On the Torelli Lie algebra
-
- Journal:
- Forum of Mathematics, Pi / Volume 11 / 2023
- Published online by Cambridge University Press:
- 14 April 2023, e13
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Wall-pressure fluctuations in an axisymmetric boundary layer under strong adverse pressure gradient
-
- Journal:
- Journal of Fluid Mechanics / Volume 960 / 10 April 2023
- Published online by Cambridge University Press:
- 05 April 2023, A28
-
- Article
-
- You have access
- Open access
- HTML
- Export citation

Strategy-Making and Organizational Evolution
- A Managerial Agency Perspective
-
- Published online:
- 06 March 2023
- Print publication:
- 23 March 2023
-
- Element
- Export citation
Development of the Residual Lesion Score for congenital heart surgery: the RAND Delphi methodology
-
- Journal:
- Cardiology in the Young / Volume 33 / Issue 6 / June 2023
- Published online by Cambridge University Press:
- 23 December 2022, pp. 977-990
-
- Article
- Export citation
23 - William R. Catton, Jr. and Riley E. Dunlap (1978)
- from Part III - Socio-Environmental Research in Economics, Sociology, and Political Science
-
- Book:
- Foundations of Socio-Environmental Research
- Published online:
- 18 November 2022
- Print publication:
- 08 December 2022, pp 343-351
-
- Chapter
- Export citation