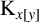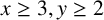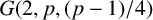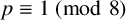109 results
Variation in the structural order of kaolinite in regolith as an effective indicator of REE mineralization
-
- Journal:
- Clays and Clay Minerals / Volume 72 / 2024
- Published online by Cambridge University Press:
- 03 June 2024, e1
-
- Article
- Export citation
P63: Best Practice Guidance on Human Interaction with Technology in Dementia Update June 2023 – Recommendations from the INDUCT and DISTINCT Networks
-
- Journal:
- International Psychogeriatrics / Volume 35 / Issue S1 / December 2023
- Published online by Cambridge University Press:
- 02 February 2024, pp. 158-159
-
- Article
-
- You have access
- Export citation
Spicy food consumption reduces the risk of ischaemic stroke: a prospective study
-
- Journal:
- British Journal of Nutrition / Volume 131 / Issue 10 / 28 May 2024
- Published online by Cambridge University Press:
- 30 January 2024, pp. 1777-1785
- Print publication:
- 28 May 2024
-
- Article
- Export citation
Genetic Association Studies in Restless Legs Syndrome: Risk Variants & Ethnic Differences
-
- Journal:
- Canadian Journal of Neurological Sciences , First View
- Published online by Cambridge University Press:
- 25 January 2024, pp. 1-16
-
- Article
- Export citation
Distribution and Fractionation of Rare Earth Elements (REE) in the Ion Adsorption-type REE Deposit (IAD) at Maofeng Mountain, Guangzhou, China
-
- Journal:
- Clays and Clay Minerals / Volume 71 / Issue 3 / June 2023
- Published online by Cambridge University Press:
- 01 January 2024, pp. 340-361
-
- Article
- Export citation
Relationship Between Pb2+ Adsorption and Average Mn Oxidation State in Synthetic Birnessites
-
- Journal:
- Clays and Clay Minerals / Volume 57 / Issue 5 / October 2009
- Published online by Cambridge University Press:
- 01 January 2024, pp. 513-520
-
- Article
- Export citation
Mineralogical Evolution of the Paleogene Formations in the Kyzyltokoy Basin, Kyrgyzstan: Implications for the Formation of Glauconite
-
- Journal:
- Clays and Clay Minerals / Volume 66 / Issue 1 / February 2018
- Published online by Cambridge University Press:
- 01 January 2024, pp. 43-60
-
- Article
- Export citation
Compact Thomson Scattering Source Based on a Mixed Injection Assisted Laser Wakefield Accelerator
-
- Journal:
- Laser and Particle Beams / Volume 2022 / 2022
- Published online by Cambridge University Press:
- 01 January 2024, e9
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Promoting conservation of fireflies in Kuala Lumpur's urban park through experiential learning
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Social mixing and network characteristics of COVID-19 patients before and after widespread interventions: A population-based study
-
- Journal:
- Epidemiology & Infection / Volume 151 / 2023
- Published online by Cambridge University Press:
- 14 August 2023, e141
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
SG-APSIC1091: Assessment of compliance to cleaning of computers by healthcare workers (HCWs) using adenosine triphosphate (ATP) measurement
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S1 / February 2023
- Published online by Cambridge University Press:
- 16 March 2023, pp. s12-s13
-
- Article
-
- You have access
- Open access
- Export citation
SG-APSIC1122: Observational study of handwashing sink activities in the inpatient setting
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S1 / February 2023
- Published online by Cambridge University Press:
- 16 March 2023, pp. s14-s15
-
- Article
-
- You have access
- Open access
- Export citation
SG-APSIC1118: Introduction of carbapenemase-producing Enterobacterales (CPE) in the aqueous environment of the newly built National Centre for Infectious Diseases (NCID) in Singapore
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S1 / February 2023
- Published online by Cambridge University Press:
- 16 March 2023, pp. s11-s12
-
- Article
-
- You have access
- Open access
- Export citation
SG-APSIC1158: COVID-19 vaccine booster hesitancy among healthcare workers: A retrospective observational study in Singapore
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S1 / February 2023
- Published online by Cambridge University Press:
- 16 March 2023, pp. s3-s4
-
- Article
-
- You have access
- Open access
- Export citation
Re-exploration of dietary iodine intake in Chinese adult males using a modified iodine balance study
-
- Journal:
- British Journal of Nutrition / Volume 130 / Issue 8 / 28 October 2023
- Published online by Cambridge University Press:
- 06 March 2023, pp. 1308-1315
- Print publication:
- 28 October 2023
-
- Article
- Export citation
Transmission roles of symptomatic and asymptomatic COVID-19 cases: a modelling study
-
- Journal:
- Epidemiology & Infection / Volume 150 / 2022
- Published online by Cambridge University Press:
- 27 September 2022, e171
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
FINITE TWO-DISTANCE-TRANSITIVE DIHEDRANTS
- Part of
-
- Journal:
- Journal of the Australian Mathematical Society / Volume 113 / Issue 3 / December 2022
- Published online by Cambridge University Press:
- 26 January 2022, pp. 386-401
- Print publication:
- December 2022
-
- Article
- Export citation
Floods Amidst COVID-19 in Malaysia: Implications on the Pandemic Responses
-
- Journal:
- Disaster Medicine and Public Health Preparedness / Volume 16 / Issue 6 / December 2022
- Published online by Cambridge University Press:
- 23 December 2021, pp. 2218-2219
-
- Article
-
- You have access
- HTML
- Export citation
Longitudinal trajectory analysis of antipsychotic response in patients with schizophrenia: 6-week, randomised, open-label, multicentre clinical trial – CORRIGENDUM
-
- Journal:
- BJPsych Open / Volume 7 / Issue 5 / September 2021
- Published online by Cambridge University Press:
- 20 August 2021, e153
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Extracellular Vesicles Modulate Formation of Transmissive Mutant Huntingtin Assemblies
-
- Journal:
- Microscopy and Microanalysis / Volume 27 / Issue S1 / August 2021
- Published online by Cambridge University Press:
- 30 July 2021, pp. 2826-2830
- Print publication:
- August 2021
-
- Article
-
- You have access
- Export citation