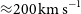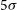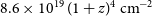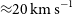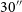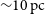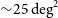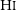185 results
Diagnostic stewardship and the coronavirus disease 2019 (COVID-19) pandemic: Lessons learned for prevention of emerging infectious diseases in acute-care settings
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 45 / Issue 3 / March 2024
- Published online by Cambridge University Press:
- 07 November 2023, pp. 277-283
- Print publication:
- March 2024
-
- Article
-
- You have access
- HTML
- Export citation
REAP-2: An interactive quantitative tool for robust and efficient dose-response curve estimation
-
- Journal:
- Journal of Clinical and Translational Science / Volume 7 / Issue 1 / 2023
- Published online by Cambridge University Press:
- 13 October 2023, e219
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Systematic Review on the Mechanisms of Action of Psilocybin in the Treatment of Depression
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S416-S417
-
- Article
-
- You have access
- Open access
- Export citation
Childhood adversities and risk of posttraumatic stress disorder and major depression following a motor vehicle collision in adulthood
-
- Journal:
- Epidemiology and Psychiatric Sciences / Volume 32 / 2023
- Published online by Cambridge University Press:
- 10 January 2023, e1
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
WALLABY pilot survey: Public release of H i data for almost 600 galaxies from phase 1 of ASKAP pilot observations
-
- Journal:
- Publications of the Astronomical Society of Australia / Volume 39 / 2022
- Published online by Cambridge University Press:
- 15 November 2022, e058
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Preoperative mental illness and postoperative atrial fibrillation in cardiac surgery patients: Identifying a vulnerable population
-
- Journal:
- Journal of Clinical and Translational Science / Volume 7 / Issue 1 / 2023
- Published online by Cambridge University Press:
- 15 November 2022, e15
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
GASKAP-HI pilot survey science I: ASKAP zoom observations of Hi emission in the Small Magellanic Cloud
-
- Journal:
- Publications of the Astronomical Society of Australia / Volume 39 / 2022
- Published online by Cambridge University Press:
- 07 February 2022, e005
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Prediction models in first-episode psychosis: systematic review and critical appraisal
-
- Journal:
- The British Journal of Psychiatry / Volume 220 / Issue 4 / April 2022
- Published online by Cambridge University Press:
- 24 January 2022, pp. 179-191
- Print publication:
- April 2022
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Antidepressant use in low- middle- and high-income countries: a World Mental Health Surveys report
-
- Journal:
- Psychological Medicine / Volume 53 / Issue 4 / March 2023
- Published online by Cambridge University Press:
- 23 September 2021, pp. 1583-1591
-
- Article
- Export citation
Evaluation of point-of-care thumb-size bispectral electroencephalography device to quantify delirium severity and predict mortality
-
- Journal:
- The British Journal of Psychiatry / Volume 220 / Issue 6 / June 2022
- Published online by Cambridge University Press:
- 02 August 2021, pp. 322-329
- Print publication:
- June 2022
-
- Article
-
- You have access
- HTML
- Export citation
Australian square kilometre array pathfinder: I. system description
- Part of
-
- Journal:
- Publications of the Astronomical Society of Australia / Volume 38 / 2021
- Published online by Cambridge University Press:
- 05 March 2021, e009
-
- Article
-
- You have access
- HTML
- Export citation
Comorbidity within mental disorders: a comprehensive analysis based on 145 990 survey respondents from 27 countries
-
- Journal:
- Epidemiology and Psychiatric Sciences / Volume 29 / 2020
- Published online by Cambridge University Press:
- 12 August 2020, e153
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
LO86: Lack of association between four biomarkers and the presence of persistent post-concussion symptoms after a mild traumatic brain injury
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 22 / Issue S1 / May 2020
- Published online by Cambridge University Press:
- 13 May 2020, pp. S38-S39
- Print publication:
- May 2020
-
- Article
-
- You have access
- Export citation
LO88: S100B serum protein level for the detection of clinically significant intracranial hemorrhage in patients with mild traumatic brain injury: a prospective cohort study
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 22 / Issue S1 / May 2020
- Published online by Cambridge University Press:
- 13 May 2020, p. S39
- Print publication:
- May 2020
-
- Article
-
- You have access
- Export citation
LO87: Influence of co-injuries on post-concussion symptoms after a mild traumatic brain injury
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 22 / Issue S1 / May 2020
- Published online by Cambridge University Press:
- 13 May 2020, p. S39
- Print publication:
- May 2020
-
- Article
-
- You have access
- Export citation
LO89: Describing the evolution of post-concussion symptoms after sports-related mTBI
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 22 / Issue S1 / May 2020
- Published online by Cambridge University Press:
- 13 May 2020, p. S40
- Print publication:
- May 2020
-
- Article
-
- You have access
- Export citation
P130: Feasibility of self-assessing functional status in older emergency department patients
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 22 / Issue S1 / May 2020
- Published online by Cambridge University Press:
- 13 May 2020, p. S111
- Print publication:
- May 2020
-
- Article
-
- You have access
- Export citation
Influence of endothelial glycocalyx layer microstructure upon its role as a mechanotransducer
-
- Journal:
- Journal of Fluid Mechanics / Volume 893 / 25 June 2020
- Published online by Cambridge University Press:
- 22 April 2020, A20
-
- Article
- Export citation
Associations of affective disorder in patients with inflammatory bowel disease
-
- Journal:
- European Psychiatry / Volume 26 / Issue S2 / March 2011
- Published online by Cambridge University Press:
- 16 April 2020, p. 2220
-
- Article
-
- You have access
- Export citation
Pkd1-targeted mutation reveals a role for the Wolffian duct in autosomal dominant polycystic kidney disease
-
- Journal:
- Journal of Developmental Origins of Health and Disease / Volume 11 / Issue 1 / February 2020
- Published online by Cambridge University Press:
- 15 August 2019, pp. 78-85
-
- Article
- Export citation