278 results
Naturally-Occurring Silicates as Carriers for Copper Catalysts used in Methanol Conversion
-
- Journal:
- Clays and Clay Minerals / Volume 40 / Issue 2 / April 1992
- Published online by Cambridge University Press:
- 28 February 2024, pp. 167-174
-
- Article
- Export citation
On the Structural Stability of Montmorillonite Submitted to Heavy γ-Irradiation
-
- Journal:
- Clays and Clay Minerals / Volume 50 / Issue 1 / February 2002
- Published online by Cambridge University Press:
- 01 January 2024, pp. 35-37
-
- Article
- Export citation
The role of primary health care in long-term care facilities during the COVID-19 pandemic in 30 European countries: a retrospective descriptive study (Eurodata study)
-
- Journal:
- Primary Health Care Research & Development / Volume 24 / 2023
- Published online by Cambridge University Press:
- 24 October 2023, e60
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Coronavirus disease 2019 is associated with long-term depressive symptoms in Spanish older adults with overweight/obesity and metabolic syndrome
-
- Journal:
- Psychological Medicine / Volume 54 / Issue 3 / February 2024
- Published online by Cambridge University Press:
- 05 September 2023, pp. 620-630
-
- Article
- Export citation
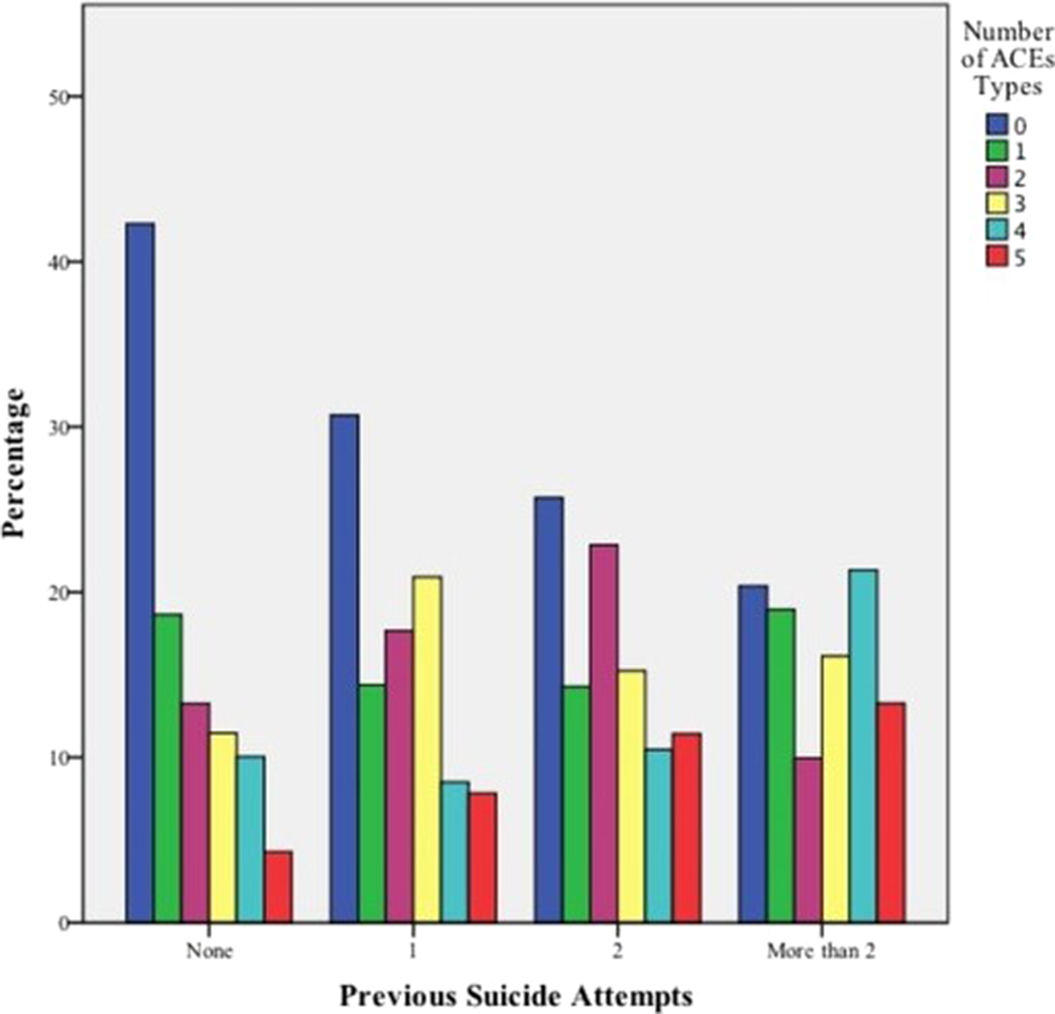
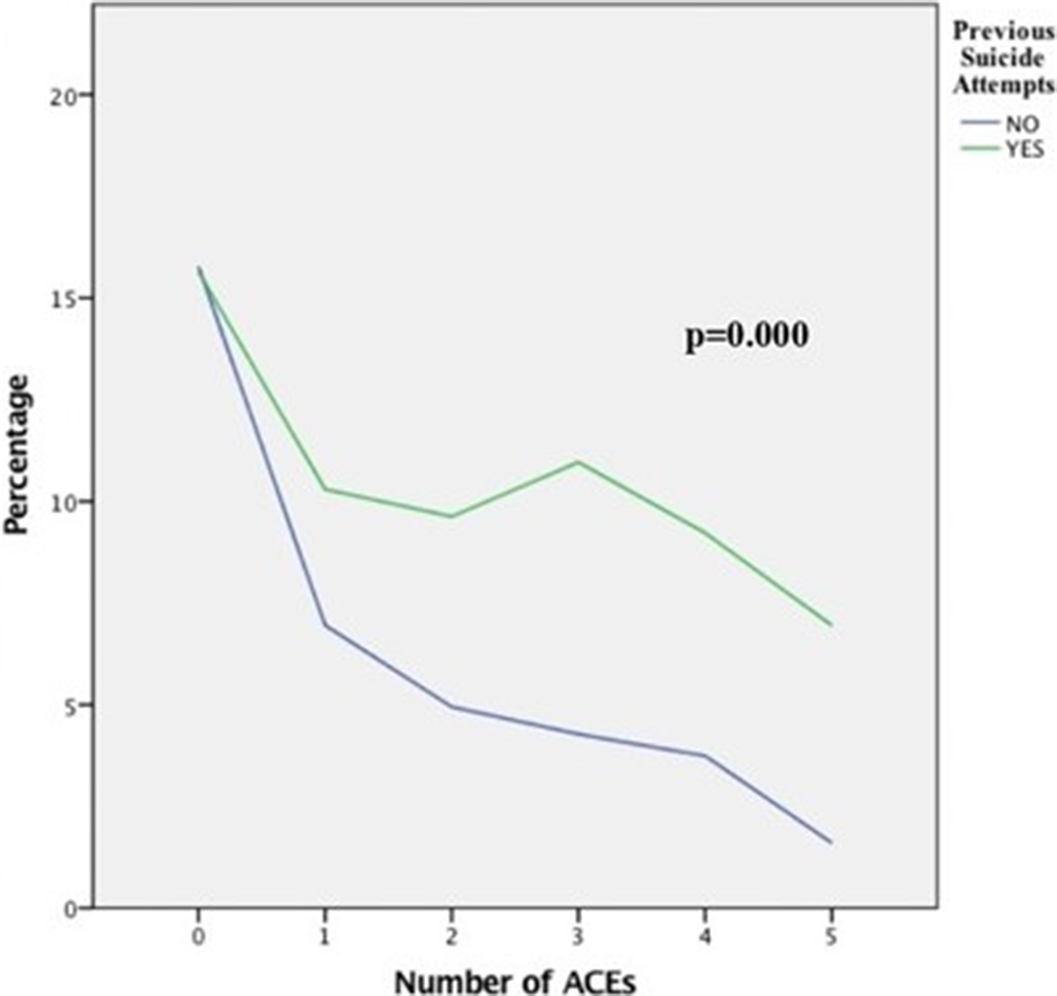
Association between adverse childhood experiences and the number of suicide attempts in lifetime
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S561-S562
-
- Article
-
- You have access
- Open access
- Export citation
Chemsex behaviours, sexual response and sexual health
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S644
-
- Article
-
- You have access
- Open access
- Export citation
Substance Use Disorders and other Mental Health Disorders associated with sexualized intravenous sbustance use (slamsex)
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S380
-
- Article
-
- You have access
- Open access
- Export citation
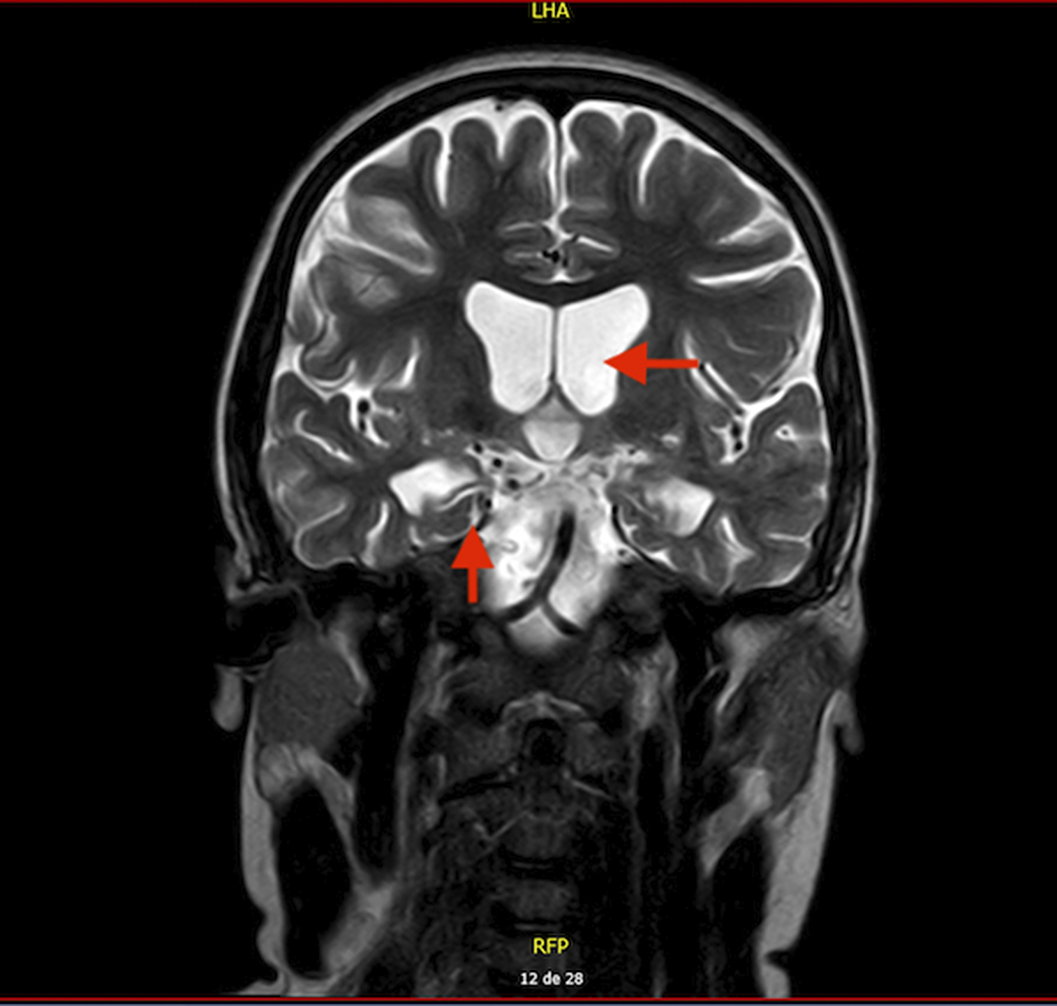
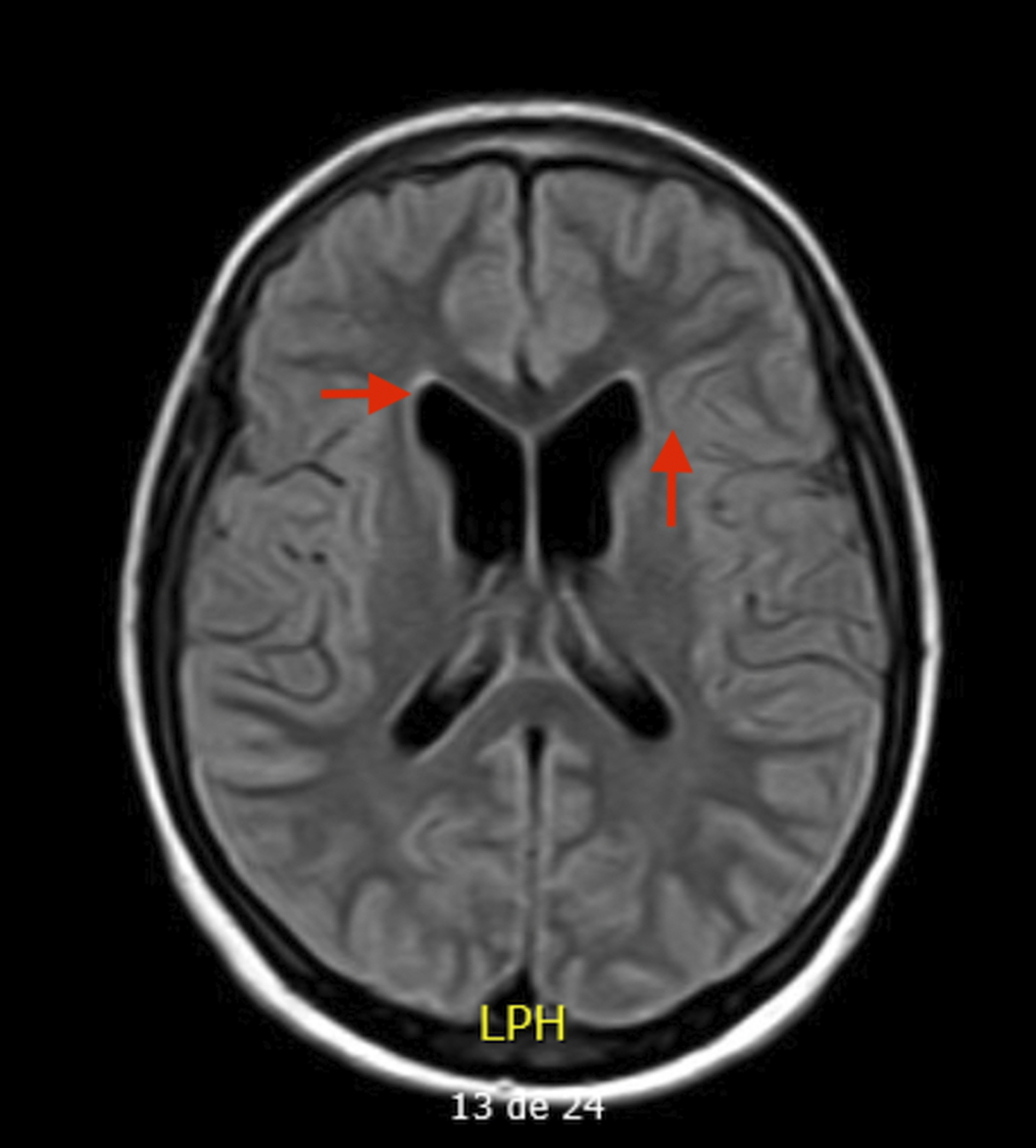
“Unspecified organic personality and behavioral disorder due to brain damage from HHV-6 encephalitis in child. case report and literature review”
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S143-S144
-
- Article
-
- You have access
- Open access
- Export citation
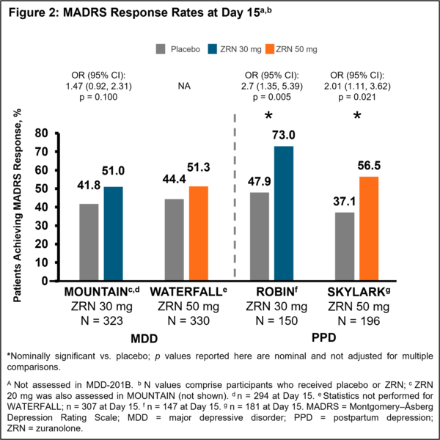
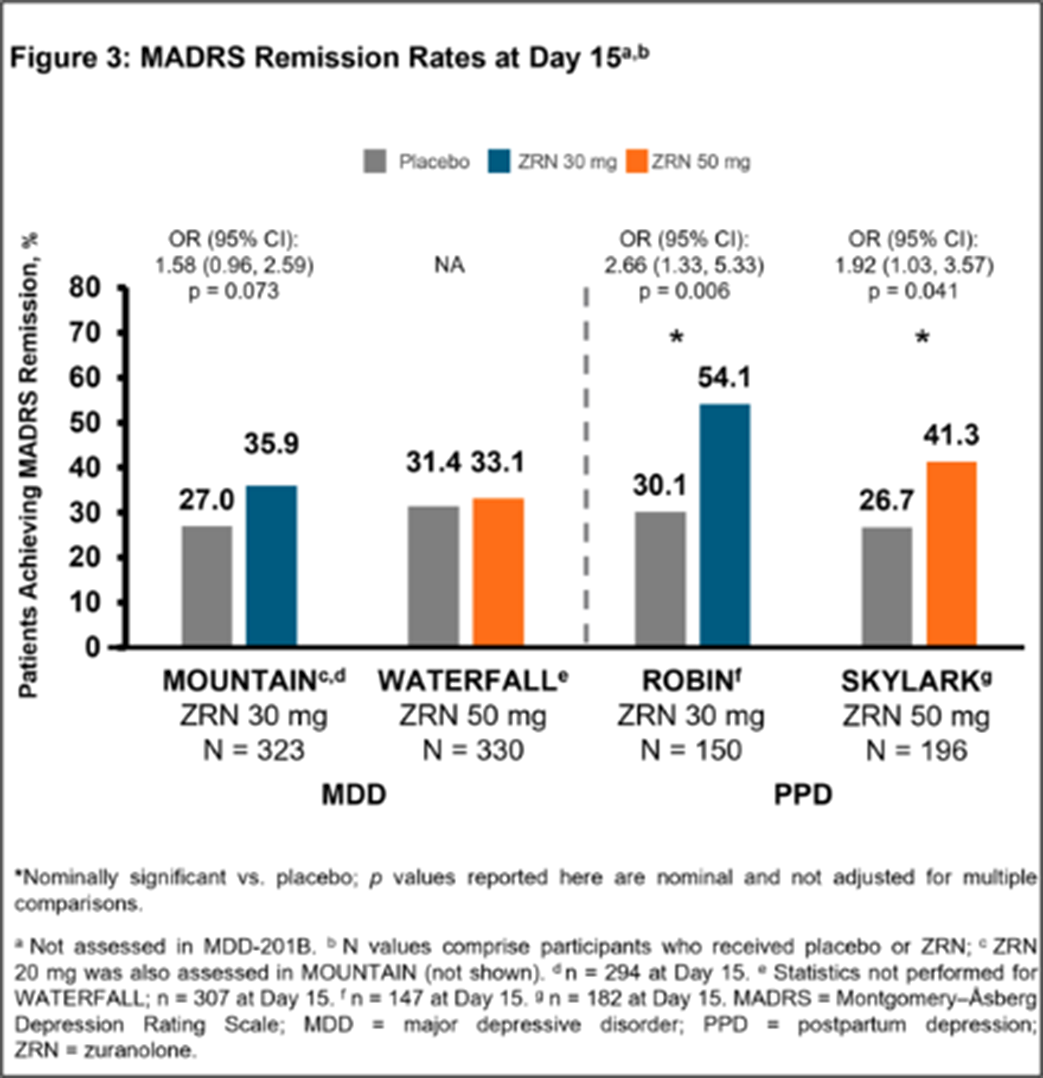
Rapid improvements in MADRS with zuranolone in major depressive disorder and postpartum depression: results from the LANDSCAPE/NEST clinical development programmes
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S93-S94
-
- Article
-
- You have access
- Open access
- Export citation
Virtual self-conversation to support people living with obesity when starting their change process towards a healthier lifestyle: Preliminary results of a longitudinal study
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S110
-
- Article
-
- You have access
- Open access
- Export citation
Changes in the characteristics of Suicide Attempts during COVID-19 pandemic
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S405
-
- Article
-
- You have access
- Open access
- Export citation
Sexual motivations for engaging in chemsex behaviours
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S662-S663
-
- Article
-
- You have access
- Open access
- Export citation
Non-schizophrenic psychotic disorders: Cycloid psychosis. Case report and literature review
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S636
-
- Article
-
- You have access
- Open access
- Export citation
Cerebellar dysfunction and autism spectrum disorders – what do we know?
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S239
-
- Article
-
- You have access
- Open access
- Export citation
Clinical characteristics of chemsex users attended in a ngo in madrid
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S644
-
- Article
-
- You have access
- Open access
- Export citation
P.026 Frontal cognitive-behavioural deficits in patients with anti-leucine-rich glioma-inactivated protein 1 antibody encephalitis
-
- Journal:
- Canadian Journal of Neurological Sciences / Volume 50 / Issue s2 / June 2023
- Published online by Cambridge University Press:
- 05 June 2023, p. S64
-
- Article
-
- You have access
- Export citation
BIG LITTLE THIEFS - Kleptomania Treatment
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S878
-
- Article
-
- You have access
- Open access
- Export citation
Mental Health and economic effects: correlation between unemployment and psychoactive drugs
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S632
-
- Article
-
- You have access
- Open access
- Export citation
Child psychiatric emergency visits during the COVID-19 pandemic
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S510-S511
-
- Article
-
- You have access
- Open access
- Export citation
Trametinib for Painful Glomus Tumors in a Patient with Neurofibromatosis Type 1
-
- Journal:
- Canadian Journal of Neurological Sciences / Volume 50 / Issue 3 / May 2023
- Published online by Cambridge University Press:
- 31 March 2022, pp. 477-478
-
- Article
-
- You have access
- HTML
- Export citation