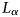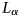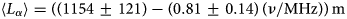169 results
Experiences of support received by carers of people who are involuntarily admitted to hospital under the Mental Health Act: qualitative study of carers’ perspectives
-
- Journal:
- BJPsych Open / Volume 10 / Issue 3 / May 2024
- Published online by Cambridge University Press:
- 16 April 2024, e82
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Modeling the Adsorption of Organic Dye Molecules to Kaolinite
-
- Journal:
- Clays and Clay Minerals / Volume 54 / Issue 4 / August 2006
- Published online by Cambridge University Press:
- 01 January 2024, pp. 456-465
-
- Article
- Export citation
Studies on the Adsorption of Dyes to Kaolinite
-
- Journal:
- Clays and Clay Minerals / Volume 54 / Issue 4 / August 2006
- Published online by Cambridge University Press:
- 01 January 2024, pp. 435-448
-
- Article
- Export citation
Competitive Adsorption of Cd and Dyes to Kaolinite
-
- Journal:
- Clays and Clay Minerals / Volume 54 / Issue 4 / August 2006
- Published online by Cambridge University Press:
- 01 January 2024, pp. 449-455
-
- Article
- Export citation
Conjugated hyperbilirubinemia is associated with increased morbidity and mortality after neonatal heart surgery
-
- Journal:
- Cardiology in the Young , First View
- Published online by Cambridge University Press:
- 18 December 2023, pp. 1-8
-
- Article
- Export citation
Radiofrequency ice dielectric measurements at Summit Station, Greenland
-
- Journal:
- Journal of Glaciology , First View
- Published online by Cambridge University Press:
- 09 October 2023, pp. 1-12
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
The Influence of Length of Time in a Rescue Shelter on the Behaviour of Kennelled Dogs
-
- Journal:
- Animal Welfare / Volume 11 / Issue 3 / August 2002
- Published online by Cambridge University Press:
- 11 January 2023, pp. 317-325
-
- Article
- Export citation
The Influence of Auditory Stimulation on the Behaviour of Dogs Housed in a Rescue Shelter
-
- Journal:
- Animal Welfare / Volume 11 / Issue 4 / November 2002
- Published online by Cambridge University Press:
- 11 January 2023, pp. 385-393
-
- Article
- Export citation
The Behaviour of Dogs in a Rescue Shelter
-
- Journal:
- Animal Welfare / Volume 1 / Issue 3 / August 1992
- Published online by Cambridge University Press:
- 11 January 2023, pp. 171-186
-
- Article
- Export citation
Caring for carers: A virtual psychosocial supervision intervention to improve the quality and sustainability of mental health and psychosocial support in humanitarian contexts
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S884
-
- Article
-
- You have access
- Open access
- Export citation
Supreme Court Impacts in Public Health Law: 2021-2022
-
- Journal:
- Journal of Law, Medicine & Ethics / Volume 50 / Issue 3 / Fall 2022
- Published online by Cambridge University Press:
- 18 November 2022, pp. 608-612
- Print publication:
- Fall 2022
-
- Article
- Export citation
Practice Variation among Canadian Stroke Prevention Clinics: Pre, During, and Post-COVID-19
-
- Journal:
- Canadian Journal of Neurological Sciences / Volume 50 / Issue 4 / July 2023
- Published online by Cambridge University Press:
- 16 June 2022, pp. 551-560
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
In situ, broadband measurement of the radio frequency attenuation length at Summit Station, Greenland
-
- Journal:
- Journal of Glaciology / Volume 68 / Issue 272 / December 2022
- Published online by Cambridge University Press:
- 30 May 2022, pp. 1234-1242
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
The long cross-over dynamics of capillary imbibition
-
- Journal:
- Journal of Fluid Mechanics / Volume 939 / 25 May 2022
- Published online by Cambridge University Press:
- 31 March 2022, A39
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Effect of managed transition on mental health outcomes for young people at the child–adult mental health service boundary: a randomised clinical trial
-
- Journal:
- Psychological Medicine / Volume 53 / Issue 6 / April 2023
- Published online by Cambridge University Press:
- 29 October 2021, pp. 2193-2204
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Legal Challenges Underlying COVID-19 Vaccinations
-
- Journal:
- Journal of Law, Medicine & Ethics / Volume 49 / Issue 3 / Fall 2021
- Published online by Cambridge University Press:
- 19 October 2021, pp. 495-499
- Print publication:
- Fall 2021
-
- Article
- Export citation
Chapter 2 - Screening and Assessment Methods for Wellness
- from Part I - Approach to Wellness
-
-
- Book:
- The Handbook of Wellness Medicine
- Published online:
- 18 September 2020
- Print publication:
- 20 August 2020, pp 13-22
-
- Chapter
- Export citation
LO09: Role of hospitalization for detection of serious adverse events among emergency department patients with syncope: a propensity-score matched analysis of a multicenter prospective cohort
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 22 / Issue S1 / May 2020
- Published online by Cambridge University Press:
- 13 May 2020, p. S10
- Print publication:
- May 2020
-
- Article
-
- You have access
- Export citation
LO08: A randomized, controlled comparison of electrical versus pharmacological cardioversion for emergency department patients with atrial flutter
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 22 / Issue S1 / May 2020
- Published online by Cambridge University Press:
- 13 May 2020, p. S9
- Print publication:
- May 2020
-
- Article
-
- You have access
- Export citation
LO20: The characteristics, clinical course and disposition of long-term care patients treated by paramedics during an emergency call: Exploring the potential impact of community paramedicine
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 22 / Issue S1 / May 2020
- Published online by Cambridge University Press:
- 13 May 2020, p. S14
- Print publication:
- May 2020
-
- Article
-
- You have access
- Export citation