123 results
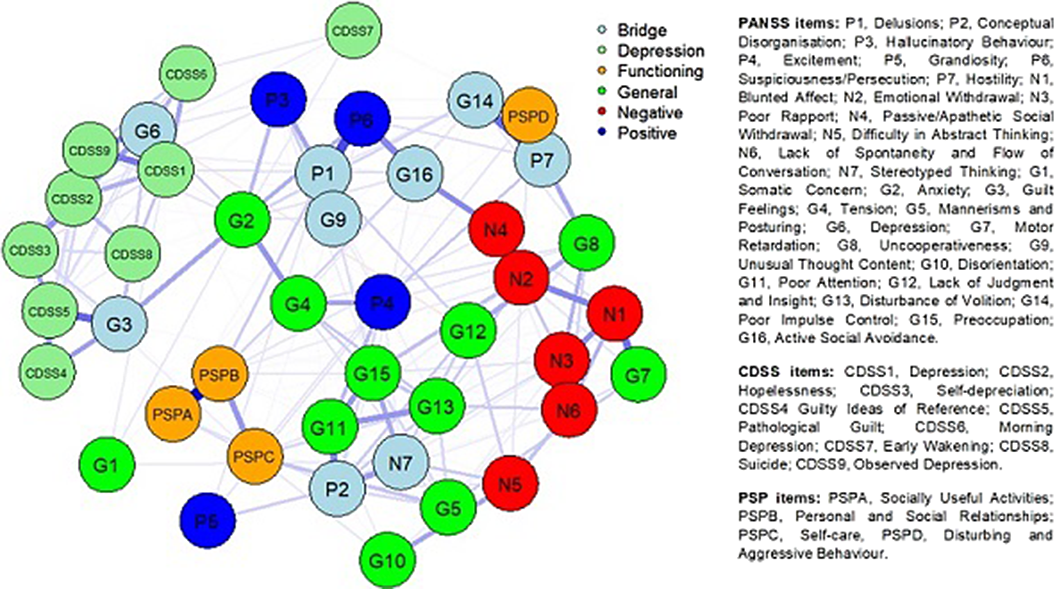
Searching for bridges between psychopathology and real-world functioning in first-episode psychosis: a network analysis from the OPTiMiSE trial
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S262-S263
-
- Article
-
- You have access
- Open access
- Export citation
Resting-state brain activity dysfunctions in schizophrenia and their associations with negative symptom domains
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S550-S551
-
- Article
-
- You have access
- Open access
- Export citation
The Brief Negative Symptom Scale: external validation of symptom domains with clinical, cognitive and functioning-related variables in subjects with schizophrenia
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S264-S265
-
- Article
-
- You have access
- Open access
- Export citation
Personalisation of the management of schizophrenia and other primary psychoses
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S45
-
- Article
-
- You have access
- Open access
- Export citation
Investigating the prevalence of mental disorders and related risk factors in refugees and asylum seekers in Campania
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S282-S283
-
- Article
-
- You have access
- Open access
- Export citation
The structure stability of negative symptoms: longitudinal network analysis of the Brief Negative Symptom Scale in subjects with schizophrenia
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S259-S260
-
- Article
-
- You have access
- Open access
- Export citation
Implementing alternatives to coercion as a key component of improving mental health care: the WPA contribution
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S29
-
- Article
-
- You have access
- Open access
- Export citation
Long-term efficacy and safety of paliperidone 6-month formulation: An open-label extension of a double-blind study in adult patients with schizophrenia
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S136
-
- Article
-
- You have access
- Open access
- Export citation
Association between cognitive deficits and negative symptoms: a systematic review of the literature
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1046-S1047
-
- Article
-
- You have access
- Open access
- Export citation
Cognitive impairment after post-acute COVID-19 infection: a systematic review of the literature
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S121-S122
-
- Article
-
- You have access
- Open access
- Export citation
High number of refugees in Italy - which strategy works in Italy?
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S30
-
- Article
-
- You have access
- Open access
- Export citation
Implementing Alternatives to Coercion in Mental Health Care
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S1
-
- Article
-
- You have access
- Open access
- Export citation
Network Analyses: Understanding the Pathways of Functional Improvement in Schizophrenia
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S32-S33
-
- Article
-
- You have access
- Open access
- Export citation
Gender differences in clinical and psychosocial features in a large sample of Italian patients with schizophrenia
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S796
-
- Article
-
- You have access
- Open access
- Export citation
Recognition and Assessment of Cognitive Impairment in Schizophrenia
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S48
-
- Article
-
- You have access
- Open access
- Export citation
Effectiveness of social skills training conducted in a group of subjects with first-episode psychosis
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S505
-
- Article
-
- You have access
- Open access
- Export citation
Resting-state functional connectivity of the ventral tegmental area and negative symptom domains in subjects with schizophrenia
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, pp. S542-S543
-
- Article
-
- You have access
- Open access
- Export citation
Investigation of electrophysiological markers to predict clinical and functional outcome of schizophrenia using sparse partial least square regression
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S542
-
- Article
-
- You have access
- Open access
- Export citation
Predictors of real-life functioning in subjects with schizophrenia: A 4-year follow-up study
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S40
-
- Article
-
- You have access
- Open access
- Export citation
Prediction of drop-out and functional impairment in recent-onset schizophrenia spectrum disorders
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, pp. S35-S36
-
- Article
-
- You have access
- Open access
- Export citation