25 results
Research agenda for antibiotic stewardship within the Veterans’ Health Administration, 2024–2028
-
- Journal:
- Infection Control & Hospital Epidemiology , First View
- Published online by Cambridge University Press:
- 02 February 2024, pp. 1-7
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
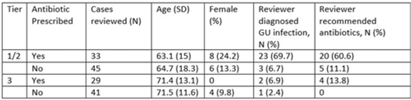
Validation of antibiotic stewardship metrics for genitourinary infection management in Veterans Affairs outpatient settings
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, p. s35
-
- Article
-
- You have access
- Open access
- Export citation
A qualitative evaluation of frontline clinician perspectives toward antibiotic stewardship programs
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 12 / December 2023
- Published online by Cambridge University Press:
- 29 March 2023, pp. 1995-2001
- Print publication:
- December 2023
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Outpatient treatment and clinical outcomes of bacteriuria in veterans: A retrospective cohort analysis
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue 1 / 2022
- Published online by Cambridge University Press:
- 12 October 2022, e168
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Implementation and outcomes of a clinician-directed intervention to improve antibiotic prescribing for acute respiratory tract infections within the Veterans’ Affairs Healthcare System
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 5 / May 2023
- Published online by Cambridge University Press:
- 15 August 2022, pp. 746-754
- Print publication:
- May 2023
-
- Article
- Export citation
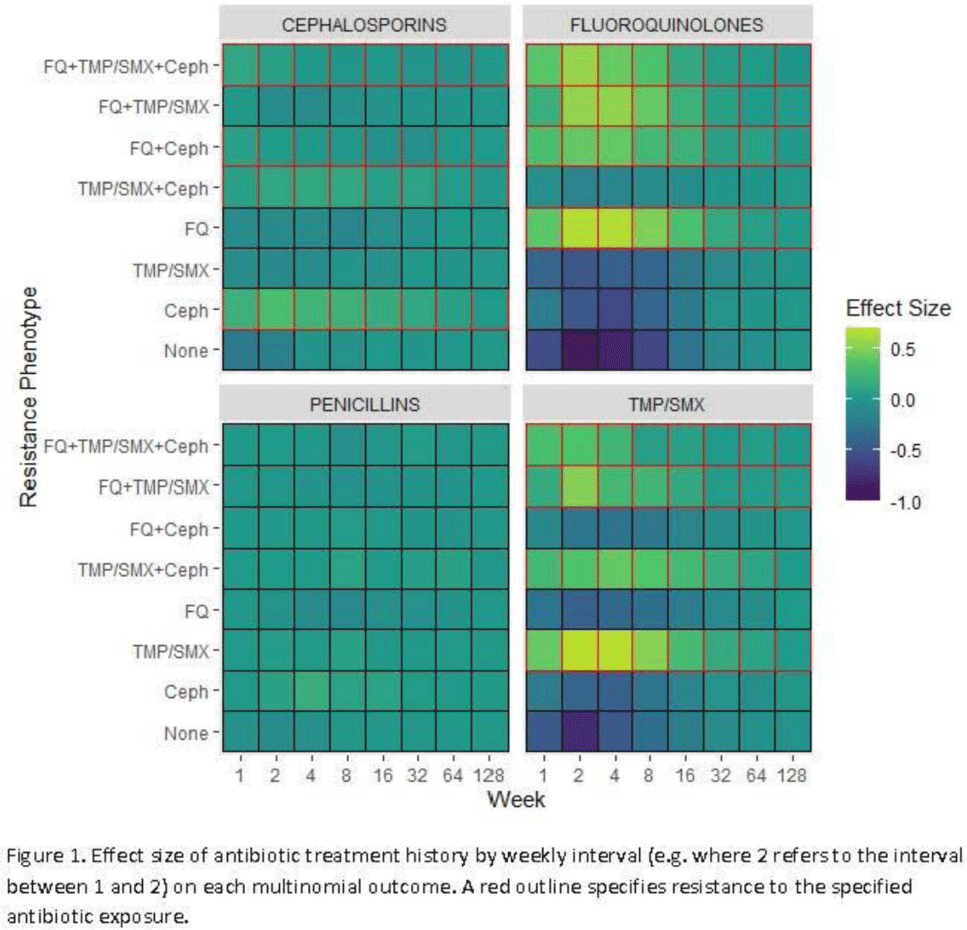
Using machine learning to predict antibiotic resistance to support optimal empiric treatment of urinary tract infections
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, p. s69
-
- Article
-
- You have access
- Open access
- Export citation
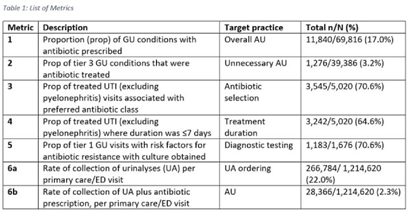
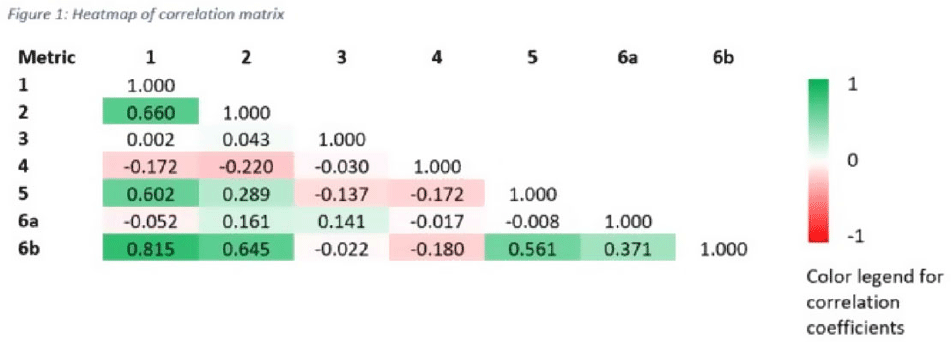
Tier-based antimicrobial stewardship metrics for genitourinary-related antibiotic use in Veterans’ Affairs outpatient settings
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, pp. s5-s6
-
- Article
-
- You have access
- Open access
- Export citation
Survey of physician and pharmacist steward perceptions of their antibiotic stewardship programs
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue 1 / 2021
- Published online by Cambridge University Press:
- 12 November 2021, e48
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
A Veterans’ Healthcare Administration (VHA) antibiotic stewardship intervention to improve outpatient antibiotic use for acute respiratory infections: A cost-effectiveness analysis
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 43 / Issue 10 / October 2022
- Published online by Cambridge University Press:
- 29 September 2021, pp. 1389-1395
- Print publication:
- October 2022
-
- Article
- Export citation
Increased Return Clinic Visits for Adults with Group A Streptococcal Pharyngitis Treated with a Macrolide
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s295-s296
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Novel Method to Evaluate Diagnostic Shifting After a Pediatric Antibiotic Stewardship Intervention
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s332-s333
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Update on Improving Outpatient Antibiotic Use Through Implementation and Evaluation of Core Elements of Outpatient Antibiotic
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, p. s422
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Association of Receipt of Antibiotics with Patient Satisfaction for Caregivers of Children Presenting to Urgent-Care Settings
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s134-s135
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
VA Antibiotic Stewardship Intervention to Improve Outpatient Antibiotic Use for ARIs: A Cost-Effectiveness Analysis
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, p. s55
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Evaluation of clinicians’ knowledge, attitudes, and planned behaviors related to an intervention to improve acute respiratory infection management
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue 6 / June 2020
- Published online by Cambridge University Press:
- 17 March 2020, pp. 672-679
- Print publication:
- June 2020
-
- Article
- Export citation
Evaluation of uncomplicated acute respiratory tract infection management in veterans: A national utilization review
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 40 / Issue 4 / April 2019
- Published online by Cambridge University Press:
- 11 April 2019, pp. 438-446
- Print publication:
- April 2019
-
- Article
- Export citation
Variation in Empiric Coverage Versus Detection of Methicillin-Resistant Staphylococcus aureus and Pseudomonas aeruginosa in Hospitalizations for Community-Onset Pneumonia Across 128 US Veterans Affairs Medical Centers
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 38 / Issue 8 / August 2017
- Published online by Cambridge University Press:
- 21 June 2017, pp. 937-944
- Print publication:
- August 2017
-
- Article
- Export citation
A Report of the Efforts of the Veterans Health Administration National Antimicrobial Stewardship Initiative
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 38 / Issue 5 / May 2017
- Published online by Cambridge University Press:
- 25 January 2017, pp. 513-520
- Print publication:
- May 2017
-
- Article
-
- You have access
- HTML
- Export citation
Characteristics of Antimicrobial Stewardship Programs at Veterans Affairs Hospitals: Results of a Nationwide Survey
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 37 / Issue 6 / June 2016
- Published online by Cambridge University Press:
- 24 February 2016, pp. 647-654
- Print publication:
- June 2016
-
- Article
- Export citation
152 - Streptococcus groups A, B, C, D, and G
- from Part XVIII - Specific organisms: bacteria
-
-
- Book:
- Clinical Infectious Disease
- Published online:
- 05 April 2015
- Print publication:
- 23 April 2015, pp 991-996
-
- Chapter
- Export citation