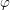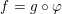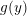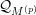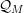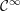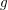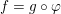Definition
Acute inflammation of the gallbladder. One-third of patients with biliary colic develop acute cholecystitis within two years.
Aetiology
90% of cases associated with obstruction of the cystic duct by a gallstone. Acalculous (absence of gallstones) cholecystitis occurs in 2–5% of cases and is associated with prolonged fasting, trauma (burns, fractures), severe illness, intensive care admission, parenteral nutrition (TPN) and AIDS.
Pathophysiology
Cystic duct obstruction with continued gallbladder secretions leads to an increase in pressure. Concomitant infection by intestinal organisms leads to gallbladder inflammation, diaphragmatic irritation. The stone often slips back into the gallbladder fundus allowing drainage and resolution of inflammation. Continued obstruction of the duct results in collection of mucus (mucocoele) and then pus in the gallbladder forming an empyema (pus-filled gallbladder). Subsequently ischaemia of the gallbladder wall may lead to infarction, necrosis, perforation and ultimately biliary peritonitis.
Acalculous cholecystitis often results from reduced gallbladder contraction due to decreased cholecystokinin release, with viscous bile thought to result in gallbladder obstruction and subsequent bacterial seeding. Cystic duct compression may also be caused by extrinsic compression (tumour, node, inflammatory mass).
Symptoms
Continuous RUQ and epigastric pain (in contrast to the fluctuating pain of biliary colic). Pain may radiate to back or to right scapula (due to peritoneal irritation via T7–9 dermatomes). Note that pain may be very similar to that of acute gastritis or peptic ulcer disease (PUD). Associated nausea, anorexia, fever and vomiting. May have known history of gallstones/ biliary colic.
Examination
Pyrexia, tachycardia, dehydration and possible tachypnoea with shallow respiration. Jaundice may result due to a common bile duct stone.