Persistent or recurrent symptoms are common features of the long-term course of depression and anxiety. Reference Judd, Akiskal, Maser, Zeller, Endicott, Coryell, Paulus, Kunovac, Leon, Mueller, Rice and Keller1,Reference Merikangas, Zhang, Avenevoli, Acharyya, Neuenschwander and Angst2 Maintenance therapy with antidepressants has been shown to prevent subsequent relapses of depressive episodes but this evidence is primarily based on randomised controlled trials of relatively short duration of up to 12 months; little is known about longer-term effects. Reference Geddes, Carney, Davies, Furukawa, Kupfer, Frank and Goodwin3 Furthermore, these trials often have strict inclusion criteria that exclude individuals with comorbid illnesses, with suicidal ideation and those who present primarily with somatic symptoms. Reference Leon, Solomon, Mueller, Endicott, Rice, Maser, Coryell and Keller4 Population-based samples, followed longitudinally, may be helpful in clarifying whether the short-term efficacy demonstrated in clinical trials extends to long-term effectiveness in the general population. The objective of the present study was to assess the long-term effect of antidepressant or anxiolytic use during an episode of mental disorder in mid-life, using a propensity score approach to account for non-random allocation to treatment. Reference Rosenbaum and Rubin5
Method
Participants
Participants were members of the Medical Research Council National Survey of Health and Development (NSHD). This is an ongoing longitudinal study of 5362 individuals who formed a stratified sample of babies born in England, Scotland or Wales during the week of 3–9 March, 1946. The sample has been prospectively studied on 21 occasions up to age 53 years. Comparisons with census data show that those remaining in the cohort (n=3673 at age 53) are broadly representative of all British-born adults currently resident in England, Scotland and Wales. Reference Wadsworth, Butterworth, Hardy, Kuh, Richards, Langenberg, Hilder and Connor6
The Psychiatric Symptom Frequency (PSF) scale, a questionnaire that records the frequency and intensity of common symptoms of anxiety and depression over the preceding year, Reference Lindelow, Hardy and Rodgers7 was administered at age 43 (n=3156). The participants used for this study were those who scored 30 or higher on the PSF, a cut-off that yields a prevalence of approximately 7% of the cohort at the time. We also report briefly on a second sample with subthreshold mental disorder, who scored between 23 and 29 on the PSF. Reference Paykel, Hayhurst, Abbott and Wadsworth8
Psychiatric treatment
Survey members reported prescription medication use to a nurse interviewer at age 43. This study describes outcomes associated with the use of anxiolytics (British National Formulary (BNF) Section 4.1.2) and antidepressants (BNF Section 4.3). 9
Outcomes of drug treatment
Primary outcome: mental disorder
The primary outcome was mental disorder at age 53 as measured by the 28-item General Health Questionnaire (GHQ), which focuses on self-reported symptoms of anxiety and depression, and associated psychosocial dysfunction, in the preceding 4 weeks. Reference Goldberg and Hillier10 The cut-off used for mental disorder was a score of 11 or higher (most severe 7%).
Secondary outcomes: associated psychiatric symptoms
A limited number of secondary outcomes were also considered. These included a broader definition of mental disorder encompassing sub-threshold symptoms (GHQ score of 7 or higher); self-reported sleeping difficulties; alcohol misuse based on the CAGE questionnaire; Reference Ewing11 and symptoms of psychosis based on four-items from a standard psychosis screening questionnaire. Reference Bebbington and Nayani12
Factors associated with treatment
Numerous factors were considered for possible associations with treatment with psychotropic medications during an episode of mental illness. Factors were also selected on the basis that they could be plausibly associated with prognosis of mental illness. In particular, we focused on factors associated with severity of symptoms and history of mental illness, since both symptom severity Reference Keller, Lavori, Mueller, Endicott, Coryell, Hirschfeld and Shea13,Reference Seivewright, Tyrer and Johnson14 and a history of symptoms Reference Seivewright, Tyrer and Johnson14,Reference Mueller, Leon, Keller, Solomon, Endicott, Coryell, Warshaw and Maser15 are associated with long-term prognosis in depression, and both factors are also associated with treatment during an episode of mental disorder. Reference Colman, Croudace, Wadsworth and Jones16
Current symptom severity
Survey members were considered to have severe symptoms if they scored 54 or higher on the PSF (top 15.8% of those with mental disorder); suicidal ideation if they reported during the PSF they had ‘thought about taking their own life’; sleep difficulties if they reported trouble sleeping; and alcohol misuse if they responded positively to two or more items on the CAGE screening questionnaire. Reference Ewing11
History of mental illness
Survey participants were considered to have mental disorder at age 36 if they scored five or higher on the Index of Definition for the Present State Examination in 1982. Reference Wing, Cooper and Sartorius17,Reference Wing, Mann, Leff and Nixon18 Treatment between age 16 and 36 was based on in- and out-patient hospital records and physician records. Reference Paykel, Watters, Abbott and Wadsworth19 Psychiatric hospitalisation up to age 43 was based on hospital records that included any admissions for mental disorder (ICD–9 codes 290–314, and ICD–10 codes F10–F69 and F90–F98) 20,21 or suicidal behaviour (ICD–9 codes E950–E959, and ICD–10 codes X6000–X8499). Finally, participants were asked at age 43 if they had ever suffered from ‘nervous trouble’.
Statistical analysis
Observational studies suffer from one crucial drawback in comparison with randomised controlled trials: individuals who receive treatment may differ, in clinical or social factors, from those who do not, and these differences may affect prognosis, thereby confounding any observed differences in outcome. Reference D'Agostino22 Naturalistic study designs must, therefore, be analysed using methods that can address these selection-to-treatment elements in order to estimate the actual impact of treatment that would have been generated by a randomised design.
One method that is now widely used for this purpose is the propensity score approach. Reference Rosenbaum and Rubin5 A propensity score is the probability of an individual being treated, calculated from a logistic regression in which all available variables likely to be associated with treatment are entered into a model predicting treatment. Reference D'Agostino22 Given that the objective is to balance as many covariates as possible that might be related to treatment or prognosis between the treated and untreated groups, it is desirable to include as many predictors as possible in the calculation of the propensity score. Reference D'Agostino22 Consequently, this study considered the eight variables described above.
If two individuals have the same probability of being treated (i.e. same propensity score), but one has been treated and the other has not, then it is as if they have been randomly assigned to treatment, assuming that no unmeasured confounders exist. Reference Rosenbaum and Rubin5,Reference D'Agostino22 If no differences exist between covariates within quintiles of the propensity score, then any overall differences in the covariates can be considered ‘ignorable’ as long as the analysis matches on the propensity score. Reference D'Agostino22 In other words, if all covariates are balanced between the treatment and non-treatment group after adjusting for the propensity score, then any observed differences between the groups should be attributable to the effects of treatment. This study used logistic regression to adjust for the propensity score in the analysis of the long-term effects of treatment with antidepressants or anxiolytics at age 43 on mental disorder at age 53, compared with those who received no pharmaceutical treatment. Reference D'Agostino22 Odds ratios of less than 1 indicate beneficial effects of treatment.
All calculations involving propensity scores used the program PSCORE for Stata 9.0.
Results
There were 204 individuals with mental disorder at age 43, a prevalence of 7.0%. Among these, 45 were using an antidepressant or anxiolytic (22.1%); 23 were using an antidepressant only, 17 were using an anxiolytic only, and 5 were using both. Of these, 157 were followed-up 10 years later at age 53 (77.0%). There was a trend to suggest that those lost to follow-up might have had more severe symptoms at age 43 (mean PSF=44.2 v. 40.7, P=0.07); however, those lost to follow-up were no more likely to be using antidepressants or anxiolytics than those with complete data at age 53 (25.5% v. 21.0%, P=0.43). The remaining analyses include those 157 with follow-up data at age 53.
Propensity-for-treatment with psychotropic medications
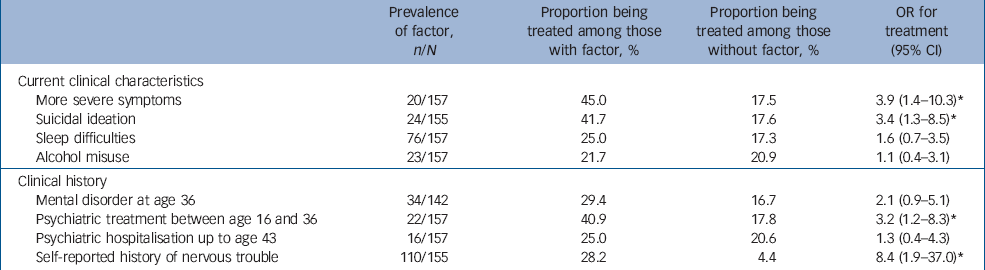
There were several differences between those treated with anxiolytics or antidepressants and those who were not (Table 1). In particular, those with a poorer mental state, including more severe symptoms and suicidal ideation, were more likely to be treated as were those with a history of mental disorder or psychiatric treatment.
Table 1 Associations between predictors and treatment with psychotropic medication for those with mental disorder at age 43
| Prevalence of factor, n/N | Proportion being treated among those with factor, % | Proportion being treated among those without factor, % | OR for treatment (95% CI) | |
|---|---|---|---|---|
| Current clinical characteristics | ||||
| More severe symptoms | 20/157 | 45.0 | 17.5 | 3.9 (1.4–10.3) * |
| Suicidal ideation | 24/155 | 41.7 | 17.6 | 3.4 (1.3–8.5) * |
| Sleep difficulties | 76/157 | 25.0 | 17.3 | 1.6 (0.7–3.5) |
| Alcohol misuse | 23/157 | 21.7 | 20.9 | 1.1 (0.4–3.1) |
| Clinical history | ||||
| Mental disorder at age 36 | 34/142 | 29.4 | 16.7 | 2.1 (0.9–5.1) |
| Psychiatric treatment between age 16 and 36 | 22/157 | 40.9 | 17.8 | 3.2 (1.2–8.3) * |
| Psychiatric hospitalisation up to age 43 | 16/157 | 25.0 | 20.6 | 1.3 (0.4–4.3) |
| Self-reported history of nervous trouble | 110/155 | 28.2 | 4.4 | 8.4 (1.9–37.0) * |
* P<0.05
All eight variables listed in Table 1 were included in a logistic regression model that calculated propensity-for-treatment (i.e. probability of treatment). This model included 140 of the 157 individuals; the 17 not included did not have complete data on all variables, but did not differ from those included with respect to mean PSF score (40.6 for those included, 41.8 for those not included, P=0.66) at age 43. This model explained 15% of the variance in likelihood of treatment, and balanced all predictive variables between those treated and those untreated within quintiles of the propensity score.
Outcome of treatment with medications
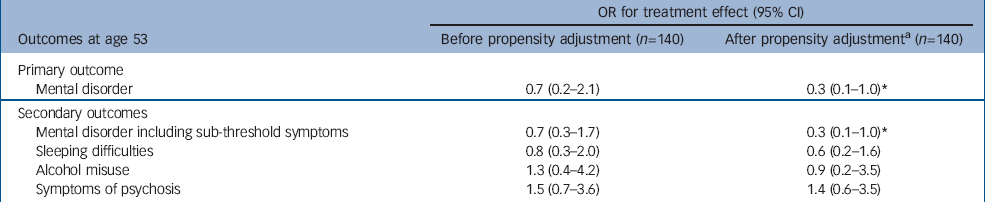
Before adjusting for propensity-for-treatment, those treated with psychotropic medications at age 43 were no more or less likely to have a mental disorder at age 53 than those not treated with medications (Table 2). The lack of effect was also similar across the secondary outcomes.
Table 2 Outcomes at age 53 for psychotropic medication use at age 43 among those with mental disorder
| OR for treatment effect (95% CI) | |||
|---|---|---|---|
| Outcomes at age 53 | Before propensity adjustment (n=140) | After propensity adjustment a (n=140) | |
| Primary outcome | |||
| Mental disorder | 0.7 (0.2–2.1) | 0.3 (0.1–1.0) * | |
| Secondary outcomes | |||
| Mental disorder including sub-threshold symptoms | 0.7 (0.3–1.7) | 0.3 (0.1–1.0) * | |
| Sleeping difficulties | 0.8 (0.3–2.0) | 0.6 (0.2–1.6) | |
| Alcohol misuse | 1.3 (0.4–4.2) | 0.9 (0.2–3.5) | |
| Symptoms of psychosis | 1.5 (0.7–3.6) | 1.4 (0.6–3.5) | |
a. See Table 1 for factors included in adjustment for propensity for treatment
* P<0.05
After adjusting for propensity-for-treatment, those treated with antidepressants or anxiolytics were significantly less likely to have mental disorder 10 years later (odds ratio (OR)=0.3, 95% CI 0.1–1.0). This relationship held when the definition of mental disorder was expanded to include sub-threshold symptoms at age 53 (Table 2). In addition, linear regression suggested that those treated with antidepressants or anxiolytics had, on average, a GHQ total score that was about three points lower (β=–3.0, 95% CI −6.3–0.2) than those not treated with medications.
Among those treated with antidepressants or anxiolytics at age 43, 24.2% were using one or both at age 53. In all cases, conclusions regarding effect of treatment on subsequent mental disorder were unchanged after adjusting for current medication use at the time of outcome assessment. Although statistical power to detect drug-specific differences was minimal, the likelihood of mental disorder was similar for antidepressants (OR=0.3, 95% CI 0.05–1.2) and anxiolytics (OR=0.2, 95% CI 0.02–1.7).
There were no significant effects of antidepressant or anxiolytic use at age 43 on sleeping difficulties, alcohol misuse or symptoms of psychosis at age 53.
Sub-threshold mental disorder
A separate analysis was performed on 156 individuals with subthreshold mental disorder at age 43 years and follow-up data at age 53. Among these, only 10 (6.4%) were using an antidepressant or anxiolytic. The same eight variables listed in Table 1 were used to calculate the propensity-for-treatment among these individuals. This second propensity model included 121 individuals and explained 17% of the variance in likelihood of treatment. Before adjusting for propensity-for-treatment, individuals who were treated with antidepressants or anxiolytics were more likely to have mental disorder 10 years later (OR=5.2, 95% CI 1.2–21.5). After adjusting for propensity-for-treatment, the likelihood of future mental disorder was similar, but was no longer statistically significant (OR=3.9, 95% CI 0.8–18.9).
Discussion
Findings and related research
Results from this study suggest that treatment with antidepressants or anxiolytics during an episode of mental disorder may have a long-term beneficial effect. Individuals with mental disorder were significantly less likely to have mental disorder 10 years later if they were using antidepressants or anxiolytics. These positive effects, however, were not apparent among individuals with less severe symptoms.
A particularly important predictor of prognosis may be the effectiveness of initial treatment. Pintor et al followed individuals for 2 years after treatment of depression and found that only 15% of those whose symptoms remitted completely during initial treatment had a relapse, while 68% of those who had partial relief of symptoms initially had a relapse during the follow-up period. Reference Pintor, Gasto, Navarro, Torres and Fananas23 This suggests that the mode of treatment delivered may be less important than the fact that an effective treatment is delivered at all, Reference Ellis and Smith24 which was supported in this study by the fact that individuals who were treated with antidepressants had similar outcomes to those treated with anxiolytics.
These results may appear to support systematic reviews showing that maintenance therapy with antidepressants helps prevent relapses of depressive episodes; Reference Geddes, Carney, Davies, Furukawa, Kupfer, Frank and Goodwin3 however, such preventive effects presume continuation of therapy. Given that less than a quarter of individuals who were using antidepressants or anxiolytics at age 43 were using them at age 53, it is unlikely the results of our study can be explained by long-term maintenance therapy. It appears more likely that the results can be explained by an initial willingness to be treated, potential successful initial treatment and an increased likelihood that these patients would seek and accept help when encountering symptoms of depression and anxiety in the future. Individuals who have been treated for mental disorder in the past are more likely to seek and receive treatment for current symptoms, Reference Mueller, Leon, Keller, Solomon, Endicott, Coryell, Warshaw and Maser15,Reference Colman, Wadsworth, Croudace and Jones25,Reference Burns, Eichenberger, Eich, Ajdacic-Gross, Angst and Rossler26 and are more likely to believe that medical interventions will be helpful for depression. Reference Jorm, Christensen, Medway, Korten, Jacomb and Rodgers27 Those who believe that antidepressants will be helpful are also more likely to use them. Reference Jorm, Medway, Christensen, Korten, Jacomb and Rodgers28
These findings are particularly interesting in the context of a World Health Organization study of outcomes of depression in primary care. Reference Simon, Goldberg, Tiemens and Ustun29 Results from that study suggested that mental health outcomes for help-seeking patients 12 months after their initial visit to a primary care physician were similar regardless of whether the patient's depressive symptoms were identified, implying that specific treatment had no long-term benefit. Those being treated in primary care may be comparable with those with sub-threshold symptoms in our study, and the lack of long-term effect we observed among this group may point to equivalent or similar initial short- or medium-term outcomes between those with less severe symptoms who are treated with antidepressants or anxiolytics and those who are not.
It is notable that long-term differences between those treated and those not treated were not apparent before accounting for propensity-for-treatment. Previous research has shown that individuals with more severe symptoms Reference Bebbington and Nayani12,Reference Keller, Lavori, Mueller, Endicott, Coryell, Hirschfeld and Shea13 and individuals with a history of mental illness Reference Keller, Lavori, Mueller, Endicott, Coryell, Hirschfeld and Shea13,Reference Seivewright, Tyrer and Johnson14 have a poorer long-term prognosis in depression and are more likely to have relapse episodes. As severity of symptoms and history of psychiatric illness are also associated with likelihood of treatment, Reference Mueller, Leon, Keller, Solomon, Endicott, Coryell, Warshaw and Maser15 they confound the observed relationship between treatment and outcome. Observational studies can be useful in the investigation of short- and long-term effects of psychotropic medications, but such other, related prognostic factors must be accounted for.
Methodological considerations
There are several limitations to this study. Most important is that although propensity scores balance all identified confounders of the treatment–outcome relationship, they do not balance unmeasured confounders in the way that is, theoretically, done with randomised controlled trials. Reference Rosenbaum and Rubin5,Reference D'Agostino22 The propensity-for-treatment model only accounted for 15% of the variance in likelihood of treatment; consequently, there must be unmeasured factors that influence treatment. However, this is only an important limitation if these unmeasured factors also influence prognosis. We were able to balance eight covariates between the treated and untreated groups, including important factors such as severity of symptoms and history of illness that are strongly associated with prognosis. Reference Bebbington and Nayani12–Reference Seivewright, Tyrer and Johnson14 Nevertheless, it is possible that unmeasured factors could explain the observed association between antidepressant and anxiolytic use and better long-term mental health. One such factor is neuroticism, which is associated with both help-seeking behaviour Reference Andrews, Issakidis and Carter30 and poorer prognosis for depression and anxiety. Reference Keller, Lavori, Mueller, Endicott, Coryell, Hirschfeld and Shea13 Since individuals who were neurotic were more likely to be in the treatment group, and more likely to have a poor outcome, the treatment effect observed in this study should be a conservative estimate without neuroticism included in the propensity model. Still, other unmeasured factors could have biased our results in the other direction, making the observed effects an over-estimation of the true effect.
Another limitation is that we have no data on what happened between the initial assessment and the outcome 10 years later. It is unknown for how long individuals continued their psychotropic medication use. In addition, it should be noted that the initial assessment was in 1989, when selective serotonin reuptake inhibitors were not as common as they are today, Reference Colman, Wadsworth, Croudace and Jones25 so the outcomes described may not be generalisable to currently prescribed medications.
A final limitation is missing data. There were 64 of 204 individuals who were excluded due to missing data on predictors of treatment or missing follow-up data. It is possible that these individuals were systematically different from those who remained in the study; in particular, those with more severe symptoms may have dropped out. Similarly, this sample was not large enough to consider a larger number of covariates that may influence the relationship between treatment and long-term outcome. Future studies, with greater statistical power, could include numerous other factors that may vary between those who are treated with psychotropic medications and those who are not such as socio-demographic or personality characteristics.
These limitations, however, are offset by some notable strengths. The sample was population-based, and the follow-up period is much longer than any comparable outcome studies of antidepressants and anxiolytics. Given the continuing under-treatment of depression in Britain and elsewhere, Reference Colman, Wadsworth, Croudace and Jones25,Reference Simon, Fleck, Lucas and Bushnell31 the long-term effects demonstrated in this study may have considerable implications for public health policy.
Acknowledgements
The authors are grateful for funding from the Institute for Social Studies in Medical Care (I.C.), the Medical Research Council (M.E.J.W., D.K.), the Stanley Medical Research Institute (P.B.J.), the National Institute of Health Research (P.B.J.), and the Leverhulme Foundation (T.J.C.). T.J.C. is funded by a Public Health Career Scientist Award from the UK Department of Health. We would also like to thank Dr James Kirkbride for reviewing an earlier draft of this manuscript.







eLetters
No eLetters have been published for this article.