Effective coordination of resources for those who have recurrent mental illness is often lacking, particularly in highly pressured services. Intensive case management (ICM) in its different forms has been adopted as an alternative model for maintaining patient support and encouraging social adaptability in patients suffering from recurrent psychotic disorders. Several studies, including recently conducted meta-analyses, have demonstrated its advantages over standard treatments for psychosis but have also outlined its weaknesses (Reference Muijen, Marks and ConnollyMuijen et al, 1992; Reference Marshall and LockwoodMarshall & Lockwood, 1998; Reference Marshall, Gray and LockwoodMarshall et al, 2000; UK700 Group, 1999b , 2000).
Reported health service costs for ICM compared to standard case management (SCM) vary widely, from reductions of up to 55% (Reference Quinlivan, Hough and CrowellQuinlivan et al, 1995) to increases of 325% (Reference Chandler, Meisel and McGowenChandler et al, 1996) although data on the total cost of care or care packages are limited. It is therefore unclear whether ICM is a necessary requirement of effective mental health provision for the group of patients with severe mental illness as a whole. In the light of such diverse findings other factors must also be explored further, including the specific patient profiles that may benefit from such an approach.
Severe mental illness is associated with low premorbid IQ and negative symptoms (Reference Tamminga, Buchanan and GoldTamminga et al, 1998; Reference BreierBreier, 1999) and IQ is a significant factor in both the onset and course of psychotic disorders. Often people with dual diagnosis of mild ‘mental retardation’ or borderline intellectual functioning and severe mental disorders are excluded from studies of course and outcome in the general population. Therefore, there is little research on interventions that are effective for this group of patients, who are not only prone to the same disorders as adults without learning disabilities, but more often than not come to the attention of generic mental health services.
Published research on outcome in this population mostly concentrates on the evaluation of interventions for challenging behaviour, which is a separate condition from mental illness (Reference Maguire and PierselMaguire & Piersel, 1992; Reference Lowe, Felce and BlackmanLowe et al, 1996). In addition, although similar terms are used to describe the practice of intensive support to vulnerable individuals with complex needs and dual diagnosis, it is in the main differently set up and has a more varied health focus than equivalent mental health models.
Patients with recurrent psychosis and low premorbid IQ are a highly relevant subgroup to study with respect to the benefits of ICM. These patients would traditionally be managed within a hospital care framework although, recently, community-directed interventions have begun to attract increasing attention. We reported earlier (Reference Hassiotis, Ukoumunne and TyrerHassiotis et al, 1999) on the prevalence and characteristics of patients with psychotic illness and borderline IQ. In this paper we present the findings of the 2-year follow-up of that cohort of patients who were randomly allocated to the two arms of the study, ICM and SCM.
METHOD
Hypotheses
The aims of this substudy were not part of the main objectives of the UK700 trial but they were specified in advance of the trial. The first hypothesis examined was that patients with borderline IQ and psychosis would make greater use of hospital services, incur greater service costs and have greater psychopathology than patients of normal IQ. The second hypothesis was that the benefits of receiving ICM would be significantly greater for patients of borderline IQ with severe mental illness than for those of normal IQ.
Study design and outcome measures
The UK700 study was a randomised controlled trial which compared the efficacy of ICM to SCM in patients with severe psychosis. The rationale and detailed methodology of the UK700 study are reported elsewhere (UK700 Group, 1999a , b ). Seven hundred and eight patients with psychosis from four centres in the UK (Manchester Royal Infirmary, and London's St Charles' and St Mary's Hospitals, St George's Hospital and the Maudsley Hospital) were allocated to either SCM (caseload 1:30-35) or ICM (caseload 1:10-15) between February 1994 and April 1996 and followed up for 2 years. The patients interviewed and recruited into the study were selected at the point of discharge from hospital or from out-patient registers.
At baseline, the Operational Criteria Checklist for Psychotic Illness (OPCRIT; Reference McGuffin, Farmer and HarveyMcGuffin et al, 1991) was used to derive diagnoses and the National Adult Reading Test (NART; Nelson et al, 1982) was performed to measure premorbid IQ. The NART error score (range 0-50) was used to identify patients according to IQ status, with those scoring 40 and above classified as being of borderline IQ (Reference Hassiotis, Ukoumunne and TyrerHassiotis et al, 1999).
The primary outcome of the study was the number of days spent in hospital for psychiatric reasons over 2 years. The number of hospital admissions was also recorded. Resource-use data were collected prospectively for each patient during the 2-year study period. The perspective taken was that of all providing sectors in society, including health services, social services, voluntary and private agencies. Information was also recorded on the use of staffed accommodation, prison and police custody. All unit costs were for the financial year 1997-1998 and future costs were discounted at a rate of 6% (UK700 Group, 2000).
Clinical assessments were carried out at baseline, 1 year and 2 years after randomisation. These included the Comprehensive Psychopathological Rating Scale (CPRS: Reference Åsberg, Perris and SchallingÅsberg et al, 1978), the Scale for the Assessment of Negative Symptoms (SANS: Reference AndreasenAndreasen, 1989), the Abnormal Involuntary Movement Scale (AIMS: Reference GuyGuy, 1976) and the Disability Assessment Schedule (DAS: Reference Jablensky, Schwartz and TomovJablensky et al, 1980), which was used to rate the level of social disability. Sub-scales for anxiety (Reference Tyrer, Owen and CicchettiTyrer et al, 1984), depression (Reference Montgomery and ÅsbergMontgomery & Åsberg, 1979) and psychotic symptoms were derived from the CPRS. Other measures rated the number of met and unmet needs reported by patients (Camberwell Assessment of Need, CAN; Reference Phelan, Slade and ThornicroftPhelan et al, 1995), quality of life (Lancashire Quality of Life Profile: Reference Oliver, Huxley and PriebeOliver, 1991) and satisfaction with mental health services (Reference Tyrer and RemingtonTyrer & Remington, 1979). High scores on the satisfaction scale indicate low levels of satisfaction. Additionally, contact between subject and case manager was recorded and whether patients spent any time in prison or suffered adverse events, such as death before the end of the study.
Statistical analysis
Hospitalisation and costs incurred over 2 years and clinical outcome scores at the 2-year follow-up were analysed in this study. Analyses of differences between the borderline- and normal-IQ patients were implemented using the t-test for continuous data and the χ2 test for dichotomous data. Potential differential benefits of ICM for the two sets of patients were investigated using tests of interaction. Regression analyses were used to implement the interaction tests, with the t-test or the χ2 test used to compare ICM to SCM within each of the IQ groups. All analyses were adjusted for centre, ethnicity and social disability at baseline. Analyses of the clinical outcomes were also adjusted for the corresponding baseline scores. Because the adjusted analyses generally yielded similar results to the unadjusted, the latter are presented in the tables, although salient differences between adjusted and unadjusted analyses are noted and commented on in the Results section. Bootstrap methods (Reference Efron and TibshiraniEfron & Tibshirani, 1993) were used to check the validity of the findings when analysing heavily skewed continuous outcomes such as the hospitalisation and cost-of-care variables. The bootstrap allows parametric statistics to be applied correctly to skewed data. As there were no marked differences from the bootstrap results, the t-test and ordinary least squares regression results are reported in the tables.
In order to validate significant findings in analyses for which there are notable differences across subgroups in the proportions of missing values on the outcome, regression models were used to impute outcome values. Ethnicity, disability status and the baseline score on the outcome, where available, were used as predictors. Analyses of the imputed variables provided essentially the same findings as the main analyses and therefore results from the latter are presented.
RESULTS
Of 586 patients who took the NART test, 104 (17.7%) were classified as having borderline IQ. Fifty-four of these were randomised to the SCM and 50 to the ICM arms of the trial. Of the 482 normal-IQ patients, 245 and 237 were allocated to the two arms of the study, respectively. Of the participants who completed the NART test at baseline, the percentage of missing values on the outcome analysed ranged between 4% and 34% for normal-IQ subjects in the SCM arm, between 4% and 24% for normal-IQ subjects in the ICM arm, between 2% and 26% for borderline-IQ subjects in the standard arm and between 6% and 32% for borderline-IQ subjects in the ICM arm. The percentages of missing values on the hospitalisation and costs outcome were no greater than 6% in each subgroup. Notable differences in percentages of missing data were apparent only for clinical assessments.
Comparison of outcome between borderline- and normal-IQ patients
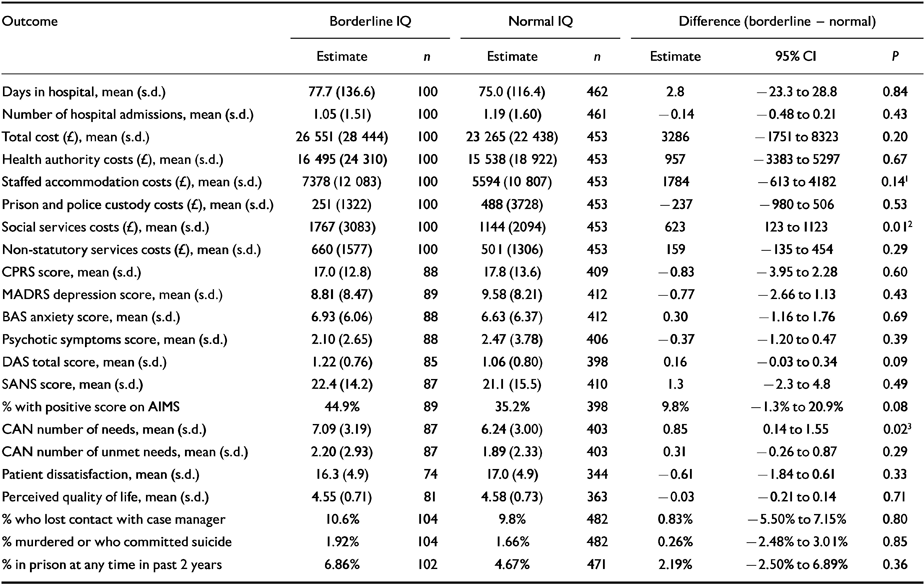
Results of the unadjusted analyses are presented in Table 1. There were no significant differences between the borderline- and normal-IQ patients with regard to hospital use and total costs over the study period. The mean number of days spent in hospital was similar between the borderline- and normal-IQ patients (77.7 v. 75.0 respectively; P=0.84) as was mean total cost of care over 2 years (£26 551 v. £23 265, P=0.20). The non-significant difference between borderline- and normal-IQ patients with respect to mean cost of staffed accommodation became significant after adjustment (adjusted means £7960 v. £ 5508 respectively, P=0.05), showing the border-line patients incurring greater costs in this sector. In contrast, the significant difference in the costs of social services became non-significant after adjustment (adjusted means £1646 in borderline v. £1211 in the normal group; P=0.09).
Table 1 Outcome results by IQ status
| Outcome | Borderline IQ | Normal IQ | Difference (borderline - normal) | ||||
|---|---|---|---|---|---|---|---|
| Estimate | n | Estimate | n | Estimate | 95% CI | P | |
| Days in hospital, mean (s.d.) | 77.7 (136.6) | 100 | 75.0 (116.4) | 462 | 2.8 | -23.3 to 28.8 | 0.84 |
| Number of hospital admissions, mean (s.d.) | 1.05 (1.51) | 100 | 1.19 (1.60) | 461 | -0.14 | -0.48 to 0.21 | 0.43 |
| Total cost (£), mean (s.d.) | 26 551 (28 444) | 100 | 23 265 (22 438) | 453 | 3286 | -1751 to 8323 | 0.20 |
| Health authority costs (£), mean (s.d.) | 16 495 (24 310) | 100 | 15 538 (18 922) | 453 | 957 | -3383 to 5297 | 0.67 |
| Staffed accommodation costs (£), mean (s.d.) | 7378 (12 083) | 100 | 5594 (10 807) | 453 | 1784 | -613 to 4182 | 0.141 |
| Prison and police custody costs (£), mean (s.d.) | 251 (1322) | 100 | 488 (3728) | 453 | -237 | -980 to 506 | 0.53 |
| Social services costs (£), mean (s.d.) | 1767 (3083) | 100 | 1144 (2094) | 453 | 623 | 123 to 1123 | 0.012 |
| Non-statutory services costs (£), mean (s.d.) | 660 (1577) | 100 | 501 (1306) | 453 | 159 | -135 to 454 | 0.29 |
| CPRS score, mean (s.d.) | 17.0 (12.8) | 88 | 17.8 (13.6) | 409 | -0.83 | -3.95 to 2.28 | 0.60 |
| MADRS depression score, mean (s.d.) | 8.81 (8.47) | 89 | 9.58 (8.21) | 412 | -0.77 | -2.66 to 1.13 | 0.43 |
| BAS anxiety score, mean (s.d.) | 6.93 (6.06) | 88 | 6.63 (6.37) | 412 | 0.30 | -1.16 to 1.76 | 0.69 |
| Psychotic symptoms score, mean (s.d.) | 2.10 (2.65) | 88 | 2.47 (3.78) | 406 | -0.37 | -1.20 to 0.47 | 0.39 |
| DAS total score, mean (s.d.) | 1.22 (0.76) | 85 | 1.06 (0.80) | 398 | 0.16 | -0.03 to 0.34 | 0.09 |
| SANS score, mean (s.d.) | 22.4 (14.2) | 87 | 21.1 (15.5) | 410 | 1.3 | -2.3 to 4.8 | 0.49 |
| % with positive score on AIMS | 44.9% | 89 | 35.2% | 398 | 9.8% | -1.3% to 20.9% | 0.08 |
| CAN number of needs, mean (s.d.) | 7.09 (3.19) | 87 | 6.24 (3.00) | 403 | 0.85 | 0.14 to 1.55 | 0.023 |
| CAN number of unmet needs, mean (s.d.) | 2.20 (2.93) | 87 | 1.89 (2.33) | 403 | 0.31 | -0.26 to 0.87 | 0.29 |
| Patient dissatisfaction, mean (s.d.) | 16.3 (4.9) | 74 | 17.0 (4.9) | 344 | -0.61 | -1.84 to 0.61 | 0.33 |
| Perceived quality of life, mean (s.d.) | 4.55 (0.71) | 81 | 4.58 (0.73) | 363 | -0.03 | -0.21 to 0.14 | 0.71 |
| % who lost contact with case manager | 10.6% | 104 | 9.8% | 482 | 0.83% | -5.50% to 7.15% | 0.80 |
| % murdered or who committed suicide | 1.92% | 104 | 1.66% | 482 | 0.26% | -2.48% to 3.01% | 0.85 |
| % in prison at any time in past 2 years | 6.86% | 102 | 4.67% | 471 | 2.19% | -2.50% to 6.89% | 0.36 |
There were no significant differences between borderline- and normal-IQ patients on the clinical outcome measures after adjustment. The significant difference between borderline and normal patients for the total number of needs became non-significant after adjustment (adjusted means 6.9 v. 6.3 respectively, P=0.10).
Eleven (10.6%) patients in the borderline-IQ group and 47 (9.8%) in the normal-IQ group lost contact with their case managers during the study period, two (1.9%) patients in the borderline group and eight (1.7%) in the normal group died (suicide 7, murder 1) and seven (6.9%) of the borderline group and 22 (4.7%) of the normal group spent time in prison. There were no significant differences between the IQ groups for these variables.
Effects of interaction between case management status and IQ status
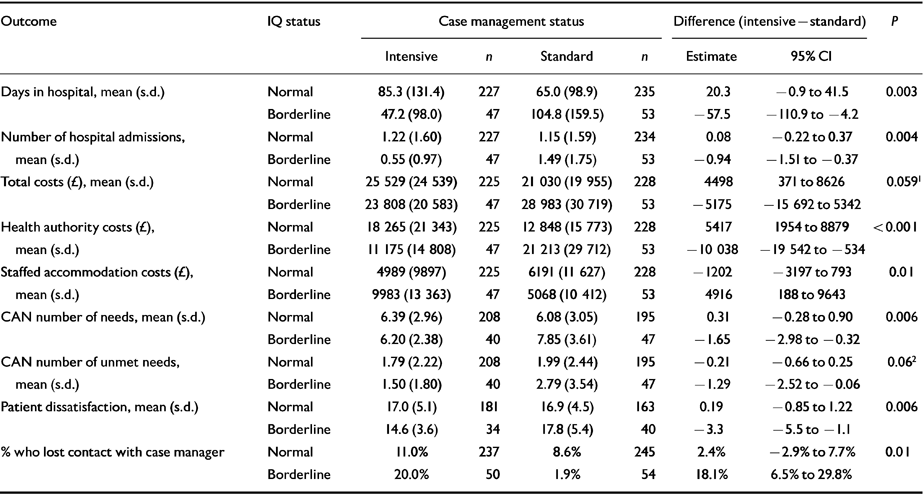
Results of unadjusted tests of interaction effect between case management status and IQ status on outcome are presented in Table 2. Only outcomes that were significant in the adjusted analyses are shown in this table. There was a significant interaction for the primary outcome, number of days in hospital for psychiatric reasons. Patients with borderline IQ and psychosis in the ICM arm spent significantly less time in hospital than their counterparts in the SCM arm (means 47.2 v. 104.8 days, respectively). This contrasts with the corresponding finding among normal-IQ patients. There was also a significant interaction for the number of hospital admissions, with ICM proving to be significantly more successful in reducing admissions than SCM for subjects of borderline IQ (means 0.55 v. 1.49, respectively).
Table 2 Outcome results by IQ status and standard v. intensive case management status
| Outcome | IQ status | Case management status | Difference (intensive—standard) | P | ||||
|---|---|---|---|---|---|---|---|---|
| Intensive | n | Standard | n | Estimate | 95% CI | |||
| Days in hospital, mean (s.d.) | Normal | 85.3 (131.4) | 227 | 65.0 (98.9) | 235 | 20.3 | -0.9 to 41.5 | 0.003 |
| Borderline | 47.2 (98.0) | 47 | 104.8 (159.5) | 53 | -57.5 | -110.9 to ‒4.2 | ||
| Number of hospital admissions, | Normal | 1.22 (1.60) | 227 | 1.15 (1.59) | 234 | 0.08 | -0.22 to 0.37 | 0.004 |
| mean (s.d.) | Borderline | 0.55 (0.97) | 47 | 1.49 (1.75) | 53 | -0.94 | -1.51 to ‒0.37 | |
| Total costs (£), mean (s.d.) | Normal | 25 529 (24 539) | 225 | 21 030 (19 955) | 228 | 4498 | 371 to 8626 | 0.0591 |
| Borderline | 23 808 (20 583) | 47 | 28 983 (30 719) | 53 | -5175 | -15 692 to 5342 | ||
| Health authority costs (£), | Normal | 18 265 (21 343) | 225 | 12 848 (15 773) | 228 | 5417 | 1954 to 8879 | <0.001 |
| mean (s.d.) | Borderline | 11 175 (14 808) | 47 | 21 213 (29 712) | 53 | -10 038 | -19 542 to ‒534 | |
| Staffed accommodation costs (£), | Normal | 4989 (9897) | 225 | 6191 (11 627) | 228 | -1202 | -3197 to 793 | 0.01 |
| mean (s.d.) | Borderline | 9983 (13 363) | 47 | 5068 (10 412) | 53 | 4916 | 188 to 9643 | |
| CAN number of needs, mean (s.d.) | Normal | 6.39 (2.96) | 208 | 6.08 (3.05) | 195 | 0.31 | -0.28 to 0.90 | 0.006 |
| Borderline | 6.20 (2.38) | 40 | 7.85 (3.61) | 47 | -1.65 | -2.98 to ‒0.32 | ||
| CAN number of unmet needs, | Normal | 1.79 (2.22) | 208 | 1.99 (2.44) | 195 | -0.21 | -0.66 to 0.25 | 0.062 |
| mean (s.d.) | Borderline | 1.50 (1.80) | 40 | 2.79 (3.54) | 47 | -1.29 | -2.52 to ‒0.06 | |
| Patient dissatisfaction, mean (s.d.) | Normal | 17.0 (5.1) | 181 | 16.9 (4.5) | 163 | 0.19 | -0.85 to 1.22 | 0.006 |
| Borderline | 14.6 (3.6) | 34 | 17.8 (5.4) | 40 | -3.3 | -5.5 to ‒1.1 | ||
| % who lost contact with case manager | Normal | 11.0% | 237 | 8.6% | 245 | 2.4% | -2.9% to 7.7% | 0.01 |
| Borderline | 20.0% | 50 | 1.9% | 54 | 18.1% | 6.5% to 29.8% | ||
The non-significant interaction for the total costs variable (P=0.06) became significant after adjustment (P=0.05). As Table 2 shows, ICM compared to SCM has the effect of reducing the total costs of care among borderline-IQ patients (means £23 808 v. £28 983, respectively). This contrasts with the effect it has of increasing the total costs for the normal-IQ subgroup. Interaction analyses by sector revealed significant effects on costs to the health sector and costs of staffed accommodation. ICM compared to SCM significantly reduced the cost of health services (means £ 11 175 v. £21 213, respectively) and significantly increased the cost of staffed accommodation (means £9983 v. £ 5068, respectively) for patients of borderline IQ. There were no significant interaction effects for the other sectors.
There were no significant interaction effects on the clinical outcomes. There were, however, significant interaction effects such that borderline-IQ patients in the intensive arm compared to their counterparts in the standard arm had fewer total needs (means 6.20 v. 7.85 respectively), fewer unmet needs (adjusted means 1.53 v. 2.88) and reported greater levels of satisfaction (means 14.6 v. 17.8). Finally, borderline patients in the intensive arms were significantly more likely to lose contact with their case manager than those in the standard arm (20.0% v. 1.9%, respectively).
DISCUSSION
Impact of IQ on outcome
There were no marked differences in long-term outcome between patients of borderline IQ and those of normal IQ, a finding that does not support our first hypothesis. We believe that the recruitment of the more severely ill and disabled patients, who are likely to face a range of long-term deficits associated with severe mental illness, may explain this finding. The results do, however, support our second hypothesis, that patients with recurrent psychosis and low premorbid IQ would benefit from intensive contact with mental health professionals.
The subgroup analyses in this study reveal that ICM did significantly reduce admissions and duration of hospitalisation for patients of borderline IQ with psychosis. Hospital admissions disrupt the social and domestic life of all patients, but for patients of borderline IQ or mild learning disability, this disruption is worsened by inherent impairments such as inflexibility and inability to tolerate stress. ICM can be seen as a more appropriate alternative to in-patient care of a highly vulnerable group of individuals.
Social functioning and ICM
Although there were no significant differences in clinical outcomes between patients with borderline and normal IQ, borderline patients in the ICM arm reported fewer met and unmet needs and increased satisfaction compared to borderline patients in the SCM arm. This is not surprising given that the ICM group were more likely to remain in their home environment with continuous, intensive community support. Patients were encouraged to be more involved in activities of daily living while receiving sufficient help to maintain motivation and social networks. Although ICM can go some way towards addressing unmet need and improve social support (Reference Thornicroft, Wykes and HollowayThornicroft et al, 1998), its multi-dimensional focus may fail to increase social functioning because managers are directly involved in meeting patients' needs (Reference Wykes, Leese and TaylorWykes et al, 1998). It is also likely that patients of borderline IQ with severe mental illness may under ICM be contained in the community without making significant gains in adaptive functioning.
Contact with case managers
The significant difference in loss of contact with the case managers between the borderline-IQ patients receiving ICM and those receiving SCM at first appears surprising and counter-intuitive. One would expect case managers who are working closely with patients to be more likely to retain contact with them. Further analyses did not reveal any notable differences in the reasons for this loss of contact. Of the 10 borderline patients receiving ICM, five moved from the catchment area or to another country, one could not be contacted, one was admitted to a secure hospital, one refused intensive support, one went to prison and one wished to continue with a community psychiatric nurse. The one borderline patient who lost contact in the standard arm of the trial moved from the catchment area. There were also no differences in reason for loss of contact between the borderline- and normal-IQ patients. Moving out of the catchment area or to another country was cited as the most common reason in both (45% (5/11) borderline, 40% (19/47) normal).
Cost and case management
Adjusted analyses found a statistically significant advantage for the borderline-IQ group in receipt of ICM compared to those receiving SCM in terms of total cost. Given the significant gains in outcome and lower costs, the results of this study strongly suggest that ICM is a more cost-effective method of care than SCM for this patient group. Evaluating costs by sector demonstrates that health authorities carry the burden of treatment costs compared to other sectors, which is in accord with recent studies of service utilisation in schizophrenia showing that in-patient care accounts for the majority of expenditure (Reference Lang, Forbes and MurrayLang et al, 1997). For the borderline-IQ group receiving ICM, significant cost savings for the health sector were found alongside significant increases in the total cost of staffed accommodation relative to borderline patients receiving SCM. These results reflect a reduced reliance on hospitalisation and corresponding increase in the level of supported community living in the borderline group receiving ICM.
Few studies have directly examined the cost of alternative interventions for people with mild learning disability or of borderline IQ with psychosis (dual diagnosis). A Dutch randomised controlled trial of out-reach v. in-patient treatment failed to show significant difference in clinical outcomes between the two groups (Reference van Minnen, Hoogduin and Broekmanvan Minnen et al, 1997). However, the study demonstrated a 40% reduction in the costs of outreach treatment. Despite the short follow-up period of 28 weeks, it is the only evidence to date of a cost-effective and acceptable alternative to hospital treatment.
Dual diagnosis and service utilisation
It is well established that individuals with mild learning disability or of borderline IQ are more susceptible to the development of mental illness. However, their use of mental health services appears to lag behind that of the normal-IQ population with psychiatric problems (Reference GustafssonGustafsson, 1997). Intellectual impairment may influence patterns of referral to and utilisation of mental health services (Reference Driessen, DuMoulin and HavemanDriessen et al, 1997). Such individuals may be transferred between adult mental health and specialist learning-disability services in the absence of management protocols for effective evaluation and treatment. Indeed, patients can often be caught between inadequately resourced health providers and social services who do not appreciate the subtleties of the coexistence of mental illness and learning disability in this population.
The multidimensional and intensive focus of ICM appears to be more suited to the complex needs of patients of low premorbid IQ with psychosis. However, we caution that these findings come from a subgroup analysis (albeit a planned one) of a trial which showed that ICM does not have a significant impact on clinical outcome and costs of care of patients with psychosis. Subgroup analyses of this kind are prone to obtaining positive results when there is in fact no real difference between groups. Therefore, the significant effect of the present study needs to be confirmed by further research.
This ‘hidden’ group of patients requires more systematic study across specialities in order to establish its needs and status. This task would be best achieved by an interagency approach to management in order to delineate suitable practice parameters for expert service delivery.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ The study provides evidence to suggest that patients of borderline IQ with psychosis respond better to intensive support than do patients of normal IQ.
-
▪ Intensive case management (ICM) appears to lower the duration and frequency of hospital admissions for patients with psychosis and of borderline IQ or with mild learning disability. Patients show more satisfaction with services and report fewer needs.
-
▪ Improvements in outcome and lower total costs of care suggest that ICM may be a more cost-effective method of treatment than standard case management (SCM) for this patient group.
LIMITATIONS
-
▪ ICM does not appear to increase social functioning or improve the clinical symptoms of patients of borderline IQ with psychosis, compared with those of normal IQ.
-
▪ Local service arrangements and perception of learning disability may limit the generalisation of our findings.
-
▪ The sample size for the main UK700 study was calculated to detect differences between ICM and SCM overall but not specifically to detect differences within the borderline- and normal-IQ subgroups. The findings need to be confirmed by further research.
ACKNOWLEDGEMENTS
The study was funded by an additional grant from the Department of Health Research and Development Programme to P. Tyrer, J. Piachaud and A. Hassiotis. There was no conflict of interest. The UK700 Group is a collaborative study team involving four clinical centres: Manchester Royal Infirmary: Tom Butler, Francis Creed, Janelle Fraser, Richard Gater, Peter Huxley, Nicholas Tarrier and Theresa Tattan; King's Hospital / Maudsley Hospital, London: Thomas Fahy, Catherine Gilvarry, Kwame McKenzie, Robin Murray, Jim Van Os and Elizabeth Walsh; St Mary's Hospital/St Charles Hospital, London: John Green, Anna Higgit, Elizabeth van Horn, Catherine Manley, Patricia Thornton, Peter Tyrer and, for the present project, Angela Hassiotis, Emma Roberts and Obioha Ukoumunne; St George's Hospital, London: Robert Bale, Tom Burns, Matthew Fiander, Kate Harvey, Andy Kent and Chiara Samele; Centre for Health Economics, York: Sarah Byford and David Torgerson; London (Statistics): Simon Thompson (Royal Postgraduate Medical School) and lan White (London School of Hygiene and Tropical Medicine). The UK700 trial was funded by grants from the UK Department of Health and NHS Research and Development programme.







eLetters
No eLetters have been published for this article.