Effective treatment of obesity in children requires parents to recognise that excess weight is an issue and be motivated to make lifestyle changes to improve weight. This is potentially more successful at younger ages when parents maintain some control over the family food and activity environment and before lifestyle habits have become entrenched( Reference Faith, Van Horn and Appel 1 ). Unfortunately it is well established that parents of young children do not recognise overweight in their offspring( Reference Miller, Grant and Drummond 2 , Reference Doolen, Alpert and Miller 3 ). In fact, excess weight may only be viewed as a concern once it is at the level of impeding physical functioning or the child is being bullied about his/her size( Reference Jain, Sherman and Chamberlin 4 ).
Concepts central to motivation include perceived importance of the issue, confidence to change and the ability to actually do so( Reference Miller and Johnson 5 ). However, while motivation is regarded as a critical prerequisite for encouraging behaviour change( Reference Miller and Rollnick 6 ), factors that may influence parental motivation for changing their child’s weight have rarely been studied. Research to date suggests that parents categorised as making preparations for, or actively engaged in, change are more likely to have older children, believe that their child’s weight is a health problem or be overweight themselves, compared with parents who are not interested in change( Reference Rhee, DeLago and Arscott-Mills 7 ). Even when parents of obese children indicate strong concern about their child’s weight (importance) and are ready to make diet and activity changes (readiness), their confidence in their ability to actually do so is markedly lower( Reference Campbell, Benton and Werk 8 ). This has important implications for success given that confidence in the ability to do well is a significant predictor of treatment completion and early weight loss, whereas importance and readiness are not related( Reference Gunnarsdottir, Njardvik and Olafsdottir 9 ). Parental motivation for weight loss is also known to be a predictor of treatment uptake( Reference Dhingra, Brennan and Walkley 10 , Reference Taylor, Williams and Dawson 11 ). How to increase motivation is therefore of importance, yet we know little about what factors determine motivation in parents for changing weight in their overweight children.
Motivation can be measured in a variety of ways. The Motivational Screening Measure (MSM) was developed as a simple tool to quickly assess motivation for behaviour change in the clinical setting. The MSM consists of three questions which assess key facets of motivation: importance, ability and commitment to change the behaviour of interest( Reference Miller and Johnson 5 ). We recently undertook a major weight-screening initiative where we measured parental motivation for changing weight in young children prior to knowledge about the child’s weight status( Reference Dawson, Brown and Cox 12 ). The aim of the present study was to determine what factors were associated with parental motivation to change body weight in a community sample of children aged 4–8 years identified as overweight through screening.
Experimental methods
The present analysis involved Phase 1 of our Motivational Interviewing and Treatment (MInT) study( Reference Taylor, Brown and Dawson 13 ), which assessed parental responses to different styles of weight feedback after a weight-screening initiative( Reference Dawson, Brown and Cox 12 ). The study has previously been described in detail( Reference Taylor, Brown and Dawson 13 ), but information relevant to the present analysis is described here. Ethical approval was obtained from the Lower South Regional Ethics Committee (LRS/09/09/039) and all parents gave informed consent.
Health check appointment
All families with children aged 4–8·99 years enrolled at nine participating general practices were invited to participate in a comprehensive health check. Recruitment occurred from March 2010 until August 2011. Children of the same age, not already enrolled at any of these practices, who attended secondary care clinics across two time periods (March 2009–March 2010 and January 2011–May 2011) were also invited to attend. Children were excluded if they had severe childhood arthritis, severe asthma, cystic fibrosis, inflammatory bowel disease, congenital or chromosomal abnormalities, severe developmental delay or were on medication that may influence body composition, or if their families were not planning to remain in the region for the next two years.
Duplicate measures of height (Tanita portable stadiometer) and weight (Tanita BC-418) were obtained following standard techniques. BMI was derived and Z-scores calculated( Reference Kuczmarski, Ogden and Guo 14 ). Questionnaires on demographics, motivation, parenting, social desirability and beliefs about the child’s weight were completed before the parents were informed of the weight status of their child. Household structure, child ethnicity and socio-economic status were assessed using questions from the New Zealand census (www.stats.govt.nz). Socio-economic status was determined using the New Zealand Deprivation index (NZDep), which is a measure of deprivation assigned to an area based on population criteria such as income, housing and qualifications( Reference White, Gunston and Salmon 15 ). Maternal height and weight were measured in duplicate at the health check appointment where possible (49 %), were self-reported (48 %) or missing (3 %).
Miller and Johnson’s( Reference Miller and Johnson 5 ) MSM assessed three constructs of motivation in parents, namely importance (‘It is important for me to…’), ability (‘I could…’) and commitment (‘I am trying to…’), in relation to three behaviours: increasing their child’s physical activity, improving their child’s diet or changing their child’s weight. Each of the nine questions was answered on an 11-point scale, where: 0 and 1= ‘definitely not’; 2, 3 and 4= ‘probably not’; 5= ‘maybe’; 6, 7 and 8= ‘probably’; and 9 and 10= ‘definitely’. Parental feeding practices thought to influence child weight were assessed using five constructs( Reference Haszard, Williams and Dawson 16 ) from the Comprehensive Feeding Practices Questionnaire( Reference Musher-Eizenman and Holub 17 ). Parenting practices were indicated by the Parenting Scale( Reference Arnold, O’Leary and Wolff 18 ), with higher scores indicating more ineffective parenting practices (possible range: 1–7). For example, in response to ‘When I give a fair threat or warning…’ the parent would indicate ‘I often don’t carry it out’ (score of 7) compared with ‘I always do what I said’ (score of 1). Social desirability was assessed in a random sample of participants using the thirteen-item short form of the Marlowe–Crowne Social Desirability Scale, with higher scores indicating more socially desirable responses( Reference Reynolds 19 ). Parental concern for the child’s weight was based on a 5-point Likert scale (1= ‘not at all concerned’, 5= ‘very concerned’), and parents were also asked to rate their child’s weight on a 5-point scale (‘a little underweight’, ‘underweight’, ‘normal weight’, ‘a little overweight’, ‘overweight’).
Baseline intervention appointment
A total of 1093 children underwent screening, of whom 271 were classified as overweight (BMI≥85th percentile of US reference data)( Reference Kuczmarski, Ogden and Guo 14 ). Parents of these children were randomised to receive information about their child’s weight status using motivational interviewing or best practice care, and were subsequently invited into a two-year intervention( Reference Dawson, Brown and Cox 12 ). Those agreeing to participate (n 203, 75 %) attended an additional appointment where the following measures were obtained. Dietary intake was assessed using the Children’s Dietary Questionnaire( Reference Magarey, Golley and Spurrier 20 ), a twenty-nine-item questionnaire which yields three subscales of interest. Parents completed the CHAOS (Confusion, Hubbub and Order Scale) questionnaire, with yes or no answers to fifteen items about structure within the home such as ‘there is very little commotion in our home’. Higher scores indicate a greater level of household chaos( Reference Matheny, Wachs and Ludwig 21 ). Parents also completed the Lifestyle Behaviour Checklist, which asks parents to rate the extent to which they experience twenty-five weight-related behaviours in their child (e.g. eating unhealthy snacks, refusing to do physical activity) on a 7-point scale (from ‘not at all’ to ‘very much’)( Reference West and Sanders 22 ).
Physical activity and time asleep were measured over seven consecutive days by ActiGraph (GT3X) accelerometers worn 24 h per day. All sleep time was removed from the files before analysis of physical activity as counts per minute or time in moderate-to-vigorous physical activity( Reference Evenson, Catellier and Gill 23 ) was calculated.
Statistics
Measures on demographics, motivation, parenting and beliefs about the child’s weight were available in all 271 overweight children (from the health check appointment). Measures of diet, physical activity, sleep, chaos and problem behaviours (Lifestyle Behaviour Checklist) were available for 203 of these children (from the baseline intervention appointment). A composite motivation for weight change score was calculated from the average of the three questions from the MSM. Cronbach’s α for this composite measure was 0·89.
Data are presented as mean and standard deviation, or as number and percentage, as appropriate. Differences between groups were compared using independent t tests. Univariate and multivariate regression analysis was used to determine which factors were related to the composite motivation for weight change score. All analyses were undertaken using the statistical software package Stata release 12.
Results
Table 1 presents the demographic characteristics of the study population. The sample was predominantly European, but included a higher proportion of ethnic minority children than is typically observed in the local population (NZ Census, 2006). Although this was a well-educated sample (one-third of mothers with a university degree), a wide range of socio-economic status was still observed. Not surprisingly, maternal BMI was high in this sample of overweight (61 %) and obese (39 %) children.
Table 1 Characteristics of the study population: children (n 271) aged 4–8 years, recruited in primary and secondary care, and their parents, Dunedin, New Zealand, March 2010–August 2011
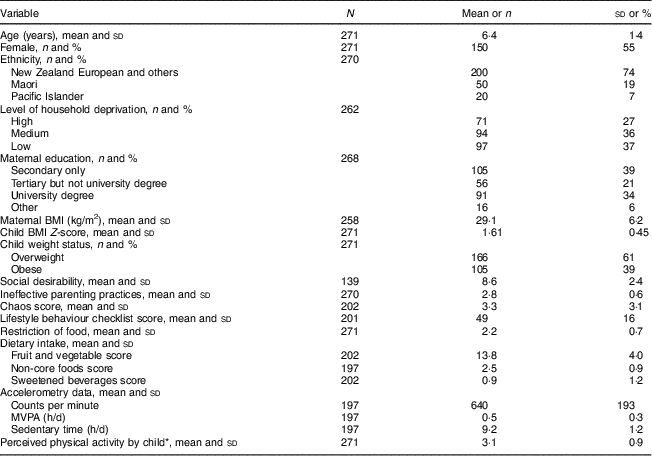
MVPA, moderate-to-vigorous physical activity.
Data are presented as mean and standard deviation, or as number and percentage, as appropriate.
* On a scale where 1=‘much less active’ and 5=‘much more active’ than children of the same age and sex.
Table 1 also reports the mean values for the various lifestyle factors of interest in this sample. Overall, parents within the sample reported low levels of chaos within the home (mean score of 3·3 from a total maximum of 15) and a low rate of ineffective parenting practices (mean score of 2·8 from a total maximum of 7). Scores obtained from the social desirability questionnaire spanned the entire range (0–13) with a mean score of 8·6, indicating that social desirability was present within this group. Fruit and vegetable intake was relatively close to the recommended level (14), but children ate more non-core foods than is advised (recommended two or less). However, sweetened drink intake was below the recommended level. Accelerometry data indicated that this was a sedentary group, with children spending more than 9 h/d in sedentary activities and only 33 min/d in moderate-to-vigorous physical activity.
The majority (n 158, 58 %) of parents rated their child as normal weight, with ninety (33 %) saying their child was a little overweight and a further twenty-three (8 %) reporting the child as overweight. Only ninety-six parents (36 %) were concerned about their child’s weight, with parents being significantly more concerned about girls compared with boys (P=0·036), despite no significant sex difference in BMI Z-scores (P=0·374). Table 2 presents the findings from the MSM. Parents were clearly more motivated for children to have a healthy diet or be more physically active than to change their body weight, despite all children being overweight or obese. For example, 79–83 % of parents scored 9 or 10 (anchor of ‘definitely’) for questions assessing the importance of eating healthily or being physically active, compared with only 8 % doing so for changing the child’s weight. Similar variation was observed for diet and activity measures of confidence (‘I could…’) and commitment (‘I am trying to…’) compared with relevant weight measures (data not shown). Within the weight subscale, confidence in the ability to change children’s weight was higher than either importance (P<0·001) or commitment (P<0·001). Similarly to weight concern, higher scores were observed for each weight motivation question in girls, indicating that parents seemed to feel it was more important to change their daughter’s weight (P=0·001) and more were actively trying to do so (P=0·005). However, confidence to do so (‘I could change their weight’) was also higher for girls compared with boys (P=0·002). By contrast, sex differences in motivation for improving diet or activity were not apparent (data not shown).
Table 2 Parental motivation scores for changing the dietary intake, physical activity participation and body weight of their overweight child (n 271), Dunedin, New Zealand, March 2010–August 2011

MSM, Motivational Screening Measure.
* Using a scale from 0 (‘definitely not’) to 10 (‘definitely’).
Few demographic variables were related to motivation for changing the child’s weight in univariate analyses (Table 3). Although increasing levels of parental motivation were observed in older children and girls, no differences in motivation were apparent by level of household deprivation or maternal BMI. Much stronger positive relationships were observed with the child’s actual weight status (BMI Z-score, P<0·001) and whether their parents perceived them to be overweight (P<0·001) or were concerned about their weight status (P<0·001).
Table 3 Predictors of parental motivation to alter child’s body weight (using composite score for motivation), Dunedin, New Zealand, March 2010–August 2011
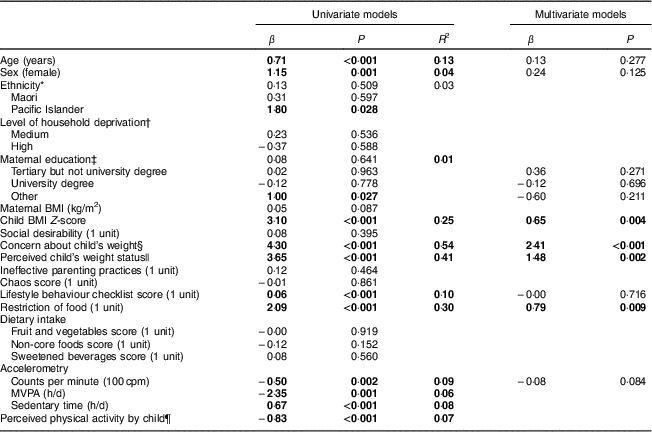
Values shown in bold were significant (P<0·05)
* Reference group is New Zealand European and Others.
† Reference group is low.
‡ Reference group is some secondary.
§ Concerned v. not concerned.
|| Overweight v. about right.
¶ On a scale from 1 (‘much less active’) to 5 (‘much more active’).
Lifestyle was also associated with parental motivation for changing weight (Table 3). Parents reported increased motivation for children who scored higher on the Lifestyle Behaviour Checklist (P<0·001), an indicator of problem behaviours common in overweight children. In total, seventy-nine children (39 %) scored 50 or more on this questionnaire, indicating significant clinical issues( Reference West and Sanders 22 ). More motivated parents also scored higher on the food restriction scale, a parental feeding strategy known to be related to body weight during growth. Motivation for weight change was not related to dietary intake (Table 3), but was higher in parents of children with lower levels of physical activity (accelerometer or questionnaire) or more sedentary time (Table 3). Interestingly, motivation to change the child’s weight was not related to social desirability, the degree of perceived chaos within the home or overall ineffective parenting practices.
All variables significant in the univariate analysis were entered in the multivariate model with the exception of ethnicity, as the overall P value was not significant. Separate multiple regression analyses were also undertaken using each of the measures of physical activity because of the high multicollinearity between these measures. Only that for counts per minute is shown here but results from the other regression models were comparable. In total, these variables explained a large proportion of the variance in MSM weight score (69 %). Age, sex, maternal education and physical activity were no longer significant. Particularly large effects were observed for parental perception of weight status and concern about weight, with relatively smaller contributions from child BMI and food restriction. For example, parents who were concerned about their child’s weight scored 2·5 units higher (almost 1 sd) on the MSM than those who were not concerned, with a difference of approximately 1·6 units for parents who classified their child as overweight compared with those who thought they were ‘about right’. Comparable differences in motivation for weight score of 0·7–0·8 were noted for 1-unit differences in actual weight status of children (one BMI Z-score) or food restriction (on a possible scale of 1–5). Because motivation for changing the child’s weight was so highly correlated with parental concern (r=0·76, P<0·001) and perception (r=0·63, P<0·001) of weight status, multivariate analyses were also undertaken excluding these two variables from the model. This alternative model still explained 52 % of the variance in motivation, with age (P=0·008), sex (P<0·001), BMI Z-score (P<0·001), food restriction (P<0·001) and physical activity (P=0·014) remaining significant predictors, and lifestyle behaviour score (P=0·537) and maternal education (P=0·09) no longer being significant.
Discussion
Our results demonstrate that parental motivation to change body weight in a community-based sample of young overweight children is low, with only 8 % of parents actively trying to influence their child’s weight. As expected, motivation was higher in children with greater degrees of overweight. However, even when restricted just to those with BMI values greater than the 97th percentile, only fourteen of sixty-seven parents (21 %) were actively trying to change their child’s weight, despite virtually all (84 %) of these parents perceiving their child as overweight. While this apparent lack of motivation may seem surprising, others have clearly shown that parents are not concerned about excess weight in young children until it really starts to impede their mental or physical health( Reference Jain, Sherman and Chamberlin 4 ). The dichotomy between parental ratings of the BMI values that suggest intervention is required, and that of expert committees, has been demonstrated previously( Reference Warschburger and Kroller 24 , Reference Wake, Canterford and Hardy 25 ). Over 70 % of parents reported that the 90th BMI percentile is the minimum point at which weight management should be initiated, of whom one in five indicated that intervention should not happen until above the 97th percentile( Reference Warschburger and Kroller 24 ). Similarly, a large Australian study could not demonstrate a discernible threshold above which mothers reliably became concerned about their young child’s weight( Reference Wake, Canterford and Hardy 25 ).
Parents indicated greater motivation to change weight in girls compared with boys, despite no sex difference in relative weight status. This is perhaps because mothers are more likely to identify( Reference Jeffery, Voss and Metcalf 26 , Reference Vanhala, Keinanen-Kiukaanniemi and Kaikkonen 27 ) or be concerned( Reference Campbell, Williams and Hampton 28 , Reference Moore, Harris and Bradlyn 29 ) about overweight in daughters compared with sons. Presumably, this reflects differing social values reflecting greater acceptance of overweight in boys relative to girls( Reference Maynard, Galuska and Blanck 30 ). Greater motivation scores were also apparent when parents recognised there was a weight issue and/or were concerned about it. This is not surprising given there would be no desire to change weight if parents did not perceive their child as overweight, or at least were not concerned about it. How parents perceive the child’s weight, whether they are concerned about it and their motivation to change weight are obviously interrelated variables of interest. While no studies appear to have examined correlates of parental motivation for changing weight in overweight children per se, studies have identified several factors predicting increased concern about weight in children including age (older v. younger) and sex (girls compared with boys)( Reference Moore, Harris and Bradlyn 29 , Reference Baughcum, Chamberlin and Deeks 31 ), parental body size( Reference Rhee, DeLago and Arscott-Mills 7 ), parents with a vested interest (overweight themselves)( Reference Carnell, Edwards and Croker 32 ), body fat distribution and intake of sweet drinks( Reference Keller, Olsen and Kuilema 33 ). Similarly, poorer maternal accuracy regarding children’s weight status has been associated with maternal education, maternal BMI, lower physical activity and rapid weight gain in infancy( Reference Manios, Moschonis and Grammatikaki 34 ).
Motivation was also higher in parents who perceived their child to have more problem behaviours as indicated by higher scores on the Lifestyle Behaviour Checklist( Reference West and Sanders 22 ), those who were less physically active and parents who reported a greater degree of food restriction. It is interesting that motivation was higher in children who recorded significantly lower participation in physical activity. In practice, however, these differences are very small, not clinically relevant and were no longer significant in multivariate analyses. Restriction refers to the parent limiting and regulating a child’s access to less healthy foods. Although this was initially thought to increase the risk of obesity( Reference Birch, Fisher and Davison 35 , Reference Faith, Berkowitz and Stallings 36 ), more recently work has demonstrated that maternal restriction is associated with lower BMI scores three years later, at least in younger children( Reference Campbell, Andrianopoulos and Hesketh 37 ). Thus parents who believe their child overeats might use restrictive feeding practices as a way of controlling that eating. Our observation that motivation was associated with restriction fits with other work demonstrating that concern is associated with restriction( Reference Birch, Fisher and Davison 35 , Reference Birch, Fisher and Grimm-Thomas 38 , Reference Webber, Hill and Cooke 39 ). However in our sample, restriction remained a significant correlate of motivation even when adjusted for parental concern about weight.
Interestingly, parents were far more receptive towards changing diet and exercise habits in their children compared with changing weight. Discussions around target behaviours obviously provide an indirect means for health professionals to use as a focus for making important changes that do not address weight directly, but should have positive impact. It may be easier to engage parental motivation and action with diet and activity as a focus rather than weight, which may address concerns health professionals have about managing weight issues without damaging doctor/parent relationships( Reference He, Piche and Clarson 40 , Reference Banks, Sheild and Sharp 41 ). Greater parental intention to change diet or activity (relative to weight) was not a function of social desirability, with no significant correlations between social desirability and any motivation score. This is important given that misreporting of dietary intake and physical activity has been associated with social desirability in children( Reference Klesges, Baranowski and Beech 42 ) and parents( Reference Börnhorst, Huybrechts and Ahrens 43 ).
The strengths of our study include the use of a community-based sample, rather than a treatment-seeking population, and the assessment of motivation and other variables of interest before feedback of weight status occurred. Our parents were predominantly unaware of the weight status of their young child and the only information provided about the purpose of the study at recruitment was that it was for screening purposes. Although we did not recruit in a truly representative manner, we did purposively recruit a wide section of general practices, resulting in a final study sample with very few demographic differences from the wider local population( Reference Dawson, Brown and Cox 12 ).
Thus the low levels of parental motivation for changing the weight of their overweight child that we observed do provide cause for concern. Recognition an issue exists is considered the first step in making appropriate behaviour change( Reference Barlow, Bobra and Elliott 44 ). Yet recognition alone is obviously not enough given our marked difference in those who rated their child as overweight (41 %) compared with those who were actively trying to change it (8 %). It appears that parents are more amenable and prepared to consider changing diet and activity than weight, which provides a useful pathway for health professionals to take when addressing overweight in young children. This may, at least in part, reflect the success of long-term public health campaigns promoting the importance of a healthy diet and regular physical activity for optimal development. Whether similar campaigns aimed at re-educating the general public about what (un)healthy weight looks like at different developmental stages would positively affect parental recognition and motivation for addressing overweight in their children is a question for future research. Despite higher levels of motivation for making dietary change, our results demonstrated a real dichotomy between parental views of their level of motivation to change diet and actual dietary behaviour, reflecting the complexity of the relationship between motivation and action. Further research investigating why parents do not appear motivated to change the weight of their overweight child should provide much-needed insight into how best to encourage healthy lifestyles for all young children( Reference Gruber and Haldeman 45 ).
Acknowledgements
Financial support: This research was funded by the Health Research Council of New Zealand (grant number 09/087B). The Health Research Council had no role in the design, analysis or writing of this article. Conflicts of interest: None. Authorship: R.W.T. is Principal Investigator of the MInT study; she conceived of the idea for the paper and wrote the first and subsequent drafts of the manuscript. S.M.W. designed and completed all statistical analyses. A.M.D., J.J.H. and D.A.B. contributed to study design and data collection. All authors contributed to writing of the manuscript. Ethics of human subject participation: This study was approved by the Lower South Regional Ethics Committee (LRS/09/09/039).







