As nuts are rich in cis-unsaturated fats, vitamins, minerals, fibre and a number of phytonutrients( Reference Alasalvar and Bolling 1 – Reference Ros 3 ), their regular consumption is recommended as part of a number of dietary guidelines around the world( 4 – 7 ). This healthy nutrient profile of nuts likely contributes to the consistent negative associations seen between regular consumption of nuts and all-cause mortality over a given period of time( Reference Grosso, Yang and Marventano 8 , Reference Hshieh, Petrone and Gaziano 9 ) and, even more strongly, the risk of CVD( Reference Ros 3 , Reference Kris-Etherton, Yu-Poth and Sabate 10 – Reference Sabate, Oda and Ros 12 ).
The National Heart Foundation of New Zealand (NZ) recommends the consumption of 30 g nuts daily as part of a cardioprotective diet( Reference Tey, Brown and Chisholm 13 ). This recommendation was recently reflected in eating and activity guidelines for NZ adults, which recommend eating a variety of nuts and replacing less healthy snack foods with 30 g nuts daily( 4 ). A qualified health claim stating that eating 42 g nuts daily may reduce the risk of heart disease was approved in 2003 in the USA( 14 ). Nuts are also a prominent component of the cardioprotective Mediterranean diet( Reference Willett, Sacks and Trichopoulou 15 ).
While these public health messages are an important step to promoting regular nut consumption, it is largely unknown how and even if these messages are incorporated into advice provided by health professionals. This is an important consideration because previous research has suggested that advice by a doctor to increase nut consumption is an important facilitator of regular nut intake( Reference Pawlak, Colby and Herring 16 , Reference Pawlak, London and Colby 17 ). In a study among individuals with or at high risk of CVD and/or diabetes, 64 % agreed that they would consume nuts on most days of the week if their doctor made such a recommendation; however, only 27 % of respondents reported that their doctor did in fact advise them to eat nuts( Reference Pawlak, London and Colby 17 ).
The need to promote regular nut consumption among the general population has become even more apparent following population studies which indicate that regular nut consumption is much lower than recommended( Reference Brown, Tey and Gray 18 – Reference O’Neil, Nicklas and Fulgoni 21 ). A nationally representative survey in NZ showed that only 6·9 % of participants had consumed any whole nuts on the study day. These whole nut consumers had a mean intake of 40 g/d, achieving the recommended NZ and US intakes. However, the overall mean population intake was only 2·8 g/d, less than one-tenth of the recommended 30 g, based on a 24 h recall( Reference Brown, Tey and Gray 18 ). In total only 29 % of New Zealanders consumed any form of nut on the study day, with a mean individual intake of 17·9 g, about one-half of the recommendation, and with a mean population intake of only 5 g/d, one-sixth of the recommendation. Similar findings in Europe and the USA suggest population-level nut intakes in a number of countries are much lower than the current guidelines and therefore need to be addressed( Reference Jenab, Sabate and Slimani 19 , Reference O’Neil, Keast and Nicklas 20 ). Studies have indicated that nuts are resistant to monotony and so habitual consumption at recommended levels may be possible if consumers can be motivated to increase their consumption( Reference Tey, Brown and Chisholm 22 , Reference Tey, Gray and Chisholm 23 ).
One approach to improving nut intakes is the promotion of regular nut consumption by doctors and, potentially, other health professionals who are also likely to offer nutrition advice. Different population groups will have different levels of contact with different health professionals and so a multi-profession approach may allow promoting consumption more widely, and reinforcement by different groups of health professionals may improve uptake of health messages. Health professionals, including nurses, doctors, pharmacists and dentists, are all regularly included near the top of lists of trusted professions, with nurses frequently being listed as the most trusted professionals of all( 24 , 25 ). However, to the best of our knowledge, there is little information on whether health professionals provide advice consistent with nut consumption guidelines. Given that the advice from health professionals may be an important facilitator of nut consumption, gaining an understanding of current nut recommendation practices is important. Therefore, the present study aimed to assess the advice regarding nut consumption provided by health professionals in NZ, particularly dietitians, general practitioners and practice nurses.
Materials and methods
The study methods are described in detail in elsewhere( Reference Brown, Yong and Gray 26 ) and only essential details are presented here.
Study design and participants
This was a cross-sectional study of health professionals who were identified from the NZ Parliamentary Electoral Roll and was conducted during September–November 2014. Three professional occupations of interest were identified, namely dietitians, general practitioners and practice nurses, reflecting those who were considered the most likely to provide dietary advice (Table 1).
Table 1 List of self-described occupations identified from the New Zealand Parliamentary Electoral Roll
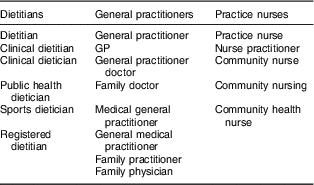
An information sheet was posted to all participants and completion of the survey (online or the paper version) was taken as informed consent.
Survey development
The self-administered questionnaire consisted of three sections for demographics, perceptions of nuts and advice regarding nut consumption. The demographics section contained questions on sociodemographic characteristics including age, sex, ethnicity and number of years as a registered practitioner. Other questions from the other sections analysed here include: whether they recommended increasing or decreasing nut consumption for some patients and the types, forms and quantity of nuts that they recommended. The types of nuts included tree nuts and peanuts, but not coconuts or chestnuts as these differ in nutritional composition. There was a combination of open-ended and multiple-choice questions and multiple-response questions. For example, the question on the recommended frequency of nut consumption had six choices ranging from every day to once or less than once per month. The question on amounts of nuts recommended was an open-ended question. The questionnaire was pre-tested and modified where appropriate using feedback from twelve health professionals including six dietitians, two general practitioners and four practice nurses, establishing both face and content validity. Both an online version and a paper copy of the questionnaire were available. For the online version of the questionnaire, Survey Gizmo© (Widgix Software, LLC, Boulder, CO, USA) was used.
Survey administration
Recruitment used an adaptation of Dillman’s four-stage tailored design method for conducting a mail survey( Reference Dillman 27 ) with an invitation to participate and the URL for the survey, followed seven days later by a postcard thanking those who had already responded and reminding those who had not. Then, after another eight days, a paper version of the questionnaire was sent to the remaining non-respondents. A second postcard was sent to all recipients of the third mail-out another twelve days later, thanking those who had responded and reminding those who had not. Users were provided with a login code so that each participant could complete the questionnaire once only. The survey remained open for two and half months.
Statistical analysis
The sample size calculations are presented in detail in elsewhere( Reference Brown, Yong and Gray 26 ), but briefly, 184 usable responses were required for each occupation (equivalent to 368, allowing for a 50 % response rate). Sufficient numbers were not available from the Electoral Roll search for all three occupations and all identified electors were included in the sample for a total of 1440 health professionals comprising 578 dietitians, 596 general practitioners and 266 practice nurses, giving 95 % CI half-widths, assuming 50 % participation, of 6·0, 5·9 and 8·9 %, respectively, and with the greater numbers of dietitians and general practitioners providing approximately the same power as the original numbers for comparisons between either of these larger groups and the smaller number of practice nurses.
Baseline characteristics of respondents are presented as arithmetic means and standard deviations or medians and interquartile ranges for continuous variables. Categorical data are presented as frequencies and percentages. For analysis purposes, ethnicity was categorised as follows: Māori, European, Asian and other (comprising the Pacific, Middle Eastern/Latin American/African (MELAA), other, and residual categories in Statistics New Zealand’s level one ethnicity categories)( 28 ). Characteristics were compared between health professions using a χ 2 test for sex, a one-way ANOVA for age, Fisher’s exact test for ethnicity and the Kruskal–Wallis test for years as a registered practitioner.
For comparisons between health professions of binary outcome variables regarding nut recommendations, unadjusted analyses were initially conducted using logistic regression when there was a minimum of twenty participants with responses at each level (following Peduzzi et al.( Reference Peduzzi, Concato and Kemper 29 ) given the two parameters being estimated). If this was not the case, χ 2 tests were used unless more than 20 % of cells had expected counts below 5, in which case Fisher’s exact test was used( Reference Cochran 30 ). For outcomes compared using logistic regression, these were further adjusted for age (continuous), sex (male/female) and ethnicity (four levels) providing there were at least seventy participants with responses at each level (again, following Peduzzi et al. given the seven parameters being estimated). For ordinal variables, such as the percentage of patients whom health professionals recommend consume more nuts (<20 %, 20–39 %, 40–59 %, 60–79 %, ≥80 %), ordinal logistic regression was used for unadjusted models only and proportionality was assessed using a generalised ordinal logistic regression model. For all models with age included as an independent variable, age-squared was added to the model as a check for non-linearity and retained when statistically significant. For linear regression models, residuals were inspected for evidence of departures from normality or homoscedasticity, with log-transformations investigated and retained when this improved the satisfaction of model assumptions. Where model assumptions were not satisfied despite log-transformations, quantile regression was used to model medians instead. Quantile regression was used to compare median frequencies and gram amounts recommended between health professions, both without and with adjustment for age, sex and ethnicity. Where interactions were considered plausible, these were investigated and noted in the text irrespective of statistical significance. Missing responses were relatively infrequent for each question and no special treatment for these was performed. The statistical software package Stata version 14.2 was used for all statistical analyses. All statistical tests were two-sided and P<0·05 was considered statistically significant. Pairwise comparisons between levels of categorical variables were conducted only where the overall Wald test was statistically significant. No formal adjustment for multiple comparisons was performed in this exploratory study. Consequently, marginally statistically significant results and results not consistent with other findings should be interpreted with caution.
Results
Response rate
A total of 759 of the 1440 (53 %) health professionals completed the questionnaire, which was slightly higher than the anticipated response rate of 50 %. The response rates were not significantly different between health professions, being 55 % for dietitians, 49 % for general practitioners and 56 % for practice nurses (χ 2 P=0·058). No reasons were given by participants for not completing the questionnaire.
Participant characteristics
The demographic characteristics of the respondents are outlined in Table 2. Dietitians comprised 42 % of the total sample, general practitioners 38 % and practice nurses the remaining 20 %. The majority of respondents were female (81 %) with this imbalance especially prevalent in dietitians (97 %) and practice nurses (96 %) compared with general practitioners (57 %; χ 2 P<0·001). Mean age was 47·3 years, with the dietitian group on average being over 8 years younger than both general practitioners and practice nurses (one-way ANOVA overall P<0·001, post hoc tests P<0·001 for both pairwise comparisons involving dietitians and P=0·769 for general practitioners v. practice nurses). The respondents had a median of 20 years as registered practitioners, with practice nurses having been registered 5 and 12 years longer than general practitioners and dietitians, respectively (Kruskal–Wallis P<0·001, all post hoc Dunn’s tests P<0·001). The majority of respondents were NZ European (86 %). This varied between professional groups (Fisher’s exact P=0·002) with evidence of higher percentages of general practitioners being Asian (10·4 v. 4·7 % for practice nurses and 5·7 % for dietitians; χ 2 P=0·034) and MELAA (3·5 v. 1·3 % for practice nurses and 0·0 % for dietitians; Fisher’s exact P=0·001) when each was compared with the rest of the ethnicities.
Table 2 Characteristics of survey respondents: health professionals, New Zealand, September–November 2014
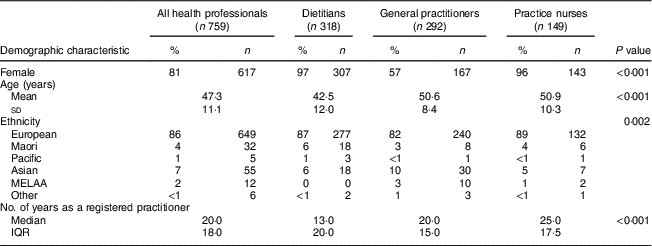
MELAA, Middle Eastern/Latin American/African; IQR, interquartile range.
P values from χ 2 test (sex), one-way ANOVA (age), Fisher’s exact test (ethnicity) and Kruskal–Wallis test (years registered).
Percentage of health professionals recommending patients to eat more nuts, fewer nuts or not mentioning nuts
Respondents were asked if they recommended that some of their patients should eat more nuts, fewer nuts, or did not mention nuts at all. There was an overall difference between the three groups of health professionals in terms of the percentage who would recommend patients to eat more nuts (i.e. are nut promoters; overall P<0·001 for both unadjusted and adjusted models), with pairwise comparisons showing that dietitians (82·7 %) were more likely to recommend the consumption of more nuts compared with 63·1 % of practice nurses and 55·5 % of general practitioners (both pairwise P<0·001 from both unadjusted and adjusted models) and with no differences between the practice nurses and general practitioners (P≥0·126 from unadjusted and adjusted models). From the adjusted model, females were more likely than males to recommend the consumption of more nuts (OR=1·68; 95 % CI 1·09, 2·58; P=0·019) with no evidence of an association with age (P=0·272) or with ethnicity (P=0·800). No evidence was found that the sex difference varied by profession when an interaction was added to the model (P=0·775).
Although fewer general practitioners said they recommended that some of their patients eat fewer nuts (e.g. reduce amounts or frequency; 26·7 %), compared with both practice nurses (45·0 %) and dietitians (41·2 %), the differences between health professionals were not statistically significant (overall P=0·064). Females were more likely than males to recommend that some of their patients eat fewer nuts (OR=2·04; 95 % CI 1·24, 3·35; P=0·005). There was evidence for a U-shape in the association with age with the numerical minimum at age 49 years (age P=0·019, age-squared P=0·023). The odds of recommending the consumption of fewer nuts was lowest at 49 years and comparisons with the youngest respondents were statistically significant (OR for 19-year-old (the youngest respondent) v. 49-year-old=3·20; 95 % CI 1·21, 8·51) but not quite statistically significant compared with the oldest respondents (OR for 77-year-old (the oldest respondent) v. 49-year-old=2·89; 95 % CI 0·95, 8·77). There was no evidence of an association with ethnicity (P=0·162; Table 3).
Table 3 Predictors of recommendations on nut consumption among responding health professionals (n 759), New Zealand, September–November 2014
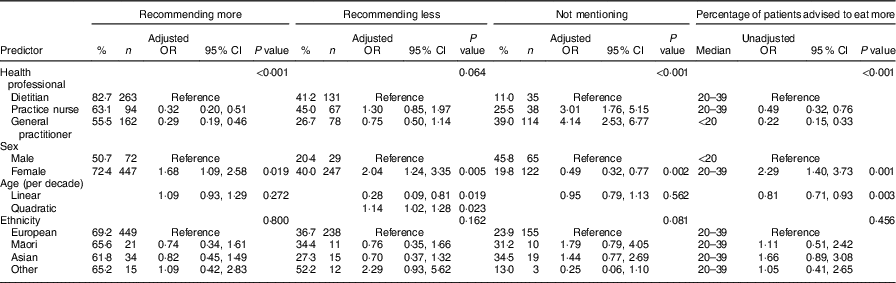
Models are binary logistic regression except for percentage of patients advised to eat more nuts, which was ordinal.
There was a significant difference between health professionals regarding the percentage who choose not to mention nuts to patients (overall P<0·001 from unadjusted and adjusted models). Only 11·0 % of dietitians did not mention nut consumption, which was significantly less than the 25·5 % of practice nurses and 39·0 % of general practitioners (both pairwise P<0·001 from both unadjusted and adjusted models). There was no difference between general practitioners and practice nurses after adjustment (unadjusted P=0·005, adjusted P=0·196). Females were less likely than males to not mention nuts (OR=0·49; 95 % CI 0·32, 0·77, P=0·002). There was no evidence of an association with ethnicity (P=0·081) or age (P=0·562), nor a profession×sex interaction (P=0·908; Table 3).
Respondents were also asked to estimate the percentage of patients they advise to eat more nuts. The median response for both dietitians and practice nurses was 20–39 % of respondents, compared with <20 % of general practitioners. There was a significant overall difference between health professions (overall ordinal logistic regression P<0·001; no evidence of non-proportionality). Pairwise comparison showed significant differences between all health professionals (all pairwise P≤0·001), with general practitioners having only about one-fifth the odds of making recommendations to eat a larger proportion compared with dietitians (OR=0·22; 95 % CI 0·15, 0·33, P<0·001) and practice nurses having about one-half the odds compared with dietitians (OR=0·49; 95 % CI 0·32, 0·76, P=0·001; Table 3). Adjusted models were not able to investigate proportionality due to the numbers of events but similar results for professions were observed in models assuming proportionality, with no evidence for associations with age, sex or ethnicity (results not shown).
Type of nuts and nut butters recommended by nut-promoting health professionals
The most common nuts recommended by health professionals were almonds, Brazil nuts and walnuts (Table 4). Significantly more dietitians recommend nuts in general compared with general practitioners and practice nurses (both pairwise P<0·001). Other significant differences between health professionals were for almonds, Brazil nuts, peanuts and walnuts (all overall P≤0·035 from adjusted models). Pairwise comparisons showed that dietitians are less likely to recommend almonds compared with general practitioners and practice nurses (both pairwise P≤0·007), and more dietitians would recommend peanuts compared with the other two health professions (both pairwise P≤0·040). In addition, fewer dietitians recommend Brazil nuts compared with general practitioners (pairwise P=0·005). Further, significantly more practice nurses recommend walnuts than both dietitians and general practitioners (both pairwise P≤0·036).
Table 4 Types of nuts and nut butters recommended by nut-promoting health professionalsFootnote *, New Zealand, September–November 2014
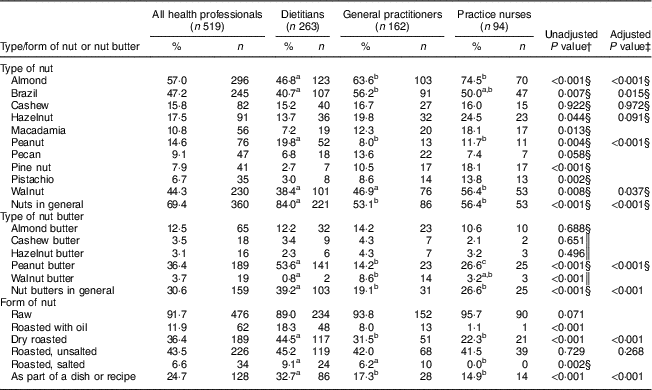
a,b,cPercentage values within a row with unlike superscript letters were significantly different after adjustment for age, sex and ethnicity (P<0·05).
* Respondents could choose multiple responses.
† P value for difference between health professionals.
‡ Adjusted for age, sex and ethnicity where there are sufficient responses.
§ Indicates logistic regression.
║ Indicates χ 2 test.
Overall, fewer health professionals reported recommending nut butters in general (30·6 %) compared with nuts in general (69·4 %). Significantly more dietitians (39 %) would recommend nut butters in general than both general practitioners (19 %) and practice nurses (27 %; both pairwise P≤0·014). In addition, significantly more dietitians (54 %) would recommend peanut butter compared with only 14 % of general practitioners and 27 % of practice nurses (both pairwise P<0·001). The difference between general practitioners and practice nurses was also significant (P=0·012). Of the tree nut butters, almond butter was the most frequently recommended by health professionals (12·5 %), while cashew butter, hazelnut butter and walnut butter were recommended by less than 4 % of health professionals. The only age, sex or ethnicity effects from adjusted models were for walnuts (overall P=0·007), where those of Asian ethnicity were more likely to recommend walnuts than those of both European (OR=3·95; 95 % CI 1·78, 8·75; P=0·001) and Māori (OR=5·53; 95 % CI 1·65, 18·53; P=0·006) ethnicity.
Nut forms recommended by nut-promoting health professionals
The most commonly recommended form of nut by all three health professionals were raw nuts (91·7 %; Table 4). This was followed by roasted, unsalted nuts (43·5 %), dry roasted (36·4 %), as part of a dish or recipe (24·7 %) and roasted with oil (11·9 %), with the least popular form being roasted and salted (6·6 %). There were overall differences between health professions for the percentage recommending dry roasted nuts, and as part of a dish (both overall P<0·001). Pairwise comparisons showed that more dietitians recommend dry roasted nuts compared with general practitioners (P=0·023) and practice nurses (P<0·001). In addition, more general practitioners recommend this form of nut compared with practice nurses (P=0·032). Compared with both general practitioners and practice nurses, more dietitians recommend nuts as part of a dish. Exact logistic regression was used to compare recommending roasted, salted nuts and found evidence of an overall difference (P=0·002), with practice nurses less likely to recommend this form than both dietitians (P=0·001) and general practitioners (P=0·015). The only age, sex or ethnicity effects from the adjusted models were that female professionals were less likely to recommend nuts roasted with oil (OR=0·28, 95 % CI 0·11, 0·71; P=0·007) and older professionals were more likely to recommend both roasted, unsalted nuts (OR per 10-year age increase=1·26; 95 % CI 1·06, 1·50; P=0·008) and nuts in a dish (OR per 10-year age increase=1·47; 95 % CI 1·21, 1·79; P<0·001).
Frequency and quantity of nuts recommended by nut-promoting health professionals
The plurality of dietitians and practice nurses recommended patients eat nuts every day (40·4 and 39·1 %), followed by 2–4 times per week (37·7 and 35·9 %). The plurality of general practitioners recommended a frequency of 2–4 times per week (35·4 %), followed by every day (32·9 %; Table 5). There was no evidence of a difference in median frequencies between groups (23·9 servings/month for all professional groups, equivalent to 5·5 servings/week) in both the adjusted and unadjusted models (quantile regression overall P=1·000 for both unadjusted and adjusted models).
Table 5 Recommended frequency of nut consumption by nut-promoting health professionalsFootnote *, New Zealand, September–November 2014
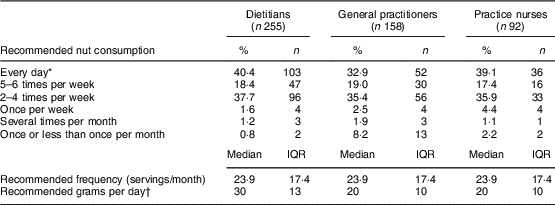
IQR, interquartile range.
* Respondents chose from a multiple-choice question.
† These data are from an open-ended question.
There was evidence for a difference in the median amounts of nuts recommended by the three different types of health professional (overall P<0·001 for both unadjusted and adjusted). The quantity of nuts recommended by dietitians (median 30 g) was significantly higher compared with both general practitioners (20 g) and practice nurses (20 g; both pairwise P≤0·001 for both unadjusted and adjusted models). There was no difference between general practitioners and practice nurses (quantile regression overall P=1·000 for unadjusted and adjusted models).
Discussion
To the best of our knowledge, the present study is the first to examine nut recommendation practices among different groups of health professionals. It is plausible that the advice provided by health professionals would influence nut consumption patterns among the general public. Indeed, previous research has suggested that individuals would consume nuts on most days of the week if advised to do so by a doctor( Reference Pawlak, Colby and Herring 16 , Reference Pawlak, London and Colby 17 ). Other health professionals such as dietitians and practice nurses also offer dietary advice; therefore, also examining these professions was considered more informative than investigating only doctors, especially given high levels of public trust in nurses( 24 , 25 ). Results may be generalisable to health professionals in other countries with similar characteristics to NZ and possibly more broadly with greater caution.
Overall, 68 % of health professionals recommended at least some of their patients to eat more nuts, with dietitians significantly more likely to do so compared to both general practitioners and practice nurses. This most likely reflects the specialised nutrition training of dietitians and the focus of their work. Interestingly, about 40 % of dietitians also recommended that some of their patients should eat fewer nuts. The reasons for recommending that some patients eat fewer nuts are reported in detail elsewhere( Reference Brown, Yong and Gray 26 ), but in brief these included the fact that nuts are high in energy and fat, cause weight gain, people may have allergies and they may be too expensive. Participants were also able to comment further regarding this recommendation. Dietitians were more likely to do so, with the majority of additional comments pertaining to the individualised dietary requirements of specific patients. For example, a reason dietitians commonly gave for recommending some patients eat fewer nuts was because the K and P concentrations were too high for patients with renal conditions. This specific advice again reflects the specialised nutrition training of dietitians and the nutrition emphasis of their consultations.
There is a distinct lack of research with which the results of the present study can be compared. Previously, Pawlak et al. reported among low-income participants that the strongest agreement regarding barriers and facilitators was with the statement ‘I would eat nuts on most days of the week if my doctor recommended me to do so’( Reference Pawlak, Colby and Herring 16 ). In a further study by this group, among those with or at risk of CVD and diabetes, 64 % of participants also agreed or strongly agreed that they would consume nuts on most days of the week if their doctor made such a recommendation( Reference Pawlak, London and Colby 17 ). Therefore, the nut recommendation practices of health professionals appear to be an important influence on nut consumption. However, in that study, only 27 % of participants agreed or strongly agreed that their doctor advises them to eat nuts( Reference Pawlak, London and Colby 17 ). In our study, 55 % of general practitioners reported they recommend some patients to eat more nuts, which was lower compared with both practice nurses and dietitians, although only significantly so compared with the latter. The present study was not designed to investigate differences between messages given and those received, but given the large difference observed, this is worthy of further research. Exploring strategies whereby more health professionals, particularly general practitioners and practice nurses, are encouraged to promote nut consumption to their patients is also justified to complement other approaches such as information from nutritionists, public health campaigns and the media. Given our results, improving knowledge of the health benefits of regular nut consumption should form the basis of such approaches.
The most popular nuts recommended by health professionals in the present study were almonds, Brazil nuts and walnuts. It is possible that these nuts are most commonly recommended, in part, due to the attention they receive in the lay media. For example, the Almond Boards of both California and Australia have active marketing campaigns, which are likely to increase the profile of this nut type. Walnuts may receive more attention than some other nuts because they are a good source of α-linolenic acid, a plant-based n-3 fat, that has received much attention in both the scientific and lay literature for reducing the risk of CVD( Reference Djousse, Arnett and Carr 31 , Reference Venkatachalam and Sathe 32 ). In addition, walnuts grow in many parts of NZ, often in domestic gardens, thus allowing for the possibility of access to fresh nuts at little cost. NZ soils are low in Se( Reference Thomson 33 ). With this knowledge in mind, health professionals in NZ may be more likely to recommend Brazil nuts as an important source of Se. It would be interesting to compare recommendations regarding Brazil nuts among health professionals in NZ with those from other countries where obtaining adequate intake of Se is less problematic.
Interestingly, dietitians were more likely to recommend nuts in general, possibly reflecting a better understanding of the overall health benefits of nuts. In the 2008/09 NZ Adult Nutrition Survey which assessed nut intake by 24 h recalls, the most popular nuts consumed were almonds, mixed nuts, cashews, Brazil nuts and walnuts( Reference Brown, Tey and Gray 18 ). This largely reflects the types of nuts recommended by health professionals in the current study.
The National Heart Foundation of NZ recommends the consumption of 30 g nuts daily( Reference Tey, Brown and Chisholm 13 ). In the present study, the most common recommendation by dietitians and practice nurses was to eat nuts on a daily basis, whereas the majority of general practitioners recommended patients eat nuts 2–4 times weekly. Although this difference was not statistically significant, it is worth noting that fewer than half of general practitioners offered a message consistent with the National Heart Foundation’s guidelines. Over one-third of each health profession recommended nuts to be eaten every second day. Therefore, a future direction for educating health professionals could be the emphasis on nuts as a literally ‘everyday’ food, which can also be used to replace less healthful snacks. The median quantity of nuts recommended by dietitians was 30 g daily, which was significantly more than both general practitioners and practice nurses (both 10 g/d less). The advice provided by dietitians most closely reflects current recommendations in NZ (30 g/d), and again this is likely to be due to their nutrition training. Improving the knowledge of nut consumption guidelines should form the basis of continuing education material for general practitioners and practice nurses but there is also room for improvement among dietitians despite their additional training.
In NZ, the consumption of nuts in their raw form is recommended( Reference Tey, Brown and Chisholm 13 ) and raw nuts were the most commonly recommended (over 90 %) nut form by all health professions in the present study. A substantial number of health professionals also recommended dry roasted nuts, with significantly more dietitians recommending this option compared with both general practitioners and practice nurses. Research suggests that roasting at temperatures below 140°C does not negatively impact the nutrient content of nuts( Reference Alasalvar, Pelvan and Amarowicz 34 – Reference Schlormann, Birringer and Bohm 36 ). The temperatures used to commercially roast nuts are typically within this range. Roasted and salted nuts were least likely to be recommended by all health professions. This likely reflects the potential negative effects of Na on health( Reference He, Li and Macgregor 37 ). Previous research has indicated that roasted nuts may be considered more palatable by some consumers( Reference Frecka, Hollis and Mattes 38 , Reference McKiernan, Lokko and Kuevi 39 ). A recent study showed that lightly salting (133 mg Na/100 g) and dry roasting nuts did not negate the health benefits seen with raw nut consumption( Reference Tey, Robinson and Gray 40 ). The amount of Na used in that study was similar to lightly salted commercial varieties (about 145 mg Na/100 g). Taken together, this suggests that health professionals should continue to recommend raw nuts, but could broaden their recommendations for patients who dislike the taste or texture of raw nuts to include dry roasted and lightly salted nuts.
Health professionals on the whole were much less likely to recommend nut butters than whole nuts. It appears nut butters are perceived as less healthy than whole nuts by this group of health professionals. Research on the health effects of regular peanut butter consumption is limited and conflicting, with some studies reporting positive effects( Reference Jiang, Manson and Stampfer 41 , Reference Li, Brennan and Wedick 42 ), while others do not( Reference Luu, Blot and Xiang 43 , Reference van den Brandt and Schouten 44 ). Given that peanut butter is relatively inexpensive and easy to consume, it could provide a viable alternative, especially for those on a low income or with mastication difficulties. The income aspect is especially important given the disproportionally higher rates of chronic disease among those in the most deprived households( 45 ). Also, nut butters may contain added sugar and fat which may deter some health professionals from recommending such products. Therefore, more research on the health effects of peanut butter (both natural and containing added fats and sugar) and other nut butters, is required, so that evidence-based recommendations can be developed.
The present study should be interpreted with several limitations and strengths in mind. First, the cross-sectional design means causal inferences cannot be drawn, but information from the study allows for generation of hypotheses for future research. The response rate was 53 %, which is comparable to other mail surveys in Australasia( Reference Lee, Dobson and Brown 46 , Reference Timperio, Cameron-Smith and Burns 47 ), but there remains the possibility that non-responders were different from responders. However, while means, medians and percentages might have been affected by interest in the survey topic, there are no clear reasons why the observed associations would differ between responders and non-responders. While studies investigating response biases in associations specific to health professionals are lacking, previous research has found no evidence for significant biases in associations involving health behaviours in the general public( Reference Martikainen, Laaksonen and Piha 48 – Reference Van Loon, Tijhuis and Picavet 50 ). The majority of respondents were female, which may limit the generalisability of the descriptive results to health professionals in general. However, to ensure that sex was not confounding associations, there was adjustment for sex in regression models whenever possible, along with age and ethnicity as further confounders. All three of these variables were found to be associated with some outcomes. Another limitation is that these professionals were identified based on their occupation description and despite our careful searching, some eligible health professionals will not have been identified either through overly general occupations in the Electoral Roll (e.g. ‘doctor’ or ‘nurse’) or possibly through descriptions that were not identified. The use of the Electoral Roll, rather than directly approaching professional bodies, changed the sampling frame from registered professionals to those with appropriate descriptions for their occupation in the Electoral Roll. While this enabled us to contact potential respondents directly and to send thank you and reminder messages, which are part of Dillman’s approach to maximise survey response and so try to decrease biases from non-response, it is possible that the professionals identified in this way differ systematically from those not so identifiable, although we cannot think of reasons for systematic differences in the outcomes from this beyond the potential confounders included in models (age, sex and ethnicity). A further limitation is that we cannot account for the mixture of patients each profession typically encounters and it is possible that some of the observed differences in responses could be attributable to this. In particular, promoting higher or lower levels of nut consumption could depend on patient characteristics and the current nut consumption levels of these patients, which could vary between general practitioners and practice nurses compared with dietitians. These results may also not generalise to countries with different health-care systems to NZ or to other health-care professions. It is also important to acknowledge that people receive information about nuts from other sources such as the media, nutritionists and public health campaigns, which may also influence nut consumption and potentially the advice they receive from health-care professionals.
A strength of the research was the careful development of the questionnaire to optimise content and face validity, including the involvement of six dietitians, two general practitioners and four practice nurses, as well as one of the co-authors being a registered dietitian. Further, the use of a rigorous mail survey utilising a modified version of Dillman’s tailored design method with a mixed-mode approach resulted in a response rate that was slightly higher than anticipated in the sample size calculations and reduces our concerns about response biases.
Conclusion
The present study provides unique information on the current nut recommendation practices of health professionals in NZ. Dietitians were more likely to recommend nuts in line with current recommendations compared with general practitioners and practice nurses. This is likely to reflect dietitian’s specialised nutrition training, but there are still gaps between the recommendations and dietetic practice. Improving knowledge on the health benefits of nuts among health professionals is likely to influence nut recommendation practices to positively impact nut consumption among the general public, given previous research which suggests that the public would consume more nuts if advised to do so by a doctor. Increasing nut consumption, especially when they are in place of less healthful snacks, is likely to lower the risk of chronic disease. Nurses may be particularly effective in this role given the high levels of trust they have with the public.
Acknowledgements
Acknowledgements: The authors would like to thank the participants for their commitment and enthusiasm in participating in this study. Financial support: This study was supported by internal funds from the Department of Human Nutrition, University of Otago. The funder had no role in the design, analysis or writing of this article. Conflict of interest: None. Authorship: R.C.B., A.R.G. and A.C. formulated the research questions; all authors contributed to the design the study; L.C.Y. was responsible for carrying out the study; R.C.B. and A.R.G. were responsible for analysing the data; all authors contributed to the writing of the manuscript. Ethics of human subject participation: The study was conducted according to the guidelines laid down in the 1964 Declaration of Helsinki and all procedures involving human subjects were approved by the University of Otago Ethics Committee (reference number D14/288).










