Vitamin D is the term used to describe two molecules: ergocalciferol (vitamin D2) and cholecalciferol (vitamin D3). The first of these is derived by ultra-violet irradiation of ergosterol widely distributed in plants and fungi, while cholecalciferol is formed from ultra-violet irradiation on the skin. Serum 25-hydroxvitamin D status (25OHD) is a good clinical indicator of vitamin D health and low 25OHD (<25 nmol/l) has been shown to affect markers of musculoskeletal health( 1 ).
The aim of this study was to further analyse the effectiveness of vitamin D food fortification in subjects with a low baseline 25OHD status (<25 nmol/l). The D2-D3 Study, participants were randomised to receive placebo, 600IU/d vitamin D2 or 600IU/d vitamin D3 for 12-weeks, delivered via fortified foods. Serum 25OHD was measured by liquid-chromatography-tandem mass spectrometry at baseline (wk0), wk6 and wk12. Two groups were included: white Europeans and South Asians (SA). The study was conducted according to the Helsinki Declaration and received full ethical approval.
In total, 335 women completed the study, of which 90 were SA( Reference Tripkovic 2 ). At baseline, 68 (20 %) of women (56 SA: 12 Europeans) presented with low total 25OHD levels (<25 nmol/L). After 12 weeks of supplementation, there was a significant improvement in 25OHD levels from baseline to week 6, and baseline to week 12 in these women randomised to either D2 or D3 supplementation (p < 0·0001 for all; Figure 1). Interestingly, 82 % of the women randomised to the D2 group (biscuit or juice) demonstrated an increase in total 25OHD levels above 25 nmol/L, while 100 % of those in the D3 group showed levels over 25 nmol/L. Subjects randomised to D3 showed significantly higher 25OHD levels than D2 participants at weeks 6 and 12 (p < 0·0001 and p = 0·0006 respectively).
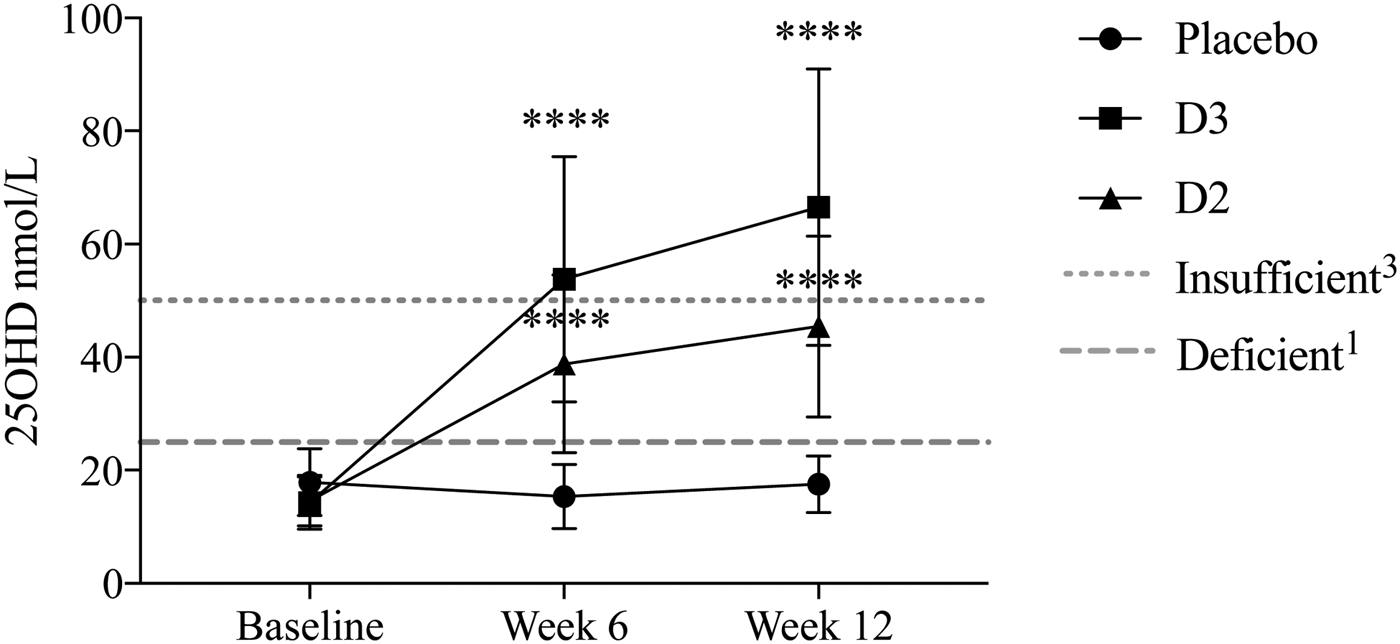
Fig. 1. Serum total 25OHD levels at baseline (n = 68), during the intervention (week 6; n = 48) and the end of the intervention (week 12; n = 43) for participants starting with total 25OHD levels below 25 nmol/L. Data are presented as mean +/− SD
Further characterisation of the diet and lifestyle habits of the study population below 25 nmol/l will be useful for public health strategies to improve the population's vitamin D health.





