Introduction
The 2015 Dietary Guidelines for Americans (DGA)( 1 ) recognises food insecurity, or without ‘consistent, dependable access to enough food for active, healthy living’( Reference Coleman-Jensen, Rabbit and Gregory 2 ) as a special circumstance that can limit an individual’s capacity to choose a healthy diet. The relationship of food security to health and nutritional outcomes among children and adolescents is a concern because of the importance of the paediatric life stage to optimal growth and development, and the establishment of healthy dietary patterns that may be carried to adulthood. Dietary intake is a modifiable risk factor for preventable chronic diseases, including many that originate in childhood( 1 ). Nutrient intake for the preservation of health and prevention of disease in the general US population aged ≥2 years is low enough to be of public health concern for Ca, K, dietary fibre and vitamin D. Fe is also a nutrient of concern for young children and adolescent girls. Dietary shortfalls from certain food groups where these nutrients originate include vegetables, fruits, whole grains and dairy products( 1 ). Additionally, nutrients that are underconsumed by the population, or not consumed in amounts necessary to achieve the Estimated Average Requirement (EAR) or to exceed the Adequate Intake, include vitamins A, E and C, folate and Mg. Na and saturated fat are overconsumed relative to the Tolerable Upper Intake Level( 3 ). Such prevalent dietary shortfall and excess in the general US population may be present in greater magnitude and severity for children living in the 16·5 % of food-insecure US households comprising children and adolescents aged ≤ 18 years in 2016( Reference Coleman-Jensen, Rabbit and Gregory 2 ).
The 8·0 % of households where food insecurity among children was present in 2016 represent direct experiences of undesirable dietary environments( Reference Coleman-Jensen, Rabbit and Gregory 2 ). Food insecurity for these children may potentially lead to suboptimal health status and failure to achieve full genetic potential through a deficient state of general nutrition( Reference Campbell 4 ) or through the lack of an essential supply of key nutrients in the necessary amount, in combination with other key nutrients, at certain time-frames in childhood. Over an extended period of time or at critical times in development this experience may influence nutritional deficiencies, sickness, and un-optimised growth and development.
Nutrient demands for normal child growth are particularly relevant to certain stages, or age ranges, of development as per the basis of six of the twelve Dietary Reference Intake value sets for children aged 0–18 years( 5 ). Additionally, the known dietary intake behaviours of children by age group vary, and present challenges to attaining sufficient nutrients for proper growth and development( Reference Birch, Savage and Ventura 6 – 8 ). Nutrient gaps among all US children begin early and become progressively prevalent and inclusive of more dietary components as children age( 3 , Reference Eicher-Miller, Park and Bailey 9 ). US toddlers and preschoolers aged 1–5 years do not consume enough vegetables and whole grains and a large proportion of this age group do not meet the EAR for vitamins D and E nor exceed the Adequate Intake for dietary fibre. For older children aged 4–8 years, intakes of vitamins D and E, fibre and K are nutrient gaps along with less than recommended amounts of vegetables, whole grains and dairy products. Adolescents face more challenges in meeting nutrient requirements compared with younger age groups. Few consume the recommended amount of fruits, vegetables, whole grains, dairy products and protein foods, especially girls. Larger proportions of adolescent children compared with younger aged children do not meet the EAR for vitamins D, C and A, and Mg and K, and did not exceed the Adequate Intake for fibre. Ca and Fe are also underconsumed among large proportions of this age group and are linked with particularly severe health outcomes including low peak bone mass (linked with high osteoporosis risk in later adulthood) and Fe-deficiency anaemia. The intake of solid fats and added sugars should be limited but intakes for these nutrients along with Na exceed the recommended daily limits for all age groups. In general, evidence suggests that younger US children as a group met dietary requirements or exceeded adequacy more prevalently for a variety of nutrients compared with older or adolescent age groups( 3 , Reference Eicher-Miller, Park and Bailey 9 ). Food-insecure children are included in these findings, but, as a subpopulation, may experience additional dietary gaps and excesses due to the restricted resources that food-insecure households have to acquire food, and the need for families to economise.
Classification of food insecurity is tied to having enough resources for food. The United States Household Food Security Survey Module (US HFSSM)( Reference Gary, Nord and Price 10 ) quantifies food security and includes eighteen items querying the experiences or behaviours related to meeting household food needs in the past 12 months. Responses to these questions by or for household adults, household children, or certain individuals may yield different classifications of food security within a household. Eight questions in the US HFSSM specifically refer to children in the household and may be used independently to quantify food insecurity among all household children or for individual children. Classification may be as a continuous score or category: high food security when no difficulty accessing food exists; marginal food security when anxiety about having enough food is present; low food security when normal dietary intake is altered in quality or variety; and very low food security when dietary intake is reduced and disrupted eating patterns are present( Reference Gary, Nord and Price 10 ).
The unique experience of food insecurity among household individuals is linked to the management of food insecurity and the potential reservation of food for certain individuals or shift in allocation of resources as they become more restricted. Children may be shielded from reduced food intake by their parents and have little reduction in the types and amounts of food consumed while residing in a food-insecure household( Reference Radimer, Olson and Greene 11 ). Not all households demonstrate similar or equivalent effectiveness in shielding children from food insecurity but a recent review supports the conclusion that parents effectively shield children from the full potential severity of compromised dietary quality because of food insecurity( Reference Hanson and Connor 12 , Reference Carlson, Andrews and Bickel 13 ). Even when child-specific questions are used to quantify food security, the classification of a particular child compared with all the children or the entire household may be very different depending on the household member relationships and other circumstances. These varying experiences, in light of varying nutritional needs of children at different stages of growth, highlight the importance of determining the most direct link of individual food access with individual dietary or health outcome.
A previous review( Reference Hanson and Connor 12 ) has determined evidence for lower dietary quality among food-insecure children as a group. However, evaluation of the evidence for a relationship of food insecurity with key nutritional outcomes for the specific stages of child growth among children has not been completed despite the nutrient demands of growth and general sub-par dietary intake of US children by age group, nor has there been a synthesis of the literature to determine evidence for the paediatric age stage where food insecurity may have the most negative impact on child dietary intake. Such information will inform federal nutrition programmes of the specific dietary components and age groups where interventions may be directed to make the largest improvements in child food security and nutrition. The objective of the present critical, narrative review was to provide a review and discussion of the strength of the current epidemiological evidence for food insecurity to be related to less desirable dietary intake compared with food security for key food groups, dietary components and nutrient intake and meeting or exceeding recommendations by age subgroup (1–5 years; 6–11 years; and 12–19 years). Results are focused on the food groups, dietary components and nutrients most important for child health and also those where requirements are less prevalently met, referred to as key nutritional outcomes (Table 1). The investigation also aimed to determine the age group where food insecurity may have the most negative dietary impact. Appraisal of the relationships was assessed by consideration of the Bradford Hill criteria( Reference Hill 14 ), or criteria used to judge the evidence for causality in hypotheses and associations shown in scientific research. The Bradford Hill criteria have frequently been applied in health behaviour research including dietary outcomes( Reference Biddle, Bennie and Bauman 15 – Reference Finck, Hart and Jennings 17 ) but not previously to outcomes related to food security. The criteria may not unconditionally confirm the presence or absence of a specific relationship but are helpful tools to understand associations of exposure–health outcomes. The strength of the association, consistency, temporality and dose–response aspects of the relationship are key factors relevant to assessing a basis for explaining the reasons or causes that are relevant to population observations( Reference Biddle, Bennie and Bauman 15 ). Additional considerations include biological plausibility, specificity, coherence, experimental evidence and analogy. Epidemiological evidence alone may not address biological plausibility and coherence, and experimental evidence from a randomised controlled trial may not be ethical when applied to the relationship of food insecurity with dietary outcomes. Thus, the present review includes discussion of:
(1) Strength of association: the magnitude of association between food insecurity and dietary outcomes and determination of meaningful differences in dietary intake for food-secure and -insecure children of various age groups.
(2) Consistency: the repeated similar finding for relationships of food insecurity and dietary intake across different populations in different settings.
(3) Dose–response: exposures of lower food security or for chronic duration lead to more severe dietary inadequacy while experiences of marginal food security and shorter duration lead to less dietary inadequacy.
(4) Aspects of temporality: the presence of food insecurity exposure in advance of dietary gaps (summarised in the Discussion).
(5) Aspects of specificity: the sensitivity of food-insecurity measures used to quantify food insecurity in relationship to the assessment of dietary intake (summarised in the Discussion).
Table 1 Key nutritional outcomes for child health on the basis of their prevalence of over- or under-consumption in the USA and/or the risks posed to each child age group when over- or under-consumed

DGA, Dietary Guidelines for Americans, 2015; EAR, Estimated Average Requirement; AI, Adequate Intake; UL, Tolerable Upper Intake Level.
Methods
Studies were systematically retrieved and identified in order to comprehensively capture all relevant work. The review content of the present study, however, was narrative in approach. An electronic search of the PubMed database (www.ncbi.nlm.nih.gov/pubmed), Purdue University Library database (www.lib.purdue.edu/) and Google Scholar (scholar.google.com) was completed. Records indexed up to January 2017 were included and the search process adhered to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) statement( Reference Moher, Liberati and Tetzlaff 18 ). Search inclusion criteria included ‘US children and adolescents’, ‘food insecure’, ‘food insecurity’, ‘food secure’, ‘food security’, and proxy terms ‘food insufficient’, ‘food insufficiency’, ‘food sufficient’, ‘food sufficiency’, ‘dietary intake’, ‘nutrient deficiency’, ‘nutrient adequacy’ and ‘nutrient gaps’. Secondary searches were performed by searching reference lists of all identified articles. To be included in the present review, research needed to be original research work, fully or partially conducted in the USA among separate children and adolescent growth-stage age groups within the span of 1–19 years. Studies that were not focused on a relationship of food insecurity with diet (for example, studies which focused on assessing how income may relate to nutrition, or examining benefits of federal or state nutrition assistance programmes) and/or specifically not on key nutritional outcomes (Table 1), studies conducted outside of the USA, studies that assessed the child food-insecure experience using tools other than specific food-security assessment tools (for example, using low income as a proxy measure for food insecurity) such as the US HFSSM( Reference Gary, Nord and Price 10 ), and studies including all children (1–19 years) analysed together were also excluded. All articles meeting the criteria were evaluated based on their contributions to address the Bradford Hill criteria( Reference Hill 14 ), in three metrics: (1) strength of association; (2) consistency; (3) dose–response. Criteria were applied in order to objectively identify and evaluate the status and gaps in the evidence for the relationship of food insecurity as a predictor of key child nutritional outcomes that were determined based on their prevalence or risks posed to each child age group (Table 1) as per the DGA( 1 ), and other resources( 3 , 5 – Reference Eicher-Miller, Park and Bailey 9 ). Application of the DGA was also consistent with use of the DGA in many of the included studies where ‘meeting recommendations’ was imposed as a cut-off criterion.
Findings from identified studies often described dietary outcomes that were not considered key nutritional outcomes for the purposes of the present paper. However, these outcomes are shown along with the key nutritional outcomes (Tables 2–7) in order to provide the full context of each study. Terms used to classify key dietary outcomes as desirable or not (Table 1) included ‘food groups or dietary components to increase’ and referred to vegetables, whole grains, dairy products, fruits, and meat or protein foods( 1 ). The outcomes ‘total vegetables and fruit’, ‘Healthy Eating Index Fruit and Vegetable score’ and ‘5-A-Day Vegetable Score’ were counted as outcomes for vegetable intake in the included studies. Similarly, ‘milk’ was considered an outcome for dairy product intake due to prevalent contributions( 1 ). ‘Nutrients to increase’ included dietary fibre, K, Fe, Ca, Mg, vitamins A, E, C and D, and ‘nutrients or dietary components to decrease’ were solid fat, added sugars and Na. ‘Energy from saturated fat’ and ‘saturated fat’ were considered outcomes of solid fats and ‘soda’, ‘sweetened beverages’, ‘sweetened beverage score’, ‘candy and cookies’, ‘sugar’ and ‘energy from added sugar’ were considered outcomes of added sugar intake as per their contributions to US added sugar intake( 1 ).
Table 2 Summary of research location and participants for studies evaluating food insecurity and key dietary outcomes among US children aged 1–5 years
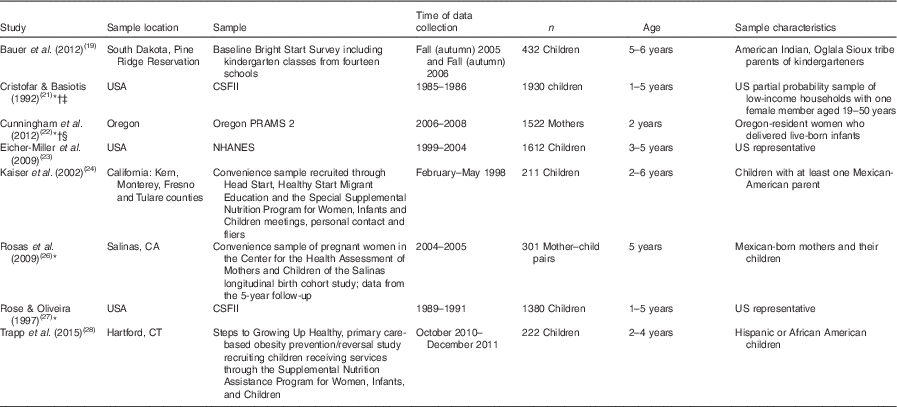
CSFII, Continuing Survey of Food Intakes by Individuals; Oregon PRAMS 2, Oregon Pregnancy Risk Assessment Monitoring System follow-back survey; NHANES, National Health and Nutrition Examination Survey.
* Study where result of less desirable dietary intake was associated with food insecurity.
† Consistency.
‡ Dose–response.
§ Strength.
Table 3 Summary of research location and participants for studies evaluating food insecurity and key dietary outcomes among US children aged 6–11 years

NHANES, National Health and Nutrition Examination Survey.
* Study where result of less desirable dietary intake was associated with food insecurity.
† Strength.
‡ Consistency.
Table 4 Summary of research location and participants for studies evaluating food insecurity and key dietary outcomes among US children aged 12–19 years
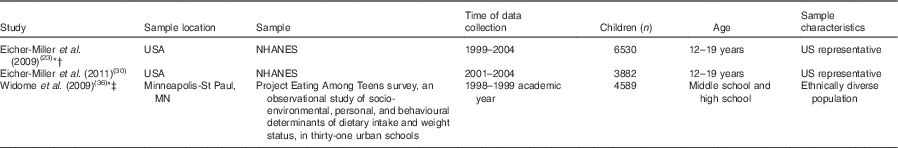
NHANES, National Health and Nutrition Examination Survey.
* Study where result of less desirable dietary intake was associated with food insecurity.
† Strength.
‡ Dose–response.
Table 5 Summary of research measures and results for studies evaluating food insecurity and key dietary outcomes among US children aged 1–5 years
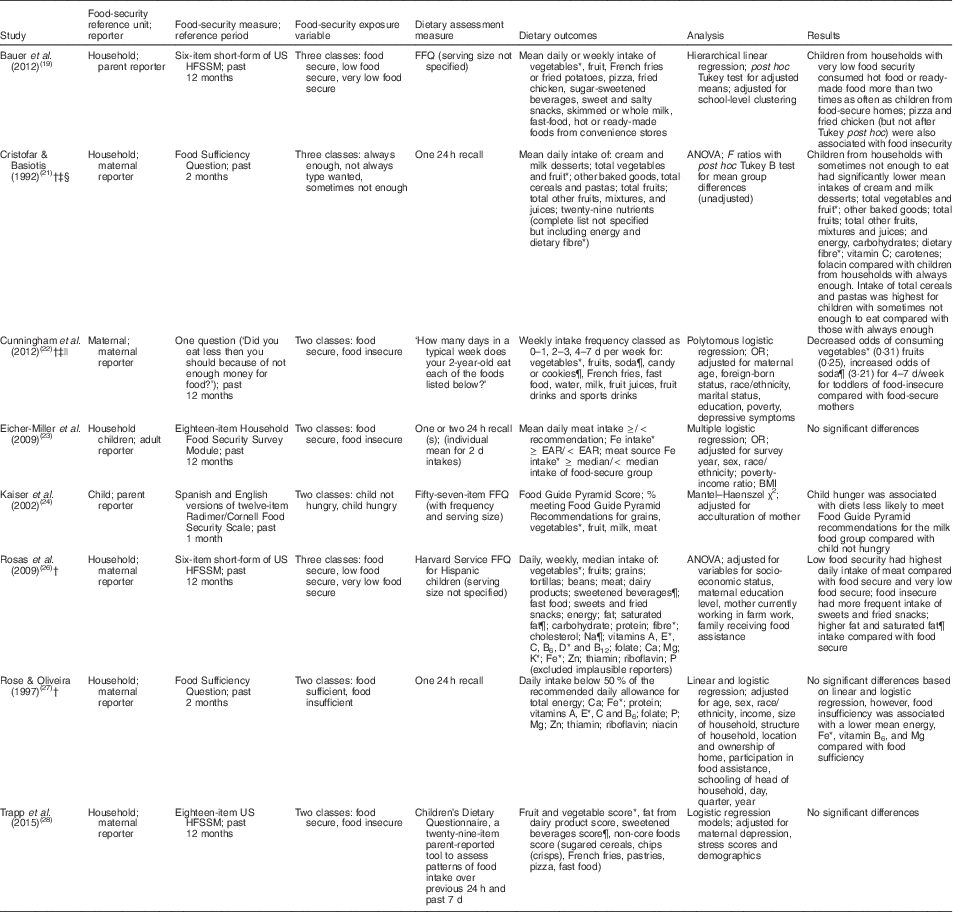
EAR, Estimated Average Requirement; US HFSSA, United States Household Food Security Survey Module.
* Key food groups or dietary components to increase for children aged 1–5 years.
† Study where result of less desirable dietary intake was associated with food insecurity.
‡ Consistency.
§ Dose–response.
|| Strength.
¶ Key food groups or dietary components to decrease for children aged 1–5 years.
Table 6 Summary of research measures and results for studies evaluating food insecurity and key dietary outcomes among US children aged 6–11 years
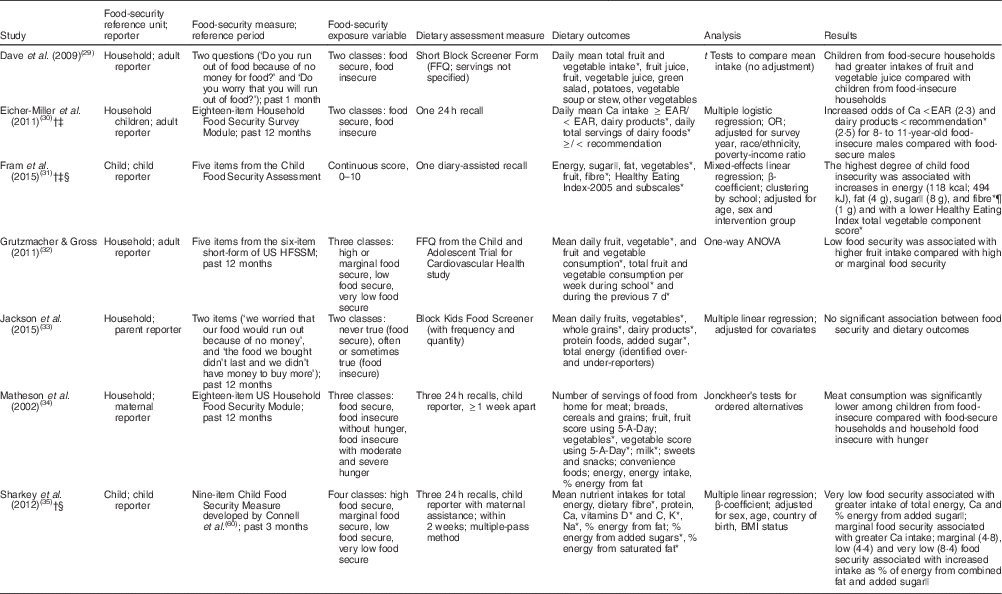
EAR, Estimated Average Requirement; US HFSSM, United States Household Food Security Survey Module.
* Key food groups or dietary components to increase for children aged 6–11 years.
† Study where result of less desirable dietary intake was associated with food insecurity.
‡ Strength.
§ Consistency.
|| Key food groups or dietary components to decrease for children aged 6–11 years.
¶ Unexpected result of a key dietary component related to food security.
Table 7 Summary of research measures and results for studies evaluating food insecurity and key dietary outcomes among US children aged 12–19 years
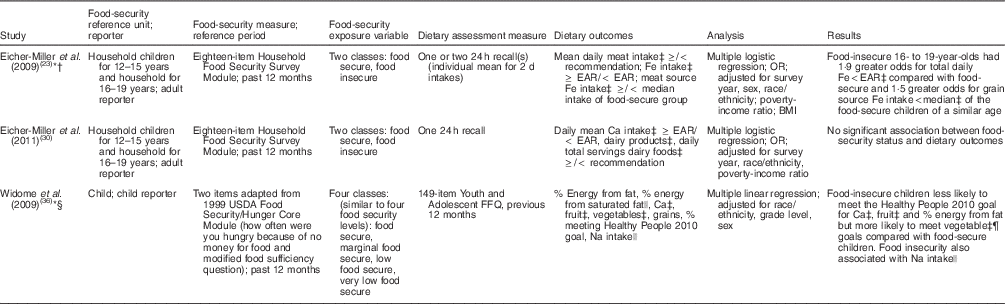
EAR, Estimated Average Requirement; USDA, US Department of Agriculture.
* Study where result of less desirable dietary intake was associated with food insecurity.
† Strength.
‡ Key food groups or dietary components to increase for children aged 12–19 years.
§ Dose–response.
|| Key food groups or dietary components to decrease for children aged 12–19 years.
¶ Unexpected result of a key dietary component related to food security.
The review is ordered according to age group: evidence for toddlers and preschoolers (aged 1–5 years) first, followed by children (aged 6–11 years), and, finally, adolescents (aged 12–19 years). Identified studies were assigned to one of the three age groups specified for the present study when the age group was inclusive of the study sample or did not extend ≤1 year. Various aspects of the studies that are relevant to the Bradford Hill criteria included the study design, sample size, location, time period of data collection, participant age range, participant race/ethnicity, unit of measure for food-security classification, method of food-security classification, food-security variable structure, dietary assessment, dietary outcome, analytical methods and results (Tables 2–7).
Results
The search strategy identified eighteen studies evaluating relationships between food insecurity and nutritional outcomes among US children and adolescents( Reference Bauer, Widome and Himes 19 – Reference Widome, Neumark-Sztainer and Hannan 36 ) and sixteen studies that evaluated key nutritional outcomes among child age groups (Tables 2–7)( Reference Bauer, Widome and Himes 19 , Reference Cristofar and Basiotis 21 – Reference Kaiser, Melgar-Quinonez and Lamp 24 , Reference Rosas, Harley and Fernald 26 – Reference Widome, Neumark-Sztainer and Hannan 36 ). The number of studies evaluating relationships decreased with age: eight studies included the youngest children aged 1–5 years (Tables 2 and 5)( Reference Bauer, Widome and Himes 19 , Reference Cristofar and Basiotis 21 – Reference Kaiser, Melgar-Quinonez and Lamp 24 , Reference Rosas, Harley and Fernald 26 – Reference Trapp, Burke and Gorin 28 ), seven studies included children aged 6–11 years (Tables 3 and 6)( Reference Dave, Evans and Saunders 29 – Reference Sharkey, Nalty and Johnson 35 ), and three studies included adolescents aged 12–19 years (Tables 4 and 7)( Reference Eicher-Miller, Mason and Weaver 23 , Reference Eicher-Miller, Mason and Weaver 30 , Reference Widome, Neumark-Sztainer and Hannan 36 ).
Children aged 1–5 years
Studies among very young children numbered the most compared with the other age groups and included eight cross-sectional studies evaluating key nutritional outcomes: vegetables; fibre; Fe; vitamins D, E and K; solid fats; Na; and added sugars. Whole grain intake was a key outcome that was not evaluated. Four of the eight studies found food insecurity significantly associated with less desirable intake of the key nutrients( Reference Cristofar and Basiotis 21 , Reference Cunningham, Barradas and Rosenberg 22 , Reference Rosas, Harley and Fernald 26 , Reference Rose and Oliveira 27 ) and four of the studies found null results( Reference Bauer, Widome and Himes 19 , Reference Eicher-Miller, Mason and Weaver 23 , Reference Kaiser, Melgar-Quinonez and Lamp 24 , Reference Trapp, Burke and Gorin 28 ). Among studies describing significant relationships, food insecurity was associated with lower mean intakes and odds of consuming vegetables( Reference Cristofar and Basiotis 21 , Reference Cunningham, Barradas and Rosenberg 22 ), lower mean fibre( Reference Cristofar and Basiotis 21 ) and Fe( Reference Rose and Oliveira 27 ) in three studies, and more frequent intake of saturated fat( Reference Rosas, Harley and Fernald 26 ) and higher odds of consuming soda( Reference Cunningham, Barradas and Rosenberg 22 ) in two studies when compared with food security.
Evidence regarding strength was demonstrated most clearly among 2-year-old Oregon children living in households of mothers who were food insecure in the past 2 months from 2006 to 2008; the children had decreased odds of consuming vegetables (0·31) and increased odds of consuming soda (3·21) for 4–7 d/week compared with their peers living in households of food-secure mothers( Reference Cunningham, Barradas and Rosenberg 22 ). The magnitude of this association (0·31) was strong (OR 0·1–0·4 to 3·0–10·0 indicates strong association)( Reference Monson 37 ) within the context of epidemiological research. The four additional studies( Reference Bauer, Widome and Himes 19 , Reference Kaiser, Melgar-Quinonez and Lamp 24 , Reference Rosas, Harley and Fernald 26 , Reference Trapp, Burke and Gorin 28 ) that evaluated fruit and vegetable intake, but did not find significant results, were smaller-scale studies in geographically bound locations among specific race/ethnic subpopulations. Evidence contributing to consistency is shown when the significant results for vegetable intake( Reference Cunningham, Barradas and Rosenberg 22 ) are taken with a similar finding of lower mean intake of total fruits and vegetables among US children aged 1–5 years living in households that were food insecure in the past 2 months from 1985 to 1986 compared with children in food-secure households( Reference Cristofar and Basiotis 21 ). Dose–response evidence may be shown when there are at least three levels of food security or the continuous food-security score used and consistent increases or decreases in intake are determined from low to high food security. Cristofar & Basiotis( Reference Cristofar and Basiotis 21 ) contributed dose–response-related findings from their analysis of US children aged 1–5 years in 1985–1986. Children who ‘always had enough and the kind I wanted’ over the past 2 months had the highest mean intake of total vegetables and fruit compared with lower intakes for those with ‘not always the types of foods they wanted’, and even less for those with ‘sometimes not enough’ food( Reference Cristofar and Basiotis 21 ). Finally, evidence contributing to dose–response was also shown among US children 5 years old of Mexican-born mothers living in Salinas, California in 2004–2005 when median intakes of saturated fat consistently decreased across food secure, low food secure, and very low food secure in the past 12 months( Reference Rosas, Harley and Fernald 26 ).
Children aged 6–11 years
The seven cross-sectional studies addressing key dietary components and nutrients of special concern in this age group included outcomes of vegetables, whole grains, dairy products, vitamin D, fibre, K, solid fat, added sugar and Na (Tables 3 and 6)( Reference Dave, Evans and Saunders 29 – Reference Sharkey, Nalty and Johnson 35 ). Vitamin E is a key nutrient of concern that was not evaluated. Food insecurity was related to lower odds for meeting the DGA recommendation for dairy products( Reference Eicher-Miller, Mason and Weaver 30 ) and a lower Healthy Eating Index total vegetable score( Reference Fram, Ritchie and Rosen 31 ) in two studies and higher sugar intake( Reference Fram, Ritchie and Rosen 31 ), percentage energy from added sugar, and percentage energy from fat and sugar in two studies( Reference Sharkey, Nalty and Johnson 35 ) compared with food security. Four of the studies did not determine significant differences in key dietary outcomes among food-security groups( Reference Dave, Evans and Saunders 29 , Reference Grutzmacher and Gross 32 , Reference Jackson, Smit and Manore 33 , Reference Matheson, Varady and Varady 34 ). Strength of association was provided by the finding of 2·5 greater odds for 8- to 11-year-old US males of households with food insecurity among children in 2001–2004 to be less likely to meet dairy product intake recommendations compared with males from households with food security among children( Reference Eicher-Miller, Mason and Weaver 30 ). A study by Fram et al. ( Reference Fram, Ritchie and Rosen 31 ) also contributed a finding toward strength in results of an approximate 0·03 lower Healthy Eating Index vegetable score (on a 0–5 unit scale) for each 1-unit decrease in child food-security score (on a scale of 0–10). This difference translates to an approximate 0·3 cups difference between child food security (score=0) and very low food security (score=10). Such a decrease in vegetable intake over time would be biologically meaningful as it would represent 20 % of the recommendation for vegetable consumption among this age group (1·5 cups)( 1 ). The sample was recruited from an ethnically diverse low-income subpopulation with a large proportion of Latino and Hispanic ethnicity living in San Diego, CA, in 2012 and included children aged 9–11 years( Reference Fram, Ritchie and Rosen 31 ). The finding of 8 g more sugar intake for the food-insecure compared with the food-secure children in the sample also contributed to evidence of strength( Reference Fram, Ritchie and Rosen 31 ). Consistency of evidence was demonstrated when the finding for greater sugar intake is taken with the results of a different child sample described by Sharkey et al. ( Reference Sharkey, Nalty and Johnson 35 ) showing that very low food security reported by children was associated with a greater mean intake of percentage energy from added sugar compared with food-secure children in a 6- to 11-year-old participant sample from highly deprived neighbourhoods in Hidalgo County, TX, from March to June 2010( Reference Sharkey, Nalty and Johnson 35 ). Evidence for a dose–response relationship was not found.
Children aged 12–19 years
Very few studies contributed evidence for a relationship between key dietary outcomes and food security among adolescents aged 12–19 years compared with younger child age groups (Tables 4 and 7). Evaluation of vegetable, dairy product, fruit, protein foods, Ca, Fe, solid fat and Na outcomes were completed( Reference Eicher-Miller, Mason and Weaver 23 , Reference Eicher-Miller, Mason and Weaver 30 , Reference Widome, Neumark-Sztainer and Hannan 36 ) but whole grains, vitamins D, E, C and A, fibre, K, Mg and added sugars were not evaluated as outcomes despite being key dietary components among this age group. Findings of less desirable dietary intake among food-insecure compared with food-secure children were determined in two( Reference Eicher-Miller, Mason and Weaver 23 , Reference Widome, Neumark-Sztainer and Hannan 36 ) of the three studies and null results were found in one study( Reference Eicher-Miller, Mason and Weaver 30 ). Lower odds of meeting the EAR for Fe and grain-source Fe intake( Reference Eicher-Miller, Mason and Weaver 23 ) along with less likelihood of 2010 Healthy Individuals Goals for Ca and fruit goals( Reference Widome, Neumark-Sztainer and Hannan 36 ) were observed for food-insecure compared with food-secure adolescents. Evidence of strength was contributed by the finding of US-representative adolescents aged 16–19 years from households with food insecurity among children in 2001–2004 having 1·5 greater odds for grain-source Fe intake to be less than the median of the food-secure group and 1·9 greater odds of total Fe intake being less than the EAR( Reference Eicher-Miller, Mason and Weaver 23 ). Consistency of evidence for any dietary outcome was not found among the various study results for this age group. Findings contributing to evidence of a dose–response relationship of decreasing food security with increasingly negative dietary outcomes were added by the estimation of increasingly lower proportions, by food-security status, of middle and high school children from an ethnically diverse sample in Minneapolis and St Paul, Minnesota, meeting the Ca intake goal( Reference Widome, Neumark-Sztainer and Hannan 36 ).
Discussion
Children aged 1–5 years
Only among children aged 1–5 years was evidence of a specific dietary outcome, less desirable fruit and vegetable intake, related to food insecurity, contributed for all three criteria: strength, consistency and dose–response. These results of lower fruit and vegetable intake among very young food-insecure compared with food-secure children are of concern because of the rich dietary contributions that these foods make to promote short-term and long-term health and development in young children( 1 , 3 , 8 ) and the already low intake of US food-secure children( 1 , Reference Eicher-Miller, Park and Bailey 9 ). Furthermore, the establishment of self-feeding dietary patterns and exposure to fruits and vegetables at this young age promote preference for these foods into adulthood( Reference Birch, Savage and Ventura 6 , Reference Carruth, Ziegler and Gordon 38 ). Parents influence child eating behaviour by selecting food for family members, serving as models for dietary choices and patterns, and by establishing feeding practices and patterns for children( Reference Birch, Savage and Ventura 6 ). When families and adults are in a restricted food-insecure environment, establishment of preferences, practices and dietary patterns among children may be altered due to changes in all of these aspects and ultimately influence future dietary intake. For example, adults in food-insecure households consumed fewer vegetables and fruits as evidenced by a review of the literature( Reference Hanson and Connor 12 ); the modelling of such behaviour for food-insecure children along with their own reduced intakes compared with food-secure children may further contribute to future non-preference for these foods and the establishment of patterns promoting lifelong reduced daily intakes of fruits and vegetables.
Children aged 6–11 years
The compiled evidence for less desirable dietary intake among children aged 6–11 years included strong results of less desirable vegetable intake associated with food insecurity, similar to the main finding for very young children. The continued significant association of food insecurity with this outcome among 6- to 11-year-old children shows a consistent dietary pattern among very young and school-aged children related to food insecurity. Vegetable intake was the most commonly investigated outcome among the seven studies and among all child age groups, so perhaps it is unsurprising that relationships were most robustly established for this outcome. However, a decrease in this dietary outcome may also be particularly provoked in situations of food insecurity among children. The likelihood for families to experience chronic food insecurity over multiple extended years spanning the ages of 1–11 years of childhood is low( Reference Ryu and Bartfeld 39 , Reference Wilde, Nord and Zager 40 ), suggesting that the dietary patterns related to food insecurity may not be consistent throughout childhood. However, early experiences of food insecurity and less vegetable access and acceptance during this stage where establishment of dietary preferences occurs, as described earlier, may be maintained in older children who have experienced food insecurity. Even among those for whom the experience of food insecurity is new, there may be little resistance to an altered dietary pattern including lower vegetable intake. Strong evidence of lower dairy product in addition to lower vegetable intake among food-insecure compared with food-secure 6- to 11-year-old children may facilitate greater added sugar intake when vegetables and foods such as milk are replaced with high-sugar foods like sweetened beverages. Such dietary trends have been observed among all children in this age group( Reference Gentry, Piernas and Popkin 41 ) but may be heightened when access to food is limited and enhance the potential for developing negative health outcomes in childhood, adolescence or later adulthood. Nutrition-related health concerns particularly related to vegetable intake at this life stage are obesity, atherosclerosis rooted in childhood and related to elevated risk for CVD in adulthood, hypertension contributing to the development of CVD and type 2 diabetes, and the development of dental caries( 7 ).
Children aged 12–19 years
Adolescents aged 12–19 years were the least studied group and present an opportunity for future research as evidenced by the low number of only three studies. The lack of studies among adolescents is notable compared with other groups, especially considering the perhaps heightened prevalence of significant findings (two out of three studies or 67 %). This age-related phenomenon for dietary disparities follows the general US child population trend of nutrient gaps that become more numerous and more prevalent with age( Reference Eicher-Miller, Park and Bailey 9 ). In the US population these trends are linked with sex, especially among adolescents; older adolescent females have even less likelihood to meet dietary recommendations and gaps which are more prevalent for this sex compared with males. Sex stratification of dietary outcome analysis by food-security status among adolescents has been rarely done( Reference Eicher-Miller, Mason and Weaver 30 ) and is a future research need.
Adolescents are at a time of increased growth velocity and progressing toward independence in establishing their own dietary patterns and habits; thus dietary choices during this time are critical for adult health( Reference Birch, Savage and Ventura 6 , 7 ). The food-insecure context presents additional challenges for obtaining a healthy diet for adolescents. The phenomenon of younger children being more protected from food insecurity than their older siblings and adults within the same households may manifest in differential access to ‘healthy’ foods and greater exposure and burden to the food-insecure experience among adolescents compared with younger children in the household. Adolescents in food-insecure households may obtain foods outside of the household or rely on their own resources in order to minimise their use of household foods( Reference Fram, Frongillo and Jones 42 ). In addition to the nutrition-related health concerns noted for children aged 6–11 years, additional concerns for children aged 12–19 years include progression of developing risk factors for the metabolic syndrome, poor bone health, and Fe deficiency for females at menarche. Osteoporosis is a disease rooted in adolescence; accumulation of peak bone mass occurs during the teenage years. Intake of recommended amounts of Ca and other bone-promoting nutrients and dietary components are especially important for adolescent children. Females’ menstruation may deplete body Fe sources and highlights the need for consuming recommended Fe intakes( 3 , 7 , 8 ). The strong evidence of total Fe less likely to meet the EAR and less Fe intake from grains among food-insecure compared with food-secure adolescents added to dose–response evidence of lower proportions of children meeting the Ca goal as food insecurity increases, indicates dietary conditions preceding immediate and future potential chronic health disparities. These strong and dose-responsive findings, the importance of the adolescent stage to adult health, nutrient gaps in the US population among this age group, vulnerability of older children in a food-insecure household, minimal studies including food-insecure adolescents and prevalence of significant results, justify adolescents aged 12–19 years as the age group where food insecurity may have the most negative dietary impact. Future studies focusing on the key dietary components identified in the present review and especially those that were not evaluated among this age group are valuable to inform interventions aimed at improving diet and health among adolescents.
Limitations
No included studies documented power calculations for prioritised dietary outcomes by food-security status; thus power to detect significant relationships is not known and may not be adequate. Results for all ranges of food security are often lacking in studies, perhaps due to the difficulty of obtaining a large enough sample size to separately analyse marginal, low and very low food security. Dichotomisation of food security impedes dose–response evidence of decreasing quality and variety with increasing food insecurity and less energy intake overall for very low food security. In addition, significant differences across food-security levels are weaker compared with testing between categories adjusted for multiple comparisons. Adjustment for multiple comparisons when a panel of dietary outcomes was completed would strengthen the results.
Temporality
Temporality is another of the Bradford Hill criteria important for evaluating relationships of exposures to outcomes. All of the studies identified were cross-sectional so the ability to determine whether food insecurity preceded less desirable dietary intake, or even if changes in dietary intake occurred as food-security status changed, was not possible. Assessment of food insecurity and dietary outcomes in the studies were self-reported and reflective of different time periods, but usually overlapping. Food security was reported over the previous 1 to 3 months or over the past 12 months. In contrast, dietary intakes were usually collected based on FFQ with reflection periods of past weeks, past month, or year and dietary recall(s), based on the intake in the past 24 h. FFQ allow more consistent time overlap with food-security measures but present more systematic bias as participants are requested to estimate their dietary intake over large periods of time. In contrast, 24 h dietary recalls have less inherent systematic bias because the period of reflection is shorter and participants are not asked to estimate intake but rather just report what they ate( 43 ). Sometimes multiple recalls were used, but these were still usually limited to a few days over the span of 1 week. A limitation of dietary assessment methods used in the studies was that the collected dietary information may not reflect an unbiased usual dietary intake over the specified time period; moreover, whether nutrient deficiency is transient or repetitive may result in varying influence on nutritional outcomes. The National Cancer Institute method( Reference Tooze, Kipnis and Buckman 44 ) or a similar statistical adjustment may be applied to two or more dietary assessments (two 24 h recalls or one 24 h recall and a FFQ) to estimate usual dietary intake and mitigate some of the bias inherent in the assessment of dietary intake, and is recommended in future studies. Temporality may be established when changes from food security to food insecurity precede changes in dietary quality and both measures accurately reflect the time period of assessment. Moreover, evidence for temporality would be strengthened using cohort studies that follow low-income, food-secure children over time to ultimately compare those who become food insecure with those who maintain food security and how these changes are related to dietary intake. Dietary outcomes should be quantified at several time points in order to better match the classification of diet with food insecurity over the past 12 months. Despite the lack of logical basis for the counterfactual case where less desirable dietary intake causes food insecurity, evidence from longitudinal study designs would strengthen a causal link of food insecurity to negative dietary outcomes.
Specificity
Few studies provided evidence for specificity of child food insecurity to be related to certain less desirable dietary outcomes, by assessing the child-specific experience of being food insecure( Reference Eicher-Miller, Mason and Weaver 23 , Reference Kaiser, Melgar-Quinonez and Lamp 24 , Reference Eicher-Miller, Mason and Weaver 30 , Reference Fram, Ritchie and Rosen 31 , Reference Sharkey, Nalty and Johnson 35 , Reference Widome, Neumark-Sztainer and Hannan 36 ). Most studies quantified a more indirect measure of food insecurity, household food insecurity or parent’s food-insecure experience, a classification that may be removed from the child’s actual dietary experience depending on how resources are managed in the household. Assessment of child-specific food security is most comparable with child-specific dietary intakes so existence of dietary differences by food-security status may be more likely to be found when child food security is classified. Similarly, adolescent self-report of food insecurity is more direct compared with household adult proxy report for the household adolescents or individual adolescent. Only three studies included classification of food-security status based on child or adolescent self-report( Reference Fram, Ritchie and Rosen 31 , Reference Sharkey, Nalty and Johnson 35 , Reference Widome, Neumark-Sztainer and Hannan 36 ). Children and adolescents may perceive and report their experience of food insecurity differently from parents. If so, responses to the US HFSSM by parents may under-report food security because of parent assumptions that adolescents are more food secure then they actually are. Parents may also under-report due to social pressure to indicate more food security for adolescents in their household than actually exists. Studies further evaluating the existance of under-reporting by adult proxy compared with direct child and adolescent assessment for food security are needed to better understand the evidence within the context of the food-security relationship to dietary outcomes.
Other considerations
Investigation of dietary under- and over-reporting in food-insecure children of all age groups should also be pursued in order to determine if the prevalence and extent of this phenomenon is similar among food-secure children and the implications for dietary comparisons among these groups. In the present review, only two studies made identification of under- and over-dietary reporting( Reference Jackson, Smit and Manore 33 ) or implausible intakes( Reference Rosas, Harley and Fernald 26 ). Under- and over-reporting of dietary intake have a potential to manifest differently compared with a general population or high-income sample of children due to the social desirability and guilt that may motivate proxy or self-reported dietary assessment responses in the restrained setting of food insecurity. Parent reporters may over-report child intakes, especially for older children, because of the guilt associated with inability to provide enough food for children to eat. However, under-reporting may present bias among parents who are unaware of foods that the child consumes outside of the household. Inclusion of a biomarker in such studies would allow calibration or quantification of bias inherent to self-reported dietary assessment.
Future studies should also include dietary supplements in the quantification of nutrient assessment; currently no studies have assessed nutrient intake from supplements and foods among food-insecure children. Dietary supplement inclusion would allow for a more complete picture of nutrient intake among this group in comparison with food-secure children. Further, the effect of an early exposure to food insecurity on later dietary and health outcomes is not known. Longitudinal studies investigating the relationship of food-insecure experience at an early life-stage with later life dietary and health outcomes are critical to determine the potential lasting impact of food insecurity. Finally, future studies should expand to investigate the specific foods, rather than food groups, that food-insecure children may frequently consume and the potentially diverse frequently consumed foods of food-insecure subpopulations. These studies would identify foods that may be ideal for inclusion in interventions.
Food security, as a situation where access to food and resources to obtain food are limited, may have seemingly obvious consequences to be negatively associated with dietary intake. However, a challenge to this logic is presented by potentially confounding circumstances and related exposures such as poverty, poor dietary choices in the general population, and others. Adjustment for related factors may be applied through the modelling of these relationships in order to improve the probability that the relationships observed between the food-security exposure and the dietary or health outcome are not due to another factor. Many of the included studies adjusted for potential confounders; however, endogeneity may still be an inherent problem as there may be unquantified characteristics that present bias and could have affected the relationships( Reference Guendersen and Kreider 45 ).
Adjustment for potential confounding is important; however, future studies should thoughtfully consider each evaluated relationship individually and prioritise adjustment for essential factors. Caution must be taken not to over-adjust for the factors that constitute and define food security. In particular for dietary studies, adjustment for income and energy when dietary intake is an outcome may threaten a significant independent relationship with food insecurity. Adjustment of energy is usually made to ensure that the dietary component of interest is truly compared without confounding by high energy intake related to overweight or obesity. Similarly, adjustment for income is usually made to ensure that differences in a food-secure and food-insecure situation are independent of income. Both of these factors may be potential confounders but they may also be inherently linked with the construct of food insecurity. Lack of resources for obtaining foods and less dietary intake are defined as very low food security so adjustment for both of these factors in modelling may undermine relationships with food security. Sensitivity analysis may be one way to evaluate their inclusion to identify the best model.
Conclusion
The current body of evidence, despite the noted gaps, is strong, consistent, and provides evidence of dose–response in findings of food insecurity related to sub-par intake of vegetables as a key dietary outcome among children aged 1–5 years and is strong and consistent for added sugars among children aged 6–11 years. Synthesis of the studies reviewed and dietary needs of adolescents aged 12–18 years indicate that this stage of growth may be particularly vulnerable to the dietary environment of food insecurity. The role of dietary intake in relationship to negative health outcomes in the food-insecure context is unclear but hypothesised to modify their risk. Longitudinal cohort studies may clarify the pathway linking food-insecure dietary intake to negative health outcomes among children following Campbell’s conceptual hypothesis( Reference Campbell 4 ); key reviews show food insecurity associated with negative health outcomes among children( Reference Larson and Story 46 , Reference Gundersen and Ziliak 47 ). Evidence of the key negative dietary outcomes related to food insecurity by age group shown in the present review is critical to informing interventions; nutrition assistance and emergency food assistance programmes, including the Women, Infants, and Children (WIC) Program, the Supplemental Nutrition Assistance Program (SNAP), the School Breakfast and National School Lunch Program, and policies directed at food-insecure groups that can act to supplement dietary intake and mitigate food-security/food-insecurity disparity( Reference Kreider, Pepper and Roy 48 – Reference Ralston, Treen and Coleman-Jensen 51 ). Hill, in his original article, notes that the amount of evidence for causality should depend on the possible consequence of interventions derived( Reference Hill 14 ). Effective interventions that reduce food insecurity( Reference Kreider, Pepper and Roy 48 , Reference Kreider, Pepper and Gundersen 49 , Reference Ralston, Treen and Coleman-Jensen 51 ) have been shown to play an indirect role in improving health and diet, thus verifying the causal pathway and suggesting that the amount and strength of evidence needed to justify the relationship of food insecurity with diet may not be as stringent compared with other types of exposure–health outcome relationships.
Acknowledgements
The authors thank Dr Alisha Coleman-Jenson for reviewing an early draft of the paper.
The present review was supported by Elanco Animal Health, An Eli Lilly Company. Elanco had no role in the design, analysis or writing of this article.
H. A.-M. and Y. Z. planned the project; Y. Z. drafted an early version of the manuscript; H. A. E.-M. significantly revised the manuscript and led the project to completion. Both authors read and approved the final version.
There are no conflicts of interest.












