Background
Caregiving, and the stress that is often associated with it, appears to be a universal experience (Lambert et al., Reference Lambert, Bowe, Livingston, Heckel, Cook, Kowal and Orellana2017; World Health Organization [WHO], 1994). Although specific care tasks may differ across cultures, the stress experienced alongside caregiving can span borders, health care systems, and socioeconomic conditions, as has been evidenced in studies examining caregivers around the globe (Lambert et al., Reference Lambert, Bowe, Livingston, Heckel, Cook, Kowal and Orellana2017; Liu, Lu, & Lou, Reference Liu, Lu and Lou2017; Vaingankar et al., Reference Vaingankar, Chong, Abdin, Picco, Jeyagurunathan, Zhang and Subramaniam2016; Verbakel, Reference Verbakel2014; Wagner & Brandt, Reference Wagner, Brandt, Borsch-Supan, Kneip, Litwin, Myck and Weber2015; WHO, 1994). However, even within a country, differences in the experiences of caregivers may surface, driven in part by the types of support available along geographic lines (Lambert et al., Reference Lambert, Bowe, Livingston, Heckel, Cook, Kowal and Orellana2017). In this regard, caregivers living in rural settings may face additional challenges compared to their urban counterparts (Brazil, Kaasalainen, Williams, & Dumont, Reference Brazil, Kaasalainen, Williams and Dumont2014; Harbison, Coughlan, Karabanow, & VanderPlaat, Reference Harbison, Coughlan, Karabanow and VanderPlaat2005). A good example of this may be the experiences of rural informal caregivers in Canada, given the country’s vast and diverse landscape.
For several decades, as in many other nations, Canadian policy concerning aging in long-term care (LTC) has emphasized a de-institutionalization approach, whereby families and communities increasingly take on the responsibilities of caring for chronically ill and aging individuals (Campbell, Bruhm, & Lilley, Reference Campbell, Bruhm and Lilley1998; Lambert et al., Reference Lambert, Bowe, Livingston, Heckel, Cook, Kowal and Orellana2017; Rand & Malley, Reference Rand and Malley2014). Indeed, as government spending on formalized care for older adults decreases, an increased reliance on informal caregiving provision is expected (Proulx & Le Bourdais, Reference Proulx and Le Bourdais2014). Informal caregiving has been defined as the provision of unpaid assistance with tasks of daily life for individuals with physical, mental, or cognitive conditions (Ontario Caregiver Coalition, 2014). Informal caregivers (sometimes termed “care partners”; Copeland, Lieberman, Oravivattanakul, & Tröster, Reference Copeland, Lieberman, Oravivattanakul and Tröster2016) can represent a network composed of relatives and friends (Proulx & Le Bourdais, Reference Proulx and Le Bourdais2014), and caregiving provision depends upon a host of factors such as the number of children within a family, geographical proximity, gender, marital status, caring demands, and closeness or emotional ties (Rutherford & Bowes, Reference Rutherford and Bowes2014). Indeed, there is as much variation in the composition of the caregiver population as there is in care recipients (Chappell, Dujela, & Smith, Reference Chappell, Dujela and Smith2014). However, what is often common among informal caregivers are their experiences of “caregiver strain” (Duxbury, Higgins & Schroeder, Reference Duxbury, Higgins and Schroeder2009) – the stress-related health impacts of caring for another individual. It is this stress to which we must pay close attention in caring for the caregivers themselves (Alpert, Reference Alpert2014; Sklenarova et al., Reference Sklenarova, Krümpelmann, Haun, Friederich, Huber, Thomas and Hartmann2015).
The complexity of support demanded from informal caregivers’ social support networks often increases with age and with the unique challenges of caregiving (Rutherford & Bowes, Reference Rutherford and Bowes2014), especially as caregivers become both providers and recipients of that support (Chappell & Funk, Reference Chappell and Funk2011). In such circumstances, what may be needed is a support network of other informal caregivers who understand and identify with the daily trials and stressors associated with informal caregiving. However, given the high demands on caregivers’ time and energy, such networks are rare. The practical realities of rural caregiving, such as increased geographical distance between services and dwellings, extreme winter weather and road conditions, social and cultural norms and attitudes toward support services, and income insecurity or lower socioeconomic status – all common in the rural Canadian context – make accessing the needed support even more challenging (Harbison et al., Reference Harbison, Coughlan, Karabanow and VanderPlaat2005; Keating, Swindle, & Fletcher, Reference Keating, Swindle and Fletcher2011). Thus, because of the increasing prevalence of informal caregiving, and the potential challenges associated with the geographical remoteness of a rural setting, in this study we aimed to explore and understand the needs, challenges, and experiences – including the perceived stress associated with those challenges and experiences – of rural informal caregivers from their perspective. Moreover, we aimed to examine how social identification as a caregiver (i.e., self-identifying as a carer and/or close ties with other carers), social interactions, and both formal and informal coping support might be related to rural caregivers’ perceived stress.
Importance of Support for Informal Caregivers
In the Canadian context, approximately 13 million people over the age of 15 have served as a caregiver for a loved one (Sinha, Reference Sinha2013). Indeed, one fifth of Canadians aged 45 and older provide unpaid long-term care to the elderly, most often their own family and friends (Blomqvist, Busby, & Canadian Electronic Library, 2012). Although rates of informal caregiving vary by province, the national average is roughly 28 per cent (Sinha, Reference Sinha2013). Simultaneously, the demand for LTC has grown over the past 50 years, and continues to escalate; the long wait times for LTC facilities in Canada demonstrate that the formal support system is overwhelmed (Office of the Auditor General of Ontario, 2012) due to a combination of underfunding and an increasingly older population. Within the province of Ontario, a variety of support services exist to aid caregivers, including online resources (e.g., caregiverexchange.ca; ontariocaregivercoalition.ca) that link caregivers to information on physical supports such as applications for respite or home care services. Government-sponsored supports are also available via the federal family caregiver tax credit (Government of Canada, 2018) and family caregiver leave, which provides 8 weeks of unpaid leave with job protection annually (Ontario Ministry of Labour, 2018). However, although some specialized support is offered within some rural communities (e.g., gatewayruralhealth.ca), such resources are not widespread. Thus, increased development of informal services, networks, and volunteers within communities to support informal caregivers have been suggested as potential methods to enhance the care for older adults living with chronic conditions.
However, there also exist debates that question the sustainability of the increasing reliance on informal and voluntary care (Herron, Rosenburg, & Skinner, Reference Herron, Rosenberg and Skinner2016; Skinner, Reference Skinner2008). The need for informal caregivers is growing to respond to a lack of formal resources in rural (as well as urban) communities; nonetheless, with this growing reliance comes an increased (and rarely met) need for early stage support and standardization of available services (Herron et al., Reference Herron, Rosenberg and Skinner2016; Skinner, Reference Skinner2008). Without adequate support services, informal caregivers can experience increased vulnerability and burnout (Skinner, Reference Skinner2008). Indeed, the societal and financial costs related to aging will rise substantially if informal caregivers are not given adequate support to care for loved ones (Forbes et al., Reference Forbes, Markle-Reid, Hawranik, Peacock, Kingston, Morgan and Jansen2008; Zhu et al., Reference Zhu, Scarmeas, Ornstein, Albert, Brandt, Blacker and Stern2015). But more than this, the human cost to caregivers themselves – who provide this much-needed support – will be formidable without better ways to support them and reduce their stress.
High levels of stress and inadequate support for caregivers can combine to result in a broad array of chronic health conditions and the deterioration of personal relationships (Amaro, Reference Amaro2017; Vitaliano, Young, & Zhang, Reference Vitaliano, Young and Zhang2004). In addition to higher levels of perceived stress, negative health outcomes can include depressive symptoms (Pinquart & Sörensen, Reference Pinquart and Sörensen2003), decreased feelings of competence, and reduced quality of life, as well as increased physical complaints (Millenaar et al., Reference Millenaar, de Vugt, Bakker, van Vliet, Pijnenburg, Koopmans and Verhey2016) and inflammation (von Känel et al., Reference von Känel, Dimsdale, Mills, Ancoli-Israel, Patterson, Mausbach and Grant2006). Moreover, poor caregiver life satisfaction and depressive symptoms can negatively affect the health and well-being of the care recipient (Grant et al., Reference Grant, Clay, Keltner, Haley, Wadley, Perkins and Roth2013). In this regard, providers and receivers of care can stress each other throughout the caregiving process, compounding the detrimental effects.
Not all caregiving experiences are inherently negative, however. Several investigations reveal that caregivers have reported immense satisfaction, enjoyment, and empowerment, and that there may be simultaneous health benefits to performing informal caregiving duties (Brown & Brown, Reference Brown and Brown2014; Chappell & Dujela, Reference Chappell and Dujela2008; O’Connor, Reference O’Connor2007). Depending on the relationship to the care recipient, the stress experienced by the caregiver can differ. For example, a spouse who provides care often accepts this role more readily than a child would, and may view caregiving more positively (Chappell et al., Reference Chappell, Dujela and Smith2014; Chappell, Dujela, & Smith, Reference Chappell, Dujela and Smith2015). Indeed, although stress appears to be a shared experience among caregivers, not all would agree that caregiving entails a significant degree of “burden” as is commonly assumed (Bastawrous, Reference Bastawrous2013). What seems to be consistent, however, is that those with the highest levels of caregiver stress often experience feelings of loneliness, isolation, and lack of appreciation compounded by the inability to take reprieve from caregiving (Bevans & Sternberg, Reference Bevans and Sternberg2012). Support for caregivers – by way of formal support services as well as the informal coping support inherent in positive social interactions and valued social identities – may help to alleviate this stress (Bjerregaard, Haslam, Mewse, & Morton, Reference Bjerregaard, Haslam, Mewse and Morton2015; Cumming, Cadilhac, Rubin, Crafti, & Pearce, Reference Cumming, Cadilhac, Rubin, Crafti and Pearce2008; Donorfio, Vetter, & Vracevic, Reference Donorfio, Vetter and Vracevic2010; Haslam, O’Brien, Jetten, Vormedal, & Penna, Reference Haslam, O’Brien, Jetten, Vormedal and Penna2005).
Social Identity among Informal Caregivers
Taking on the responsibilities of an informal caregiver can be a significant transition in one’s life, as it demands the adoption of a new role and, subsequently, a new social identity (Barrett, Hale, & Butler, Reference Barrett, Hale and Butler2014; O’Connor, Reference O’Connor2007). Broadly defined, social identification refers to an individual’s “knowledge of his [or her] membership of a social group (or groups) together with the value and emotional significance attached to that membership” (Tajfel, Reference Tajfel1978, p. 63). Social identity differs from personal identity, which represents distinct characteristics that are unique to the individual (e.g., competence, talent, and sociability). Whereas personal identity refers to self-perceptions as an individual, social identity refers to self-perceptions in terms of the social groups to which one belongs (Deschamps & Devos, Reference Deschamps, Devos, Worchel, Morales, Páez and Deschamps1998; Luhtanen & Crocker, Reference Luhtanen and Crocker1992).
In this regard, social identity theory aims to delineate the implications of belonging to a specific group, including the cognitive (e.g., centrality of the identity to the self-concept), evaluative (e.g., being pleased to be a group member), and affective (e.g., feeling strong ties to others) dimensions of social identities (Cameron, Reference Cameron2004; Doosje, Ellemers, & Spears, Reference Doosje, Ellemers and Spears1995; Tajfel & Turner, Reference Tajfel, Turner, Austin and Worchel1979). Becoming an informal caregiver is an important social identity acquisition not only because more Canadians will be adopting this role in coming years, but because caregiving concerns and responsibilities can vary greatly in duration, experience, and impact on an individual’s life, health, and well-being (Bjerregaard et al., Reference Bjerregaard, Haslam, Mewse and Morton2015; Do, Norton, Stearns, & Van Houtven, Reference Do, Norton, Stearns and Van Houtven2015). Notably, even in the absence of regular contact with other group members (as is often the case with informal caregivers due to time demands), understanding oneself as a group member (“we”) has been observed to provide a sense of belonging and support and thereby to foster greater well-being, including lower levels of stress (Greenaway et al., Reference Greenaway, Haslam, Cruwys, Branscombe, Ysseldyk and Heldreth2015; Haslam et al., Reference Haslam, O’Brien, Jetten, Vormedal and Penna2005; Haslam, Jetten, O’Brien, & Jacobs, Reference Haslam, Jetten, O’Brien and Jacobs2004; Jetten, Haslam, & Haslam, Reference Jetten, Haslam and Haslam2012).
Informal caregivers, however, may not always feel that they identify with the term caregiver; instead, they often perceive their role of “carer” or “care partner” to be an expected or a natural responsibility of adult life and are faced with the challenge of “positioning” themselves within this new identity and their concurrent pre-existing familial relation (Barrett et al., Reference Barrett, Hale and Butler2014; Chappell et al., Reference Chappell, Dujela and Smith2015; Hughes, Locock, & Ziebland, Reference Hughes, Locock and Ziebland2013; O’Connor, Reference O’Connor2007). Unfortunately, those who typically assume caregiving tasks – adult children or spouses – often also report the greatest caregiver stress (Paulson & Lichtenberg, Reference Paulson and Lichtenberg2011). Incorporating the notion of caregiver into one’s personal identity, therefore, may not always protect informal caregivers against the poorer physical health, mental health, and caregiver strain that they are likely to incur in the midst of caregiving (Duxbury & Higgins, Reference Duxbury, Higgins and Schroeder2009; Rutherford & Bowes, Reference Rutherford and Bowes2014).
Caregivers who are especially vulnerable to this type of stress are those who simultaneously have children or dependents of their own, and are employed but required to reduce their work-related duties once they have taken on caregiving tasks; of this group, women tend to be most at risk of leaving employment to take on caregiving responsibilities and to experience caregiver strain compared to their male counterparts (Proulx & Le Bourdais, Reference Proulx and Le Bourdais2014). Caregivers themselves can also sometimes unintentionally undermine their caregiver identity by concealing the extent of informal care provision in an effort to “protect” their care recipient, thereby reducing the likelihood of receiving social recognition or the support resources they need (Moore & Gillespie, Reference Moore and Gillespie2014). This lack of support-seeking or -receiving may be further exacerbated by geographical location, with rural caregivers experiencing additional isolation, challenges, and stressors.
Challenges of Providing Informal Care in a Rural Setting
Many studies have sought to identify the needs of informal caregivers (Silva, Teixeira, Teixeira, & Freitas, Reference Silva, Teixeira, Teixeira and Freitas2013) and to assess their satisfaction with the current availability of home and community-based services (Canadian Home Care Association, 2007). It has been shown that availability of information, such as reliable information on diseases and conditions, and tangible support, such as respite care or assistance with home maintenance, is of great importance to caregivers (Brazil et al., Reference Brazil, Kaasalainen, Williams and Dumont2014). Other research has examined the extent to which home-care services are helpful for caregivers and their care recipients (Forbes et al., Reference Forbes, Markle-Reid, Hawranik, Peacock, Kingston, Morgan and Jansen2008; Hinojosa, Rittman, & Hinojosa, Reference Hinojosa, Rittman and Hinojosa2009; Sun, Roff, Klemmack, & Burgio, Reference Sun, Roff, Klemmack and Burgio2008). However, this work has demonstrated that having access to supportive services does not always lead to their use, as some caregivers are hesitant to reach out for help, or simply do not believe they need it (Forbes et al., Reference Forbes, Markle-Reid, Hawranik, Peacock, Kingston, Morgan and Jansen2008). Conversely, some caregivers may also be unaware of the formal services available to them in the first place – services that have the potential to prevent caregiver stress and “burnout” (Morgan et al., Reference Morgan, Semchuk, Stewart and D’Arcy2002). However, there is a relative lack of knowledge regarding the experiences of informal caregivers in rural areas given that a great number of these studies have focused on urban areas (Innes, Morgan, & Kostineuk, Reference Innes, Morgan and Kostineuk2011; Stewart et al., Reference Stewart, Morgan, Karunanayake, Wickenhauser, Cammer, Minish and Hayduk2014).
There is some evidence to suggest that rural inhabitants more commonly provide informal care compared to urbanites, in addition to spending more time and travelling farther distances to provide care (Sinha, Reference Sinha2013). These challenges are often further complicated by barriers to funding and timely service delivery in rural settings (Rural Ontario Institute, 2013) as well as social and cultural norms and attitudes – including those towards support services – in rural settings. For example, values such as independence and self-reliance, as well as social norms casting leisure activities as peripheral to hard work, are often particularly strong in rural communities (Harbison et al., Reference Harbison, Coughlan, Karabanow and VanderPlaat2005; Keating et al., Reference Keating, Swindle and Fletcher2011; Witcher, Holt, Spence, & Cousins, Reference Witcher, Holt, Spence and Cousins2007). Indeed, such values and norms can also be integral to rural identity formation over time (Keating et al., Reference Keating, Swindle and Fletcher2011) including how people come to self-identify as carers (Rutherford & Bowes, Reference Rutherford and Bowes2014).
Although research findings on the links between rural residency, stress, and health have been mixed, caregiving has been recognized as a chronic stressor for many Canadians, including those in rural areas (Brannen, Johnson Emberly, & McGrath, Reference Brannen, Johnson Emberly and McGrath2009). Indeed, stress was negatively related to perceived health among American rural caregivers, in part due to the distance required to travel for medical care (Sanford, Johnson, & Townsend-Rocchiccioli, Reference Sanford, Johnson and Townsend-Rocchiccioli2005). Moreover, health status among rural caregivers was also significantly poorer than that of the general population (Sanford & Townsend-Rocchiccioli, Reference Sanford and Townsend-Rocchiccioli2004). Similar findings have emerged among Canadian caregivers as well, with several facets of social location (e.g., gender, geography, social connectedness) suggested as crucial factors affecting caregivers’ health and well-being (Williams et al., Reference Williams, Sethi, Duggleby, Ploeg, Markle-Reid, Peacock and Ghosh2016). Thus, depending on the care recipient’s needs, location, and proximity to services, the type of assistance caregivers require may differ, and only in recent years has there been a concerted effort to better understand the support needs of rural caregivers (Innes et al., Reference Innes, Morgan and Kostineuk2011; Keating et al., Reference Keating, Swindle and Fletcher2011; Williams et al., Reference Williams, Sethi, Duggleby, Ploeg, Markle-Reid, Peacock and Ghosh2016) and how to mitigate stress in this often isolated population.
Present Research
Our research aimed to explore and understand the needs of rural informal caregivers, specifically those living in the rural community of Almonte in Ontario, Canada. Rural is defined as an area outside a census metropolitan area (total population of 100,000 or more with 50,000 living in the urban core) and census agglomerations (has an urban core of 10,000 or more; Statistics Canada, 2009). The community of Almonte has a total population of 5,039, with 1,310 people (26% of the population) aged 65 years and older (Statistics Canada, 2017). Almonte is in the “Ottawa Valley area”, a loosely defined region encompassing rural areas to the east and west of Ottawa, following the course of the Ottawa River. Almonte is a former mill town which now has many galleries, boutiques, and museums, and hosts various festivals throughout the year (Eades, Reference Eades2018).
In line with other research recommending a more holistic approach to examining caregivers’ experiences of stress (e.g., Bastawrous, Reference Bastawrous2013), we used a mixed-methods approach in conducting both a focus group and an online survey with rural informal caregivers in this community. Our goals were to explore caregivers’ greatest needs for support and assistance as well as various social factors that are potentially associated with caregiver stress (with the end goal to suggest ways through which that stress might be reduced). In this regard, we examined relationships among social identification as a caregiver; social interactions; and formal, informal, and coping support as well as perceived stress.
Methods
This research project used a mixed-methods approach in an effort to gather data from multiple perspectives, and to confirm themes emerging from both phases of the project. Qualitative data collection entailed a focus group with informal caregivers in the small town of Almonte, which is situated approximately 50km from Ottawa (the closest major urban centre) and has a population of approximately 5,000. Quantitative data collection followed by way of a survey – available both online and in paper format – to reach other informal caregivers in the community. Ethics approval from Carleton University’s Research Ethics Board was obtained before data collection commenced.
Focus Group
Participants and Procedure
Phase one of the present research involved a 90-minute focus group held with volunteers from the local hospital and LTC facility. Volunteer coordinators from the Almonte General Hospital and Fairview Manor LTC facility helped to identify and recruit participants through their networks. Eight individuals (7 women, 1 man) participated. The research team specifically aimed to recruit participants who were community and hospital volunteers, and included both previous and current informal caregivers in order to have participants who were knowledgeable about the Almonte community and services available in the town. The goal of this focus group session was to gather information in three domains: (a) resources and services available to informal caregivers in the community (e.g., “Do you know of any types of support for informal caregivers in Almonte?”), (b) resources and services used and desired by informal caregivers in the community (e.g., “In a perfect world, what are three services you think every caregiver should have access to?”), and (c) the most effective ways to distribute surveys to informal caregivers (e.g., “At which places will you often find informal caregivers in Almonte?”). Two members of the research team facilitated the discussion, while another two took detailed notes. The session was also recorded using two separate devices, and verbatim transcripts were later created for qualitative analysis. We obtained informed consent before beginning the session. Focus group participants were compensated for their time with the option of being entered into a draw to win a $50 gift certificate.
Analysis
Analysis of the focus group transcript was conducted in two ways. We first extracted main ideas from responses to each question in order to determine whether the resources and services that were available (i.e., known) to informal caregivers differed from those that were actually used (i.e., known but not used, perhaps due to cost, time, or transportation constraints, for example). Then, we conducted conventional content analysis on the transcript as a whole to search for overall themes that emerged during the focus group discussion (Hsieh & Shannon, Reference Hsieh and Shannon2005). Each member of the research team performed analysis of the transcript independently, and then reconvened as a group to discuss any discrepancies until consensus was reached.
Survey
Participants and Procedure
The second phase of this research project involved a survey, based on the results of our focus group data analyses, which explored the support needs and experiences of informal caregivers in a rural area. A total of 22 caregivers (14 women, 4 men, 4 unspecified) participated in the survey. The mean age of these caregivers was 69 years (SD = 8.0). The mean age of care recipients was 79 years (SD = 16.4), and included 8 women (50%) and 8 men (50%); 6 caregivers did not disclose the gender of their care recipient. Participants completed this survey either online or using a paper copy, and were recruited by posters displayed locally (e.g., in shops and community centres) and through social media on community websites. The only inclusion criterion was that participants were English-speaking, in order to be able to participate in the focus group or complete the survey. Based on themes generated from the focus group discussion, the survey included questionnaires that assessed informal caregivers’ experiences of coping, social interactions, formal and informal support, social identification as a caregiver, and perceived stress.
Measures
Social Identity
Informal caregivers’ social identity (i.e., feeling as though they are part of an informal caregiver community) was assessed using a 7-point scale (from 1 = “do not agree at all” to 7 = “agree completely”; Doosje et al., Reference Doosje, Ellemers and Spears1995). Three questions explored the cognitive (“I identify with other informal caregivers”), evaluative (“I am pleased to be an informal caregiver”), and affective (“I feel strong ties to other informal caregivers”) aspects of social identification (α = .65).
Social Interactions and Support
We posed 10 questions modified from Peeters, Van Beek, Meerveld, Spreeuwenberg, and Francke (Reference Peeters, Van Beek, Meerveld, Spreeuwenberg and Francke2010)Footnote 1 to explore informal caregivers’ experiences of social interactions and support. These assessed social interactions (3 items; e.g., “Do you have difficulty finding time to spend with friends because of your caregiving responsibilities?”; α = .87), formal support (2 items; r = .68), and informal support (2 items; i.e., “Do you feel you are offered enough [formal/informal] support to cope with the [physical/emotional] difficulties related to informal caregiving?”; r = .78, p < .001), as well as perceived coping support (3 items; e.g., “Is there someone you can turn to with your questions or problems?”; α = .52, p < .05). Responses were ranked on 5-point scales (from 1 = “strongly disagree” to 5 = “strongly agree”). We reverse-coded responses as needed such that higher scores indicated more positive responses.
Needs for More Support
Also, on the basis of research by Peeters et al. (Reference Peeters, Van Beek, Meerveld, Spreeuwenberg and Francke2010) and in keeping with one of the study’s goals to identify caregivers’ perceived needs for further support, we asked several questions relating to caregivers’ desires for general support (e.g., in setting up help for care recipient), daily assistance and support, physical care support, sharing caregiving responsibilities, communication with health care professionals, and other forms of support. For example, with regard to the “Sharing caregiver responsibilities” item in our survey, caregivers were asked to select whether they would benefit from “sharing the care with family and friends”, and/or “someone taking over, once in a while, in the support, help, and care of the person I am caring for”. A score of 1 was given if respondents indicated that they would like to receive that additional type of support, versus 0 if they did not.
Perceived Stress
A perceived stress scale, designed specifically to assess personal distress among family members of people with dementia (Greene, Smith, Gardiner, & Timbury, Reference Greene, Smith, Gardiner and Timbury1982), enabled us to measure stress experienced by informal caregivers (α = .94). This scale has 15 items comprising 3 subscales including personal distress (e.g., “Do you ever get depressed by the situation?”; α = .86), life upset (e.g., “How much has the household routine been upset?”; α = .83), and negative feelings (e.g., “Do you ever feel frustrated at times with the care recipient?”; α = .86). Each item was rated using a 5-point scale (from 0 = “not at all” to 4 = “to a high degree”).
Demographics
We also collected demographic information at the end of the survey about both the informal caregiver and the care recipient, including age, gender, education level, marital status, living arrangements, and current use of support services.
Analysis
We computed mean scores for all variables where appropriate, with reverse-coded variables as needed. We conducted correlational analyses to assess the relationships among caregiver social identity; social interactions; informal, formal, and coping support, as well as the three subscales of perceived stress. Frequency analyses were conducted to assess caregivers’ needs for additional support, and for an overview of caregiver and care recipients’ demographic characteristics and current use of support services.
Results
Focus Group
We extracted four themes from the focus group responses: (a) currently available services and lack of options, (b) challenges faced by informal caregivers, (c) needs of informal caregivers, and (d) sense of community.
Currently Available Services and Lack of Options
We asked focus group participants to describe resources and services that were currently available for informal caregivers in the area. Participants noted that there were very few support services available for caregivers, and some involved a cost, making them less accessible. It was also stated that caregivers were not aware of important questions they should be asking health care professionals when trying to support their care recipient. As one participant observed:
I don’t even know if the services are there or not. I don’t. I think everyone has such an individual case for needs that I don’t think there is just one unit that can help a caregiver.
Challenges Faced by Informal Caregivers
According to the focus group, the greatest challenge that informal caregivers faced was balancing multiple responsibilities, which results in a lack of time for informal caregivers to care for themselves. As exemplified by the quote below, many participants noted that even if more services were available to assist informal caregivers with coping, they would not have time to use the services:
Alzheimer’s Society does have a support group but you don’t have any time to use it. When I went, I was the only one there and I didn’t feel comfortable just sitting there.
In addition to a lack of time for addressing their own needs, it was noted that informal caregivers were often challenged by a sense of guilt, and in some cases would face the double responsibility of caring for their care recipient in addition to their own immediate families:
We are absorbing all of this, it is affecting us as well. Emotionally, etc. And if you stop then you feel guilty. There is nobody else to cover. You feel like you are caught in a snowball.
Needs of Informal Caregivers
When asked what types of resources or services should be made readily available to informal caregivers, the focus group participants emphasized the importance of transportation for care recipients, as this appeared to be an especially prevalent stressor among rural informal caregivers. As one participant put it:
Transportation in a rural area is a biggie. There are services available but the government doesn’t pay for it.
Increasing ease of access to support services for caregivers was also seen as important, as the discussion indicated that it is not often clear where to find information on support services within the community. The most common source of information used was general practitioners.
Sense of Community
Despite the emphasis of the focus group questions on the resources and services available or needed by caregivers, a final focus group theme emphasized a more positive aspect of the informal caregiving experience, namely the importance of volunteering and devoting time to one’s community. Indeed, it seemed that many participants equated informal caregiving with volunteering, and the discussion continually illustrated the great sense of community belonging these individuals felt. As one participant commented:
We are the ones who are helping out a friend of ours … We have to drive her long distances and out of our way. But you do that for neighbours.
Survey
Building on our focus group results, an online survey of rural informal caregivers also explored caregivers’ needs for support and assistance, and ways in which their caregiver stress might be alleviated by social interactions and support, and identifying with other caregivers.
Caregiver and Care Recipient Characteristics
Sample characteristics of both the caregivers who completed the survey and their care recipients are detailed in Tables 1 and 2. Consistent with previous research, most caregivers were women. Most caregivers were also married, were caring for either a parent or a partner, and had been caregiving for more than four years. Notably, as seen in Table 1, 75 per cent of survey respondents indicated that their frequency of caregiving was daily. Those daily activities ranged from washing and dressing the care recipient, administrative tasks, and coping with the fears, anger, or confusion of their loved one.
Table 1: Rural informal caregiver sample characteristics (n = 22)
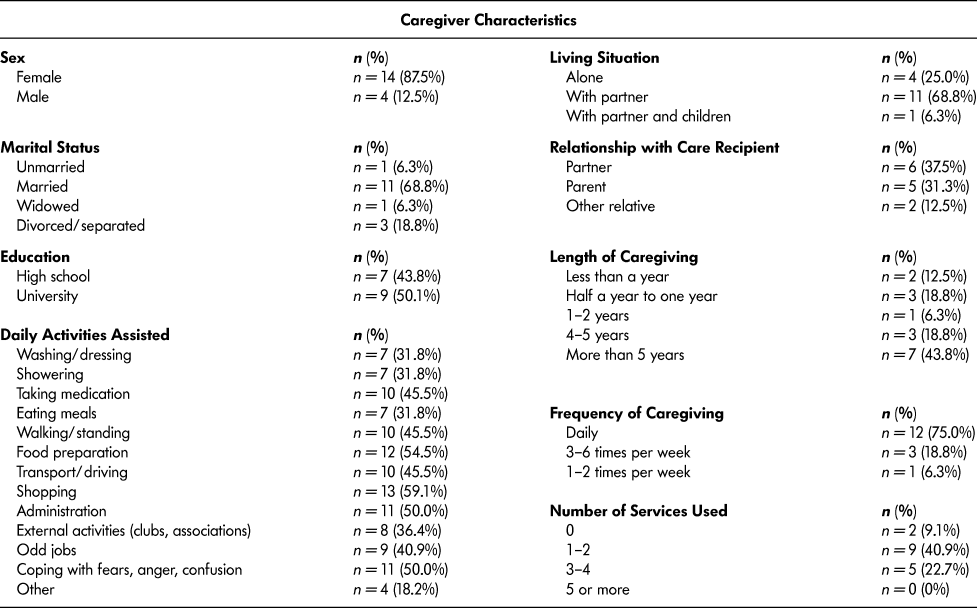
Table 2: Care recipient characteristics of rural informal caregivers (n = 22)
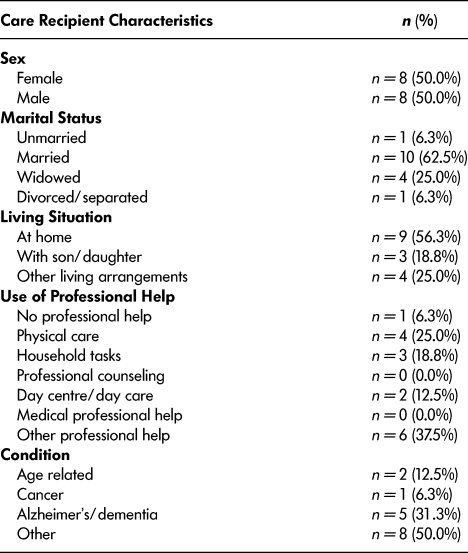
As seen in Table 2, when asked the reason for providing care, caregivers reported that 5 (31.3%) care recipients had Alzheimer’s disease or dementia, 2 (12.5%) had age-related ailments (arthritis, illness, etc.), 1 (6.3%) had cancer, and 8 (50%) care recipients suffered from other issues including stroke, cardiovascular diseases, macular degeneration, catheterization, and multiple sclerosis. Several of the care recipients also received some degree of professional help with physical care, household tasks, or other forms of help including physiotherapy, occupational therapy, respite care, personal grooming, and assistance from personal support workers.
Caregivers’ Needs for More Support
Table 3 summarizes caregivers’ desires for additional support. These were mixed, with no particular type of further support being singled out as most urgently needed. Whereas some caregivers reported the desire for more assistance with daily tasks (e.g., gardening, repairs) and struggles (e.g., dealing with feelings of isolation), others noted their need for more support with physical care (e.g., fall prevention, incontinence). When assessing the role of health care providers, however, some caregivers wanted both better coordination of care with other health care providers and better communication between themselves, their care recipients, and health care professionals.
Table 3: Rural informal caregivers’ needs for more support
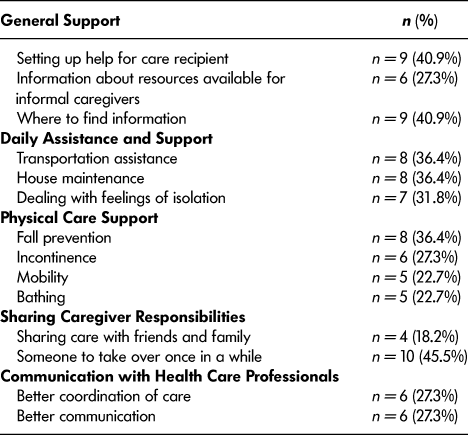
If caregivers were able to share their responsibilities, many (45.5%) respondents expressed the desire for someone to take over their caregiving responsibilities occasionally. Indeed, the open-ended responses from the survey also indicated that caregivers would benefit from occasional overnight support so they could visit relatives that live out of town, a formal support group with whom to share experiences, receiving further guidance from a health care professional (such as nurse or support worker), utilizing video chat services as support networks, and increased networking opportunities with other informal caregivers. However, the difficulties of balancing full-time employment and providing caregiving assistance were described as barriers to accessing such support. Caregivers also expressed the need for more preventive services that would address their needs for early stage support, rather than those that could only be used once a crisis has already occurred.
Correlations among Variables of Interest
In addition to an overview of informal caregivers’ needs for additional support, given the many challenges associated with caregiving and particularly in a rural setting, of primary interest in the current research were the types of support and social interactions that might buffer the stress that caregivers often experience on a daily basis. We thus assessed relationships among caregivers’ social identification, social interactions, informal support (i.e., from family or friends), formal support (i.e., from health care providers, community programs), perceived coping support, and perceived stress (including personal distress, life upset, and negative feelings). As Table 4 shows, levels of caregiver social identification were quite high across the sample, and this was significantly and positively associated with social interactions, both formal and informal support, and perceived coping support. As expected, having a strong sense of caregiver social identity was also negatively associated with each index of stress, including personal distress, life upset, and experiencing negative feelings.
Table 4: Means, standard deviations, and inter-correlations among survey variables
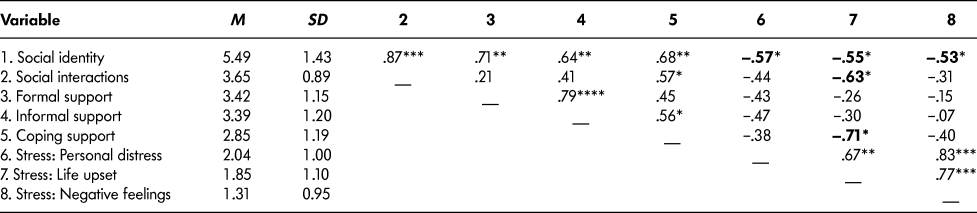
Note. Significant correlations between each of the social/support and stress variables have been bolded for ease of interpretation. M = mean; SD = standard deviation.
*p < .05. **p < .01. ***p < .001.
Correlations among the remaining variables were inconsistent; not surprisingly, perceived coping support was positively associated with both social interactions and informal support, and the strongest relationship was found between formal and informal support. Of particular interest, however, were the relationships between these variables and perceived stress. Whereas social identification was negatively related to each type of stress (as mentioned above), only social interactions and perceived coping support were associated with reduced stress – and only with regard to stressors causing life upset (e.g., disruptions of household routine). In effect, social identification may have buffered caregivers’ stress on many levels.
Discussion
Taken together, our mixed-methods research findings provide some preliminary insight into the experiences of informal caregivers living in rural areas. The results of both the focus group and survey suggest that, although they face many challenges, the rural informal caregivers of the small Ontario town of Almonte value their caregiving identity and feel a strong sense of community. Although it appears that the available formal services (e.g., emotional and practical) in this rural setting may often fall short of meeting informal caregivers’ needs – or that informal caregivers simply do not have the time to use them – other options might be available for reducing the stress associated with their caregiving responsibilities, such as facilitating access to coping support, increasing social interactions, and especially enhancing caregiver social identity. In the midst of a system where formalized services are often not available or accessible, such efforts are needed in order to determine how best to promote social support alternatives that might help caregivers cope with their ongoing stress in the absence of social change.
Informal Caregivers’ Challenges and the Experience of Stress
The four major themes arising from the focus group – lack of options for support services, challenges faced by informal caregivers, needs of informal caregivers, and the importance of a sense of community – reflect those often found in previous research (Blair, Volpe, & Aggarwal, Reference Blair, Volpe and Aggarwal2014), especially among rural caregivers (Brazil et al., Reference Brazil, Kaasalainen, Williams and Dumont2014; Sanford et al., Reference Sanford, Johnson and Townsend-Rocchiccioli2005). Together, they paint a picture of the challenges and experiences of informal caregivers in a rural community. Importantly, the first three themes reflected challenges or unmet needs that informal caregivers frequently experienced, which undoubtedly contributed to higher levels of caregiver stress.
Formal Support Services in a Rural Community
Having few formal support services available appears to be an experience common to rural informal caregivers (Crosato & Leipert, Reference Crosato and Leipert2006; Forbes et al., Reference Forbes, Morgan and Janzen2006, Reference Forbes, Markle-Reid, Hawranik, Peacock, Kingston, Morgan and Jansen2008; Keating et al., Reference Keating, Swindle and Fletcher2011; Kuluski, Williams, Berta, & Laporte, Reference Kuluski, Williams, Berta and Laporte2012; Peeters et al., Reference Peeters, Van Beek, Meerveld, Spreeuwenberg and Francke2010; Tryssenaar & Tremblay, Reference Tryssenaar and Tremblay1999). Barriers to formal support use in a rural area often include a lack of available services, and high costs of services that are available. Indeed, a recurring theme was limited access to costly services and transportation within the rural setting by caregivers and care recipients while on a pension (Forbes et al., Reference Forbes, Markle-Reid, Hawranik, Peacock, Kingston, Morgan and Jansen2008; Morgan et al., Reference Morgan, Semchuk, Stewart and D’Arcy2002; Sanford et al., Reference Sanford, Johnson and Townsend-Rocchiccioli2005). Since services are often spread out geographically in rural areas, taxi fares become much more expensive than in urban areas. In order to mitigate some of these barriers, our focus group participants suggested having volunteer drivers, while recognizing that volunteering itself is a large commitment and is perhaps not sustainable as a long-term solution.
The limited availability of services that meet the specific needs of rural informal caregivers might explain why our survey results suggested no association between formal support service use and levels of caregiver stress. This lack of appropriate or accessible services is in alignment with previous studies exploring the needs of rural informal caregivers, demonstrating this to be a common challenge and not unique to our study population (Crosato & Leipert, Reference Crosato and Leipert2006; Forbes et al., Reference Forbes, Markle-Reid, Hawranik, Peacock, Kingston, Morgan and Jansen2008; Innes et al., Reference Innes, Morgan and Kostineuk2011). Similarly, even when services are available, informal caregiving is often described as being “24/7”, with no spare time to even access a support group (Brazil et al., Reference Brazil, Kaasalainen, Williams and Dumont2014), thereby potentially exacerbating the stress and social isolation often associated with caregiving.
Challenge of a Balancing Act
In line with the notion of caregivers’ time being too limited to access formal support services, both our focus group and survey participants noted that a common challenge faced by informal caregivers is in performing a balancing act of multiple responsibilities. Moreover, the strain often caused by balancing caregivers’ demands on time (Khan, Pallant, & Brand, Reference Khan, Pallant and Brand2007) is often exacerbated by guilt, including caregivers feeling unable to decline taking on additional tasks even when they already feel overwhelmed. We suggest that a contributing factor to this finding in the present research is the often close-knit nature of rural communities (Brannen et al., Reference Brannen, Johnson Emberly and McGrath2009). Caregivers may feel like they have failed their care recipient if others in the community know that they have approached formal services for help, or are unable to take on additional caring tasks (Crosato & Leipert, Reference Crosato and Leipert2006).
Previous research suggests that this feeling of failure is especially prevalent among female caregivers in rural areas (like our own sample), who often feel additional pressure because of the double responsibility of caring for their families and their care recipient (Crosato & Leipert, Reference Crosato and Leipert2006). Indeed, there are many barriers to the use of formal services, such as stigma, social, and cultural norms, lack of awareness of service availability, and low accessibility of services (Harbison et al., Reference Harbison, Coughlan, Karabanow and VanderPlaat2005; Keating et al., Reference Keating, Swindle and Fletcher2011; Morgan, Semchuk, Stewart, & D’Arcy, Reference Morgan, Semchuk, Stewart and D’Arcy2002; Rand & Malley, Reference Rand and Malley2014; Stewart et al., Reference Stewart, Barnfather, Neufeld, Warren, Letourneau and Liu2006). This information becomes especially important with the knowledge that low service use can result in adverse caregiver health effects as their needs go unmet (Morgan et al., Reference Morgan, Semchuk, Stewart and D’Arcy2002). Unfortunately, this can also negatively affect the care recipients’ physical and mental well-being – such as adding to levels of chronic stress (Blair et al., Reference Blair, Volpe and Aggarwal2014; Grant et al., Reference Grant, Clay, Keltner, Haley, Wadley, Perkins and Roth2013) – which underscores the importance of adequate support for rural informal caregivers.
Analysis of our survey results also reflected the balancing act of caregiving reported by focus group participants as well as possible solutions to help alleviate caregiver stress. Our findings indicate that a lack of effective coping support and social interactions, including having no one to turn to when faced with problems and feeling isolated, are associated with increased stress, especially with regard to stressors involving life upset, such as sleep interruptions and disturbances to the household routine. Coping support often plays a central role in managing the stress associated with providing care on an ongoing basis. Similar to findings in previous research (Blair et al., Reference Blair, Volpe and Aggarwal2014), we found caregivers in our study reported that friends, family, and colleagues help them cope with stressful situations and periods of particularly heavy caregiver strain. These results therefore point to the need for the promotion of increased coping resources and social interactions to help alleviate caregiver stress, especially as it relates to balancing the daily needs of life as an informal caregiver in a rural setting (Sanford et al., Reference Sanford, Johnson and Townsend-Rocchiccioli2005).
Meeting the Needs of Informal Caregivers
Studies that have focused on rural informal caregivers have generally found that their primary needs include information, emotional support, financial assistance, respite care, homemaker services, and case management support (Bee, Barnes, & Luker, Reference Bee, Barnes and Luker2009; Edelman, Kuhn, Fulton, & Kyrouac, Reference Edelman, Kuhn, Fulton and Kyrouac2006; Forbes, Morgan, & Janzen, Reference Forbes, Morgan and Janzen2006; Hystad & Carpiano, Reference Hystad and Carpiano2012). Although rural informal caregivers tend to prioritize having information and emotional support over physical support and practical assistance (Bee et al., Reference Bee, Barnes and Luker2009; Diehl-Schmid et al., Reference Diehl-Schmid, Schmidt, Nunnemann, Riedl, Kurz, Förstl and Cramer2013; Edelman et al., Reference Edelman, Kuhn, Fulton and Kyrouac2006; Peeters et al., Reference Peeters, Van Beek, Meerveld, Spreeuwenberg and Francke2010), it is interesting to note that our focus group participants did not prioritize emotional support needs and indicated that even if formal emotional support groups were available, they likely would not have the time to use them. Likewise, very few of the rural informal caregivers who completed our survey reported wanting assistance in managing the emotional challenges associated with caregiving (e.g., dealing with feelings of social isolation). Although this result contrasts with some earlier research (cf. Abu Bakar, Weatherley, Omar, Abdullah, & Aun, Reference Abu Bakar, Weatherley, Omar, Abdullah and Aun2014), it simultaneously highlights the uniqueness of each individual caregiver’s situation. In place of emotional support, focus group participants emphasized that they lacked more tangible forms of support, and especially the sharing of caregiver responsibilities to help alleviate some of the stress associated with balancing their caregiving and other responsibilities.
Finally, focus group participants expressed their desire for a single resource they could use to increase knowledge and accessibility of support services, in large print and in accessible language. This suggestion for a “one-stop” for information appears to be common, as participants in studies by both Forbes et al. (Reference Forbes, Markle-Reid, Hawranik, Peacock, Kingston, Morgan and Jansen2008) and Blair et al. (Reference Blair, Volpe and Aggarwal2014) suggested that a comprehensive resource guide be created for caregivers. In response, we created such a resource for the community in which our research was conducted, with the goal of making a more immediate and tangible contribution to reducing caregiver stress within this communityFootnote 2.
Caregiver Social Identity as a Potential Stress Buffer
In contrast to the challenges reported by informal caregivers in our research that may have contributed to their (in)ability to cope with stress, an important theme that was captured by focus group participants was a “sense of community”, or the degree to which the informal caregivers in our study felt connected to others within their small, rural community – a finding that corroborates other research involving Canadian caregivers and that reveals the importance of social connectedness and location (Williams et al., Reference Williams, Sethi, Duggleby, Ploeg, Markle-Reid, Peacock and Ghosh2016) as well as stress among rural Canadians (Brannen et al., Reference Brannen, Johnson Emberly and McGrath2009). Indeed, focus group participants reported having a strong sense of community, saying that when it comes to assisting others, there is no question: “you just do it”. This contrasts with previous research that has explored the personal identity of informal caregivers, who felt that they did not identify with the term “informal caregiver” because they perceived this role to be simply another part of their relationship with the care recipient (Hughes, Locock, & Ziebland, Reference Hughes, Locock and Ziebland2013).
A few explanations can be offered for this discrepancy. For instance, these results may point to differences between personal identity (which Hughes et al., Reference Hughes, Locock and Ziebland2013, looked at exclusively) and social identity (Tajfel & Turner, Reference Tajfel, Turner, Austin and Worchel1979) – our participants were not only asked about their personal feelings about being a caregiver, but also whether they felt connected to other informal caregivers. Another explanation could be the geographical setting of the study. Community ties vary considerably across settings (Brannen et al., Reference Brannen, Johnson Emberly and McGrath2009; Ferrari, Kapoor, Bristow, & Bowman, Reference Ferrari, Kapoor, Bristow and Bowman2006); our findings may reflect the intimate nature of the small community where our study took place. Nonetheless, there is reason to believe that it may be indicative of other rural communities in Canada as well (DesMeules et al., Reference DesMeules, Pong, Read Guernsey, Wang, Luo, Dressler, Kulig and Williams2012).
Analysis of data from the 2000–2001 Canadian Community Health Survey demonstrated that an increased level of community belonging may be associated with a higher self-rating of general and mental health (Ross, Reference Ross2002). Indeed, both social identity and sense of community share their emphasis on a valued group membership and shared emotional connections or experiences (Bjerregaard et al., Reference Bjerregaard, Haslam, Mewse and Morton2015; Omoto, Reference Omoto2014). To provide a quantitative measure of a “sense of community” with other caregivers specifically, survey respondents were asked how closely they identified as an informal caregiver, whether they were pleased to be an informal caregiver, and whether they felt “strong ties” with other informal caregivers, reflecting the cognitive, evaluative, and affective dimensions of social identification respectively (Cameron, Reference Cameron2004; Doosje et al., Reference Doosje, Ellemers and Spears1995).
The results of our survey reflect findings similar to that of previous research regarding the potential benefits to mental and physical health associated with a sense of community belonging more generally (see Jetten et al., Reference Jetten, Haslam and Haslam2012, for a review), and among older adults in particular (Haslam et al., Reference Haslam, Haslam, Ysseldyk, McCloskey, Pfisterer and Brown2014; Steffens, Cruwys, Haslam, Jetten, & Haslam, Reference Steffens, Cruwys, Haslam, Jetten and Haslam2016; Ysseldyk, Haslam, & Haslam, Reference Ysseldyk, Haslam and Haslam2013), in that perceived stress and social identity were negatively related. The more one identified as a caregiver, the less stress reported, and this was true across all three dimensions of perceived stress. Indeed, although the associations between both social interactions and coping support were limited to lower “life upset” stress (as mentioned earlier), a stronger caregiver social identity was not only associated with reduced stress of this nature but also with reduced personal distress and negative feelings about caregiving. Thus, social identification appeared to buffer caregivers’ stress on many levels, whereas the benefits of social interactions and coping support seemed to be more limited.
Along with our findings that neither formal nor informal support was related to perceived stress at all, these results also corroborate earlier research (Majerovitz, Reference Majerovitz2001) on the buffering effects of social support on caregiver stress – in this case, through caregivers’ social identity. We suggest that by identifying as a caregiver, one becomes part of a wider group of caregivers in their community, and a sense of comfort is gained in simply knowing that they are not alone in the challenges and experiences that they face. Given the socially isolated locations in which many Canadian caregivers often find themselves, this may be especially valuable for informal caregivers in a rural setting.
Strengths and Limitations
A strength of our research was the use of a mixed-methods approach by way of collecting both qualitative and quantitative data. As a result, we were able to identify, with greater confidence, important patterns and associations among the variables of interest. Importantly, the results of phase one of our study (i.e., the focus group, which was aimed at collecting caregivers’ experiences of the availability and use of support services, and through which themes such as a sense of community identity emerged) informed our choice of measures for phase two (i.e., the survey, which included measures directed at capturing caregiver social identity specifically, as well as further exploration of the needs, challenges, and stressors of caregivers’ daily lives). Indeed, by using both focus group and survey data, we were able to provide a more comprehensive picture of caregivers’ needs and experiences, as well as the importance of social identity – both with a community of caregivers and the larger community – in managing caregiver stress. Moreover, given the rural origin of our samples, this study also adds valuable information to the scarce amount of existing literature focusing on rural informal caregivers.
Of course, these strengths are also balanced by some limitations. The sample sizes comprising our focus group and survey respondents were small, and some surveys were incomplete; thus, our findings may not be representative of all informal caregivers in this or other rural areas, and the findings of the present research should therefore be considered as preliminary. However, our sample size may also reflect the smaller population size of rural areas, which would in turn contribute to lower numbers of specific subpopulations, such as informal caregivers. This concurs with findings noted by other researchers, who found that informal caregivers were so busy caring for their recipients that filling out the survey associated with their research was regarded as too time-consuming (Brazil et al., Reference Brazil, Kaasalainen, Williams and Dumont2014). A similar situation may have occurred in our study as well. Moreover, our experience of obtaining relatively small sample sizes may have also reflected the challenges inherent to community-based research, especially with older adults (see Ysseldyk, Paric, & Luciani, Reference Ysseldyk, Paric and Luciani2016). Thus, rather than negating the value of the research, this provides yet another example of the importance of reaching this socially isolated population.
Nonetheless, although correlations were deemed to be most appropriate for examining relations among the variables of interest (Bland & Altman, Reference Bland and Altman2009) given the small sample size and our cross-sectional survey methodology, we must be cautious about making any definitive or causal conclusions about the nature of the relationships between variables. For example, although we can suggest that higher levels of social identification potentially buffer against caregiver stress, it may also be that the informal caregivers in our sample who reported lower levels of perceived stress were subsequently more inclined to reach out to, or identify with, other informal caregivers. Likewise, variations on these relations might be evident if data from a larger sample of rural caregivers could have been achieved, or if additional focus groups within this or other rural settings were conducted. And of course, within any population, there are those caregivers who do not wish to be caregivers at all, and for whom the stress-related implications of identifying as such may not be as beneficial as for others.
Relatedly, Brannen et al., Reference Brannen, Johnson Emberly and McGrath2009, have suggested that measuring stress may be problematic in rural settings because rural people may not identify or associate their lifestyle as one that is stressful in the same way their urban counterparts would describe. Thus, further research is warranted in order to better understand perceptions of stress in rural communities alongside self-identity. Finally, the limitations of using an online survey with this population should also be acknowledged. A systematic review by Remillard, Mazor, Cutrona, Gurwitz, and Tjia (Reference Remillard, Mazor, Cutrona, Gurwitz and Tjia2014) suggested that the use of internet-based questionnaires in research related to aging may lead to issues with recruitment and generalizability. Older adults, especially those in rural areas, may not feel comfortable using computers to access or complete online surveys due to a variety of limitations, including not having access to up-to-date technology or high-speed internet, or physical limitations such as visual impairment (Herron et al., Reference Herron, Rosenberg and Skinner2016; Remillard et al., Reference Remillard, Mazor, Cutrona, Gurwitz and Tjia2014). Although our study recruitment also included paper-based posters in local community centres and shops, as well as the option to complete a paper-based questionnaire, future research should continue to explore additional ways to reach informal caregivers in rural areas (outside of posters and electronic links), who may be too busy to participate in a focus group or to start or complete a survey.
Conclusion
Much previous literature has noted that rural caregivers are often more overwhelmed or stressed and have more limited access to formal support services than their urban counterparts (see Keating et al., Reference Keating, Swindle and Fletcher2011). Although informal caregivers residing in rural areas face unique challenges, a minimal amount of research has been conducted on their experiences (Stewart et al., Reference Stewart, Morgan, Karunanayake, Wickenhauser, Cammer, Minish and Hayduk2014). Our findings add to the small, yet growing, body of research regarding this population. Informal caregivers living in rural areas face a host of challenges – a lack of formal services, the necessity for balancing responsibilities, and a continuous need for further support – not only as a result of their caregiver tasks but from their geographic isolation as well.
In the Canadian context, where geographic and social isolation is a common reality, it is crucial that the needs of rural informal caregivers are attended to, especially as they currently represent an integral component of our health care system. Indeed, as a large subset of the Canadian population ages and support for institutionalized care wanes, the demand for informal caregiving grows. And yet, despite the many challenges they face, our research suggests that informal caregivers living in rural areas may consider caregiving to be an important part of their self-concept – their social identity – and that this is associated with lower perceived stress overall. This research thus represents a promising avenue for further investigation to help alleviate the stress experienced by so many informal caregivers. As one of our focus group participants said best, when it comes to informal caregiving, “it takes a village, so it’s time we start working together”.








