Cervical artery dissection (CAD) is a rare but important cause of stroke, especially in young and middle-aged adults.Reference Debette and Leys 1 Imaging is essential for the early recognition, differential diagnosis and appropriate management of CAD. Trans-femoral cerebral angiography (TFCA), CT angiography (CTA) and magnetic resonance angiography (MRA) are widely used to assess the vascular luminal status of CAD, such as long tapered stenosis and aneurysmal dissection. However, these methods do not provide information about the carotid wall adjacent to the lumen where the pathology exists. Therefore, vascular wall MRI is becoming increasingly popular.Reference Rastogi, Xia and Wang 2 Here we present short-term changes of MRI in a patient with CAD and discuss the technical aspects of the fat-saturated T1-weighted DANTE-SPACE sequence. DANTE (Delay Alternating with Nutation for Tailored Excitation) is a blood-flow suppression method, whereas SPACE (Sampling Perfection with Application optimized Contrasts using different flip angle Evolution) is a three-dimensional turbo-spin echo MRI sequence.
A 34-year-old healthy woman with transient left-side weakness and right-side blurred vision underwent radiologic evaluation. She had a history of minor head trauma during swimming 2 weeks before symptom onset. Initial fat-saturated T1-weighted DANTE-SPACE revealed bright mural hematoma signal (arrow) in the right internal carotid artery, suggestive of artery dissection. The excellent cancellation of blood-flow signal in the carotid lumen concomitant with consistent fat suppression (arrow heads) in the cervical region enabled clear depiction of CAD (Figure 1A). TFCA showed a tapered long segmental stenosis (arrows), which is a typical appearance of proximal carotid artery dissection (Figure 1B). The patient showed good clinical recovery and was subsequently discharged after 7 days. Follow-up MRI taken at 10 weeks after onset depicted resolution of the CAD (arrow) (Figure 2). In this case, non-invasive visualization of a dynamic change of CAD using DANTE-SPACE obviated the need for follow-up TFCA.
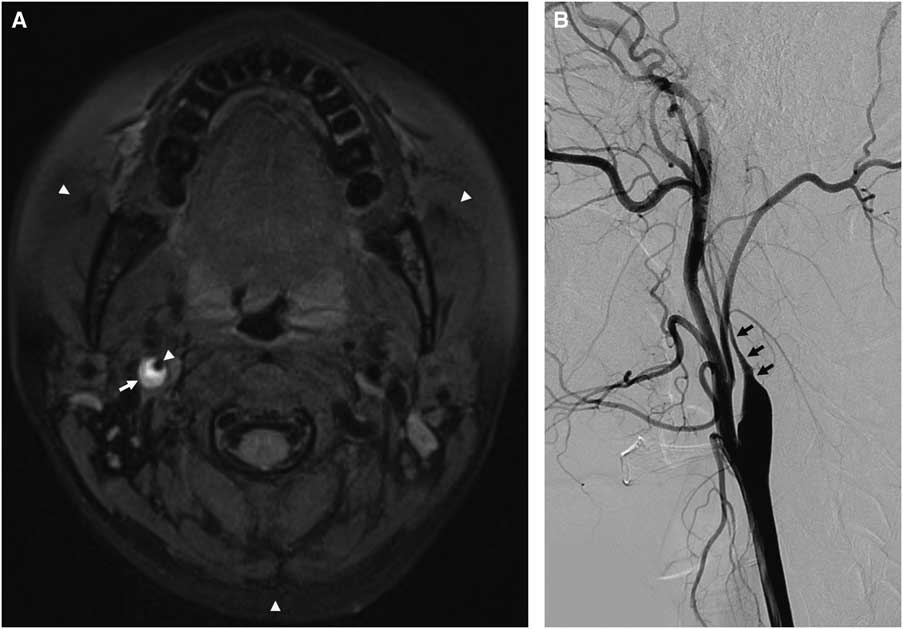
Figure 1 Precontrast T1-weighted DANTE-SPACE MRI revealed eccentric bright signal in right proximal carotid artery, suggestive of carotid dissection (A). Catheter angiography showed typical tapering appearance of proximal ICA, suggestive of carotid dissection (B).
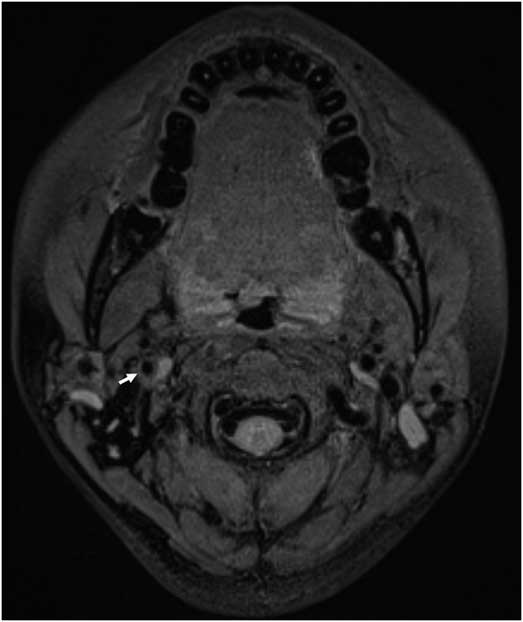
Figure 2 Follow-up T1-weighted DANTE-SPACE showed resolution of eccentric bright signal after 10 weeks.
MRI provides excellent soft tissue contrast of the carotid wall and exhibits no post-calcific shadowing. These two characteristics make MRI superior to CT and ultrasound with respect to carotid plaque characterization. Previous multi-contrast MRI with blood-flow suppression techniques have been used to determine carotid wall pathology using a combination of T2-weighted, T1-weighted, contrast-enhanced T1-weighted and proton-density-weighted MRI. Among these, fat-saturated T1-weighted MPRAGE (Magnetization-Prepared Rapid Acquisition Gradient Echo) shows a high detection rate of intraplaque hemorrhage, showing a high agreement rate with surgical specimens.Reference Takaya, Yuan and Chu 3
DANTE-SPACE, in and of itself, shows great promise for carotid wall imagingReference Xie, Yang, Xie, Pang, Fan and Li 4 compared with the previous MRI sequences. First, it is a three-dimensional imaging technique that enables (a) high resolution to detect small structures, (b) multi-planar reconstruction and (c) extended anatomical coverage. Sub-millimeter high-resolution images with tailored reconstruction are beneficial in evaluating the intimal flap of dissection or fibrous cap of atheroma. Multi-planar images and large anatomic coverage enable simultaneous cervical and intracranial vessel wall imaging. Second, DANTE-SPACE yields consistent suppression of blood flow irrespective of blood velocity. Slow and turbulent flow can often degrade the quality of blood-flow suppression around the stenotic carotid lumen. Previous MPRAGE sequences using various methods of blood-flow suppression such as double inversion recovery or motion-sensitized-driven equilibrium were affected by slow-flow signal, whereas DANTE-SPACE is immune to this shortcoming. Third, DANTE-SPACE has consistent fat suppression, higher signal-to-noise ratio and is less sensitive to motion and/or susceptibility artifacts, because it is a spin echo (as opposed to a gradient-recalled echo) sequence. Although DANTE-SPACE has a higher specific absorption rate (i.e., power deposition) and longer acquisition time compared with MPRAGE, it may play a key role in clinically diagnosing CAD and characterizing vessel wall in general.
Acknowledgment
The authors thank ML Lauzon, PhD, for helpful discussions.
Statement of Authorship
KL prepared the manuscript; HSC contributed to concept and design; JK revised the manuscript; BSK was involved in image acquisition; and YSS supervised the study.
Disclosure Information
All authors report no disclosures.






