Background
Dementia is a broad category of neurological disease that leads to loss of independence, decreased quality of life, significant caregiver burden, and elevated healthcare costs.Reference Fiest, Jetté and Roberts1 As Canada’s population ages, the number of people living with dementia continues to increase.Reference Charles, Parmar, Bremault-Phillips, Dobbs, Sacrey and Sluggett2 The Alzheimer Society of Canada estimated that in 2016, there were 564,000 persons in Canada living with dementia. It is predicted that this number will increase to 937,000 by 2031.3 A number of cognitive functions are impaired in dementia including memory, orientation, language, and executive function.4, Reference Voskou, Douzenis, Exonomou and Papageorgiou5 A matter of concern is the limited capacity of these individuals to take part in complex decisions regarding their financial and personal affairs.Reference Burla, Rego and Nunes6 Questions regarding personal belongings and property, management of finances, and medical treatment may all arise when an individual is diagnosed with dementia. Legal documents such as a Will, Power of Attorney, and Advanced Healthcare Directive thus become critical to guide decision-making in these patients.
A Will is a legal document that provides instructions regarding the disposition of a person’s estate. Making this document allows a person to devise, bequeath, or dispose of all real or personal property in which he or she has an interest at the time of his or her death.7 The document also allows one to appoint an executor to administer one’s estate. Provincial legislation in each province governs the formation and validity of a Will.
The requirements for a valid Will are similar across most Canadian provinces. One necessary requirement for a Will is not found in legislation but is governed by common law: testamentary capacity. The four requirements for testamentary capacity are set out in the 1870 case of Banks v Goodfellow.8 According to this case, the person creating a Will must understand the nature and effects of the act of making a Will, understand the extent of the property they are disposing of, comprehend and appreciate who will benefit from the estate, and be free from any delusions that may influence the making of the Will.8 Testamentary capacity can be challenged for legally defined reasons such as senility, insanity, delusions, and drugs or alcohol. It is important to note that although senility is still included in the legal literature, it is no longer a medical diagnosis and is not used in dementia literature.
“Senility” cases touch on issues that can arise for individuals with dementia. The Supreme Court of Canada recognizes that dementia patients can have a sliding scale of memory loss, and when a Will is made during one’s illness, it is possible to have times of lucidity that do not necessarily invalidate the document. Testamentary capacity is important for the moment when instructions are given, and less so for the moment when the document is signed, as long as the person making the Will recalls having provided the instructions.9 Meanwhile, when someone with dementia becomes unable to meet the necessary elements of testamentary capacity, he or she is no longer able to create a valid Will.
It is important to create a Will in a timely manner, especially when an individual exhibits early signs of cognitive decline. If someone is unable to make a Will, their estate will, upon their death, be subject to the rules of intestacy. In this case, provincial estate administration legislation governs the way estates are dealt with.10 This legislation provides for a variety of familial situations and directs how the estate is to be divided.
A Power of Attorney is a document that allows a person to appoint another person to act on their behalf according to the terms of the document. As with the creation of a Will, provincial legislation in each province governs the creation of a Power of Attorney. The person creating the document, called the grantor, can appoint an attorney for property, for personal care, or for both. An attorney for property acts for the grantor in matters of property and financial affairs, whereas an attorney for personal care deals with the personal affairs of the grantor.11 A grantor must have capacity at the time of creating the document. A Power of Attorney can be contingent or enduring. If an enduring Power of Attorney is created, the power granted to the attorney is given to them at the time of the execution of the document. This authority will remain in place after the grantor loses capacity.11 If the Power of Attorney is contingent, it can be executed by the grantor while they have capacity, and the authority to act on their behalf will not vest in the attorney until the grantor loses capacity.11
An Advanced Healthcare Directive is a document that gives instructions for healthcare decisions and/or the appointment of a substitute healthcare decision maker. In general, provincial legislation requires that the maker of the Advanced Healthcare Directive have capacity at the time of creating the directive.12 For instance, the person must have the ability to understand information relevant to a healthcare decision about a proposed treatment, appreciate the reasonably foreseeable consequences of making or not making a healthcare decision about a proposed treatment, and communicate a healthcare decision about a proposed treatment.12 It is standard for the directive to come into effect when a person loses capacity to make healthcare decisions.
As with a Will and Power of Attorney, capacity considerations are among reasons to have an Advanced Healthcare Directive prepared in an expedient manner. Should a patient fail to create an Advanced Healthcare Directive or appoint a substitute healthcare decision maker prior to losing capacity, alternate procedures for his or her healthcare decision-making are available. If possible, the nearest relative should make the decision on the patient’s behalf.12 Beyond the nearest relative, each province sets out an ordered list of who is authorized to give consent to care on behalf of the patient.
Despite the importance of these documents, a large number of Canadians do not have them. Only 50.7% of Canadians aged 65 and older have an up-to-date Will, 29% have a Power of Attorney, and 60% of hospitalized patients at high risk of dying have an Advanced Healthcare Directive.Reference Hewson13–15 While these figures are a useful representation of the general population, there is no published data specific to patients with dementia.
Saskatchewan is a western Canadian province with a population of approximately 1 million. About 40% of this population lives in rural areas and small towns.Reference Elliot16 These centers tend to have proportionally larger elderly populations than urban centers, with about one in five rural residents in Saskatchewan older than age 65.Reference Elliot16 Along with the aging population elsewhere in Canada, these residents are at high risk of developing dementia. With a small population dispersed across a large province, geographical location is a critical barrier to accessing healthcare for people in rural communities.Reference Laurent17 To improve access to specialized dementia care for the aging population in rural Saskatchewan, the Rural and Remote Memory Clinic (RRMC) was developed in 2004. At the initial presentation to the clinic, patients are assessed by a neurologist, neuropsychologist, physiotherapist, and dietitian.Reference Crossley, Morgan, Lanting, Dal Bello-Haas and Kirk18 At the end of their visit, patients receive a diagnosis and a treatment plan. The clinic utilizes telehealth to follow-up with patients. This helps to limit the burden placed on caregivers and the healthcare system.Reference McEachern, Kirk, Morgan, Crossley and Henry19 More information on the RRMC is available elsewhere.Reference Crossley, Morgan, Lanting, Dal Bello-Haas and Kirk18–Reference Steve, Kirk and Crossley28
Decision-making is an increasingly important issue for patients with dementia. As the rates of dementia rise, more patients will experience irreversible cognitive incapacity and a loss of autonomy.Reference Charles, Parmar, Bremault-Phillips, Dobbs, Sacrey and Sluggett2 The timely creation of a Will, Power of Attorney, and Advanced Healthcare Directive allows patients to participate in personal and medical decisions and alleviates stress from families. It remains unclear whether or not there are patient characteristics associated with having these documents. The objective of this study was to identify patient factors that are associated with having a Will, Power of Attorney, and Advanced Healthcare Directive in patients presenting to the RRMC. Identifying these factors may help physicians to better understand what makes patients more or less likely to have legal documents.
Methods
Ninety-five consecutive patients seen at the RRMC were included in this study. Sociodemographic and clinical variables were collected from questionnaires completed by patients and caregivers at the initial presentation to the RRMC. Variables include age, sex, ethnicity, years of formal education, education level, marital status, current housing, household members, and relationship of the caregiver to the patient. Cognition was screened with the Mini Mental Status Examination (MMSE).Reference Folstein, Folstein and McHugh29 The Center for Epidemiologic Studies Depression Scale (CES-D) was used to screen for depression.Reference Radloff30 Both patients and caregivers rated the patient’s quality of life and ability to perform activities of daily living using the Quality of Life Scale (QOLS) and the Bristol Activities of Daily Living Scale (BADLS), respectively.Reference Flanagan31–Reference Bucks, Ashworth, Wilcock and Siegfried33 Patients also completed the Instrumental Activities of Daily Living Scale (IADL).Reference Lawton and Brody34 Caregiver-rated functional status of the patient was evaluated by the Functional Assessment Questionnaire (FAQ) and the severity component of the Neuropsychiatric Inventory Scale (NPI-S).Reference Pfeffer, Kurosaki, Harrah, Chance and Filos35, Reference Cummings, Mega, Gray, Rosenberg-Thompson, Carusi and Gornbein36 The Clinical Dementia Rating Scale Sum of Boxes (CDR-SOB) was used to measure the severity of cognitive and functional impairment.Reference Hughes, Berg, Danziger, Coben and Martin32 Patients and their families were asked as part of their routine clinical assessment whether or not the patient had a Will, Power of Attorney, and/or an Advanced Healthcare Directive.
Neuropsychological testing included a 2-hour battery measuring the following cognitive domains: suboptimal performance, estimated premorbid verbal intelligence, expressive and receptive language, simple and complex attention, speed of mental processing, visuoperception/construction, memory, executive function, and social cognition. The battery results in over 100 possible scores, but for the sake of simplicity, we only present some of these scores with an emphasis on higher order cognitive functions. In particular, we include subtests from the Delis–Kaplan Executive Function System (D–KEFS) – specifically the Trail Making Test (Number-Letter Switching: Time-to-Completion), Verbal Fluency Test (Letter Fluency: Total Correct; Category Fluency: Total Correct; Category Switching: Total Correct Responses; Category Switching: Total Switching Accuracy), and Color-Word Interference Test (Inhibition: Time-to-Completion; Inhibition/Switching: Time-to-Completion).Reference Delis, Kaplan and Kramer37 The Logical Memory I and II (immediate and delayed recall of a short story) subtest from Wechsler Memory Scale – Fourth Edition (WMS-IV) and California Verbal Learning Test – Second Edition (CVLT-II) Short-form (immediate recall, learning, free delayed recall, cued delayed recall, recognition) were used to assess memory.Reference Wechsler38, Reference Delis, Kramer, Kaplan and Ober39 At the end of the initial clinic day, patients were given a diagnosis as agreed upon by the assessment team. Data from all 95 patients were analyzed for three separate analyses: the presence of a Will, Power of Attorney, and Advanced Healthcare Directive. For each analysis, patients were sorted into two groups based on whether or not they had the indicated document.
Data underwent statistical analysis using SPSS version 24.40 Descriptive analyses were performed using frequencies, measures of central tendency, and measures of variance. For each of the three categories, the two groups (yes vs no) were compared using independent sample t-tests for continuous variables and χ 2 for categorical variables. Exact test p values were reported when expected values were small. Ethical approval was obtained from the University of Saskatchewan Behavioral Research Ethics Board.
Results
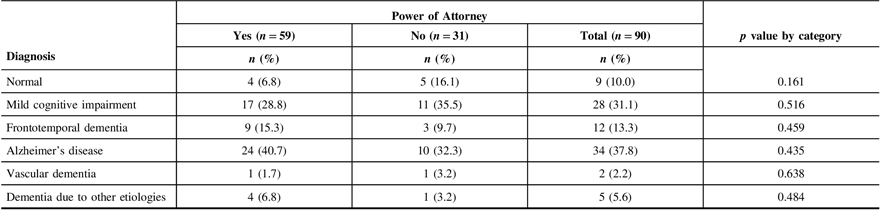
Ninety-five consecutive patients who underwent initial assessment at the RRMC were included in this study. Mean age was 70.84 years (SD = 10.18 years) with a range of 43–90 years and a median age of 72. The sample comprised 46 males (48.4%) and 49 females (51.6%). The most frequent diagnosis was Alzheimer’s disease (N = 34), followed by mild cognitive impairment (N = 28), frontotemporal dementia (N = 12), normal (N = 9), dementia due to other etiologies (N = 5), and vascular dementia (N = 2) (Tables 3, 6, and 9).
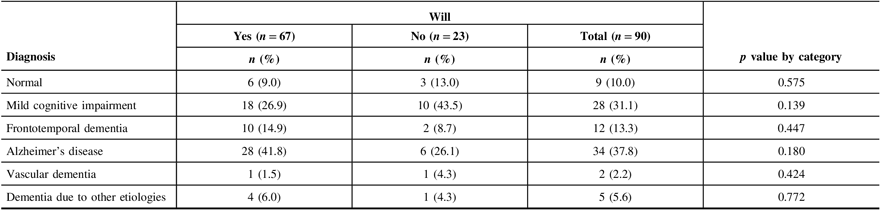
Seventy patients (73.7%) had a Will (Table 1). Patients who lived with others, aside from a spouse only, were significantly less likely to have a Will (p = 0.010). Patients who were accompanied to the clinic by someone other than an immediate family member were also less likely to have a Will (p < 0.0001). European ethnicity was significantly associated with having a Will (p = 0.015). There was no statistically significant difference in age, sex, years of formal education, education level, marital status, or current housing between those who had a Will and those who did not. Patients with a better quality of life, as rated by the patient and the caregiver, were significantly more likely to have a Will (patient p = 0.001; caregiver p = 0.055). There was no significant association between having a Will and MMSE score, depressed mood, or patient function. Neuropsychological data revealed an association between a low verbal fluency performance and having a Will (category switching total [TTL] p = 0.055; category switching accuracy p = 0.025; % set loss errors p = 0.002) (Table 1). Memory performance and severity of cognitive and functional impairment were not significantly associated with having a Will (Table 2). Likewise, there was no significant association between diagnosis (normal, mild cognitive impairment, frontotemporal dementia, Alzheimer’s disease, vascular dementia, and dementia due to other etiologies) and having a Will (Table 3). The full comparison of patients with and without a Will is detailed in Tables 1–3.
Table 1: Characteristics of patients with and without a Will*
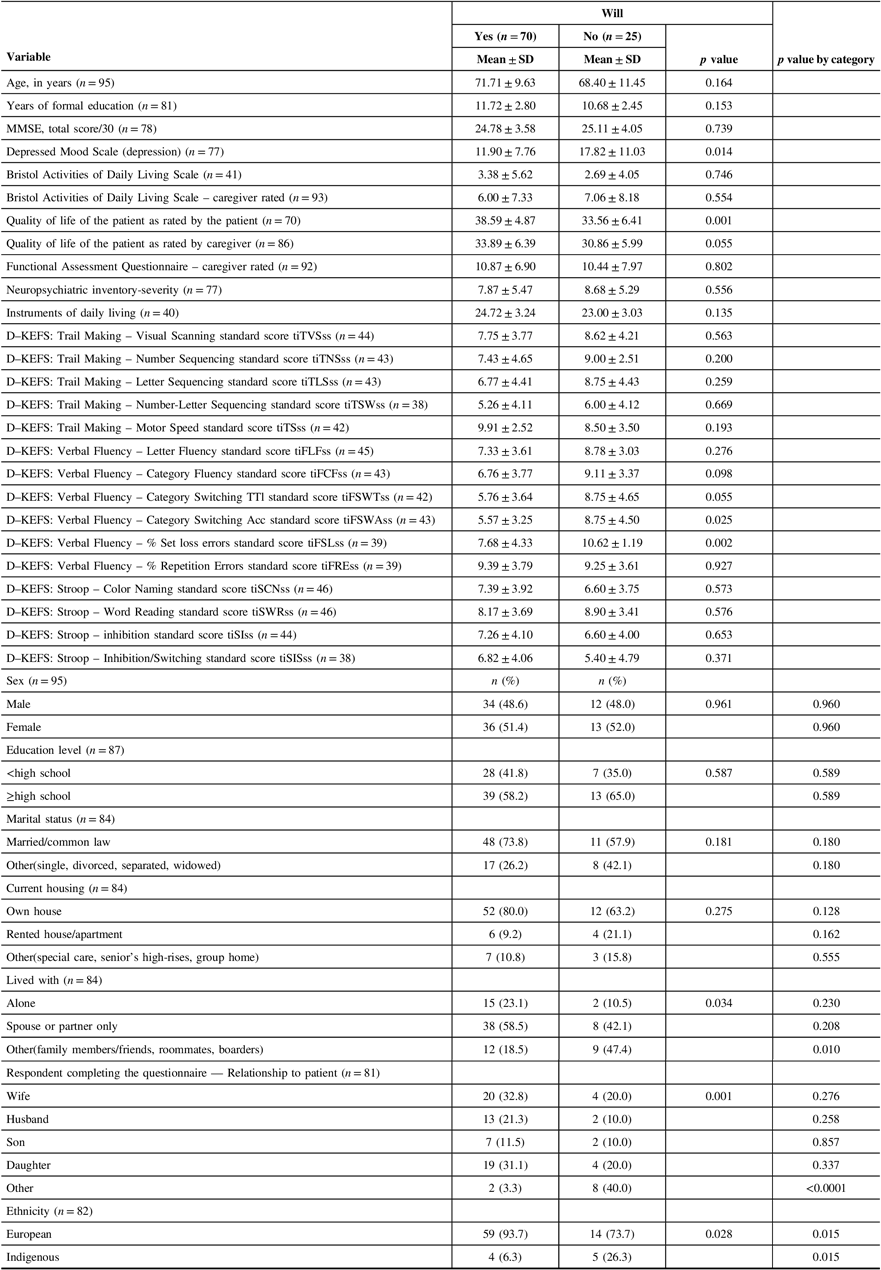
* All variables have missing values except age and sex.
Table 2: Memory and severity characteristics of patients with and without a Will
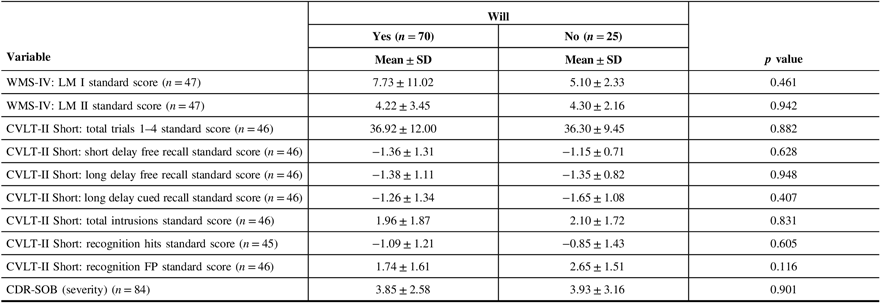
Table 3: Neurological diagnosis of patients with and without a Will
Of the 95 patients in our sample, 62 (65.3%) had a Power of Attorney (Table 4). Living with others, except for a spouse only, was significantly associated with not having a Power of Attorney (p = 0.038). There was no significant difference in age, sex, ethnicity, years of formal education, education level, marital status, current housing, or relationship of caregiver to the patient between patients who had a Power of Attorney and those who did not. Patients who reported a better quality of life were significantly more likely to have a Power of Attorney (patient p = 0.031; caregiver p = 0.050). MMSE, depressed mood, and patient function were not significantly associated with having a Power of Attorney. Lower scores on visual scanning, number sequencing, and letter sequencing were significantly associated with having a Power of Attorney (visual scanning p = 0.009; number sequencing p = 0.010; letter sequencing p = 0.045). Patients with lower scores on verbal fluency were significantly more likely to have a Power of Attorney (category fluency p = 0.015; category switching accuracy p = 0.053) (Table 4). Measures of memory and severity (Table 5) as well as diagnostic category (Table 6) were not significant. The full comparison of patients with and without a Power of Attorney is presented in Tables 4–6.
Table 4: Characteristics of patients with and without a Power of Attorney*
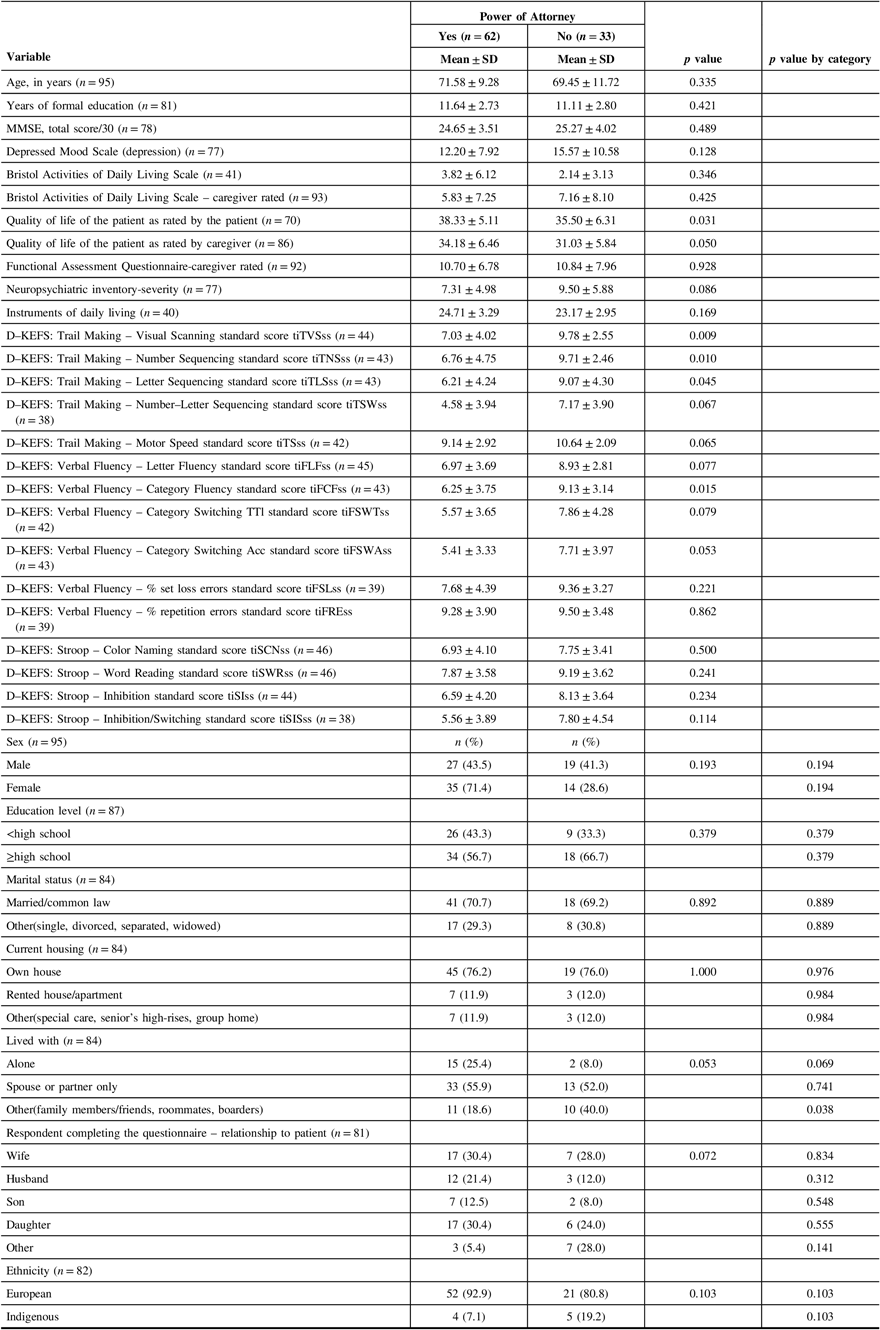
* All variables have missing values except age and sex.
Table 5: Memory and severity characteristics of patients with and without a Power of Attorney
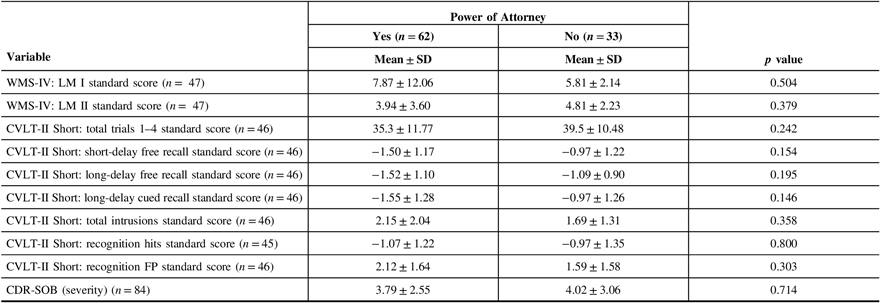
Table 6: Neurological diagnosis of patients with and without a Power of Attorney
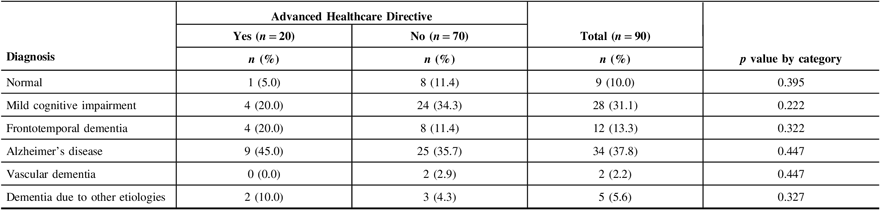
The majority of patients did not have an Advanced Healthcare Directive, with only 21 patients (22.1%) in the “yes” group (Table 7). Patients who had an Advanced Healthcare Directive were significantly older than those who did not (p = 0.015). Living in housing categorized as “other,” such as special care, senior’s centers, and group homes was significantly associated with having an Advanced Healthcare Directive (p = 0.038). There was no association with sex, ethnicity, years of formal education, education level, marital status, relationship of the caregiver to the patient, or with whom the patient lived. Patients with a lower level of caregiver-rated function and independence were significantly more likely to have an Advanced Healthcare Directive (p = 0.047). MMSE, depressed mood, and patient quality of life were not significant. Poor verbal fluency was significantly associated with having an Advanced Healthcare Directive (category switching TTI p = 0.023; category switching accuracy p = 0.004). Other neuropsychological measures including memory were not significant (Table 7). Patients with greater severity of cognitive and functional impairment as measured by CDR-SOB were significantly more likely to have an Advanced Healthcare Directive (p = 0.023) (Table 8). There was no significant association between having an Advanced Healthcare Directive and diagnosis (Table 9). The full comparison of patients with and without an Advanced Healthcare Directive is outlined in Tables 7–9.
Table 7: Characteristics of patients with and without an Advanced Healthcare Directive*
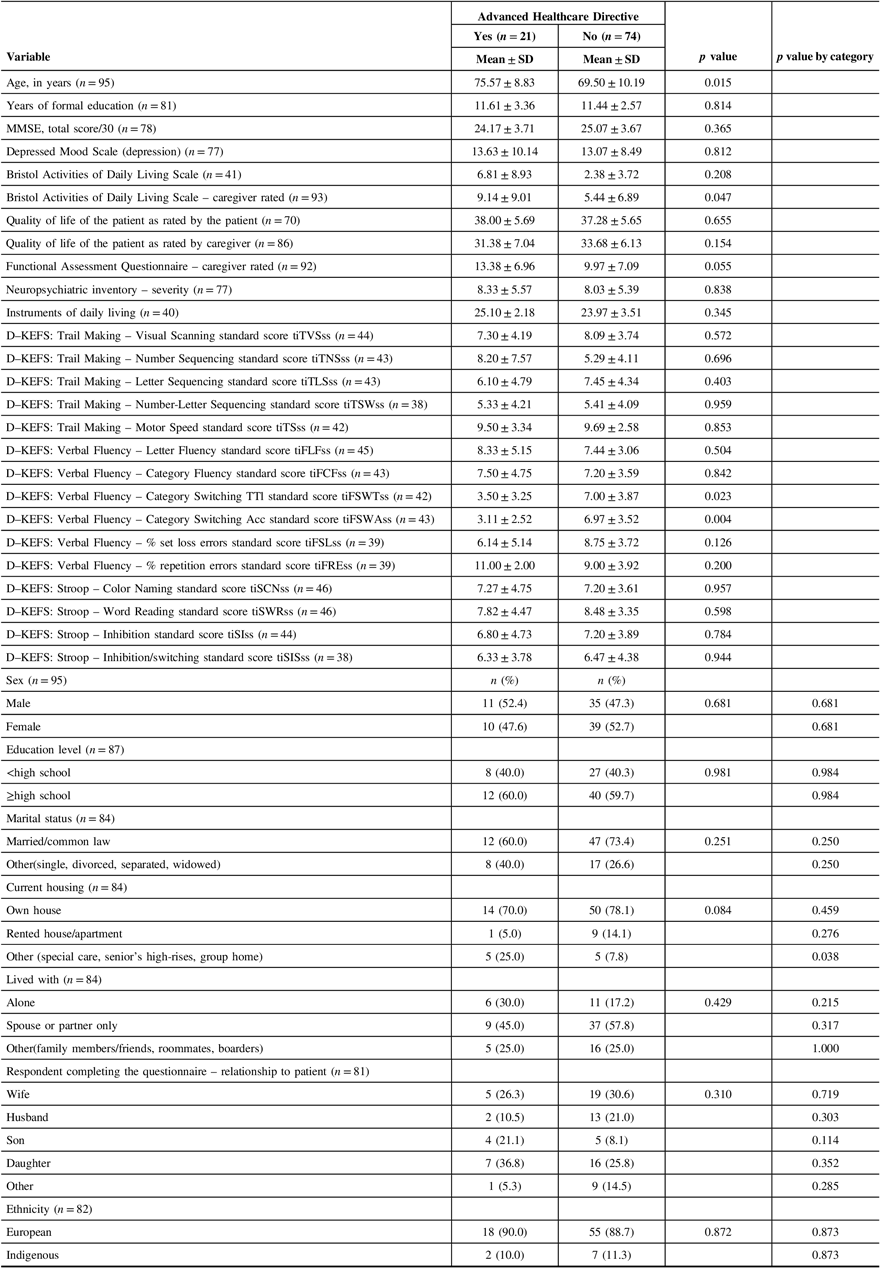
* All variables have missing values except age and sex.
Table 8: Memory and severity characteristics of patients with and without an Advanced Healthcare Directive
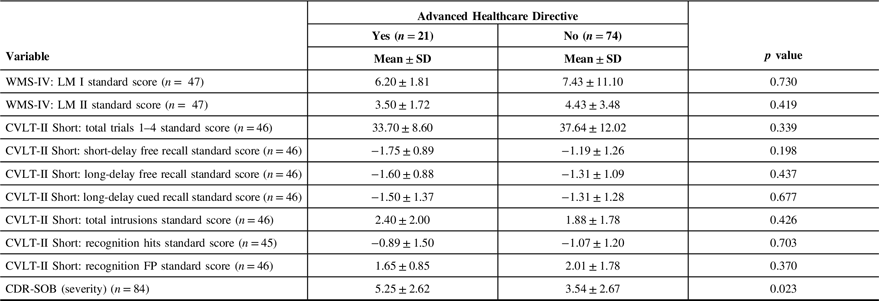
Table 9: Neurological diagnosis of patients with and without an Advanced Healthcare Directive
Discussion
Decision-making requires many of the cognitive domains that are compromised in dementia.Reference Voskou, Douzenis, Exonomou and Papageorgiou5, Reference Burla, Rego and Nunes6 Legal documents such as a Will, Power of Attorney, and Advanced Healthcare Directive become critical for patients who develop significant deficits in cognition. It is unknown whether there exist patient factors that might contribute to a greater likelihood of procuring these documents. In order to better address issues of decision-making and cognitive capacity in patients with dementia, we sought to identify trends in their clinical and demographic characteristics. This may help to recognize patients who are at greater risk of not having legal documents and those who are likely to benefit from further attention to legal planning.
Our data revealed similarities between patients who had a Will and patients who had a Power of Attorney. With whom patients lived was a strong clinical indicator. Patients who lived with others, excluding a spouse or partner only, were less likely to have a Will and Power of Attorney. One explanation for this may be that patients who live with family members, friends, roommates, or boarders do not have ownership or are not the sole owners of the property where they are living, thus decreasing the need to create a Will. Compared to living alone or with a spouse of similar functional capacity, perhaps living with others provides patients with more opportunities to have help with managing their finances, therefore lessening the perceived need for a Power of Attorney. Patients who were accompanied to the clinic by someone other than an immediate family member were less likely to have a Will. Interestingly, older age was not significantly associated with having either a Will or a Power of Attorney.
We found that patients with a Will and/or Power of Attorney tended to have a better quality of life as rated by both the patient and caregiver. It is possible that those with a better quality of life are more impacted by physical and cognitive changes as they age and thus become more aware of the need for a Will or Power of Attorney. The QOLS used to rate quality of life in this study considers factors such as energy level, living situation, family, and money.Reference Flanagan31 Patients who are lacking in any of these areas may experience more difficulty scheduling and keeping an appointment to create a Will or Power of Attorney, or they may not have the finances to do so. Physicians should discuss finances and the ability to execute a plan with patients when recommending that they create legal documents.
A common pattern emerged among patients with a Will, patients with a Power of Attorney, and patients with an Advanced Healthcare Directive. In all three groups, poor verbal fluency was associated with having the specified document. Verbal fluency tasks require patients to retrieve words from their mental lexicon, focus on the task, select words meeting certain constraints, and avoid repetition.Reference Fisk and Sharp41 Thus, deficits in either verbal ability or executive control manifest themselves in poor performance on the fluency tasks.Reference Shao, Janse, Visser and Meyer42 Although it is common to experience word-finding difficulties with normal aging, more profound deficits in verbal ability may indicate cognitive impairment.Reference Burke and Shafto43 It may be that noticeable problems with verbal fluency, unlike other cognitive deficits, spur family members to recognize there is a problem and to advocate for the completion of legal documents. Interestingly, measures of memory were not strongly associated with having any of the three legal documents. In contrast to language difficulties, patients may be more able to hide their memory problems in the early stages of dementia. Compensatory strategies used by patients with memory loss may include avoiding tasks that they no longer remember how to perform, relying on their spouse to fill in memory gaps or inventing stories to excuse lapses in memory.Reference Dixon, Hopp, Cohen, de Frias and Backman44 Caregivers and family members may fail to recognize changes in the patient’s memory or attribute memory problems to normal aging.Reference Perry-Young, Owen, Kelly and Owens45, Reference Ahmed, Mitchell, Arnold, Dawson, Nestor and Hodges46
Our data revealed that lower scores on Trail Making tasks were associated with having a Power of Attorney. Trail Making tasks reflect a wide variety of cognitive processes including simple and complex attention, visual search and scanning, psychomotor integration, sequencing and shifting, flexibility, ability to execute and modify a plan of action, and ability to maintain two trains of thought simultaneously.Reference Salthouse47 It is possible that many of these cognitive functions are involved in managing finances or maintaining a budget. Thus, patients who demonstrate poor performance on Trail Making tasks may also have an increased need for a Power of Attorney.
Social and cultural factors may play a role in how likely a patient is to create legal documents. All of the non-European patients included in our study were Indigenous. We found that patients of European ethnicity were more likely to have a Will, whereas patients of Indigenous background were less likely to have a Will. Indigenous people make up about 16% of the population of Saskatchewan, with about 65% identifying as First Nations, 33% as Metis, 0.2% as Inuit, and 1% as other or more than one Indigenous identity.48 Over half (53%) of all First Nations people in Saskatchewan live on a reserve.48 Indigenous patients face special barriers to accessing the legal system. Common barriers include a lack of legal services within Indigenous communities, systemic racism, a distrust for the fairness of the legal system, and a lack of transportation to reach existing legal services.Reference Wright49 Furthermore, Indigenous populations live as the lowest economic group in Canada, adding an additional impediment to legal planning, given the high cost of most legal services.Reference Morse50 It should be noted that legal planning for Indigenous populations is a distinct topic and is beyond the scope of this discussion.
Having an Advanced Healthcare Directive was associated with factors that were not related to having a Will or Power of Attorney. Older patients were more likely to have an Advanced Healthcare Directive than younger patients. Impaired function and a high level of dependency as determined by the FAQ and BADLS were also significant. Similarly, patients with greater severity of cognitive and functional impairment were more likely to have an Advanced Healthcare Directive. Current housing type classified as “other,” which included senior’s centers, group homes, and special care homes, was also positively associated. These results are consistent with the well-known finding that many patients over age 65 experience increased medical morbidity and are less likely to live independently in the community.Reference Salive51 Living with multiple chronic conditions is associated with elevated risk of death, disability, and poor functional status.Reference Salive51 Consequently, these patients are more likely to express their medical wishes. There was likely a bias toward having an Advanced Healthcare Directive in patients living in an “other” housing category. Advanced Healthcare Directives are often discussed with patients and families at the time of admission to long-term care and may even be required by some residences.
We anticipated that patients with worse scores on the MMSE and more advanced dementia would be more likely to have legal documents. Our findings, however, indicate no significant association between MMSE score or diagnosis and having any of the three legal documents. This raises concern because patients with poor cognition will have greater difficulty creating legal documents due to a potential lack of testamentary capacity.Reference Voskou, Douzenis, Exonomou and Papageorgiou5 As there are no definitive predictors of who will develop dementia and who will not, it is important to create a Will, Power of Attorney, and Advanced Healthcare Directive when one is still in good health.Reference Verity, Kirk, O’Connell, Karunanayake and Morgan21
Limitations to this study include a relatively small sample size and a cross-sectional study design where patient follow-up is not reported. Longitudinal follow-up would benefit future research in this area. Our study only included patients from rural areas. Access to lawyers is more difficult in rural centers compared to urban centers. For instance, there is only one private lawyer who serves the entire northern half of Saskatchewan. It would be interesting to compare data from our study with that of patients living in urban centers.
Conclusion
In this study, we observed a number of differences between patients who had a Will, Power of Attorney, and/or Advanced Healthcare Directive and those who did not. While there is no single indicator of having these documents, taking age, living situation, ethnicity, quality of life, functional status, and language difficulties into consideration may help to recognize patients who are at increased risk of leaving their legal affairs unattended to. Physicians who work with elderly populations, especially primary care physicians, can play an important role in enhancing patient access to the legal system. In particular, physicians can counsel patients who demonstrate risk factors for requiring further attention to legal planning. These risk factors may include being of older age, living at home with others, being of Indigenous background, having poor quality of life, having good functional status, and having good language fluency. By discussing legal documents early on with patients who might be at risk, we can better address challenges in legal and medical decision-making that arise when patients develop cognitive impairment.
Acknowledgements
Funding from the Saskatchewan Ministry of Health supports clinical staff in the Rural and Remote Memory Clinic where the data were collected.
Disclosures
DM receives grants from the Canadian Institutes of Health Research (CIHR). SL, AK, EAK, CK, and MOC have nothing to disclose.
Statement of Authorship
SL wrote the manuscript. AK developed the research question, oversaw data collection, and assisted with manuscript preparation. EAK wrote sections of the manuscript pertaining to legal subject matter and assisted with manuscript preparation. CK performed the statistical analysis and assisted with manuscript preparation. MOC oversaw neuropsychological testing and assisted with manuscript preparation. DM oversaw data collection and assisted with manuscript preparation.













