Nutritional status declines in old age. In the UK National Diet and Nutrition Survey the proportion of free-living individuals aged 75 years old with biochemical evidence of deficiency was approximately 8 % for Fe, 10 % for vitamin B12, 30 % for folate and 18 % for vitamin C, while 10 % men and 20 % women were deficient in vitamin DReference Finch, Doyle, Lowe, Bates, Prentice, Smithers and Clarke1. The high prevalence of nutritional deficiency in old individuals is partly due to reduced appetite and lower physical activity as a result of musculo-skeletal and other health problems. The decrease in energy and nutrient intake may be compounded by malabsorption due to poor function of the digestive system or side effects of medication.
There is limited evidence for a relationship between low nutritional status and subsequent mortality in old individuals. A 29-year cohort study based on the 1969 Busselton Health Survey in Western Australia found no association between folate or vitamin B12 status and all-cause mortalityReference Hung, Beilby, Knuiman and Divitini2. By contrast, a 4-year cohort study of individuals over 75 years old living in the community in the UK found that those in the lowest quintile of vitamin C status had a significantly lower hazard ratio for all-cause mortality than those in the highest quintileReference Fletcher, Breeze and Shetty3. A beneficial effect of vitamin C was also suggested by large cohort studies which included younger adultsReference Khaw, Bingham, Welch, Luben, Wareham, Oakes and Day4, Reference Simon, Hudes and Tice5. A 31-month follow up of men and women living in residential age care facilities in Sydney, Australia found that vitamin D status was significantly associated with all-cause mortality after adjustment for age and sex, though this effect was not seen after further adjustment for confounding variables such as health status at baselineReference Sambrook, Chen, March, Cameron, Cumming, Lord, Schwarz and Seibel6.
In an earlier study designed to identify predictors of poor nutritional status in later life, we obtained measurements of blood markers of Fe, vitamin B12, folate, vitamin C and vitamin D status in 398 men and women over 75 years old living in the community. In the present study we investigated possible associations between these blood nutrient levels and mortality in the following 5 years.
Methods
Participants and measurement of nutritional status
A full description of the recruitment of subjects and methods of measurement of blood analytes has been reported elsewhereReference McNeill, Vyvyan, Peace, McKie, Seymour, Hendry and McPherson7. Briefly, a random sample of individuals aged 75 years old or over living in the community in Aberdeen, Scotland were selected from the Community Health Index (CHI), a comprehensive list of all patients registered with family doctors in the UK National Health Service. A small number of individuals with terminal illness or severe dementia that could have led to difficulties cooperating with the study were excluded by their family doctor. Initially, 821 men and 1122 women were invited to participate by letter and 208 (25 %) men and 197 (17 %) women agreed to participate and completed the study. A 114-item health and lifestyle questionnaire (including sunlight exposure, supplement use and intake of selected foods) was administered in the participants' homes by a research nurse who also measured height and weight and took a venous blood sample. The blood samples were taken in the morning after a light breakfast without fruit juice or breakfast cereal. The samples were treated with EDTA and stored at − 70°C before analysis of plasma vitamin C by HPLC and serum 25-hydroxycholecalciferol (25-OHD), vitamin B12 and ferritin and erythrocyte folate by RIA.
Mortality
Deaths of participants were determined up to 12 December 2005 by matching with the Grampian CHI and records kept by the General Register Office for Scotland (GROS)8, which incorporates information on deaths occurring in England. Seven participants who were recorded as having died on the CHI but not with the GROS were assumed to have died. Four participants who were recorded on the CHI as having moved out of Scotland but were not recorded as having died with the GROS were assumed to be still living. The GROS also supplied information on causes of death, with the 10th International Classification of Disease (ICD-10) used for deaths which occurred after November 1999 and ICD-9 used for those occurring before this time.
Data analysis
For all models, survival time was a continuous variable which ranged 0–80 months from the baseline measurements. Sex-specific quintiles of blood markers of nutritional status were created, with quintiles ranging from 1 (lowest) to 5 (highest). Two participants with the highest serum ferritin levels (1232·0 and 1847·0 μg/l) were excluded from the analysis for Fe as these levels were assumed to reflect recent infection. The relationship between baseline nutritional status and mortality was assessed using a test for linear trend across the quintiles in logistic regression. Hazard ratios were estimated using Cox proportional hazard models for quintiles 1–4 referent to quintile 5. The analysis was carried out in all subjects together and in men and women separately. The sample size provided 80 % power at a 5 % significance level to detect hazard ratios of 2·7 or greater between the highest and any other quintile, assuming a mortality rate of 60/1000 individual years. Adjustment for confounding variables that could affect mortality was included in models 1–3. In model 1, results were adjusted for age and sex. In an effort to control for pre-existing illness, self-perceived health status and taking five or more kinds of medicine were added into model 2. Model 3 adjusted the results further by adding self-reported heart disease and/or diabetes at baseline.
To test the possibility that any relationship between vitamin D status and survival could be the result of reverse causation, with participants who were ill having lower sunlight exposure as a result of their illness, we assessed whether associations between survival and vitamin D status could be attenuated by including two covariates which influence vitamin D levels, i.e. sunlight exposure and use of a supplement containing vitamin D, either separately (models 4 and 5 respectively) or in combination (model 6). Sunlight exposure was estimated from three variables in the baseline survey: season of blood sampling, frequency of sunbathing and participation in outdoor physical activity.
All analysis was carried out using SPSS version 14.0 (SPSS Inc., Chicago, IL, USA).
Results
Overall, seventy-one men (34·3 %) and fifty-eight women (30·4 %) had died by 12 December 2005. The median time of follow up was 69·2 (range 1·0–79·9) months. Among those who had died, 32·8 % men and 25·9 % women had died from IHD (ICD-10 codes I20–I25 or ICD-9 codes 410–414), 11·9 % men and 24·0 % women had died from cerebrovascular disease (ICD-10 codes I60–I69) and 30·0 % men and 15·5 % women had died from cancer (ICD-10 codes C00–C97). The average mortality rate during the follow-up period in the study participants was 56/1000 population per year (61/1000 in men and 53/1000 in women). This was lower than the mortality rate of the population of Grampian, Scotland aged 75 years old or over in 2005 of 93/1000 in men and 80/1000 in women8, which probably reflects the fact that those who participated in the original study were more likely to have been in good health at the time of recruitment than those who did not participate.
Table 1 presents the general characteristics of the study participants. More than half of the participants reported having heart disease in 1999–2000 while 13·3 % were supplement users (defined as taking any kind of nutrient supplement at least once per d). Men had a higher income, a better self-perceived health status, were more physically active and were more likely to spend time outdoors in sunny weather than women. Women had higher plasma vitamin C status than men while men had higher levels of serum ferritin, erythrocyte folate and serum 25-OHD. Survivors were significantly younger, had a slightly higher BMI, were less likely to have heart disease and/or diabetes at baseline, were less likely to be taking more than five kinds of medicine, generally had a better self-perceived health status, were more likely to be physically active, spend time outdoors in sunny weather and to take a supplement containing vitamin D than those who died. Survivors also had significantly higher plasma vitamin C and serum 25-OHD levels than those who had died.
Table 1 General characteristics of study participants (n 398) (Medians and ranges)

25-OHD, 25-hydroxycholecalciferol.
* P value for difference between men and women.
† P value for difference between survivors and non-survivors (χ2 test for categorical variables and Mann–Whitney test for continuous variables, two-tail).
‡ Only 356 participants with BMI available, as height of others could not be measured due to difficulty with standing up straight.
§ Any exercise other than walking, for example, dancing, bowling, gardening or swimming.
‖ Taking nutrient supplement at least once per d.
¶ Two participants who had the highest ferritin levels (1232·0 and 1847·0 μg/l) were excluded.
Table 2 shows the hazard ratios for mortality across the quintiles and the significance of linear trends. There was no trend in the associations between quintiles of serum ferritin, serum vitamin B12, erythrocyte folate or plasma vitamin C status and mortality but for vitamin C the participants in the lowest quintile had significantly higher mortality than those in the highest quintile in all three models. Serum 25-OHD had a highly significant inverse relationship with risk of death, with participants in the lowest quintile having over twice the risk of those in the highest quintile.
Table 2 Hazard ratios (HR) of risk of death referent to the highest quintile of baseline nutritional status and significance of linear trends across sex-specific quintiles for men and women combined

25-OHD, 25-hydroxycholecalciferol.
* Total number of participants n 398 apart from ferritin (n 396) and folate (n 391).
† Model 1, adjusted for age and sex.
‡ Model 2, model 1+ taking five or more kinds of medicine and self-perceived health status.
§ Model 3, model 2+ having heart problem and/or diabetes at baseline.
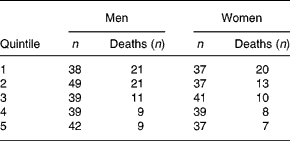
When the analysis for vitamin D was repeated for men and women separately, the trends remained significant in both men and women (both P = 0·02) (Figs. 1 (a) and (b) and Table 3).

Fig. 1 Survival curves for quintiles (Q) of baseline serum 25-hydroxycholecalciferol (25-OHD) in men (a) and women (b). Hazard ratios (HR) were adjusted for variables in model 3 (see Table 2), i.e. age, taking five or more kinds of medicine, self-perceived health status and pre-existing heart disease and/or diabetes. The linear trend across quintiles was significant for both men (P for trend 0·02) and women (P for trend 0·02).
Table 3 Numbers of participant and numbers of deaths in each quintile
When sunlight exposure and vitamin D supplementation were added into the models the hazard ratios were attenuated but the trend across quintiles was still significant (Table 4).
Table 4 Hazard ratios (HR) of risk of death referent to the highest quintile of serum 25-hydroxycholecalciferol concentrations (nmol/l) and significance of linear trends across sex-specific quintiles for men and women combined

* Model 3, adjusted for age, sex, taking five or more kinds of medicine, self-perceived health status and pre-existing heart disease and/or diabetes.
† Model 4, model 3+ sunlight exposure, i.e. season of blood sampling + sunbathing + outdoor physical activity.
‡ Model 5, model 3+ use of a supplement containing vitamin D.
§ Model 6, model 3+ variables in model 4 and model 5.
Discussion
Comparison with other studies
The results of the present study are consistent with an inverse association between vitamin D status and mortality. They also provide some evidence for an inverse association between vitamin C status and mortality, but no evidence for any association between Fe, vitamin B12 or folate status and mortality. The lack of association between blood Fe status and mortality is consistent with results from the NHANES II mortality studyReference Mainous, Wells, Carek, Gill and Geesey9 in which associations were found only in those who had elevated Fe storage with high dietary Fe intake or high meat consumption, as only 2·9 % men and 7·9 % women in the present study had elevated Fe storage (defined as ferritin levels above 300 μg/l in men or above150 μg/l in womenReference Dacie and Lewis10). The lack of association between vitamin B12 or folate status and mortality is consistent with the results from the Busselton Health SurveyReference Hung, Beilby, Knuiman and Divitini2. The finding that those in the highest quintile of plasma vitamin C status had a significantly lower risk of death than those in the highest quintile is consistent with the results from other studiesReference Fletcher, Breeze and Shetty3–Reference Simon, Hudes and Tice5, though in the present study there was no significant trend across the quintiles, as was seen in the other studies.
One possible explanation for the inverse association between blood vitamin D status and mortality is that participants who had serious illness at baseline would have spent more time indoors which would lead to a low vitamin D status. However, this would be expected to lead to a greater association with survival in the early years of follow up whereas the slope of the survival curves for the first few years of follow up was similar to that in the later years (Figs. 1 (a) and 1 (b)). The fact that the association was attenuated when sunlight exposure and taking supplements containing vitamin D were included in the model also supports the possibility that the association could be causal. However, the association was not abolished in these models, which could reflect residual confounding by factors such as dietary intake or hormonal status, which were not measured in the original survey, or that sunlight exposure was not assessed accurately by the questionnaire. The results for vitamin D in the present study are similar to those of a study of participants of mean age 83 years carried out in AustraliaReference Sambrook, Chen, March, Cameron, Cumming, Lord, Schwarz and Seibel6 who had lower serum 25-OHD levels than participants in the present study despite living at lower latitude (33·6°S) than Aberdeen (57·9°N). In the Sydney study the hazard ratio for the vitamin D-sufficient group compared with that of the deficient group (serum 25-OHD < 39 nmol/l) was 1·39 (95 % CI 1·17, 1·65) (P = 0·01). While the association was not significant after adjustment for parathyroid hormone status, this could reflect the fact that parathyroid hormone status has a direct effect on vitamin D levels. Further evidence that vitamin D may have a protective effect on survival in older individuals is provided by a study of vitamin D supplementation in men and women aged 65–85 years in the UK in whom oral vitamin supplements given at 4-monthly intervals led to a reduced hazard ratio for death from all causes (hazard ratio 0·88 (95 % CI 0·74, 1·06)) over 5 yearsReference Trivedi, Doll and Khaw11.
Possible mechanisms for an association between vitamin D and survival
In adults vitamin D deficiency causes secondary hyperparathyroidism that can precipitate and exacerbate osteoporosis and osteomalacia and hence fractures, while vitamin D deficiency has also been found to increase the risk of many other common and life-threatening diseases in old individuals, including some common cancers, CVD and type 1 diabetesReference Holick12. 1,25-Dihydroxyvitamin D has been found to down regulate hyperproliferative cell growth, thereby possibly suppressing the development of cancerReference Feldman, Zhao and Krishnan13, Reference Lowe, Guy, Mansi, Peckitt, Bliss, Wilson and Colston14. 1,25-Dihydroxyvitamin D also has the ability to down regulate renin and angiotensin production, thereby decreasing blood pressure and CVD riskReference Li, Kong, Wei, Chen, Liu and Cao15. 1,25-Dihydroxyvitamin D can also activate T and B lymphocytes and macrophages which may explain the associations of vitamin D with the incidence of most common autoimmune diseases including type 1 diabetesReference Gregori, Giarratana, Smiroldo, Uskokovic and Adorini16.
Strength and limitations of the present study
The participants in the present study were similar to the local population in aspects of socio-economic statusReference Hung, Beilby, Knuiman and Divitini2. All deaths occurring in the UK were likely to have been recorded on the CHI or GROS, but the lower mortality rate in the participants compared with the general population contributed to reduced power to detect associations between mortality and nutrient status. The fact that the blood samples were taken in the morning without the subjects having had fruit juice or breakfast cereal reduced the possibility of variation in vitamin C, Fe and folate levels due to recent ingestion. However, blood nutrient levels may vary within subjects and do not necessarily reflect concentrations in other tissues.
Around half of the participants in the present study reported having heart disease at baseline, and we cannot rule out the possibility that pre-existing disease contributed to the lower vitamin C or vitamin D levels, though including pre-existing disease in the model did not affect the associations. To assess whether the associations are seen in those with no pre-existing disease would require a larger study in healthy older individuals.
Summary
In summary, we found evidence for an association between serum 25-OHD levels and all-cause mortality, with some evidence to suggest that this association might reflect reverse causation. We also found weaker evidence for an association between vitamin C levels and all-cause mortality. Blood vitamin D status can be increased by spending time outdoors in sunny weather, increasing intake of food rich in vitamin D such as oily fish, dairy products or fortified margarine or breakfast cereals or taking cod-liver oil or other supplements with vitamin D, while vitamin C levels can be increased by increasing consumption of citrus fruit or juice or taking supplements containing vitamin C. All of these are low-cost interventions with little risk of side effects. Further randomized trials of improving dietary intake or increasing sunlight exposure in large numbers of subjects will be needed to assess whether the associations reported here could be causal and whether lifestyle changes could contribute to improved survival in older individuals.
Acknowledgements
We thank Val Angus for providing data on survival status from the CHI.









