Current recommendations advise initiation and continuation of breast-feeding for more than 6 months to promote child health(Reference Gartner, Morton and Lawrence1–4). Previous studies have suggested that breast-feeding has protective effects on the risks of CVD in adulthood(Reference Martin, Ben Shlomo and Gunnell5, Reference Ravelli, van der Meulen and Osmond6). Also, several studies have suggested that breast-feeding leads to a lower risk of obesity in later life(Reference Gartner, Morton and Lawrence1–Reference Martin, Ben Shlomo and Gunnell5). These associations have been shown in several studies and meta-analyses, also after adjustment for several potential confounders(Reference Owen, Martin and Whincup7). Furthermore, a dose-dependent association has been shown, suggesting that a longer duration of breast-feeding is associated with a lower BMI in older children and adulthood(Reference Harder, Bergmann and Kallischnigg8).
Studies on the associations of breast-feeding with the risks of overweight and obesity in early childhood are scarce and have shown inconsistent results(Reference Beyerlein, Fahrmeir and Mansmann9–Reference Agras, Kraemer and Berkowitz11). This inconsistency may be due to differences in study designs, indicators of overweight or obesity and assessment of breast-feeding(Reference Anderson12). Also, not all studies have data available about the exclusivity of breast-feeding. Assessing the associations of breast-feeding and childhood obesity at young ages is important since the risk of developing obesity may be partly explained by early postnatal growth patterns(Reference Anderson12). These growth patterns in early childhood might be intermediates in the associations of breast-feeding with obesity in later life(Reference Stettler, Stallings and Troxel13). Especially, high growth rates during the first months of life are associated with metabolic syndrome outcomes(Reference Stettler, Bovet and Shamlaye14, Reference Leunissen, Kerkhof and Stijnen15).
We hypothesised that prolonged duration and exclusivity of breast-feeding lead to lower growth rates during the first year of life and subsequently to lower risks of overweight and obesity in preschool children. We examined, in a population-based prospective cohort study among 5047 children, the associations of breast-feeding duration and exclusivity with growth rates in infancy and the risks of overweight and obesity until the age of 3 years.
Methods
Design
The present study was embedded in the Generation R Study, a population-based prospective cohort study of pregnant women and their children from fetal life onwards in Rotterdam, The Netherlands(Reference Jaddoe, Bakker and van Duijn16, Reference Jaddoe, van Duijn and van der Heijden17). Enrolment in the study was aimed at early pregnancy (gestational age < 18 weeks) but was possible until birth of the child. Assessments during pregnancy included physical examinations, fetal ultrasound examinations and administration of questionnaires(Reference Jaddoe, van Duijn and van der Heijden17). All children were born between April 2002 and January 2006 and form a prenatally enrolled birth cohort with a planned follow-up until young adulthood.
Postnatal growth data for the present study were available until the age of 3 years. Of all eligible children in the study area, 61 % participated in the study at birth(Reference Jaddoe, van Duijn and van der Heijden17). The present study was conducted according to the guidelines laid down in the Declaration of Helsinki, and all procedures involving human subjects were approved by the Medical Ethical Committee of the Erasmus Medical Center, Rotterdam, The Netherlands. Written informed consent was obtained from all participants.
Duration and exclusiveness of breast-feeding
Information about breast-feeding initiation and continuation was obtained from delivery reports and postal questionnaires at the ages of 2, 6 and 12 months after birth(Reference Jaddoe, van Duijn and van der Heijden17). Mothers were asked whether they ever breast-fed their child (yes, no) and at what age they quitted breast-feeding. Subsequently, breast-feeding duration was categorised into four groups: (1) never; (2) less than 3 months; (3) 3–6 months; (4) 6 months or longer. Duration of exclusive breast-feeding was defined by using information about at what age other types of milk and/or solids were introduced in the first 6 months of life, according to a short FFQ. The information about duration and exclusiveness of breast-feeding was combined and categorised into the following three categories: (1) never; (2) partial breast-feeding until 4 months; (3) exclusive breast-feeding until 4 months. ‘Never’ indicates infants who were never breast-fed. ‘Partial’ indicates infants receiving breast-feeding, formula-feeding and/or solids in the first 4 months. ‘Exclusive’ indicates infants who have been breast-fed, without any other milk, solids or fluids during the first 4 months.
Postnatal growth characteristics
Postnatal growth was repeatedly measured at the community health centres according to a standard schedule and procedures by well-trained staff at the median ages of 3·1 months (95 % range 1·1–4·5), 6·6 months (95 % range 5·2–10·7), 13·0 months (95 % range 11·1–15·9), 24·3 months (95 % range 18·2–28·3) and 36·4 months (95 % range 30·4–39·9). Length was measured in the supine position to the nearest millimetre until the age of 14 months using a neonatometer, after which height was measured in standing position by a Harpenden stadiometer (Holtain Limited, Crymych, Dyfed, UK). Weight was measured using a mechanical personal scale (SECA, Almere, The Netherlands). BMI (kg/m2) was calculated. Standard deviation scores (SDS) for postnatal growth characteristics were obtained using Dutch reference growth charts (Growth Analyzer 3.0; Dutch Growth Research Foundation, Rotterdam, The Netherlands). Relative overweight was defined as a BMI >1·1–2·3 SDS (approximate adult BMI of 25–30 kg/m2), and obesity was defined as a BMI >2·3 SDS (approximate adult BMI >30)(Reference Fredriks, van Buuren and Wit18). Growth rates were defined as the change in SDS in age intervals between 0–3, 3–6 and 6–12 months.
Covariates
Gestational age, sex and birth weight were obtained from midwife and hospital registries at birth. Information about highest attained maternal educational level (low, moderate and higher), maternal ethnicity (European, non-European) and parity (primiparity, multiparity) was obtained at enrolment in the study. Ethnicity and educational level of the parents were defined according to the classification of Statistics Netherlands(19, 20). Information on maternal smoking (yes, no) and alcohol consumption during pregnancy (yes, no) was retrieved from prenatal questionnaires. Maternal height and weight were measured at enrolment while the mother stood without shoes and heavy clothing, and BMI was calculated (kg/m2). Maternal age was registered at enrolment.
Population for analysis
In total, 7295 children and their parents participated in the postnatal phase of the study and gave consent for participating in the questionnaire studies (Fig. 1). Children without complete information on breast-feeding and twins were excluded from the analyses. Of the remaining singleton live births with complete data on breast-feeding, information about postnatal growth characteristics that measures at least one age was available in 5074 children.
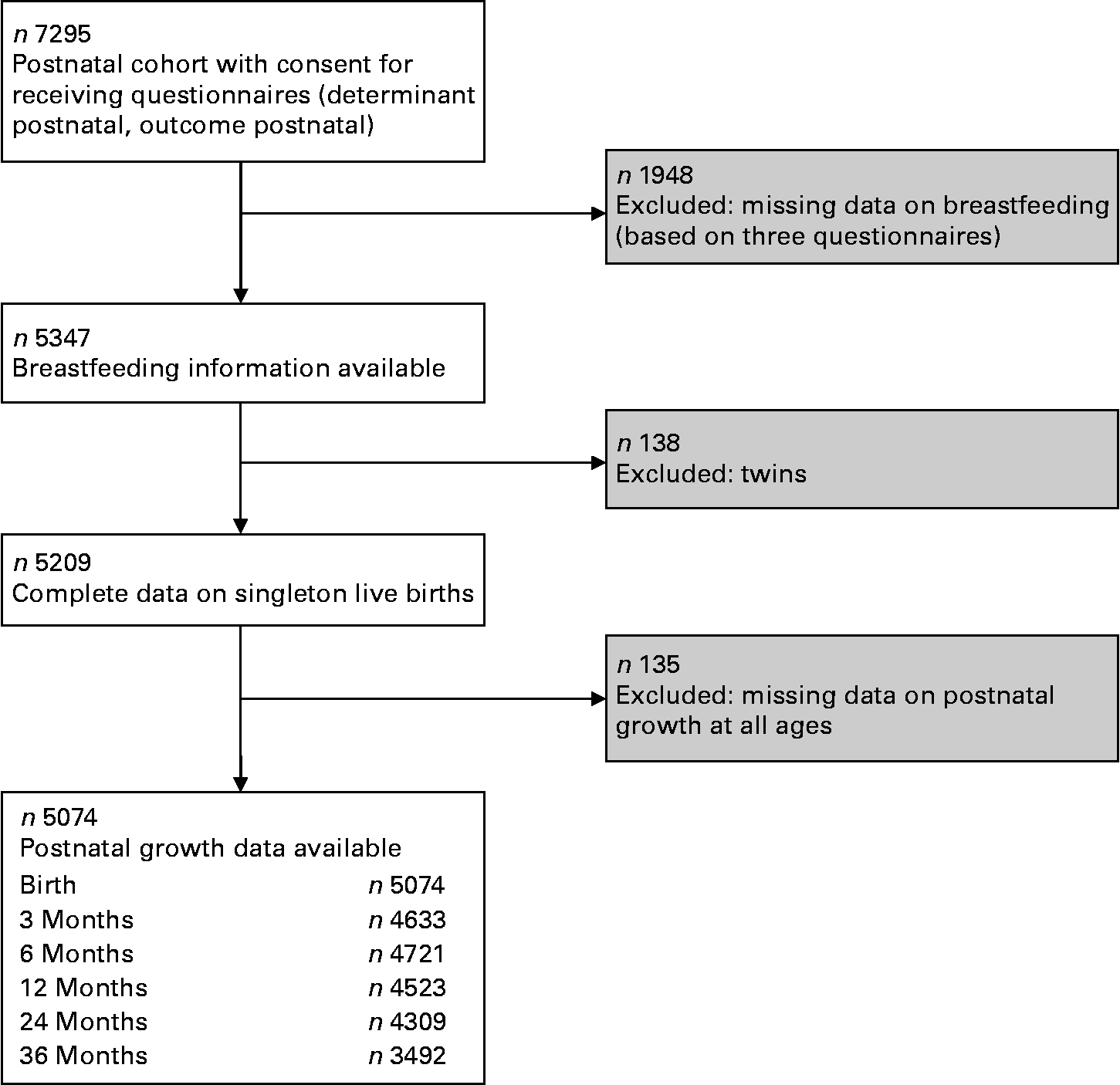
Fig. 1 Flow chart of participants in the study.
Statistical analysis
Differences in baseline characteristics between the breast-feeding duration categories were compared with ANOVA for continuous variables and χ2 tests for categorical variables. The associations of breast-feeding (never, ever), breast-feeding duration (never, 0–3, 3–6 and 6–12 months) and breast-feeding exclusivity (never, partial until 4 months and exclusive until 4 months) with the change in postnatal growth characteristics (length, weight and BMI) in SDS for different age periods (0–3, 3–6 and 6–12 months) were assessed using multiple linear regression models. Both dependent and independent variables were quantitative, and categorical variables were recoded to binary variables. The models were adjusted for potential confounders including child's age at visit, sex, birth weight, gestational age, maternal ethnicity, maternal education, maternal BMI, parity and smoking. Gestational age at enrolment was not included in the models since it did not materially change the results. Confounders were included in the models based on the literature or a change in effect estimates of more than 10 %. We used the ‘enter’ method for including and excluding the independent variables.
For the analyses focused on the associations of breast-feeding duration with growth characteristics until the age of 3 months, we combined the breast-feeding groups into never and ever (0–3, 3–6 and >6 months). For the analyses focused on growth characteristics at the age of 3–6 months, we combined the breast-feeding duration groups into never, 0–3 and 3–6 months (3–6 and >6 months). Furthermore, we examined the associations of breast-feeding duration and exclusivity with differences in BMI at the ages of 1, 2 and 3 years, and the risks of overweight and obesity at the same ages, using linear regression and logistic regression models, respectively. Finally, we assessed the associations of breast-feeding duration and exclusivity with longitudinally measured SDS of BMI in terms of overweight or obesity (combined outcome BMI >1·1 SDS) using the generalised estimating equation, taking into account correlations within subjects and assessing both time-dependent and -independent associations.
Tests for trends were performed by treating each categorised variable as a continuous term and by entering the variable into the fully adjusted linear regression model. To handle missing values in covariates, we performed multiple imputations by generating five independent datasets for all analyses. For the generalised estimating equation analyses, we performed multiple imputations of the data using Proc MI and Proc MIAnalyze. Imputations were based on the relationships between all covariates included in the present study. All measures of association are presented with their 95 % CI. Cross-sectional analyses were performed using the Statistical Package of Social Sciences version 17.0 for Windows (SPSS, Inc., Chicago, IL, USA). The generalised estimating equations analysis, including the Prox Genmod module, was performed with the Statistical Analysis System (version 9.1; SAS Institute, Inc., Cary, NC, USA).
Results
Of the total group of 5074 children, 89·8 % had ever been breast-fed (Table 1). Compared with mothers who breast-fed their children for more than 6 months, those who never breast-fed their children tended to have a younger age, higher BMI, higher rate of obesity, lower educational level, Dutch or European background and were more likely to smoke during pregnancy. Also, children who were never breast-fed had a lower weight at birth and a higher prevalence of small size for gestational age and pre-term birth (all P < 0·05). The median duration of breast-feeding was 4·4 (95 % range 0·5–12·0) months. In total, 65·7 % of all children were breast-fed partially until the age of 4 months, and 24·1 % of all children were breast-fed exclusively until the age of 4 months.
Table 1 Subject characteristics according to the duration of breast-feeding†
(Mean values, standard deviations, percentages or medians (90 % ranges) for variables with a skewed distribution, n 5074)

Differences in maternal and child characteristics for the breast-feeding duration groups were evaluated using ANOVA for continuous variables and χ2 tests for categorical variables: * P < 0·05, ** P < 0·01.
† Overweight is defined as BMI >25–29·9 kg/m2. Obesity is defined as BMI >30 kg/m2. Small-for-gestational age is defined as the lowest 5 % of gestational age-adjusted birth weight.
Table 2 shows the associations of breast-feeding, breast-feeding duration and exclusivity with postnatal growth rates (length, weight and BMI) in different time periods presented as changes in SDS. Breast-feeding duration and exclusivity were not associated with growth rates before the age of 3 months. Compared with children who were ever breast-fed, those who never breast-fed had a higher gain in length and weight between the age of 3 and 6 months (difference 0·07 (95 % CI 0·01, 0·14) SDS) and (0·06 (95 % CI 0·01, 0·12) SDS), respectively. Compared with children who were breast-fed for more than 3 months, children who were breast-fed shorter than 3 months also had a higher gain in length and weight between the ages of 3 and 6 months (all P for trend < 0·01). The highest gain in length was observed in children who were breast-fed for only 0–3 months. We observed similar tendencies for the associations between breast-feeding exclusivity and gain in length, weight and BMI between the age of 3 and 6 months. Children who were never breast-fed or breast-fed partially until 4 months showed a higher increase in length, weight and BMI. The highest effects were observed for children who were never breast-fed. Breast-feeding duration and exclusivity were not associated with growth between the age of 6 and 12 months.
Table 2 Breast-feeding duration and exclusivity and growth rates in different intervals during the first year of infancy†
(Regression coefficients and 95 % confidence intervals, n 5074)

SDS, standard deviation score; NA, not applicable.
Using multiple linear regression models: *P < 0·05, **P < 0·01.
† Models are adjusted for child's age at visit, sex, birth weight, gestational age, maternal ethnicity, maternal education, maternal BMI, smoking and parity. For the analyses focused on growth characteristics at the age of 0–3 months, we combined the breast-feeding duration groups into never and ever (0–3, 3–6 and >6 months). For the analyses focused on growth characteristics at the age of 3–6 months, we combined the breast-feeding duration groups into never, 0–3 months and 3–6 months (3–6 and >6 months).
Fig. 2 shows the results from the longitudinal generalised estimating equation models, which indicates no consistent associations between breast-feeding duration and exclusivity with the risks of overweight and obesity (BMI >1·1 SDS) at the ages of 1, 2 and 3 years. In addition, there was no consistent association between breast-feeding duration and exclusivity with BMI, overweight or obesity (see Table S1 of the supplementary material available at http://www.journals.cambridge.org/bjn).

Fig. 2 Breastfeeding and the risks of overweight and obesity in the first 3 years. (a) Breastfeeding duration. (b) Breastfeeding exclusivity. Values are OR with 95 % CI represented by horizontal bars. Breastfeeding duration for more than 6 months and breastfeeding exclusivity until 4 months, are considered as the reference groups in (a) and (b), respectively. Using generalised estimating equations: * P < 0·05, ** P < 0·01. Models are adjusted for child's age at visit, sex, birth weight, gestational age, maternal ethnicity, maternal education, maternal BMI, smoking and parity. Outcome is defined as age- and sex-adjusted BMI >1·1 standard deviation scores.
Discussion
Main findings
Breast-feeding duration and exclusivity were inversely associated with growth rates in length, weight and BMI between the ages of 3 and 6 months. We did not observe associations between breast-feeding duration and exclusivity and the risks of overweight and obese in the first 3 years of life.
Strengths and weaknesses
An important strength of the present study was the population-based cohort, with a large number of subjects being studied from early pregnancy onwards and information about a large number of potential confounders available. Information was available about duration and exclusivity of breast-feeding. Some methodological issues need to be considered. Of all children in the present study, questionnaires with breast-feeding information were available in 68 %. This non-response would lead to biased effect estimates if the associations of breast-feeding duration and exclusivity with postnatal growth characteristics would be different between those included and not included in the analyses. However, this seems unlikely because biased estimates in large cohort studies mainly arise from loss to follow-up rather than from non-response at baseline(Reference Nohr, Frydenberg and Henriksen21). In the present analysis, loss to follow-up was < 10 %. However, the number of follow-up measurements was smaller with increasing age. Information about breast-feeding was prospectively collected by questionnaires without direct reference to any growth characteristic. Although assessing breast-feeding by questionnaires seems to be a valid method, misclassification may occur(Reference Li, Scanlon and Serdula22, Reference Cupul-Uicab, Gladen and Hernández-Avila23). We estimated breast-feeding exclusivity according to whether the child received breast-feeding without any other infant formula, milk or solids according to the short FFQ. This definition does not cover the strict criteria used by the WHO, which suggest that even the use of water in combination with breast-feeding does not fulfil the definition of exclusivity. However, we did ask for the most commonly introduced solids and fluids. Furthermore, in The Netherlands, it is not common that children receive breast-feeding in combination with the use of water to prevent dehydration. Therefore, we think that our measurement of exclusive breast-feeding is a good proxy for exclusive breast-feeding according to the WHO criteria.
Finally, we used BMI for defining overweight and obesity in early childhood. We should be careful with these definitions, as at this young age there is no clear cut-off point to define obesity, and BMI cannot differentiate between fat and lean mass.
Comparison of main findings with other studies
In line with previous studies(Reference Hebebrand24–Reference Gillman26), we observed differences in maternal characteristics between breast-feeding duration groups. We previously showed socio-economic and ethnic differences in breast-feeding duration(Reference van Rossem, Vogel and Steegers27, Reference van Rossem, Oenema and Steegers28). In the present study group, mothers who never breast-fed their children were also more likely to have a younger age, higher BMI, Dutch or European background and were more likely to smoke during pregnancy. We additionally observed that children who were never breast-fed had a lower weight at birth and a higher risk of small size for gestational age and pre-term birth. The associations of maternal and birth characteristics with breast-feeding initiation and duration show that these characteristics should be considered as potential confounders when studying the associations between breast-feeding and childhood growth.
It has been shown that after the first week of life, growth patterns appear to be similar between breast-fed and formula-fed children for the first 2–3 months(Reference Nommsen-Rivers and Dewey29). However, thereafter, the growth rates between breast-fed and formula-fed children diverge with less distinct differences in length gain than in weight gain. Previous studies have suggested that breast-fed children have a slower growth between 3 and 12 months of life(Reference Victora, Morris and Barros30–Reference Michaelsen, Petersen and Greisen33). The present results are in line with the findings, but we showed that children who were never breast-fed have higher growth rates in length and weight only between the ages of 3 and 6 months. After the age of 6 months, it is very likely that complementary foods such as fruit and vegetable snacks are introduced. This may explain why we did not observe any effects in growth after the age of 6 months. We also showed that exclusive breast-feeding for 4 months was associated with a lower gain in length, weight and BMI during the first 3–6 months. This is in line with a previous study in randomly selected healthy newborns from Denmark and Iceland, which showed that exclusive breast-feeding influenced growth rates during infancy(Reference Michaelsen, Petersen and Greisen33). The authors suggested that exclusive breast-feeding until 2 months is related to lower weight gain from 2 to 6 months as well as from 6 to 12 months.
The biological mechanisms by which breast-feeding might protect against high growth rates are not well understood. One suggested mechanism is that high protein intake in formula-feeding stimulates the secretion of insulin-like growth factor I, which accelerates growth and increases muscle mass and adipose tissue(Reference Gunnarsdottir, Schack-Nielsen and Michaelsen34). Prolonged breast-feeding duration might also reduce plasma levels of appetite-related peptide and ghrelin(Reference Gunnarsdottir, Schack-Nielsen and Michaelsen34, Reference Michels, Willett and Graubard35). Furthermore, formula-fed infants have higher plasma insulin concentrations, which might result in increased insulin resistance(Reference Michels, Willett and Graubard35).
Studies that focused on the associations between breast-feeding and the risk of overweight and obesity in early childhood have shown inconsistent results(Reference Beyerlein, Fahrmeir and Mansmann9–Reference Agras, Kraemer and Berkowitz11). In the present study, breast-feeding duration and exclusivity were not consistently associated with the risk of overweight and obesity in the first 3 years of life. We observed that partial feeding until 4 months may increase the risk of overweight and obesity. However, this association was not consistent with the other results. We cannot explain this specific association, which might also be a chance finding.
Similar results in this age range have been observed in previous studies(Reference Fuiano, Rapa and Monzani36–Reference Owen, Martin and Whincup38). Furthermore, high postnatal growth rates in the first 6 months of life are independently associated with the risks of overweight and obesity in later life(Reference Ong, Ahmed and Emmett39). Therefore, the associations between shorter duration of breast-feeding and the risks of overweight and obesity might appear at older ages.
Conclusion
The present results suggest that shorter breast-feeding duration and exclusivity are associated with increased postnatal growth rates for height, weight and body mass in the first 3–6 months of life. Breast-feeding duration and exclusivity are not associated with the risks of overweight and obesity in the first 3 years. Further research is needed to assess whether and from which age breast-feeding duration and exclusiveness are associated with childhood obesity.
Acknowledgements
The Generation R Study is conducted by the Erasmus Medical Center in close collaboration with the School of Law and Faculty of Social Sciences of the Erasmus University Rotterdam, Rotterdam, The Netherlands; the Municipal Health Service Rotterdam area, Rotterdam, The Netherlands; the Rotterdam Homecare Foundation, Rotterdam, The Netherlands; the Stichting Trombosedienst and Artsenlaboratorium Rijnmond, Rotterdam, The Netherlands. We gratefully acknowledge the contribution of participating mothers, general practitioners, hospitals, midwives and pharmacies in Rotterdam. The first phase of the Generation R Study is made possible by financial support from the Erasmus Medical Center, Rotterdam, The Netherlands; the Erasmus University Rotterdam, Rotterdam, The Netherlands; the Netherlands Organization for Health Research, The Hague, The Netherlands. V. W. V. J. reports receipt of additional funding from the Netherlands Organization for Health Research and Development (ZonMw 90700303). The authors declare that there is no conflict of interest. The authors' contributions are as follows: B. D. and V. W. V. J. had a role in conception and design, performed the statistical analysis and wrote the manuscript. L. v. R., L. D., L. R. A., H. R., H. A. M., A. H. and E. A. P. S. provided comments and consultation regarding the analyses and the manuscript. All authors gave final approval of the version to be published.








