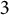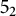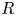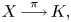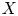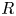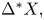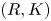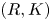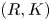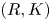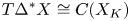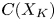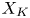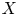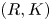622 results
14 - Intra-Abdominal Surgery
- from Section 3 - Practical Use
-
-
- Book:
- Hemodynamic Monitoring and Fluid Therapy during Surgery
- Published online:
- 11 April 2024
- Print publication:
- 02 May 2024, pp 149-167
-
- Chapter
- Export citation
Adjoint Reidemeister torsions of some 3-manifolds obtained by Dehn surgeries
- Part of
-
- Journal:
- Canadian Mathematical Bulletin , First View
- Published online by Cambridge University Press:
- 22 April 2024, pp. 1-15
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Aortic dilation in adults with repaired tetralogy of Fallot: a single-centre study
-
- Journal:
- Cardiology in the Young , First View
- Published online by Cambridge University Press:
- 27 February 2024, pp. 1-3
-
- Article
- Export citation
Acute Spontaneous Posterior Fossa Haemorrhage
-
- Published online:
- 15 February 2024
- Print publication:
- 29 February 2024
-
- Element
- Export citation
Comparison of electrically evoked stapedial reflexes in patients with cochlear implants surgically implanted using Veria and posterior tympanotomy approaches
-
- Journal:
- The Journal of Laryngology & Otology , First View
- Published online by Cambridge University Press:
- 05 February 2024, pp. 1-6
-
- Article
- Export citation
II.33 - John of Gaddesden, an Operation to Remove a Cataract, from Rosa Anglica
- from Fourteenth Century
-
- Book:
- The Cambridge Anthology of British Medieval Latin
- Published online:
- 11 January 2024
- Print publication:
- 01 February 2024, pp 304-308
-
- Chapter
- Export citation
Chapter 15 - The Changing Face of Traumatic Injury
- from Section 2 - Clinical Aspects of Traumatic Injuries, Epidemics, and Pandemics
-
-
- Book:
- Major Incidents, Pandemics and Mental Health
- Published online:
- 11 January 2024
- Print publication:
- 01 February 2024, pp 99-106
-
- Chapter
- Export citation
12 - “Dying Inside”: Obstacles to Treatment – and the Catastrophic Consequences
- from Part Three - The Prevention Problem
-
- Book:
- Enough
- Published online:
- 11 January 2024
- Print publication:
- 11 January 2024, pp 176-198
-
- Chapter
- Export citation
6 - The Toll of Treatment
- from Part Two - The Science behind Cervical Cancer
-
- Book:
- Enough
- Published online:
- 11 January 2024
- Print publication:
- 11 January 2024, pp 66-79
-
- Chapter
- Export citation
Chapter 37 - Postsurgical Nerve Entrapment
- from Part VI - Misc
-
-
- Book:
- Cambridge Handbook of Pain Medicine
- Published online:
- 01 December 2023
- Print publication:
- 14 December 2023, pp 303-307
-
- Chapter
- Export citation
Changes in audiovestibular handicap following treatment of vestibular schwannomas
-
- Journal:
- The Journal of Laryngology & Otology / Volume 138 / Issue 6 / June 2024
- Published online by Cambridge University Press:
- 29 November 2023, pp. 608-614
- Print publication:
- June 2024
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Barriers to Surgical Intervention and Factors Influencing Motor Outcomes in Patients with Severe Peripheral Nerve Injury: A Province Wide Cohort Study
-
- Journal:
- Canadian Journal of Neurological Sciences , First View
- Published online by Cambridge University Press:
- 23 November 2023, pp. 1-9
-
- Article
- Export citation
Applications of electrothermal bipolar vessel sealing devices in transoral head and neck surgery
-
- Journal:
- The Journal of Laryngology & Otology / Volume 138 / Issue 4 / April 2024
- Published online by Cambridge University Press:
- 09 October 2023, pp. 457-460
- Print publication:
- April 2024
-
- Article
- Export citation
Chapter 14 - Pregnancy Associated Breast Cancer
-
-
- Book:
- Gynaecology for the Obstetrician
- Published online:
- 14 July 2023
- Print publication:
- 03 August 2023, pp 146-158
-
- Chapter
- Export citation
P-wave asystole after a tetralogy of Fallot correction surgery
-
- Journal:
- Cardiology in the Young / Volume 33 / Issue 11 / November 2023
- Published online by Cambridge University Press:
- 26 July 2023, pp. 2449-2451
-
- Article
- Export citation
Correlation of narrow-band imaging findings using the Ni and European Laryngeal Society classification systems during in-office flexible laryngoscopy with histopathology
-
- Journal:
- The Journal of Laryngology & Otology / Volume 138 / Issue 2 / February 2024
- Published online by Cambridge University Press:
- 19 June 2023, pp. 203-207
- Print publication:
- February 2024
-
- Article
- Export citation
Pre-habilitation with intratympanic gentamicin in vestibular schwannomas: a systematic review
-
- Journal:
- The Journal of Laryngology & Otology / Volume 137 / Issue 9 / September 2023
- Published online by Cambridge University Press:
- 26 April 2023, pp. 985-991
- Print publication:
- September 2023
-
- Article
- Export citation
A geometric interpretation of Ranicki duality
-
- Journal:
- Proceedings of the Royal Society of Edinburgh. Section A: Mathematics , First View
- Published online by Cambridge University Press:
- 31 March 2023, pp. 1-18
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Legitimacy of Cost Concern for Health Insurance Coverage of Gender-Affirming Surgeries: Comparison of the Interest in Keeping Insurance Cost Down versus the Cost-Effectiveness of Including Gender-Affirming Surgeries in Employer Health Insurance Plans
-
- Journal:
- American Journal of Law & Medicine / Volume 49 / Issue 1 / March 2023
- Published online by Cambridge University Press:
- 28 June 2023, pp. 102-111
- Print publication:
- March 2023
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
9 - What to Do When Your Patient Fails Two Antiseizure Medicines
-
- Book:
- Seizure and Epilepsy Care
- Published online:
- 28 January 2023
- Print publication:
- 09 February 2023, pp 156-174
-
- Chapter
- Export citation