92 results
7 - The Postmodern Moment in Gender Studies and Anthropology
- from Part Two - Knowledges and Domains
-
-
- Book:
- The Cambridge Handbook for the Anthropology of Gender and Sexuality
- Published online:
- 29 September 2023
- Print publication:
- 19 October 2023, pp 184-212
-
- Chapter
- Export citation
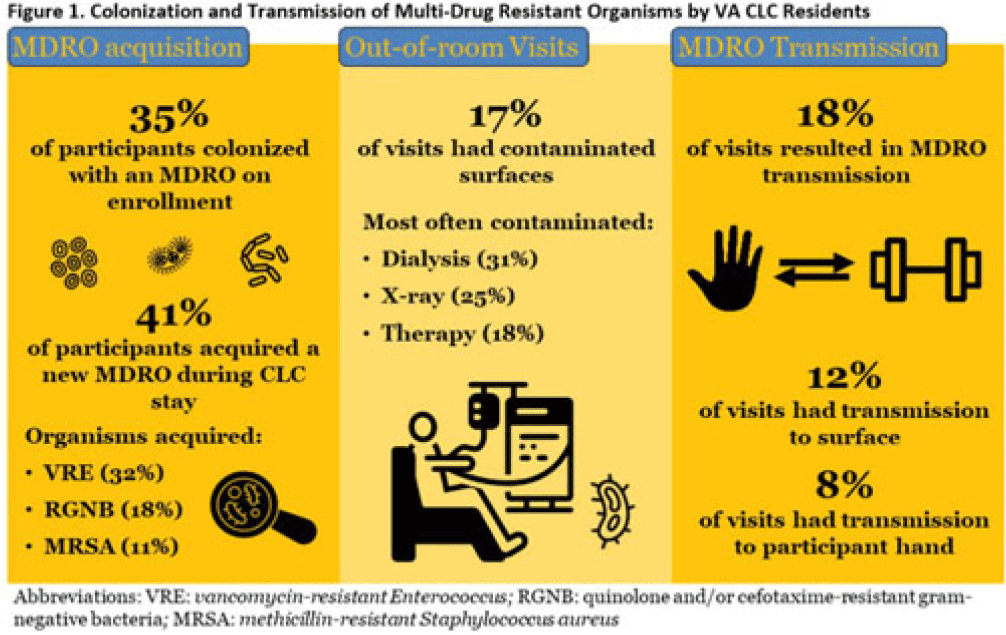
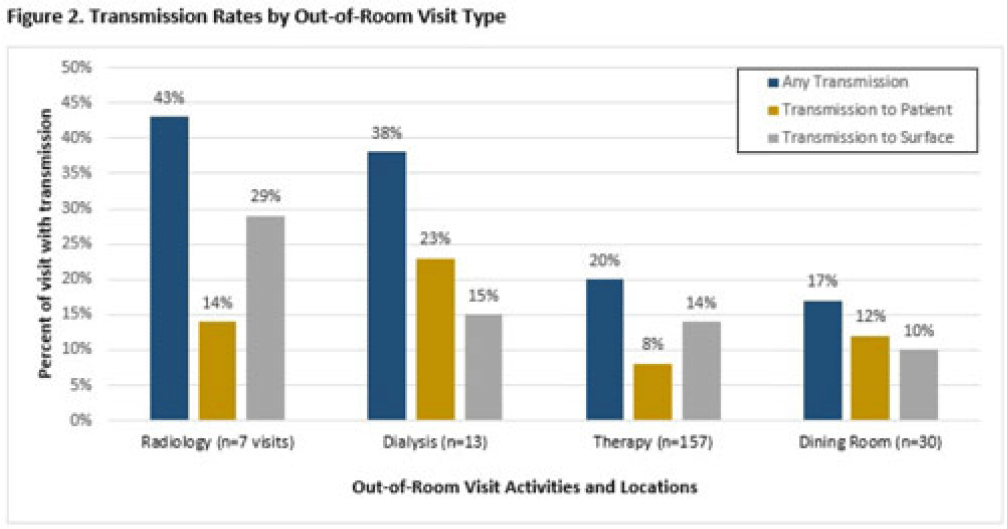
Transmission of multidrug-resistant organisms by VA CLC residents: A multisite prospective study
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s116-s117
-
- Article
-
- You have access
- Open access
- Export citation
What US hospitals are doing to prevent common device-associated infections during the coronavirus disease 2019 (COVID-19) pandemic: Results from a national survey in the United States
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 12 / December 2023
- Published online by Cambridge University Press:
- 01 June 2023, pp. 1913-1919
- Print publication:
- December 2023
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Developing relevant assessments of community-engaged research partnerships: A community-based participatory approach to evaluating clinical and health research study teams
-
- Journal:
- Journal of Clinical and Translational Science / Volume 7 / Issue 1 / 2023
- Published online by Cambridge University Press:
- 11 May 2023, e123
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Acknowledgements
-
- Book:
- Sexual Restraint and Aesthetic Experience in Victorian Literary Decadence
- Published online:
- 02 March 2023
- Print publication:
- 09 March 2023, pp vi-viii
-
- Chapter
- Export citation
3 - ‘A Holy Indifference and Tolerant Favour’
-
- Book:
- Sexual Restraint and Aesthetic Experience in Victorian Literary Decadence
- Published online:
- 02 March 2023
- Print publication:
- 09 March 2023, pp 114-144
-
- Chapter
- Export citation
Contents
-
- Book:
- Sexual Restraint and Aesthetic Experience in Victorian Literary Decadence
- Published online:
- 02 March 2023
- Print publication:
- 09 March 2023, pp v-v
-
- Chapter
- Export citation
2 - ‘A Passionate Coldness’
-
- Book:
- Sexual Restraint and Aesthetic Experience in Victorian Literary Decadence
- Published online:
- 02 March 2023
- Print publication:
- 09 March 2023, pp 76-113
-
- Chapter
- Export citation
Bibliography
-
- Book:
- Sexual Restraint and Aesthetic Experience in Victorian Literary Decadence
- Published online:
- 02 March 2023
- Print publication:
- 09 March 2023, pp 241-258
-
- Chapter
- Export citation
Copyright page
-
- Book:
- Sexual Restraint and Aesthetic Experience in Victorian Literary Decadence
- Published online:
- 02 March 2023
- Print publication:
- 09 March 2023, pp iv-iv
-
- Chapter
- Export citation
Conclusion
-
- Book:
- Sexual Restraint and Aesthetic Experience in Victorian Literary Decadence
- Published online:
- 02 March 2023
- Print publication:
- 09 March 2023, pp 203-207
-
- Chapter
- Export citation
5 - ‘Men Have Died of Love’
-
- Book:
- Sexual Restraint and Aesthetic Experience in Victorian Literary Decadence
- Published online:
- 02 March 2023
- Print publication:
- 09 March 2023, pp 175-202
-
- Chapter
- Export citation
Notes
-
- Book:
- Sexual Restraint and Aesthetic Experience in Victorian Literary Decadence
- Published online:
- 02 March 2023
- Print publication:
- 09 March 2023, pp 208-240
-
- Chapter
- Export citation
4 - ‘An Ascetic Epicureanism’
-
- Book:
- Sexual Restraint and Aesthetic Experience in Victorian Literary Decadence
- Published online:
- 02 March 2023
- Print publication:
- 09 March 2023, pp 145-174
-
- Chapter
- Export citation
Introduction
-
- Book:
- Sexual Restraint and Aesthetic Experience in Victorian Literary Decadence
- Published online:
- 02 March 2023
- Print publication:
- 09 March 2023, pp 1-31
-
- Chapter
- Export citation
Index
-
- Book:
- Sexual Restraint and Aesthetic Experience in Victorian Literary Decadence
- Published online:
- 02 March 2023
- Print publication:
- 09 March 2023, pp 259-266
-
- Chapter
- Export citation
1 - Loss and Gain
-
- Book:
- Sexual Restraint and Aesthetic Experience in Victorian Literary Decadence
- Published online:
- 02 March 2023
- Print publication:
- 09 March 2023, pp 32-75
-
- Chapter
- Export citation

Sexual Restraint and Aesthetic Experience in Victorian Literary Decadence
-
- Published online:
- 02 March 2023
- Print publication:
- 09 March 2023
The Province and Politics of the Economic Torts. By John Murphy. [London: Hart Publishing, 2022. xxx + 287 pp. Hardback £85.00. ISBN 978-1-50992-731-9.]
-
- Journal:
- The Cambridge Law Journal / Volume 82 / Issue 1 / March 2023
- Published online by Cambridge University Press:
- 26 April 2023, pp. 171-173
- Print publication:
- March 2023
-
- Article
- Export citation
Development and validation of the ASKFV-SE tool to measure children's self-efficacy for requesting fruits and vegetables
-
- Journal:
- Journal of Nutritional Science / Volume 12 / 2023
- Published online by Cambridge University Press:
- 06 January 2023, e3
-
- Article
-
- You have access
- Open access
- HTML
- Export citation