133 results
“They say I’m crazy, but I’ve lived through hell.”
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S524
-
- Article
-
- You have access
- Open access
- Export citation
Differential attrition in randomized controlled trials of digital mental health interventions in the workplace: A systematic review and meta-analysis (EMPOWER H2020 project)
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S151-S152
-
- Article
-
- You have access
- Open access
- Export citation
Association between loneliness in childhood and first-episode psychosis
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S88-S89
-
- Article
-
- You have access
- Open access
- Export citation
Change of measure in a Heston–Hawkes stochastic volatility model
- Part of
-
- Journal:
- Advances in Applied Probability , First View
- Published online by Cambridge University Press:
- 24 July 2024, pp. 1-30
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Treatment Interruptions and Mortality Among Puerto Rican Women With Gynecologic Cancers in Puerto Rico After Hurricanes Irma and María: A Retrospective Cohort Study
-
- Journal:
- Disaster Medicine and Public Health Preparedness / Volume 18 / 2024
- Published online by Cambridge University Press:
- 21 May 2024, e105
-
- Article
- Export citation
88 Feasibility of a Home-based Physiotherapy Program to Increase Physical Activity Levels in Older Adults with Diabetes Mellitus
- Part of
-
- Journal:
- Journal of Clinical and Translational Science / Volume 8 / Issue s1 / April 2024
- Published online by Cambridge University Press:
- 03 April 2024, p. 23
-
- Article
-
- You have access
- Open access
- Export citation
2 Cognitive Heterogeneity and Risk of Progression in Data-Driven Subtle Cognitive Decline Phenotypes
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 103-104
-
- Article
-
- You have access
- Export citation
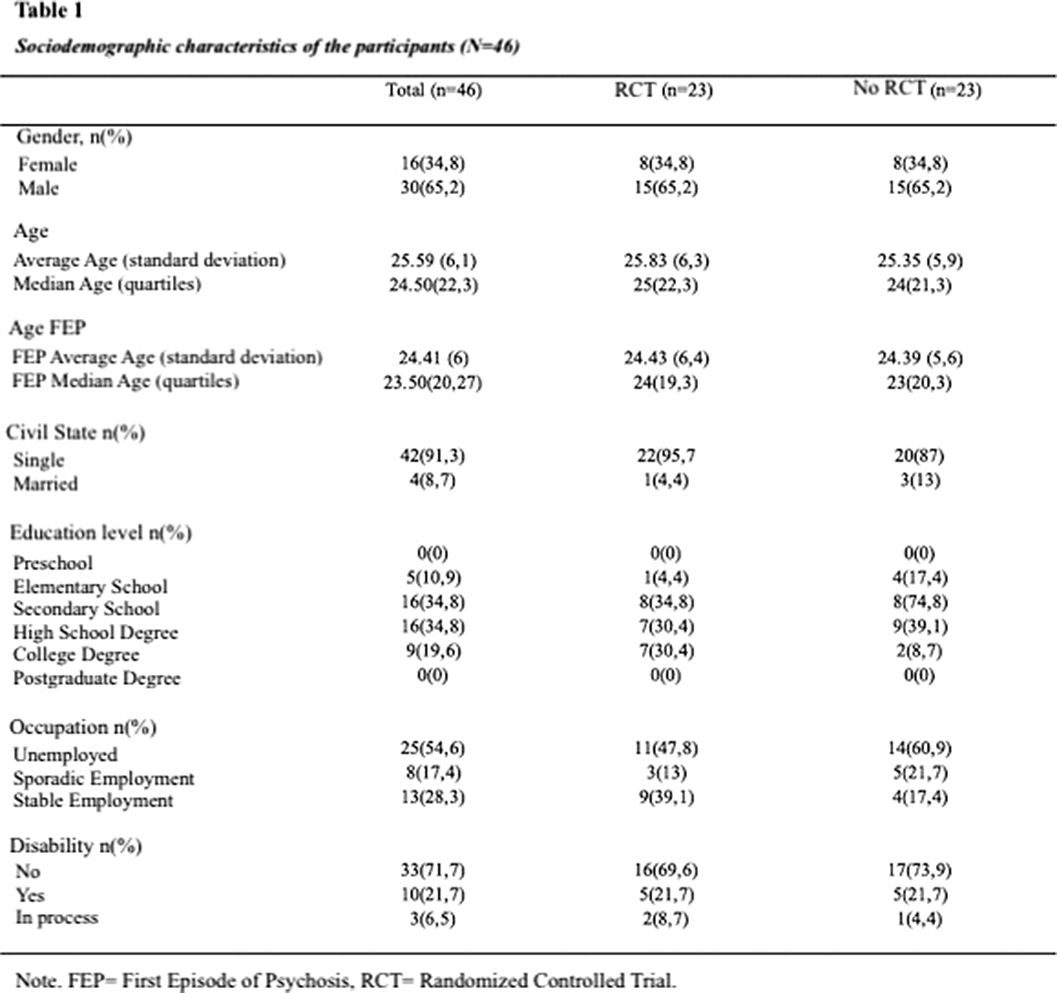
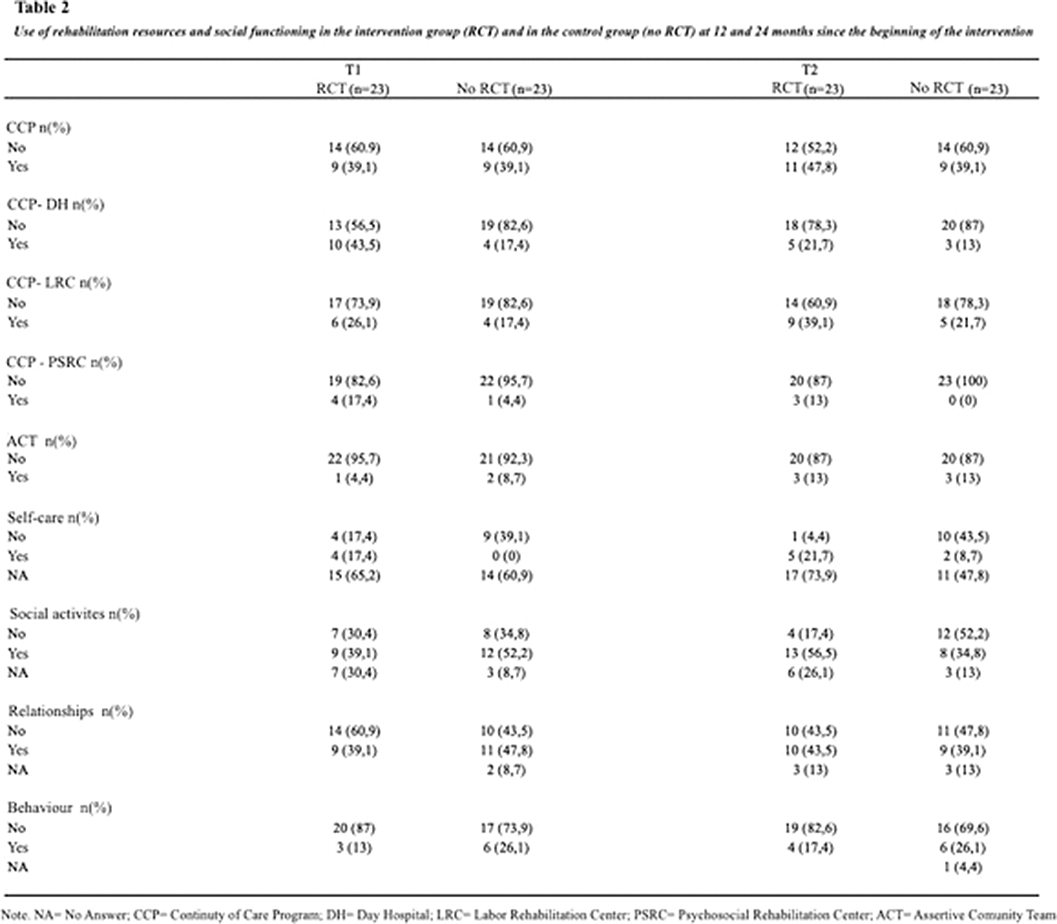
Group psychotherapy for patients with first-episode psychosis: Effect on the clinical status and use of resources
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S635-S636
-
- Article
-
- You have access
- Open access
- Export citation
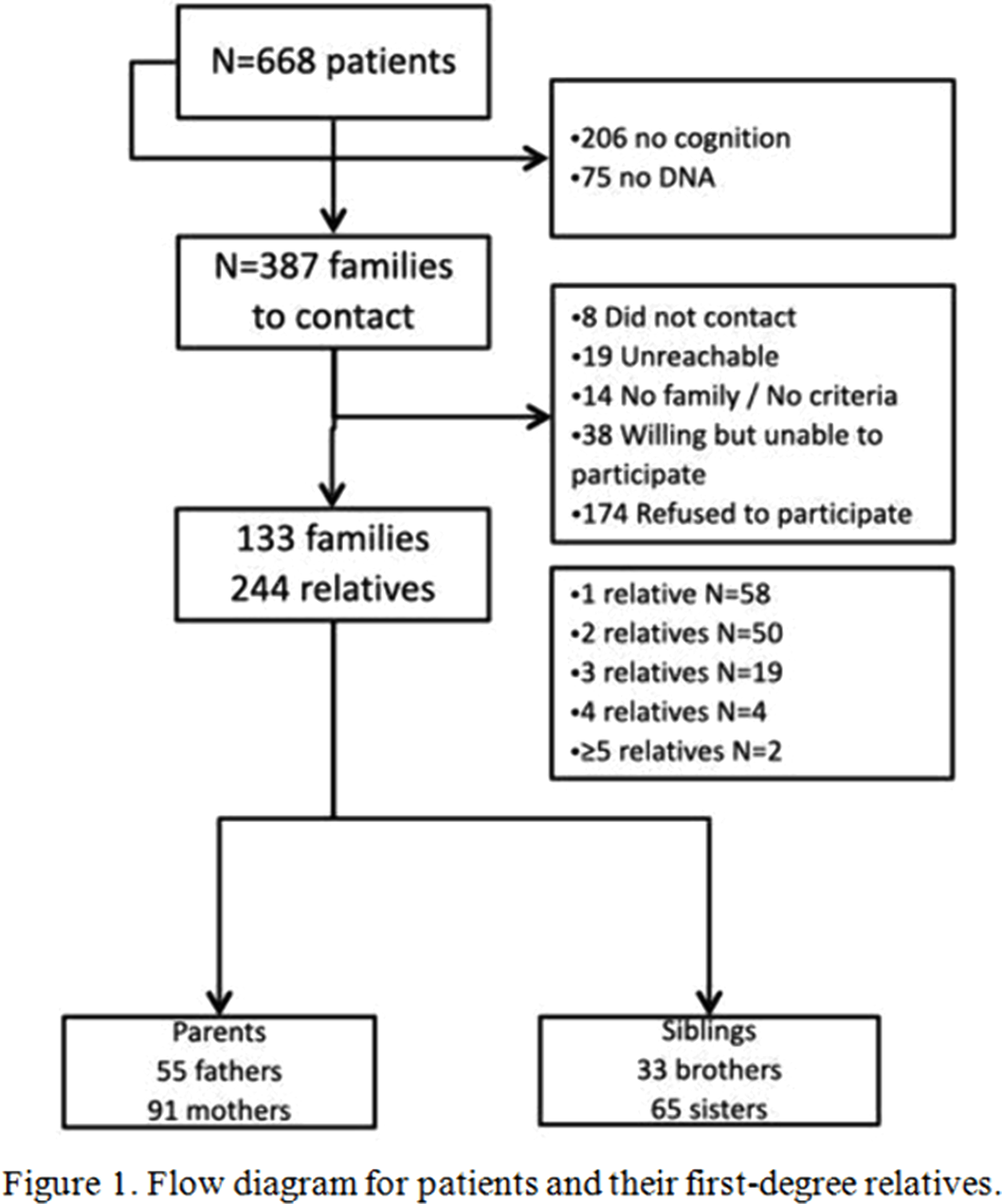
The use of Polygenic Scores in a family design of First Episode Psychosis
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S631
-
- Article
-
- You have access
- Open access
- Export citation
AGESMind clinical trial: SocialMIND® results at 16 weeks
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S480-S481
-
- Article
-
- You have access
- Open access
- Export citation
“Social functioning and use of rehabilitation resources in a group of people who experienced a first episode of psychosis and participated in a psychotherapeutic group program versus a control group”
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S185
-
- Article
-
- You have access
- Open access
- Export citation
Intelligence Quotient changes over 10 years: diversity of cognitive profiles in first episode of psychosis and healthy controls
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S630
-
- Article
-
- You have access
- Open access
- Export citation
Efficacy and safety of a 4-week course of repeated subcutaneous ketamine injections for treatment-resistant depression (KADS study): randomised double-blind active-controlled trial
-
- Journal:
- The British Journal of Psychiatry / Volume 223 / Issue 6 / December 2023
- Published online by Cambridge University Press:
- 14 July 2023, pp. 533-541
- Print publication:
- December 2023
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
108 Pilot Project Awardees Productivity Award Metrics at The Alliance Idea-CTR
- Part of
-
- Journal:
- Journal of Clinical and Translational Science / Volume 7 / Issue s1 / April 2023
- Published online by Cambridge University Press:
- 24 April 2023, pp. 31-32
-
- Article
-
- You have access
- Open access
- Export citation
312 Metabolomics Approach to Cellular Senescence: Characterizing the Secretory Phenotype and Metabolism of Irradiation-Induced Senescent Human Pre- Adipocytes
- Part of
-
- Journal:
- Journal of Clinical and Translational Science / Volume 7 / Issue s1 / April 2023
- Published online by Cambridge University Press:
- 24 April 2023, p. 94
-
- Article
-
- You have access
- Open access
- Export citation
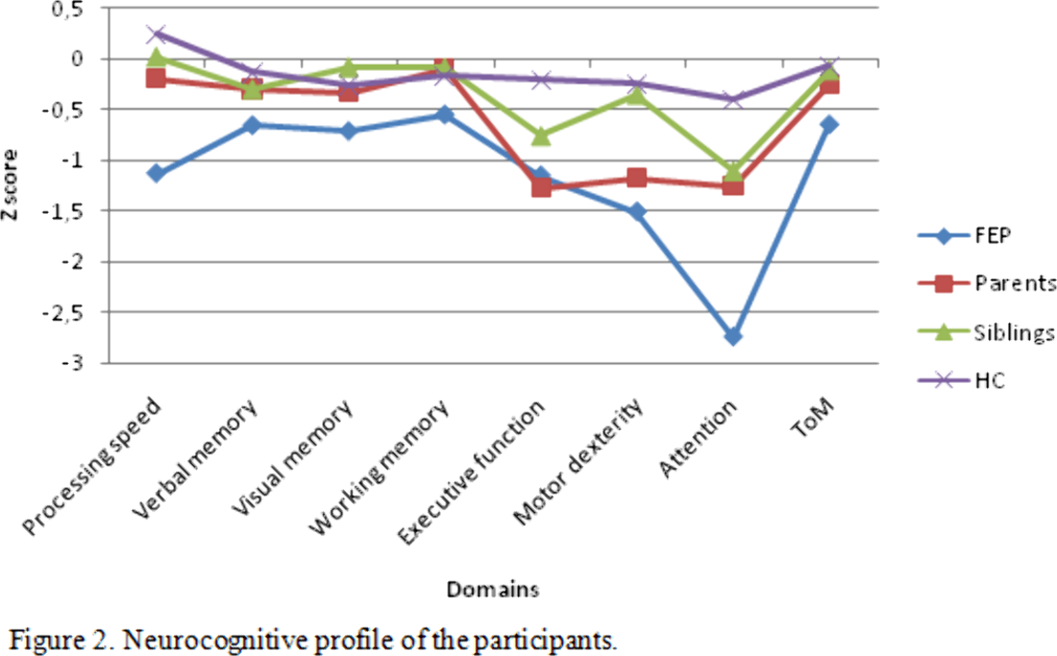
A family study on first episode of psychosis patients: exploring neuropsychological performance as an endophenotype
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S108-S109
-
- Article
-
- You have access
- Open access
- Export citation
Mental health service requirements after hospitalization due to COVID-19: a 1- year follow-up study
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S381
-
- Article
-
- You have access
- Open access
- Export citation
Disentangling early and late onset of psychosis in women
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S356
-
- Article
-
- You have access
- Open access
- Export citation
Paralization and online adaptation of an ongoing clinical trial in La Paz University Hospital (Madrid, Spain) during the COVID-19 worldwide pandemic
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S617-S618
-
- Article
-
- You have access
- Open access
- Export citation
Pattern of long-term weight and metabolic changes after a first episode of psychosis: Results from a 10-year prospective follow-up of the PAFIP program for early intervention in psychosis cohort
-
- Journal:
- European Psychiatry / Volume 65 / Issue 1 / 2022
- Published online by Cambridge University Press:
- 16 August 2022, e48
-
- Article
-
- You have access
- Open access
- HTML
- Export citation