284 results
Modern arable and diverse ley farming systems can increase soil organic matter faster than global targets
-
- Journal:
- Renewable Agriculture and Food Systems / Volume 39 / 2024
- Published online by Cambridge University Press:
- 18 September 2024, e17
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Survey of VA Laboratory Practices for Carbapenem-resistant Acinetobacter baumannii and Pseudomonas aeruginosa
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s79
-
- Article
-
- You have access
- Open access
- Export citation
Effect of behavioural activation for individuals with post-stroke depression: systematic review and meta-analysis
-
- Journal:
- BJPsych Open / Volume 10 / Issue 5 / September 2024
- Published online by Cambridge University Press:
- 30 July 2024, e134
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Development and implementation of a nationwide multidrug-resistant organism tracking and alert system for Veterans Affairs medical centers
-
- Journal:
- Infection Control & Hospital Epidemiology , First View
- Published online by Cambridge University Press:
- 24 May 2024, pp. 1-6
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
How to co-create content moderation policies: the case of the AutSPACEs project
-
- Journal:
- Data & Policy / Volume 6 / 2024
- Published online by Cambridge University Press:
- 15 May 2024, e28
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Facility- and patient-level factors associated with implementation of contact precautions in hospitalized VA patients with positive CRE cultures
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue 1 / 2024
- Published online by Cambridge University Press:
- 03 May 2024, e76
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
251 The Appalachian Translational Research Network (ATRN) Newsletter: Supporting Communication and Collaboration among Academic and Community Partners to Improve Health in Appalachia
- Part of
-
- Journal:
- Journal of Clinical and Translational Science / Volume 8 / Issue s1 / April 2024
- Published online by Cambridge University Press:
- 03 April 2024, pp. 75-76
-
- Article
-
- You have access
- Open access
- Export citation
Using latent class analysis to investigate enduring effects of intersectional social disadvantage on long-term vocational and financial outcomes in the 20-year prospective Chicago Longitudinal Study
-
- Journal:
- Psychological Medicine , First View
- Published online by Cambridge University Press:
- 25 March 2024, pp. 1-13
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Near-source passive sampling for monitoring viral outbreaks within a university residential setting
-
- Journal:
- Epidemiology & Infection / Volume 152 / 2024
- Published online by Cambridge University Press:
- 08 February 2024, e31
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
P114: Experiences of nursing home residents with dementia and chronic pain using an interactive social robot: A qualitative study of multiple stakeholders
-
- Journal:
- International Psychogeriatrics / Volume 35 / Issue S1 / December 2023
- Published online by Cambridge University Press:
- 02 February 2024, pp. 171-172
-
- Article
-
- You have access
- Export citation
Parliamentary reaction to the announcement and implementation of the UK Soft Drinks Industry Levy: applied thematic analysis of 2016–2020 parliamentary debates
-
- Journal:
- Public Health Nutrition / Volume 27 / Issue 1 / 2024
- Published online by Cambridge University Press:
- 24 January 2024, e51
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Reductive Degradation of p,p′-DDT cy Fe(II) in Nontronite NAu-2
-
- Journal:
- Clays and Clay Minerals / Volume 58 / Issue 6 / December 2010
- Published online by Cambridge University Press:
- 01 January 2024, pp. 821-836
-
- Article
- Export citation
Treatment effectiveness of antibiotic therapy in Veterans with multidrug-resistant Acinetobacter spp. bacteremia
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue 1 / 2023
- Published online by Cambridge University Press:
- 12 December 2023, e230
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Population monitoring of a Critically Endangered antelope, the mountain bongo, using camera traps and a novel identification scheme
-
- Journal:
- Oryx , First View
- Published online by Cambridge University Press:
- 13 November 2023, pp. 1-8
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
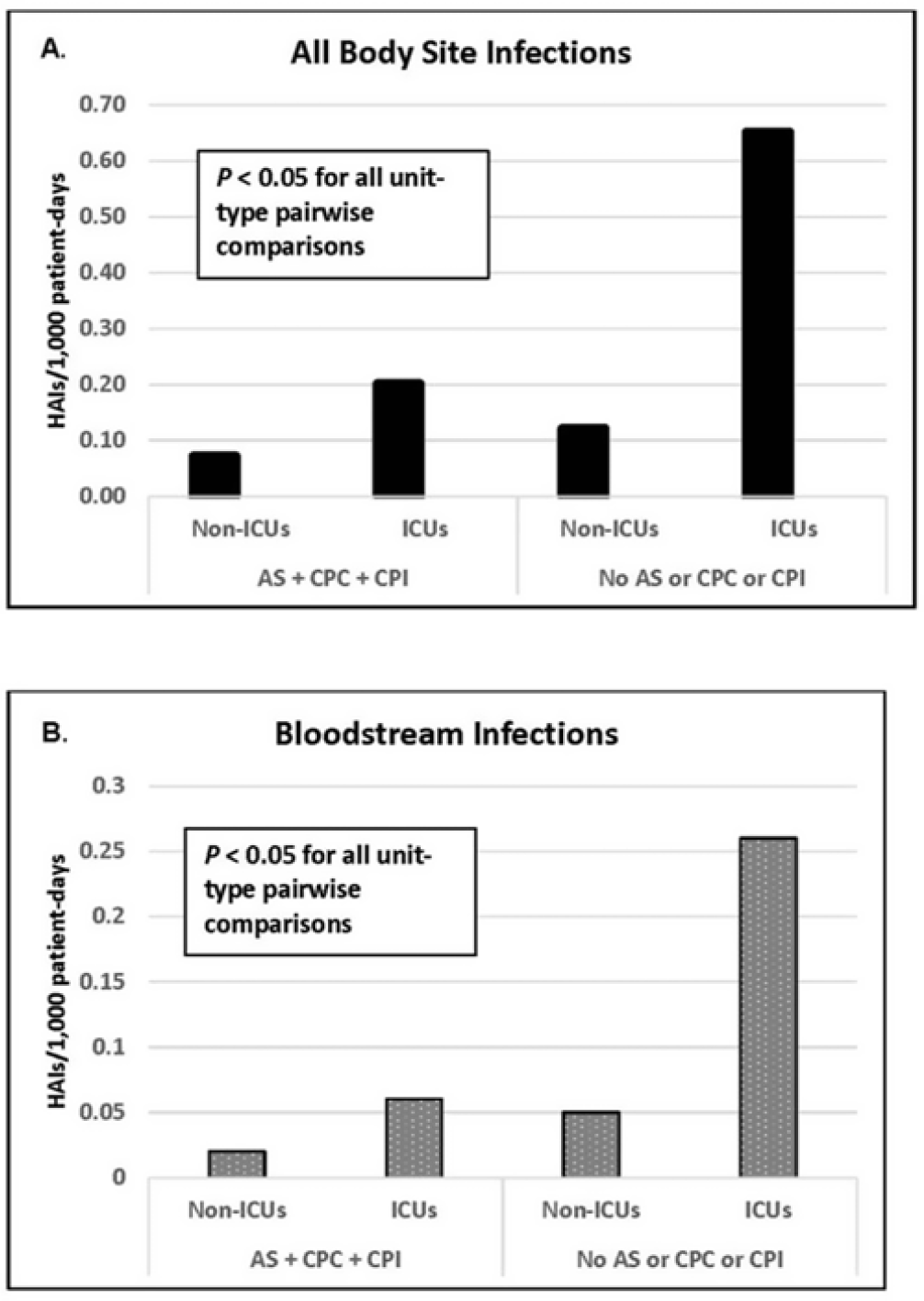
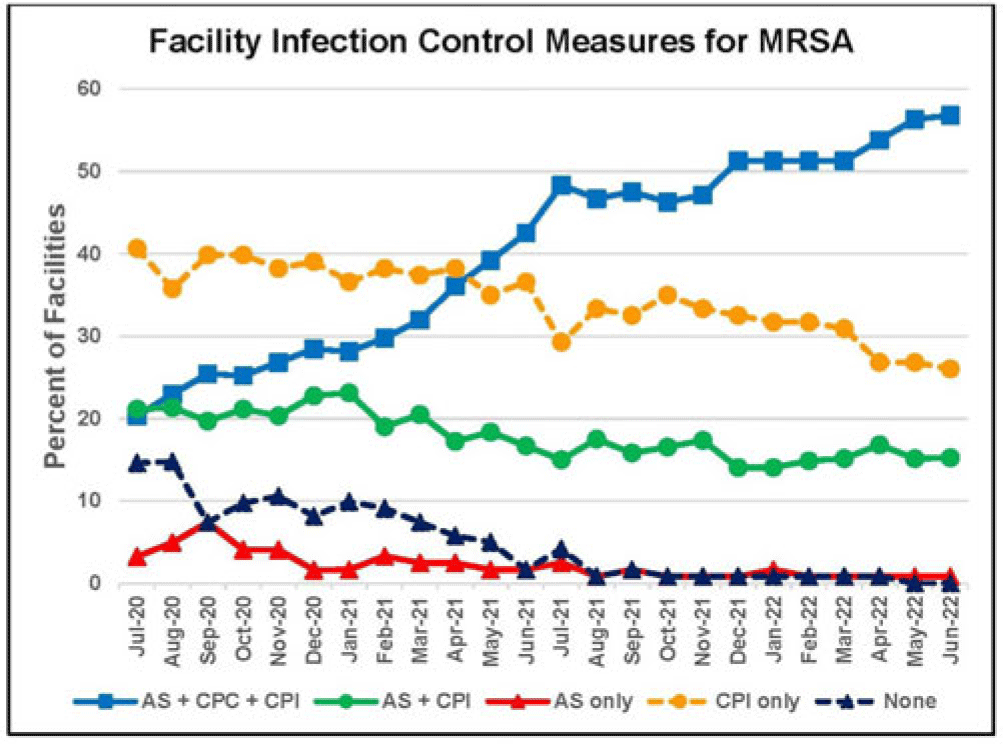
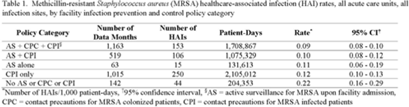
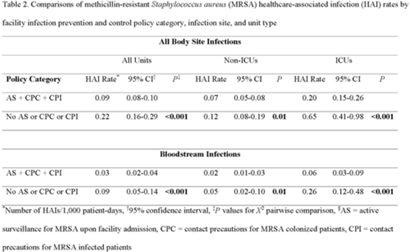
Active surveillance and contact precautions for preventing MRSA healthcare-associated infections during the COVID-19 pandemic
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s117-s118
-
- Article
-
- You have access
- Open access
- Export citation
Increasing Registration for a VA Multidrug-Resistant Organism Alert Tool
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s124-s125
-
- Article
-
- You have access
- Open access
- Export citation
A multi-country comparison of jurisdictions with and without mandatory nutrition labelling policies in restaurants: analysis of behaviours associated with menu labelling in the 2019 International Food Policy Study
- Part of
-
- Journal:
- Public Health Nutrition / Volume 26 / Issue 11 / November 2023
- Published online by Cambridge University Press:
- 04 September 2023, pp. 2595-2606
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
CosmoDRAGoN simulations—I. Dynamics and observable signatures of radio jets in cosmological environments
-
- Journal:
- Publications of the Astronomical Society of Australia / Volume 40 / 2023
- Published online by Cambridge University Press:
- 12 April 2023, e014
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Extraction and applications of Rayleigh wave ellipticity in polar regions
-
- Journal:
- Annals of Glaciology / Volume 63 / Issue 87-89 / September 2022
- Published online by Cambridge University Press:
- 29 March 2023, pp. 3-7
-
- Article
-
- You have access
- Open access
- HTML
- Export citation