12 results
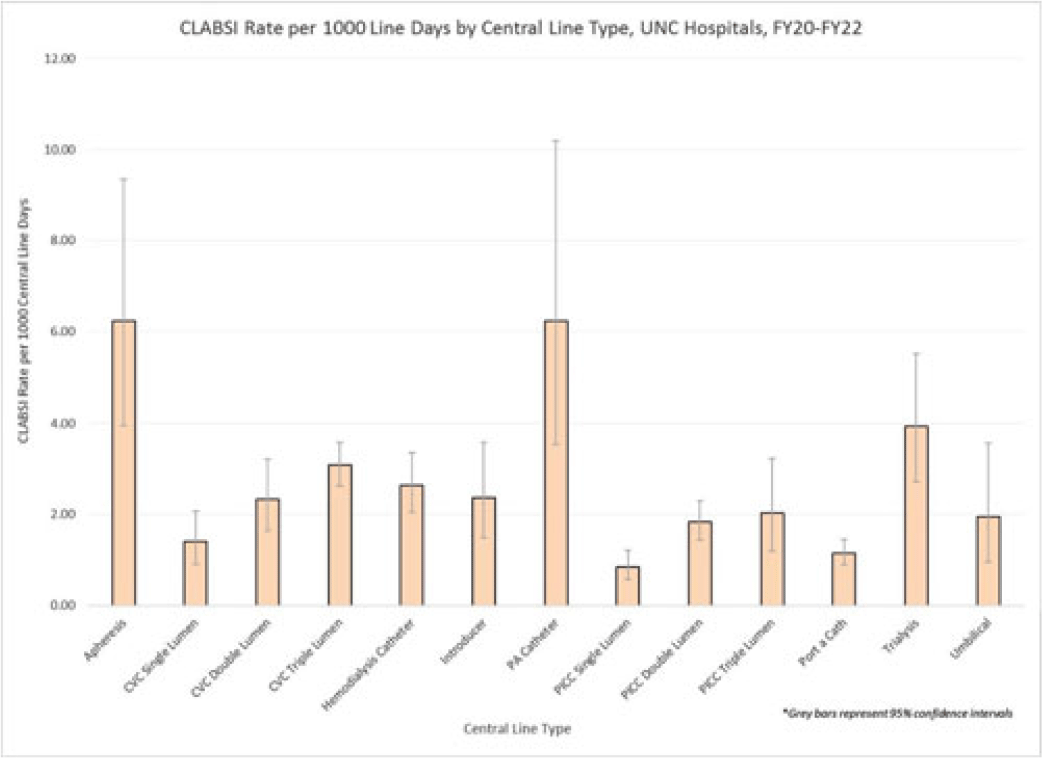
Examining CLABSI rates by central-line type
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s48-s49
-
- Article
-
- You have access
- Open access
- Export citation
A new paradigm for infection prevention programs: An integrated approach
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 1 / January 2023
- Published online by Cambridge University Press:
- 14 July 2022, pp. 144-147
- Print publication:
- January 2023
-
- Article
-
- You have access
- HTML
- Export citation
Creation and impact of containment units with high-risk zones during the coronavirus disease 2019 (COVID-19) pandemic
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 6 / June 2023
- Published online by Cambridge University Press:
- 17 June 2022, pp. 908-914
- Print publication:
- June 2023
-
- Article
- Export citation
Characterization of healthcare-associated infections with the severe acute respiratory coronavirus virus 2 (SARS-CoV-2) omicron variant at a tertiary healthcare center
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 1 / January 2023
- Published online by Cambridge University Press:
- 26 May 2022, pp. 133-135
- Print publication:
- January 2023
-
- Article
- Export citation
Building a PPE Monitor Team as Part of a Comprehensive COVID-19 Prevention Strategy
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue S1 / July 2021
- Published online by Cambridge University Press:
- 29 July 2021, p. s47
-
- Article
-
- You have access
- Open access
- Export citation
Successfully Sustaining Infection Reductions: A Catheter–Associated Urinary Tract Infection (CAUTI) Prevention Initiative Five Years In
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, p. s395
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
The little things matter—How peer audits contribute to CLABSI prevention
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue 2 / February 2020
- Published online by Cambridge University Press:
- 16 December 2019, pp. 246-248
- Print publication:
- February 2020
-
- Article
- Export citation
The holy grail of hand hygiene compliance: Just-in-time peer coaching that leads to behavior change
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue 2 / February 2020
- Published online by Cambridge University Press:
- 13 December 2019, pp. 229-232
- Print publication:
- February 2020
-
- Article
- Export citation
ten - Combating malnutrition in hospitals
-
-
- Book:
- The New Dynamics of Ageing Volume 2
- Published by:
- Bristol University Press
- Published online:
- 13 April 2022
- Print publication:
- 25 July 2018, pp 177-196
-
- Chapter
- Export citation
Assessment of Self-Contamination During Removal of Personal Protective Equipment for Ebola Patient Care
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 37 / Issue 10 / October 2016
- Published online by Cambridge University Press:
- 01 August 2016, pp. 1156-1161
- Print publication:
- October 2016
-
- Article
- Export citation
Invasive Cutaneous Rhizopus Infections in an Immunocompromised Patient Population Associated with Hospital Laundry Carts
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 37 / Issue 10 / October 2016
- Published online by Cambridge University Press:
- 26 July 2016, pp. 1251-1253
- Print publication:
- October 2016
-
- Article
- Export citation
Longitudinal Trends in All Healthcare-Associated Infections through Comprehensive Hospital-wide Surveillance and Infection Control Measures over the Past 12 Years: Substantial Burden of Healthcare-Associated Infections Outside of Intensive Care Units and “Other” Types of Infection
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 36 / Issue 10 / October 2015
- Published online by Cambridge University Press:
- 25 June 2015, pp. 1139-1147
- Print publication:
- October 2015
-
- Article
- Export citation