17 results
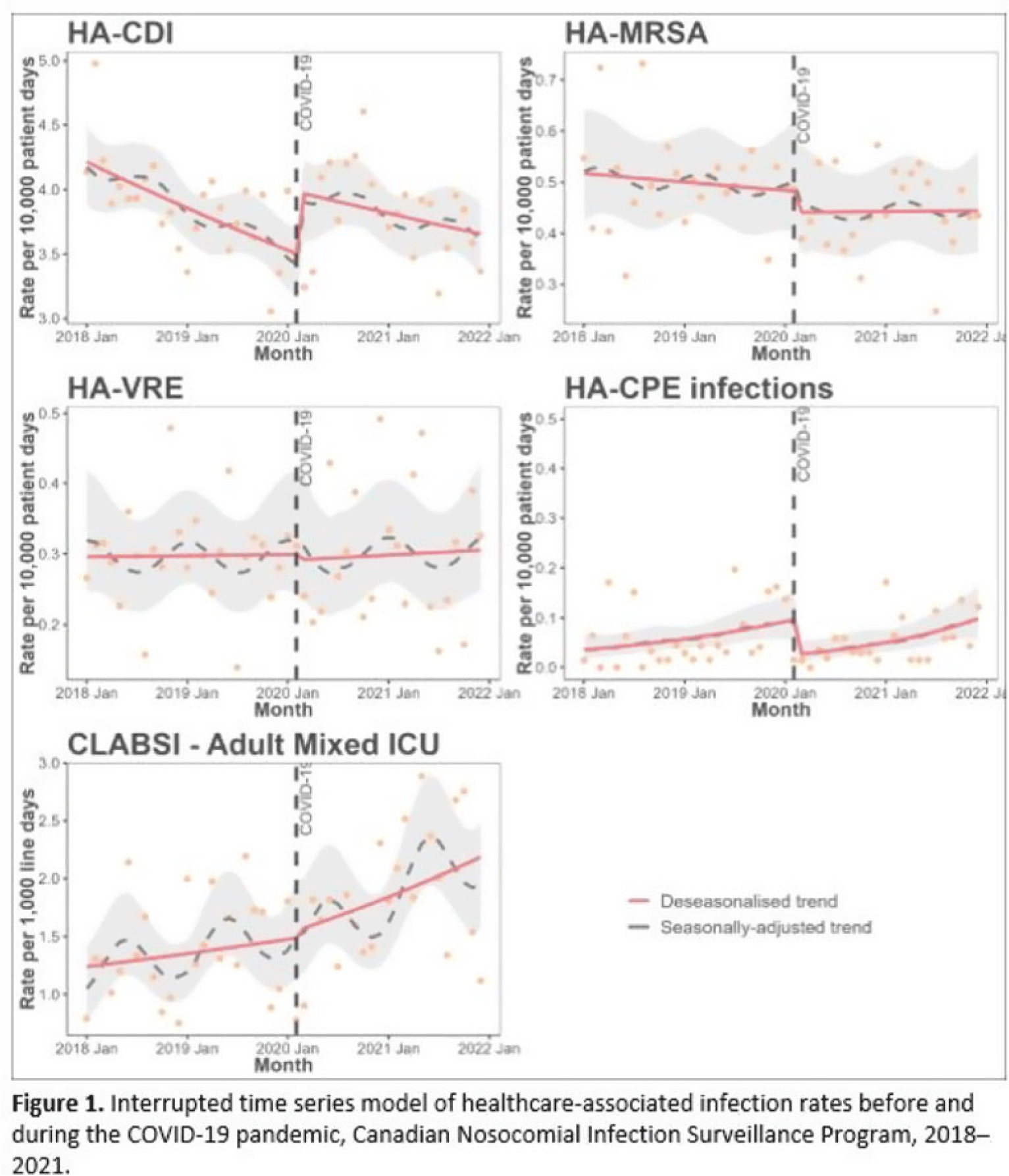
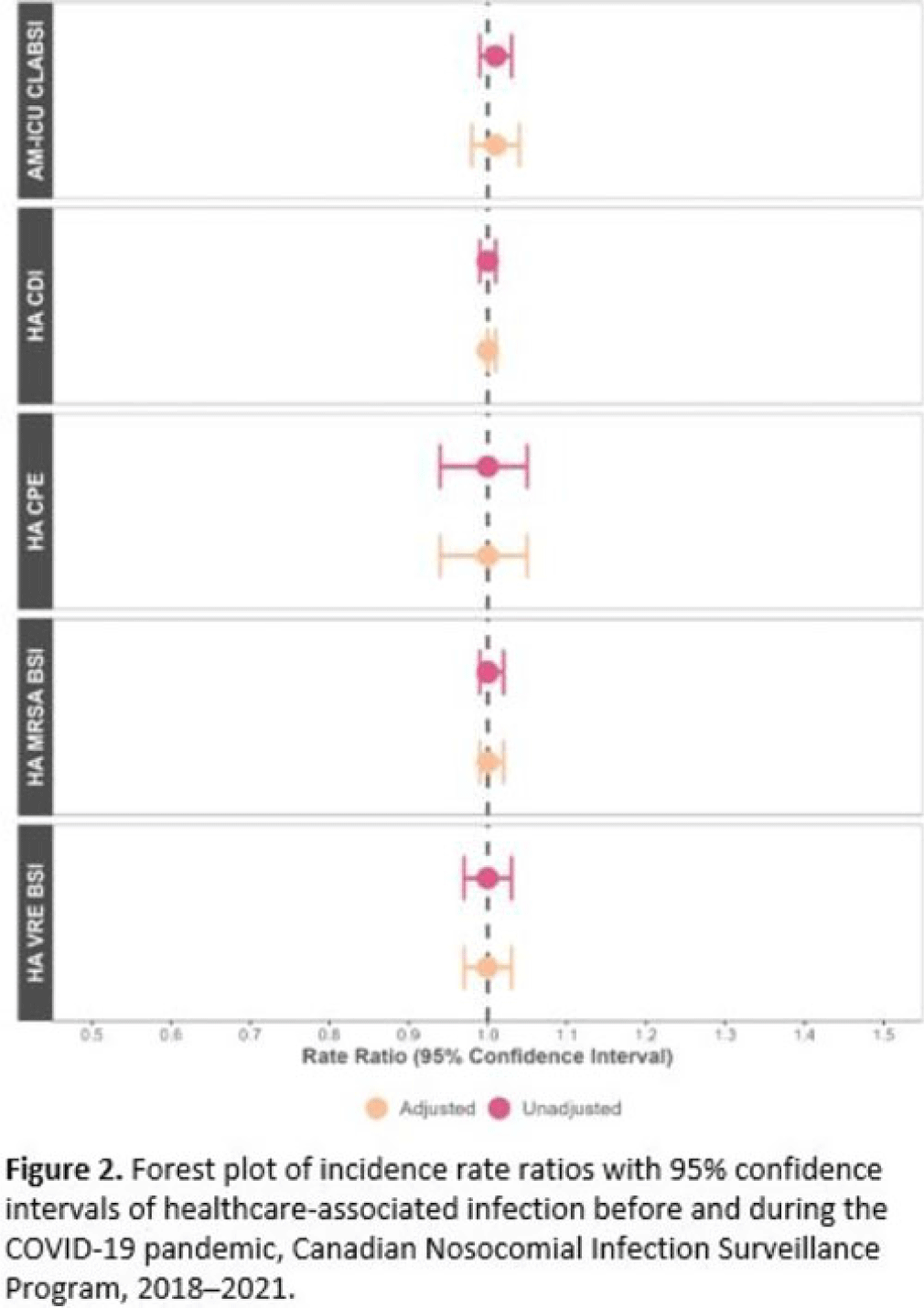
Impact of COVID-19 on healthcare-associated infections in Canadian acute-care hospitals: Interrupted time series (2018–2021)
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s112-s113
-
- Article
-
- You have access
- Open access
- Export citation
Antibiotic Selection and Duration for Catheter-Associated Urinary Tract Infection in Non-Hospitalized Older Adults: A Population-Based Cohort Study
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue 1 / 2023
- Published online by Cambridge University Press:
- 01 August 2023, e132
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Coronavirus disease 2019 (COVID-19) outbreak on an in-patient medical unit associated with unrecognized exposures in common areas—Epidemiological and whole-genome sequencing investigation
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 11 / November 2023
- Published online by Cambridge University Press:
- 13 March 2023, pp. 1829-1833
- Print publication:
- November 2023
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Trends in Clostridioides difficile infection rates in Canadian hospitals during the coronavirus disease 2019 (COVID-19) pandemic
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 7 / July 2023
- Published online by Cambridge University Press:
- 18 August 2022, pp. 1180-1183
- Print publication:
- July 2023
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Validation and implementation of group electronic hand hygiene monitoring across twenty-four critical care units
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 43 / Issue 7 / July 2022
- Published online by Cambridge University Press:
- 25 June 2021, pp. 834-839
- Print publication:
- July 2022
-
- Article
- Export citation
Low yield of severe acute respiratory coronavirus virus 2 (SARS-CoV-2) asymptomatic routine screen testing, despite high community incidence
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 43 / Issue 10 / October 2022
- Published online by Cambridge University Press:
- 24 June 2021, pp. 1527-1528
- Print publication:
- October 2022
-
- Article
-
- You have access
- HTML
- Export citation
Dealing with coronavirus disease 2019 (COVID-19) outbreaks in long-term care homes: A protocol for room moving and cohorting
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 42 / Issue 11 / November 2021
- Published online by Cambridge University Press:
- 28 October 2020, pp. 1402-1403
- Print publication:
- November 2021
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Infection Prevention and Control for 2019 Novel Coronavirus (2019 nCoV) in Acute Healthcare Settings: The Canadian Response
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s17-s18
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Epidemiological and Molecular Characterization of Clostridioides difficile Infection in Canadian Outpatient Settings, 2015–2019
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s472-s473
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Interfacility patient sharing and Clostridioides difficile infection incidence in the Ontario hospital system: A 13-year cohort study
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue 2 / February 2020
- Published online by Cambridge University Press:
- 25 November 2019, pp. 154-160
- Print publication:
- February 2020
-
- Article
- Export citation
Infection prevention and control practices related to carbapenemase-producing Enterobacteriaceae (CPE) in acute-care hospitals in Ontario, Canada
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 40 / Issue 9 / September 2019
- Published online by Cambridge University Press:
- 27 June 2019, pp. 1006-1012
- Print publication:
- September 2019
-
- Article
- Export citation
Increased environmental sample area and recovery of Clostridium difficile spores from hospital surfaces by quantitative PCR and enrichment culture
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 39 / Issue 8 / August 2018
- Published online by Cambridge University Press:
- 09 August 2018, pp. 917-923
- Print publication:
- August 2018
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Falls and Wrist Fracture: Relationship to Women’s Functional Status after Age 50
-
- Journal:
- Canadian Journal on Aging / La Revue canadienne du vieillissement / Volume 35 / Issue 3 / September 2016
- Published online by Cambridge University Press:
- 01 July 2016, pp. 361-371
-
- Article
- Export citation
VRE and VSE Bacteremia Outcomes in the Era of Effective VRE Therapy: A Systematic Review and Meta-analysis
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 37 / Issue 1 / January 2016
- Published online by Cambridge University Press:
- 05 October 2015, pp. 26-35
- Print publication:
- January 2016
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Prevalence and Predictors of Antibiotic Use in Community-Based Elderly in Ontario, Canada
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 32 / Issue 7 / July 2011
- Published online by Cambridge University Press:
- 02 January 2015, pp. 710-713
- Print publication:
- July 2011
-
- Article
- Export citation
The Temporal Relationship Between Depression, Anxiety, and Functional Status after Traumatic Brain Injury: A Cross-lagged Analysis
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 17 / Issue 5 / September 2011
- Published online by Cambridge University Press:
- 01 June 2011, pp. 781-787
-
- Article
- Export citation
Carbon and nitrogen allocation patterns in two intertidal fucoids: Fucus serratus and Himanthalia elongata (Phaeophyta)
-
- Journal:
- European Journal of Phycology / Volume 33 / Issue 4 / November 1998
- Published online by Cambridge University Press:
- 01 November 1998, pp. 307-313
- Print publication:
- November 1998
-
- Article
- Export citation