55 results
Factors Associated with Voluntary Discharge in a Hospital Detoxification Unit: An Observational and Descriptive Analysis
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S135-S136
-
- Article
-
- You have access
- Open access
- Export citation
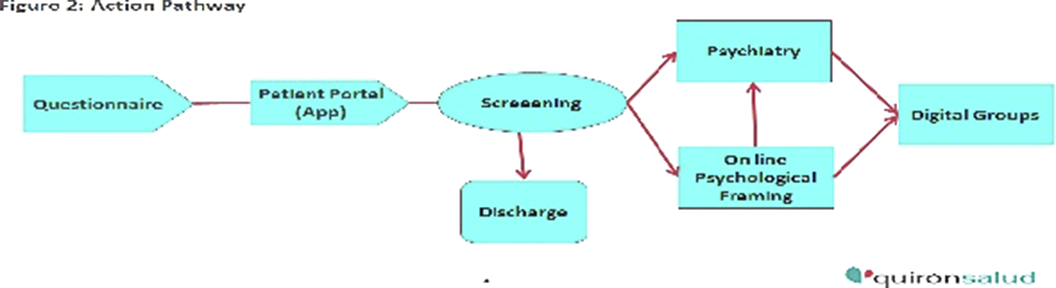
Mental Health and Addictions in Pregnancy: Feasibility and Acceptability of a Computerized Clinical Pathway and Prevalence Rates
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S66-S67
-
- Article
-
- You have access
- Open access
- Export citation
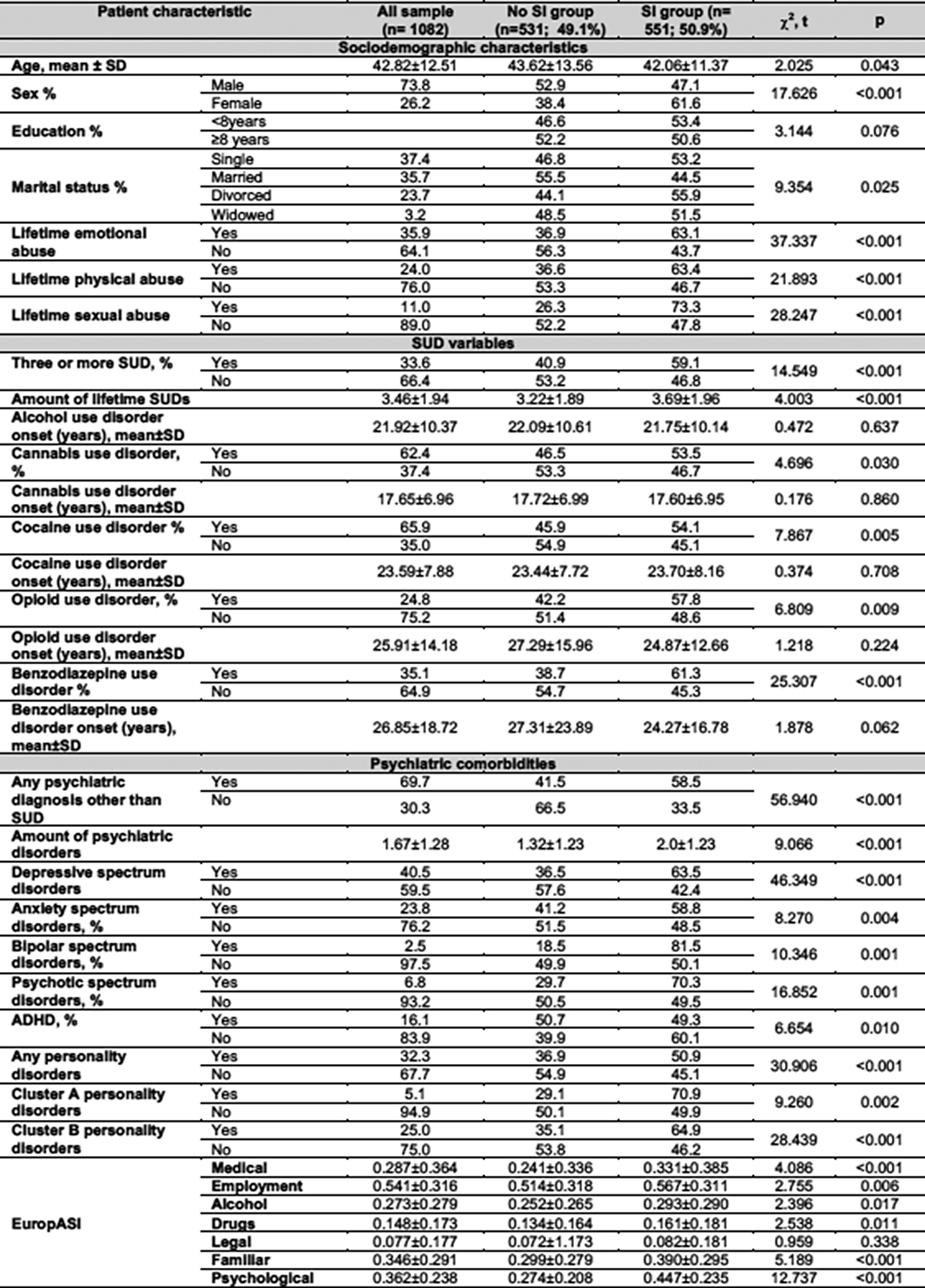
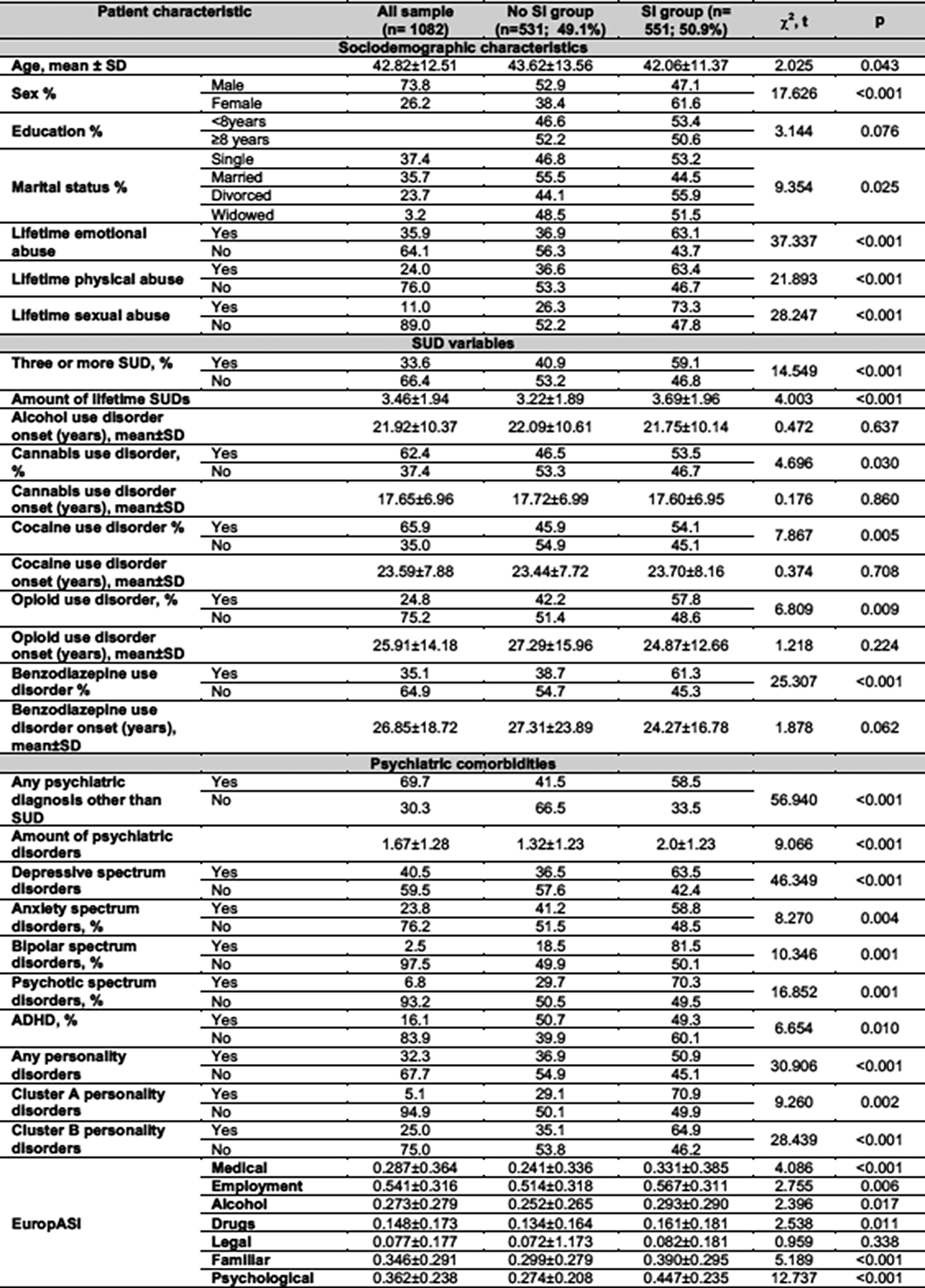
Clinical features and factors related to suicidal ideation in adult patients with benzodiazepine use disorder
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S135
-
- Article
-
- You have access
- Open access
- Export citation
A preliminary analysis of clinical characteristics of patient with alcohol use disorder and suicidal ideation
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S132-S133
-
- Article
-
- You have access
- Open access
- Export citation
A preliminary analysis of clinical characteristics of patient with alcohol use disorder and suicidal ideation
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S185-S186
-
- Article
-
- You have access
- Open access
- Export citation
Group therapy for problematic chemsex in Ngos community treatment settings in Spain
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S413-S414
-
- Article
-
- You have access
- Open access
- Export citation
Somatic multicomorbidity and disability in patients with psychiatric disorders in comparison to the general population: a quasi-epidemiological investigation in 54,826 subjects from 40 countries (COMET-G study)
-
- Journal:
- CNS Spectrums / Volume 29 / Issue 2 / April 2024
- Published online by Cambridge University Press:
- 25 January 2024, pp. 126-149
-
- Article
-
- You have access
- HTML
- Export citation
18 Regional patterns of mitochondrial function using phosphorus magnetic resonance spectroscopy in older adults at-risk for Alzheimer’s disease.
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 331-332
-
- Article
-
- You have access
- Export citation
Biomarkers and clinical predictors of long-term course in obsessivecompulsive disorder: A prospective cohort study
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S231
-
- Article
-
- You have access
- Open access
- Export citation
Aluminium Matrix Composite (AA6061/CaSiO3) Powders Obtained by Ball Milling
-
- Journal:
- Microscopy and Microanalysis / Volume 28 / Issue S1 / August 2022
- Published online by Cambridge University Press:
- 22 July 2022, pp. 2772-2773
- Print publication:
- August 2022
-
- Article
-
- You have access
- Export citation
A new player in the field: Methylphenidate in post-traumatic stress disorder treatment
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S453
-
- Article
-
- You have access
- Open access
- Export citation
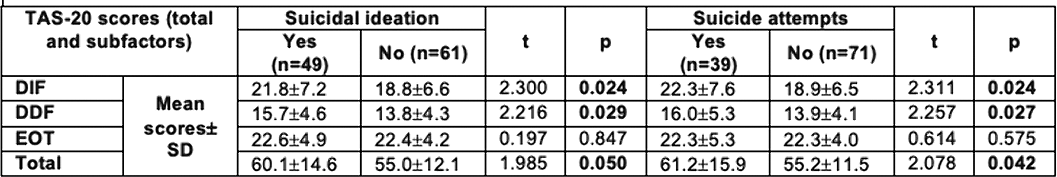
Patients with substance use disorder who have higher alexithymia levels present more suicidality history: Preliminary results in an outpatient addiction treatment center in Spain
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, pp. S581-S582
-
- Article
-
- You have access
- Open access
- Export citation
Inhibitory effect of positional syllable frequency in Spanish 2nd and 4th grade readers
-
- Journal:
- Applied Psycholinguistics / Volume 42 / Issue 1 / January 2021
- Published online by Cambridge University Press:
- 26 November 2020, pp. 1-17
-
- Article
- Export citation
PW01-51 - The Effect Of Broadening Generalized Anxiety Disorders Definition On Healthcare Resources Utilization And Costs: A Corollary From The Adan Study
-
- Journal:
- European Psychiatry / Volume 25 / Issue S1 / 2010
- Published online by Cambridge University Press:
- 17 April 2020, 25-E1453
-
- Article
-
- You have access
- Export citation
P03-313 - Art And Suicide
-
- Journal:
- European Psychiatry / Volume 25 / Issue S1 / 2010
- Published online by Cambridge University Press:
- 17 April 2020, 25-E1367
-
- Article
-
- You have access
- Export citation
P01-153 - Effect of Pregabalin on Patients with Refractory-severe Generalized Anxiety Disorder and Concomitant Severe Symptoms of Depression in Daily Medical Practice
-
- Journal:
- European Psychiatry / Volume 25 / Issue S1 / 2010
- Published online by Cambridge University Press:
- 17 April 2020, 25-E358
-
- Article
-
- You have access
- Export citation
Use of anticonvulsant agents in the management of alcohol dependence
-
- Journal:
- European Psychiatry / Volume 26 / Issue S2 / March 2011
- Published online by Cambridge University Press:
- 16 April 2020, p. 78
-
- Article
-
- You have access
- Export citation
Effect of pregabalin on generalized anxiety disorder patients with severe symptoms of anxiety and depression refractory to duloxetin
-
- Journal:
- European Psychiatry / Volume 26 / Issue S2 / March 2011
- Published online by Cambridge University Press:
- 16 April 2020, p. 173
-
- Article
-
- You have access
- Export citation
Broadening diagnostic criteria of generalized anxiety disorders from DSM-IV: The impact on patient level of disability
-
- Journal:
- European Psychiatry / Volume 26 / Issue S2 / March 2011
- Published online by Cambridge University Press:
- 16 April 2020, p. 172
-
- Article
-
- You have access
- Export citation
P0367 - Cognitive-behavioral group treatment for pathological gambling: Analysis of effectiveness and predictors of therapy outcome
-
- Journal:
- European Psychiatry / Volume 23 / Issue S2 / April 2008
- Published online by Cambridge University Press:
- 16 April 2020, p. S300
-
- Article
-
- You have access
- Export citation