68 results
Reflections on resilience
-
- Journal:
- Development and Psychopathology , First View
- Published online by Cambridge University Press:
- 23 February 2024, pp. 1-8
-
- Article
- Export citation
Resilience in children with chronic illness: Tests of the shift-and-persist and skin-deep resilience theories
-
- Journal:
- Development and Psychopathology / Volume 35 / Issue 5 / December 2023
- Published online by Cambridge University Press:
- 21 June 2023, pp. 2264-2274
-
- Article
- Export citation
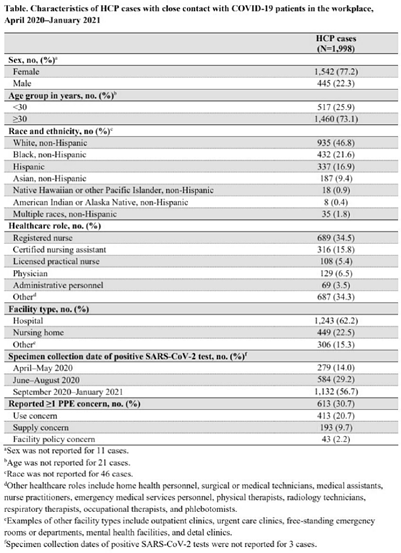
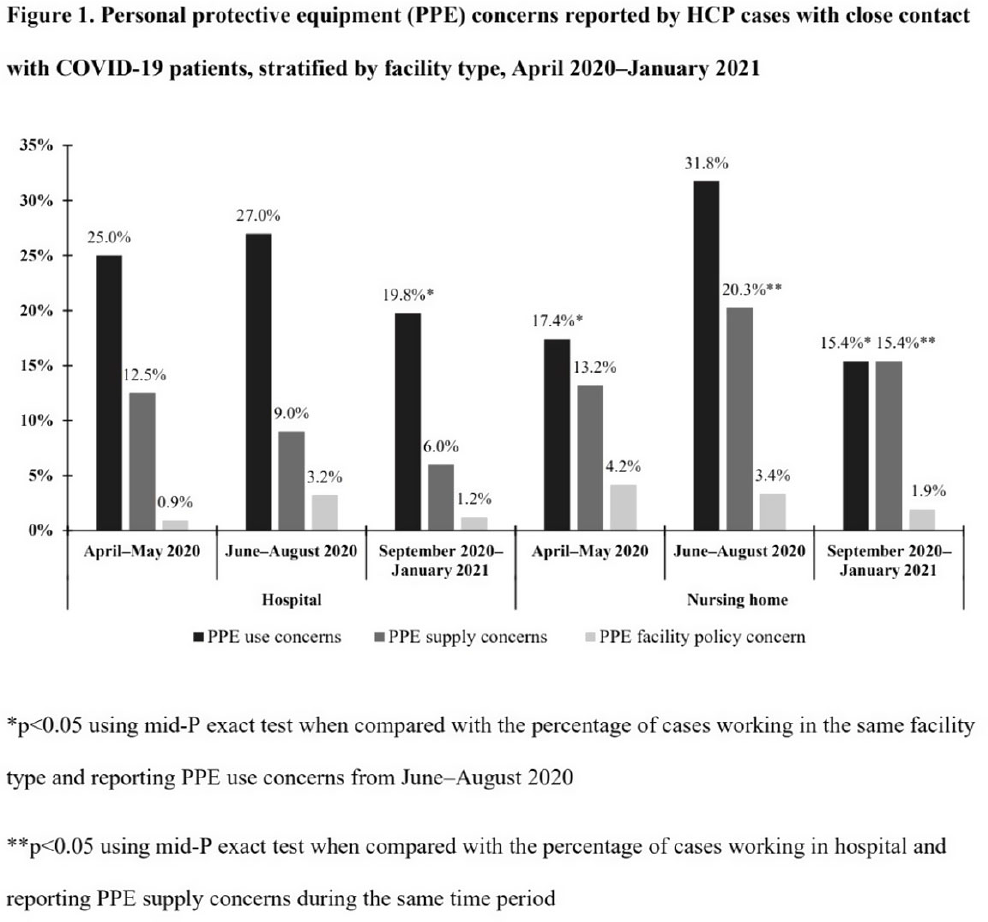
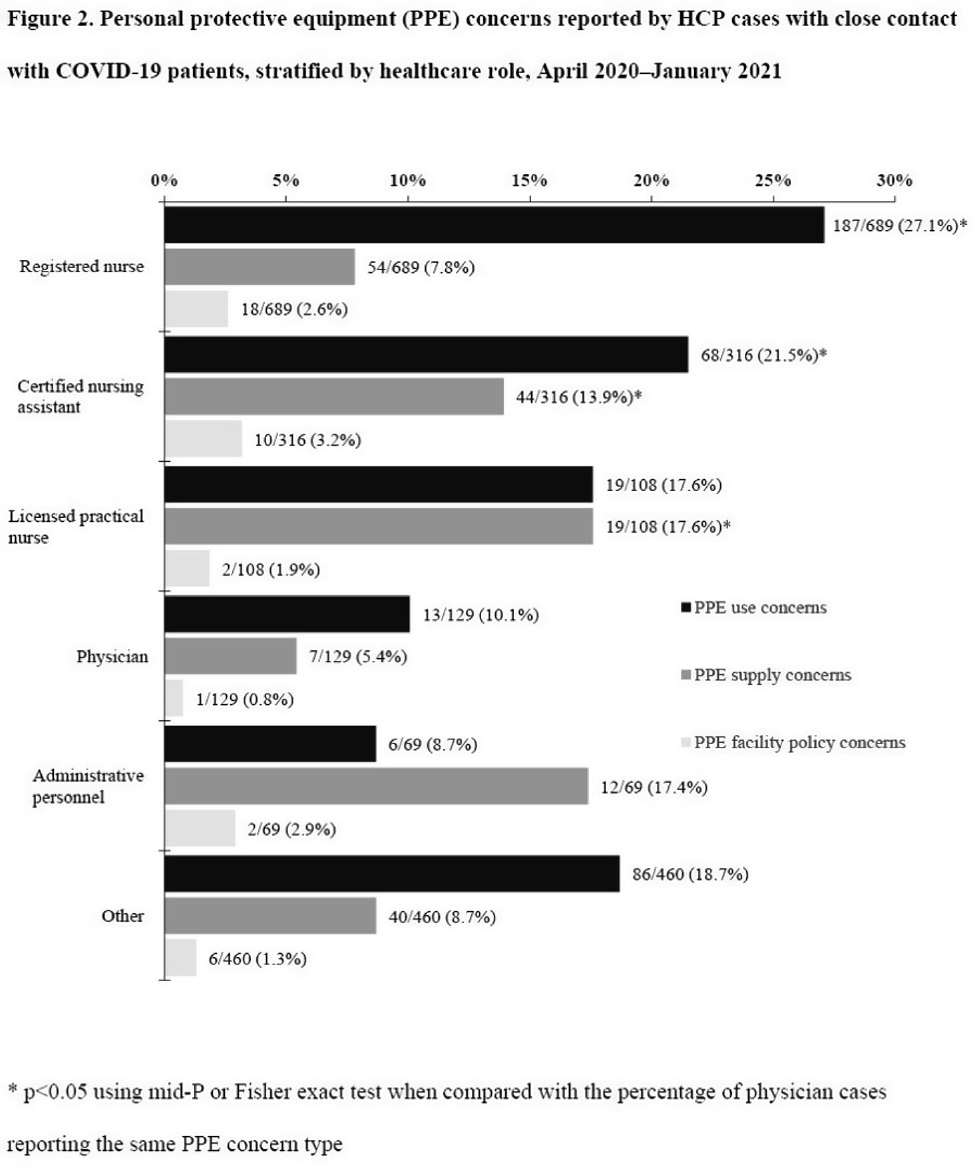
Characteristics of healthcare personnel who reported concerns related to PPE use during care of COVID-19 patients
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, pp. s8-s9
-
- Article
-
- You have access
- Open access
- Export citation
341 An intracranial EEG map of naturalistic images in the human brain
-
- Journal:
- Journal of Clinical and Translational Science / Volume 6 / Issue s1 / April 2022
- Published online by Cambridge University Press:
- 19 April 2022, p. 63
-
- Article
-
- You have access
- Open access
- Export citation
Harshness and unpredictability: Childhood environmental links with immune and asthma outcomes
-
- Journal:
- Development and Psychopathology / Volume 34 / Issue 2 / May 2022
- Published online by Cambridge University Press:
- 20 December 2021, pp. 587-596
-
- Article
- Export citation
23154 Electrical stimulation of hippocampus and amygdala produces multiple distinct responses in human ventral temporal cortex
-
- Journal:
- Journal of Clinical and Translational Science / Volume 5 / Issue s1 / March 2021
- Published online by Cambridge University Press:
- 31 March 2021, pp. 92-93
-
- Article
-
- You have access
- Open access
- Export citation
39 - Commentary on “The Impact of Faculty Psychology and Theories of Psychological Causation on the Origins of Modern Psychiatric Nosology”
- from Section 13
-
-
- Book:
- Levels of Analysis in Psychopathology
- Published online:
- 02 April 2020
- Print publication:
- 02 April 2020, pp 479-490
-
- Chapter
- Export citation
20 - Challenges in the Relationships between Psychological and Biological Phenomena in Psychopathology
- from Section 7
-
-
- Book:
- Levels of Analysis in Psychopathology
- Published online:
- 02 April 2020
- Print publication:
- 02 April 2020, pp 238-266
-
- Chapter
- Export citation
Life stress and cortisol reactivity: An exploratory analysis of the effects of stress exposure across life on HPA-axis functioning
-
- Journal:
- Development and Psychopathology / Volume 33 / Issue 1 / February 2021
- Published online by Cambridge University Press:
- 03 March 2020, pp. 301-312
-
- Article
- Export citation
Identifying strategies to promote team science in dissemination and implementation research
-
- Journal:
- Journal of Clinical and Translational Science / Volume 4 / Issue 3 / June 2020
- Published online by Cambridge University Press:
- 09 September 2019, pp. 180-187
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
3377 A cross-sectional analysis of opioid prescribing patterns among gynecologic oncologists using Medicare fee-for service provider utilization & payment data
-
- Journal:
- Journal of Clinical and Translational Science / Volume 3 / Issue s1 / March 2019
- Published online by Cambridge University Press:
- 26 March 2019, p. 31
-
- Article
-
- You have access
- Open access
- Export citation
18 - The Turks
- from Part III - Social and Cultural Context
-
-
- Book:
- Martin Luther in Context
- Published online:
- 16 August 2018
- Print publication:
- 30 August 2018, pp 152-159
-
- Chapter
- Export citation
Improving maternal–infant bonding after prenatal diagnosis of CHD
-
- Journal:
- Cardiology in the Young / Volume 28 / Issue 11 / November 2018
- Published online by Cambridge University Press:
- 06 August 2018, pp. 1306-1315
-
- Article
- Export citation
One size does not fit all: Links between shift-and-persist and asthma in youth are moderated by perceived social status and experience of unfair treatment
-
- Journal:
- Development and Psychopathology / Volume 30 / Issue 5 / December 2018
- Published online by Cambridge University Press:
- 06 August 2018, pp. 1699-1714
-
- Article
-
- You have access
- HTML
- Export citation
Brand Luther: 1517, Printing, and the Making of the Reformation. By Andrew Pettegree. New York: Penguin, 2016. xvi + 383 pp. $18.00 paper.
-
- Journal:
- Church History / Volume 87 / Issue 2 / June 2018
- Published online by Cambridge University Press:
- 30 July 2018, pp. 558-560
- Print publication:
- June 2018
-
- Article
- Export citation
Prehospital Modified HEART Score Predictive of 30-Day Adverse Cardiac Events
-
- Journal:
- Prehospital and Disaster Medicine / Volume 33 / Issue 1 / February 2018
- Published online by Cambridge University Press:
- 10 January 2018, pp. 58-62
- Print publication:
- February 2018
-
- Article
-
- You have access
- HTML
- Export citation
Threat vigilance and socioeconomic disparities in metabolic health
-
- Journal:
- Development and Psychopathology / Volume 29 / Issue 5 / December 2017
- Published online by Cambridge University Press:
- 22 November 2017, pp. 1721-1733
-
- Article
- Export citation
Childhood abuse and neglect and physical health at midlife: Prospective, longitudinal evidence
-
- Journal:
- Development and Psychopathology / Volume 29 / Issue 5 / December 2017
- Published online by Cambridge University Press:
- 22 November 2017, pp. 1935-1946
-
- Article
- Export citation
Knowledge, Attitudes, and Practices among Members of Households Actively Monitored or Quarantined to Prevent Transmission of Ebola Virus Disease — Margibi County, Liberia: February-March 2015
-
- Journal:
- Prehospital and Disaster Medicine / Volume 32 / Issue 6 / December 2017
- Published online by Cambridge University Press:
- 27 July 2017, pp. 673-678
- Print publication:
- December 2017
-
- Article
- Export citation
Impact of premix antimicrobial preparation and time to administration in septic patients
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 20 / Issue 4 / July 2018
- Published online by Cambridge University Press:
- 15 June 2017, pp. 565-571
- Print publication:
- July 2018
-
- Article
-
- You have access
- HTML
- Export citation