In many low- and middle-income countries, undernutrition, in the form of stunting, underweight, wasting and micronutrient deficiency, continues to be a major public health burden for children younger than 5 years of age( Reference Abdullah1). However, many low- and middle-income countries have started experiencing the double burden of malnutrition, where undernutrition and overweight are found in the same individuals, households and communities( 2). Worldwide, the prevalence of overweight and obesity among children younger than 5 years of age has increased from 4·2 % in 1990 to 6·7 % in 2010 and is expected to reach 9·1 % by 2020( Reference de Onis, Blössner and Borghi3). The relative increase over the past two decades has been greater in developing (+65 %) than in developed countries (+48 %)( Reference de Onis, Blössner and Borghi3). While the absolute prevalence of overweight among young children has increased more in middle-income countries, it has increased at a slightly faster pace in low-income countries( Reference Tzioumis, Kay and Bentley4). Among low-income sub-Saharan African countries, Rwanda has experienced one of the largest increases in overweight among children younger than 5 years of age( Reference Tzioumis, Kay and Bentley4, Reference Tzioumis and Adair5). Based on the most recent Demographic and Health Survey, 9·3 % of Rwandan children younger than 5 years of age are underweight and 7·7 % are overweight( 6).
The WHO has issued a call for double-duty actions for nutrition( 7) and to end malnutrition within a decade( Reference Hawkes, Demaio and Branca8). ‘Double-duty actions’ refer to interventions, programmes and policies that have the potential to address both undernutrition and overnutrition at the community level, acknowledging in part the similar biological, environmental and socio-economic factors affecting both forms of malnutrition( 7). For example, according to the WHO( 7), promotion of exclusive breast-feeding up to 6 months of age and appropriate complementary feeding practices in infants and young children are potential ‘double-duty actions’ based on initial evidence. Currently, most nutrition-specific and nutrition-sensitive programmes and policies focus primarily on reducing undernutrition( Reference Black, Victora and Walker9). More recently, some Ministries of Health have recognized the increasing prevalence of overweight and obesity but have yet to identify practical strategies to address this challenge( 10). In addition, little research has been conducted on strategies to prevent overweight and obesity in low- and middle-income countries( Reference Jaacks, Perry and Nyaku11).
One approach is to develop effective community-level interventions aimed at changing nutrition-related practices. Considering the sociocultural context and practical reality of the target populations, programmes should ensure that recommended practices are feasible and realistic( 12). Trials of Improved Practices (TIPs) is a formative research method designed to collect quantitative and qualitative data from families and communities regarding promotion, elimination or modification of specific health practices and the barriers and facilitators to performing the new practices( 12). The methodology was originally developed to examine the acceptability of complementary feeding recommendations among caregivers of young children in low-income countries( Reference Dickin, Griffiths and Piwoz13), and has since been applied to inform the development of other nutrition-specific interventions in low- and middle-income countries, such as improving dietary and iron–folate intake among pregnant Indian women( Reference Shivalli, Srivastava and Singh14) and dietary intake and feeding practices in Egyptian children younger than 2 years of age( Reference Kavle, Mehanna and Saleh15). In Rwanda, the TIPs methodology has been used with mothers of children younger than 2 years of age to identify the most acceptable and feasible changes to feeding practices to incorporate in counselling tools to address malnutrition( Reference Karumba16). However, data are lacking on the acceptability of practices specifically for young overweight children and practices that apply to both under- and overweight children.
The goal of the present study was to identify feasible and acceptable behaviours that might achieve more optimal dietary intake and physical activity practices among both under- and overweight children from 6 to 59 months of age in Rwanda. Specifically, the study explored: (i) the usual feeding and physical activity behaviours among under- and overweight children in Rwanda and related caregiver beliefs; and (ii) caregivers’ experiences when trying recommended practices to improve their child’s feeding and physical activity practices using the TIPs methodology.
Methods
Study setting
We collected data in the urban district of Gasabo (population over 530 000 people) in the City of Kigali and in the rural district of Rulindo (population nearly 300 000) in the North Province to represent areas with different prevalence of overweight/underweight and different food availability. Based on data from the Rwanda Demographic and Health Survey, in urban areas overweight in children is more common than underweight (11 v. 7 %); conversely, in rural areas underweight in children is more prevalent than overweight (10 v. 6 %)( 6). Almost all Rwandan children are breast-fed for at least some time, but only 19 % of children aged 6–23 months met minimum dietary diversity standards and were fed at least the minimum number of times( 6).
Sample
The sample size was based on the minimum number of interviews to achieve saturation in each subgroup of interest( Reference Baker and Edwards17, Reference Guest, Bunce and Johnson18). Sampling was purposive, based on the inclusion criteria of the child’s age (i.e. 6–59 months) and weight status (i.e. underweight defined as weight-for-age Z-score < −2 or overweight defined as weight-for-height/length Z-score > +2)( 19). We recruited primary caregivers, defined as a self-reported biological parent who spent the most time with the eligible child, and we included only one caregiver per child and one child per caregiver in the study. When there were multiple eligible children for one caregiver, the child who best helped fulfil the sampling quota according to child age, weight status and urban/rural location was selected. We intentionally oversampled caregivers of overweight children because less information is available regarding the feeding and physical activity practices for overweight children in sub-Saharan Africa compared with underweight children. Because child feeding practices vary greatly from 6 to 59 months, we divided the sample into groups of caregivers of children aged 6–11 months, 12–23 months and 24–59 months.
We identified potentially eligible caregivers with assistance from local leaders and community health workers. Out of the 2341 caregivers that we screened, 141 caregivers were eligible and were recruited and enrolled. Four caregivers were lost to follow-up, while one caregiver was excluded from data analysis because of implausible child anthropometric measurements. Our final sample comprised 136 caregivers (mainly mothers, with a few fathers and grandmothers), evenly divided between urban and rural areas. We obtained informed consent from all interested and eligible caregivers, who also consented on behalf of the children.
Procedures
We developed counselling guides for each age group that included specific practices for trained data collectors to recommend to families based on an initial assessment and identification of behaviours to modify towards more optimal feeding and physical activity practices. Counselling guides were based on current international recommendations for complementary feeding( 20– 22) and young children’s physical activity( 23– 25), as well as Rwanda’s National Community Maternal, Infant and Young Child Nutrition Counselling Package( 26), the counselling guides from a previously implemented TIPs study in Rwanda( Reference Karumba16) and recently developed guidelines specific to responsive feeding( Reference Peréz-Escamilla, Segura-Pérez and Lott27). Counselling guides included recommendations for behaviours regarding breast-feeding, appropriate quantity of food, appropriate consistency of food, appropriate feeding frequency, dietary diversity and diet quality (hereafter referred to as ‘dietary diversity’), responsive feeding, hygiene and food handling, feeding during and after illness, and physical activity. Data collectors participated in a 5 d training on the content and methodology for the study and a 3 d pilot study to test and refine the data collection instruments and procedures.
The study followed the structured TIPs methodology( Reference Dickin, Griffiths and Piwoz13) such that data collectors visited each household a total of three times, first to collect baseline information on the child’s feeding and physical activity practices, second to recommend practices based on issues identified in the first visit and work with the caregiver to select new practices to try, and third to assess the family’s experience with trying the practices. TIPs employs a variety of data collection methods (i.e. open- and closed-ended questions, observations, dietary assessments) and, at each household visit, we collected both quantitative and qualitative data. Participants received approximately $US 5 per household visit to compensate them for their time.
Visit 1: Interview and in-home observation
Data collectors conducted structured interviews with caregivers to obtain demographic information on household socio-economic status, household hunger( Reference Ballard, Coates and Swindale28), breast-feeding and other feeding practices, recent history of child illness, child use of electronics and child physical activity patterns. Data collectors also conducted in-home observations to assess feeding and physical activity practices using a scripting method( Reference Bentley, Boot and Gittelsohn29). Data collectors observed a meal and documented interactions between the child and the caregiver and other family members while eating, any mealtime distractions, the types and amount of food given to the child, and hygiene and food handling behaviours. Data collectors also spent 1 h before or after the interview observing and recording the level and type of physical activity exhibited by the child, including time spent being sedentary. On average, Visit 1 lasted approximately 3 h.
Following Visit 1, data collectors rapidly assessed the data to identify discrepancies between the child’s feeding and physical activity practices and international recommendations using a tool designed by the study investigators. The tool guided data collectors through a series of questions and indicated where to find the Visit 1 data needed to answer each question and where to look in the age-appropriate counselling guide to identify relevant practices to recommend. Data collectors then used the counselling guide for the child’s age group to select specific practices to recommend to the caregiver that might lead to more optimal feeding and physical activity behaviours. In situations where multiple practices were relevant to recommend to a caregiver, data collectors were instructed to use other information from the assessment (e.g. food security) to prioritize recommendations that might be most feasible for and acceptable to the caregiver.
Visit 2: Counselling on recommended new practices
The second household visit occurred 1–2 d after Visit 1 and functioned as a ‘counselling visit’, during which data collectors provided feedback to the caregiver about current feeding and physical activity practices, recommended three to five specific practices selected from the counselling guides, and encouraged each caregiver to select one to three of the recommended practices to try during the following week (see Table 2 for example practices). On average, Visit 2 lasted approximately 1 h.
Visit 3: Examination of the acceptability of new practices
Seven days after Visit 2, the data collector returned to the household to interview the caregiver about the family’s experience trying the new practices. Data collectors captured information regarding the practices caregivers tried, the facilitators and barriers encountered, reactions of others who were informed about the recommended practices, whether caregivers were willing to continue the new practices after the trial period, and whether caregivers would recommend the new practices to others in the community. On average, Visit 3 lasted approximately 1 h.
Analysis
We entered all quantitative data from each household visit into the data processing software package CSPro version 7.0.0 (US Census Bureau, ICF International and Serpro SA) and verified entries against original paper copies when we identified discrepancies. Univariate statistics were conducted to describe demographic characteristics and tabulate practices recommended and tried by caregivers. We calculated all quantitative analyses using the statistical software package Stata version 13.0 (StataCorp LP). Audio recordings from interviews conducted in Kinyarwanda were transcribed and translated into English, and written observations were translated into English. We conducted thematic content analysis on interviews and observations( Reference Gibbs30). We used the qualitative data analysis software Dedoose version 7.0.23 (SocioCultural Research Consultants LLC) to code and sort the coded data by weight subgroups and then placed them into data matrices( Reference Miles and Huberman31). We focused our analysis on identifying similarities and differences between under- and overweight children and used qualitative data to complement and contextualize the quantitative data.
Results
Table 1 provides characteristics of the participants. Most caregivers were married with at least some education, and the child in the study was generally not their first child.
Table 1 Child and household characteristics, by child weight category and overall, in the sample of caregivers and their under- or overweight children from 6 to 59 months of age (n 136), Rwanda, May–September 2017
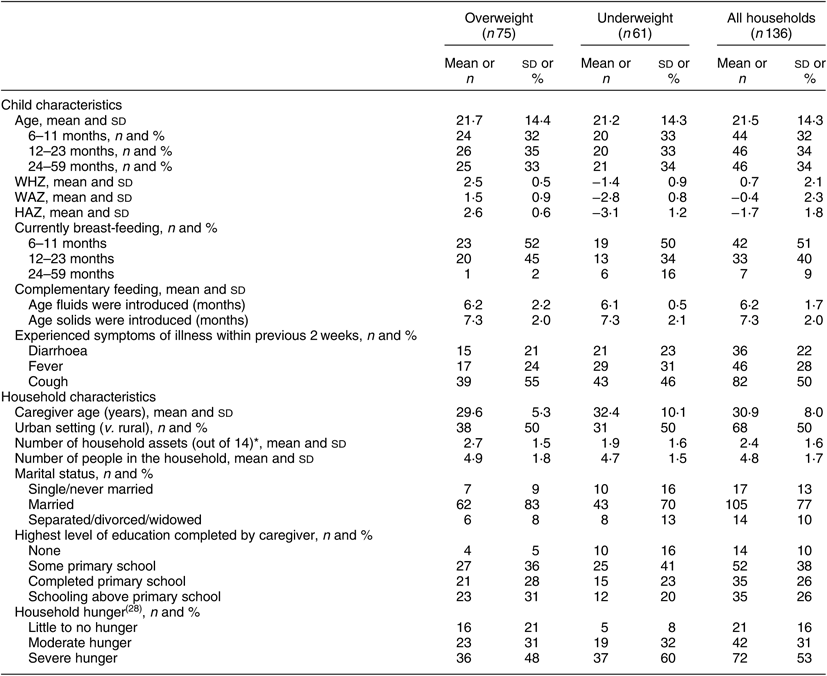
WHZ, weight-for-height Z-score; WAZ, weight-for-age Z-score; HAZ, height-for-age Z-score.
* Household assets include electricity, radio, watch, refrigerator, bicycle, motorcycle or motor scooter, animal-drawn cart, car or truck, boat without a motor, boat with a motor, non-mobile telephone, mobile telephone, television and computer.
As data from each household visit inform data from the subsequent household visits, we present the remaining results according to the sequential household visits and highlight similarities and differences between under- and overweight children where applicable.
Visit 1: Description of usual child feeding and physical activity practices and related caregiver beliefs
Data collected from the in-home observations and interviews of child feeding and physical activity practices showed both similarities and differences regarding feeding behaviours and activity levels of under- and overweight children. Observations conducted during the first household visit revealed that many underweight children did not eat all that was offered while overweight children seemed to be more likely to finish it all. Within a given meal, we observed many caregivers of overweight children continuing to try to feed the child after he/she exhibited fullness cues. During interviews, more caregivers of over- than underweight children reported feeding their child on a schedule, rather than on demand:
‘She eats at the time I set for her … I decide to feed her according to the time.’ (Caregiver of 12–23-month-old overweight child, rural area)
‘Every time she’s hungry I feed her.’ (Caregiver of 24–59-month-old underweight child, rural area)
Caregivers of both under- and overweight children recognized the importance of children eating a diverse diet, as evidenced through descriptions of feeding the child a variety of foods, and ‘nutrients’ and ‘vitamins’ seemed to be known. They appropriately cited foods as contributing to a balanced diet (e.g. vegetables, fruits, beans, animal-source foods) and as being unhealthy for children (e.g. foods with too much oil, sugar and salt):
‘If a child eats the same foods very often it can cause a child to be unhealthy.’ (Caregiver of 12–23-month-old overweight child, urban area)
‘[The good foods] are fruits, vegetables, energy giving and nutritive foods like meat, dodo [amaranth], dry small fishes, beans, cassava, sweet potatoes, milk and porridge. They are good because they include foods with nutrients like energy giving, body building. A full diet must also include vegetables, beans, fruits and porridge.’ (Caregiver of 12–23-month-old underweight child, rural area)
Caregivers widely acknowledged the importance of hygiene for their child, but then some caregivers of both under- and overweight children failed to wash their child’s hands before meals or allowed their child to eat off the floor. In instances when children experienced diarrhoea or fever in the previous 2 weeks, most caregivers reported feeding their child during and afterwards in ways that were generally aligned with international guidelines( 20). Health workers were cited as the top source of information on infant and young child feeding (IYCF) among caregivers of both under- and overweight children.
Many caregivers reported associating a physically active and playful child with being a healthy child. The sentiment that a child being ‘fat’ was a sign of a healthy child was also expressed by some caregivers of under- and overweight children in both urban and rural areas, although this was slightly more prevalent among caregivers of overweight children:
‘A healthy child is a child who doesn’t like to be sick, who actively plays with others with no problem, who does not like to be alone, and is not too quiet.’ (Caregiver of 24–59-month-old overweight child, urban area)
‘A healthy child is a child who is very fat, plays without any problem, not lonely, very active, strong and has started to stand up and crawl.’ (Caregiver of 6–11-month-old underweight child, rural area)
Overweight and underweight children were observed to engage in similar types of physical activities (e.g. crawling, walking and/or jumping; throwing a ball or toy; short bursts of activity). However, 53 % of caregivers of underweight children said their child was a lot less active than other children compared with 9 % of caregivers of overweight children. Observations showed similar use of electronics among under- and overweight children, but interview responses revealed overweight children may play with mobile phones slightly more than underweight children (33 % of overweight children play with mobile phones daily compared with 13 % of underweight children).
Visits 2 and 3: Practices recommended and tried
Data collectors recommended two or three practices per caregiver, for a total of 192 and 238 practices recommended to caregivers of under- and overweight children, respectively (Fig. 1). Practices most frequently recommended to caregivers of overweight children related to dietary diversity, hygiene and food handling, quantity of food and feeding frequency. Practices most frequently recommended to caregivers of underweight children were the same except that, instead of practices related to feeding frequency, practices related to food consistency were frequently recommended. Dietary diversity recommendations were the most frequently recommended for both under- and overweight children (43·8 v. 53·3 %, respectively).
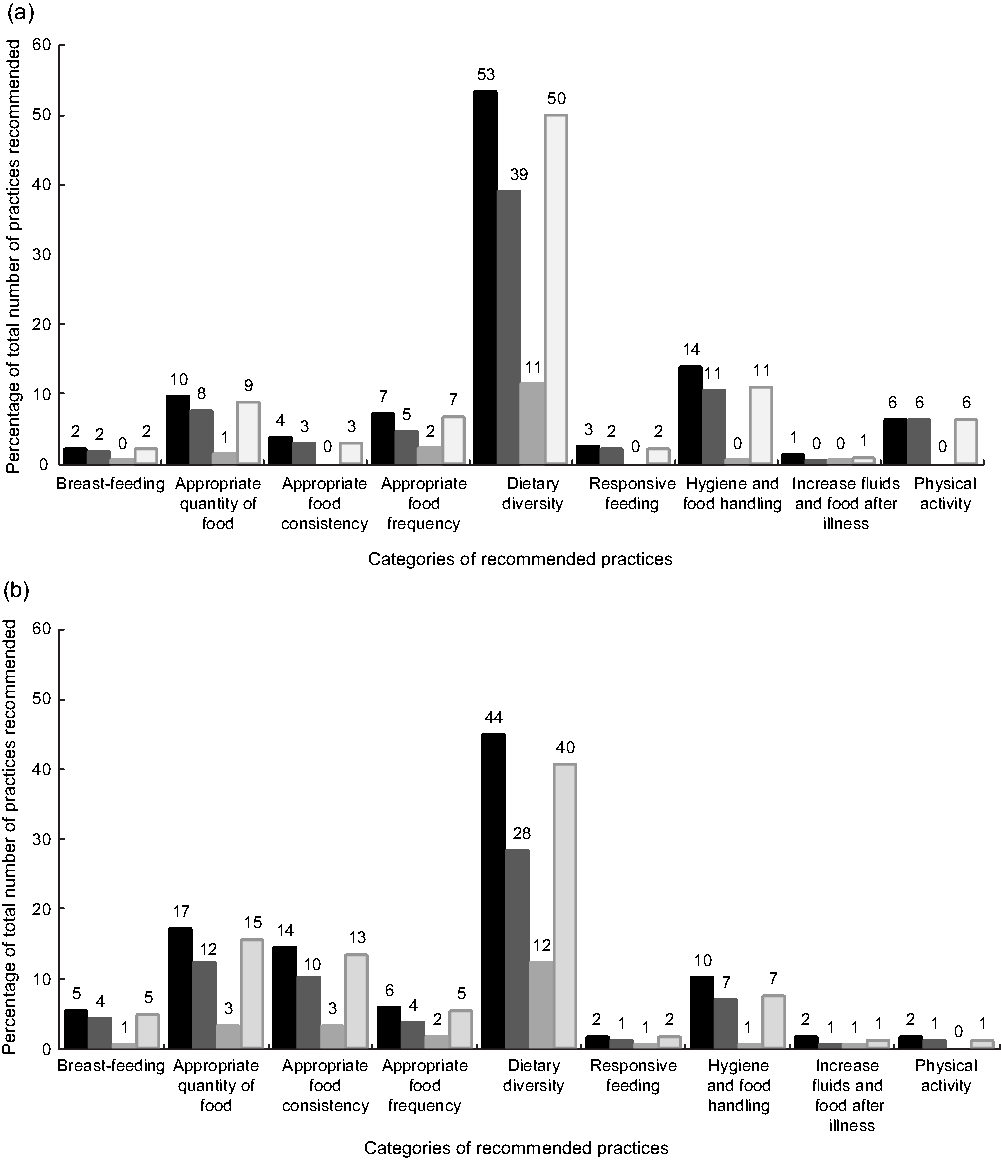
Fig. 1 Percentage of child feeding and physical activity practices recommended to (![]() ) and tried (
) and tried (![]() , tried without modification;
, tried without modification; ![]() , tried with modification;
, tried with modification; ![]() , planned to continue) by caregivers of (a) overweight and (b) underweight children from 6 to 59 months of age (n 136), Rwanda, May–September 2017. A total of 238 and 192 practices were recommended to caregivers of over- and underweight children, respectively
, planned to continue) by caregivers of (a) overweight and (b) underweight children from 6 to 59 months of age (n 136), Rwanda, May–September 2017. A total of 238 and 192 practices were recommended to caregivers of over- and underweight children, respectively
Out of a total of eighty-two unique practices that were recommended, 33 % (27/82) were tried only by caregivers of underweight children, 37 % (30/82) were tried only by caregivers of overweight children and 30 % (25/82) were tried by both caregivers of under- and overweight children (Fig. 2). Table 2 shows the twenty-five specific practices in Fig. 2 that both caregivers of under- and overweight children tried.
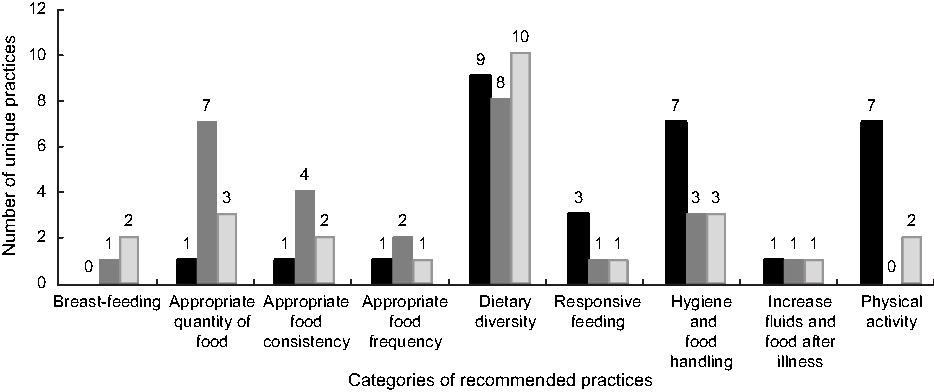
Fig. 2 Of eighty-two unique child feeding and physical activity practices recommended, number that were tried (![]() , overweight only;
, overweight only; ![]() , underweight only;
, underweight only; ![]() , both) by caregivers of under- and overweight children from 6 to 59 months of age, Rwanda, May–September 2017
, both) by caregivers of under- and overweight children from 6 to 59 months of age, Rwanda, May–September 2017
Table 2 Practices recommended to both caregivers of overweight children and caregivers of underweight children from 6 to 59 months of age, Rwanda, May–September 2017

Visit 3: Acceptability of recommended practices
Facilitators and barriers to trying new practices
The most common facilitator to trying a practice among caregivers of both under- and overweight children was its perceived benefit for the child’s health. Other facilitators expressed by caregivers included caregivers’ perceptions that the child liked the new practice; the availability and/or affordability of the input (e.g. food, water, ash, or a local water treatment product); the ease of implementing the practice; and the counselling received from data collectors:
‘I liked it more because I took enough time to take care and feed him myself. I tried it, I saw that it was good, and I saw that he eats more than he ate before.’ (Caregiver of 24–59-month-old underweight child, urban area)
Almost all careivers reported they were willing to continue the recommended practices (Fig. 1) and for the same reasons that they were willing to try them, namely perceived child health benefits and child’s preference for the practice. For example,
‘[I plan to continue the practice] because the child responds well. When I change food and I find that she eats it, it makes me proud as a parent. It is therefore good because as she continues to eat well, she will grow well.’ (Caregiver of 12–23-month-old underweight child, rural area)
Reported reasons for not trying a recommended practice included child illness during the practice testing period, financial constraints, limited food availability, competing interests for caregivers’ time, forgetting, or fear of a negative response from the child. Many caregivers did not report barriers to the new practices they tried. The difficulties named by some were similar to reasons reported for not trying a new practice; a few caregivers said these same factors could constrain their ability to continue with the practice:
‘The problem I have is to find time to feed her all the food until she finishes it. It requires much more time, and I have a lot to do.’ (Caregiver of 12–23-month-old underweight child, rural area)
‘It is hard to find the type of flour for porridge that I want to buy here in our community. I have to go to a shop far away.’ (Caregiver of 6–11-month-old overweight child, rural area)
For nearly all feeding and physical activity categories, at least one caregiver reported modifying the recommended practices to overcome a barrier. Modifications usually involved implementing the parts of the practice that were most feasible for caregivers, such as purchasing or feeding only one or two foods from a list of many food options (e.g. vitamin A-rich fruits and vegetables) or implementing the practice less frequently than intended:
‘I was able to buy beans, dodo [amaranth leaves], isombe [cassava leaves], meat and fruits such as mangoes and avocados. That’s all I got. Other foods … I could not buy them. I didn’t have enough money to buy everything.’ (Caregiver of 12–23-month-old underweight child, rural area)
Child responses to new practices
Caregivers reported that child responses to new practices were far more positive than negative. The child ‘seemed to like it [the practice they had tried]’ was the most common response. Caregivers reported that the child was happy during the practice, did not refuse it or had no problems with it. Other positive responses reported included children eating more and/or ‘with appetite’, having increased strength or energy, sleeping better, gaining weight and playing with others:
‘She didn’t have any problem [with the thicker porridge]. She liked it.’ (Caregiver of 24–59-month-old overweight child, urban area)
The only negative response reported by caregivers showed a reluctance among children to try the new practice and/or food or that the child did not like it. In many cases, this was accompanied by what caregivers described as an initial 1–2 d adjustment period, followed by the child accepting the new practice or food. These negative responses and adjustment periods were noted more by caregivers of overweight children than caregivers of underweight children:
‘For the first two days [of not giving child biscuits or fried foods], it was hard as he used to take porridge with biscuits or mandazi [doughnuts]. But now he accepted it as his habit.’ (Caregiver of 12–23-month-old overweight child, urban area)
External support for trying new practices
Nearly half of all caregivers (62/136) said they had told at least one person about one or more of their new practices and received positive responses, including support and encouragement to continue the practice. About 20 % (12/62) of caregivers received negative feedback from others, pertaining to the practice not being easy, the practice not being effective or the practice being unnecessary:
‘The neighbours discouraged me. They said that my child was normal and that it wasn’t worth reducing his food intake. They said that a child who is fat is healthy.’ (Caregiver of 12–23-month-old overweight child, rural area)
Discussion
The present study used TIPs to examine caregivers’ and their children’s reactions to trying recommended behaviours that might lead to more optimal feeding and physical activity practices in both under- and overweight infants and young children. Our goal was to take an initial step towards addressing the WHO( 7) call to identify double-duty actions that have the potential to address the double burden. Formative research including the TIPs method is helpful for designing behavioural interventions because it elucidates key information related to a specific context and potential beneficiaries’ current behaviours and beliefs that can influence the success of an intervention and its intended impacts on nutrition outcomes( Reference Daelmans, Ferguson and Lutter32– Reference Bentley, Johnson and Wasser38). While previous TIPs studies have focused on healthy, undernourished and/or ill children( Reference Karumba16, 39– 42), we used TIPs with a new population, caregivers of overweight children, to identify whether existing international and national IYCF and physical activity messages are relevant to and acceptable among caregivers of under- and overweight children and to delineate how other messages may need to be adapted for each group.
We identified several categories of practices (e.g. dietary diversity, responsive feeding) and twenty-five specific practices that were relevant for both under- and overweight children and demonstrated their feasibility and acceptability by caregivers in Rwanda. The categories of practices most frequently recommended in our study were related to dietary diversity, quantity of food, and hygiene and food handling. Dietary diversity, especially inclusion of animal-source foods and vitamin A-rich fruits and vegetables in the diet, was an issue for both under- and overweight children in our study. This is not surprising given that only 30 % of children aged 6–23 months in Rwanda achieve minimum dietary diversity( 6) and indicates that diet quality may be inadequate regardless of child weight status. While some foods were missing in the diets of both under- and overweight children, we recommended to caregivers of overweight children more frequently than caregivers of underweight children that they should reduce the child’s consumption of fried foods and sugar-sweetened beverages (indicative of poor diet quality).
As with dietary diversity, some of the recommendations about appropriate quantity of food were adapted for the child’s weight status. For example, whereas we explicitly encouraged caregivers of underweight children to increase the quantity of food they fed to their child at one time (while also paying attention to hunger and fullness cues), we only recommended caregivers of overweight children look for fullness cues to know when to stop feeding rather than suggesting that they decrease the amount of food they fed to their child. While current international IYCF guidelines provide approximate daily energy needs for infants and young children in kilocalories, they also recognize it is challenging for caregivers to know how many kilocalories children have consumed through breast milk and complementary foods. Consequently, the guidelines encourage caregivers to use responsive feeding techniques to help them determine how much food to offer their child, in addition to ensuring adequate energy density through inclusion of nutritious foods and adequate feeding frequency( 20, 21). Caregivers’ attentiveness to their child’s fullness cues may not be an effective strategy in the context of overweight, when satiation may be altered( Reference Herbert and Pollatos43– Reference Slyper, Kopfer and Huang45). Some research suggests that breast-feeding promotes children’s self-regulation of feeding( Reference Brown and Lee46, Reference Rose, Savage and Birch47), so recommending exclusive breast-feeding for 6 months and continued breast-feeding for 24 months may be beneficial in this regard.
Hygiene and food handling may be a concern for both under- and overweight children( 6). Literature suggests that poor hygiene and sanitation may contribute to stunting( Reference Cumming and Cairncross48, Reference Mbuya and Humphrey49) and research is ongoing regarding the biological causal mechanisms( Reference Null, Stewart and Pickering50), including changes to the gut microbiome and architecture( Reference Blanton, Barratt and Charbonneau51). Researchers are also exploring the potential link between the microbiome and overweight/obesity in children and adults( Reference Sanmiguel, Gupta and Mayer52, Reference Koleva, Bridgman and Kozyrskyj53). It is likely that data collectors in the current study recommended hygiene behaviours frequently because facilities for good hygiene, such as handwashing stations with clean water and soap or ash, are limited in Rwanda and a strong emphasis has been placed on the link between hygiene/sanitation and nutrition in the country.
Data from our first household assessment visits revealed evidence of the cultural belief in both urban and rural areas in Rwanda that overweight in children is a sign of good health. We also found that mainly caregivers of overweight children received negative responses from relatives and other community members about the practices they were testing as part of the study. Some of these responses are indicative of a failure to recognize that the child is overweight or that being overweight could be linked with poor health. Beliefs that larger body sizes in children are healthy have been reported in other African countries, including Malawi and Egypt( Reference Kavle, Mehanna and Saleh41, Reference Flax, Thakwalakwa and Ashorn54), and have likely developed from generations of experience with the impact of undernutrition on child mortality. Sensitizing communities about the importance of appropriate complementary feeding practices for overweight children may be a necessary component for future interventions tackling the double burden of malnutrition, particularly in low-resource countries where families may consider overweight to be good for their child. Caregivers in the present study cited women’s and parent’s groups, church meetings, health centres and community gatherings as places where they would discuss new IYCF practices and they could be appropriate settings for sensitization in addition to dissemination avenues for future interventions. Studies demonstrating the health benefits of appropriate weight within these communities might also be beneficial for combatting these entrenched beliefs.
Aside from the negative responses given to caregivers of overweight children, all other caregivers in the current study who reported telling someone about a recommended practice received positive responses, including encouragement and support to continue. While IYCF interventions and programmes have historically targeted mothers, research in several African countries has recognized the importance of grandmothers and fathers in breast-feeding and child feeding decisions( Reference Aubel55– Reference Susin and Giugliani62). Caregivers in the present study reported husbands, grandmothers, sisters, aunts and other mothers in their communities as main contacts they told about the new practices; thus, these influencers would be important to incorporate in a future intervention. Contact with health workers has also been cited as an influencer in maternal and child health decisions in low-resource settings( Reference Agho, Dibley and Odiase63– Reference Flax, Hamela and Mofolo65) and caregivers in the present study overwhelmingly cited health workers as the source of their IYCF knowledge. Recently, the WHO recommended that health workers at primary health-care facilities provide counselling on nutrition and physical activity to caregivers of overweight children younger than age 5 years to prevent overweight and obesity later in life. Specific information on the content of the counselling guidance is forthcoming( 66).
Our study had some limitations. First, because recommendations were based on the Visit 1 assessment, we were not able to test all practices to the same extent; some were not tested at all. Second, caregivers had only 1 week to try the new practices, as recommended in the TIPs manual( Reference Dickin, Griffiths and Piwoz13). A longer trial period, as tested in other studies( Reference Shivalli, Srivastava and Singh14, Reference Dickin and Seim67), would reveal more about the sustainability of behaviours. Third, we should be cautious when interpreting the self-reported data, as social desirability bias may have affected responses from caregivers about their experiences with the practices and their intentions to continue. These limitations are present in most TIPs studies and do not detract from the use of the findings as formative data to inform future interventions or programmes.
Conclusion
In conclusion, the findings from this new application of the TIPs methodology can be used in Rwanda to adapt global IYCF and physical activity messages to the local setting to develop interventions addressing the double burden. We recommend placing an emphasis on diet quality (e.g. eating more fruits and vegetables; reducing intake of foods and beverages high in sugar, salt and fat) as a key double-duty action( 68– Reference Mennella, Reiter and Daniels77). In addition, future double burden interventions targeted at children in Rwanda need to address cultural beliefs related to child overweight and facilitators and barriers to adopting the practices while also involving key influencers. Messaging in interventions should capitalize on the benefit to the child’s health as a motivator for behaviour change and inform caregivers of potentially temporary negative responses from the child. Furthermore, many of our recommended practices were applicable to more than one feeding category (e.g. addressed both quantity of food and responsive feeding), but were categorized to only one topic for analysis. The complex nature of and interrelated aspects of IYCF point to the need to address child weight status through a suite of integrated behaviours rather than recommending single practices to families in isolation. A complete set of double-duty messages should be tested for their impact on the child’s dietary behaviour, longer-term implementation by caregivers, and the growth and development of under- and overweight children in Rwanda.
Acknowledgements
Acknowledgements: The authors thank Carrie Rains and John Baron of RTI International and Kyle McNally, Eden Clayton and Becky Cathcart of Three Stones Consulting for their research assistance. Financial support: RTI International provided research funding for this study. RTI International funders had no role in the design, analysis or writing of this article. Conflict of interest: There are no conflicts of interest. Authorship: V.L.F., M.K.M., C.H.S. and P.A.W. formulated the research questions and designed the research. S.N. and J.R. contributed to development of data collection instruments, enrolled participants and conducted the study. C.H.S. and H.S. analysed the data. P.A.W., C.H.S., V.L.F. and H.S. wrote the first draft of the manuscript. All authors contributed to the interpretation of the data, edited the manuscript and approved its final contents. P.A.W. has primary responsibility for the paper’s final content. Ethics of human subject participation: This study was conducted according to the guidelines laid down in the Declaration of Helsinki and all procedures involving human subjects were approved by the Rwanda National Ethics Committee and RTI International’s Institutional Review Board. Written consent was obtained from all participants.
Author ORCIDs
Pamela A Williams, 0000-0002-6040-6972. Courtney H Schnefke, 0000-0003-0181-1502. Valerie L Flax, 0000-0003-0200-3355.








