Hypertension is a strong and modifiable determinant for the development of several chronic diseases( Reference Lloyd Jones, Adams and Brown 1 ). Hypertension is the first leading global risk factor for mortality in the world. It is responsible for 13 % of deaths( 2 ) and 92 million disability-adjusted life-years (6 % of the total). Therefore, complications associated with hypertension account for 9·4 million deaths worldwide yearly( Reference Lim, Vos and Flaxman 3 ), and it is responsible for at least 45 % of deaths due to heart disease and 51 % of deaths due to stroke( 4 ).
Available evidence supports the important role of food habits in the aetiology of hypertension( Reference Ibrahim and Damasceno 5 ). Cooking methods may modify the role of some foods or nutrients with respect to the risk of hypertension. Among cooking methods, frying is one of the most common methods in Western countries. The consumption of fried foods is increasing due to their desirable characteristic flavour, brown colour and crispy texture, which make them very popular with consumers( Reference Boskou, Salta and Chiou 6 ). The frying process involves many factors: some factors are dependent on the process itself, whilst others are related to the type of food and fat that are used for frying( Reference Saguy and Pinthus 7 ). According to previous studies such as the Seguimiento Universidad de Navarra (SUN) cohort study( Reference Sayon-Orea, Bes-Rastrollo and Basterra-Gortari 8 ) and the Pizarra study( Reference Soriguer, Almaraz and García-Almeida 9 ), most people in Spain use olive oil for frying at home. In contrast, the most common oil used for frying away from home, especially in fast-food restaurants, is maize oil( Reference Jahren and Schubert 10 ).
Frequent fried food consumption has been reported to be associated with a higher risk of overweight/obesity in Spain( Reference Sayon-Orea, Bes-Rastrollo and Basterra-Gortari 8 , Reference Guallar-Castillón, Rodríguez-Artalejo and Fornés 11 ). This association together with some biological mechanisms (trans-fatty acids produced during the frying process may cause an impaired endothelial function, which will increase blood pressure)( Reference Gerber, Holemans and O'Brien Coker 12 ) make it likely that fried food consumption might also be associated with a higher risk of hypertension. Evidence from epidemiological studies linking fried food consumption and hypertension is scarce and inconsistent. A cross-sectional study conducted in Spain has found that a high prevalence of hypertension is associated with the consumption of fried foods (especially when these foods are fried with reused vegetable oils such as sunflower oil)( Reference Soriguer, Rojo-Martnez and Dobarganes 13 ). More evidence exists on the association between the consumption of fried foods and the risk of CVD. However, results of studies on the association between the consumption of fried foods and the risk of CVD are inconsistent: one case–control study( Reference Iqbal, Anand and Ounpuu 14 ) and one cohort study( Reference Mozaffarian, Lemaitre and Kuller 15 ) have found a positive association, while another cohort study( Reference Guallar-Castillon, Rodriguez-Artalejo and Lopez Garcia 16 ) and a case–control study( Reference Kabagambe, Baylin and Siles 17 ) have reported no association. It is widely known that unhealthy lifestyle factors such as overweight/obesity, physical inactivity, alcohol intake and smoking status, among others, cause high blood pressure( Reference Gu, Wildman and Wu 18 ). In one clinical trial, changes in unhealthy cooking habits (e.g. changing the cooking method from frying to boiling, among others) have been found to be beneficial for controlling blood pressure and obesity in the general population( Reference Kisioglu, Aslan and Ozturk 19 ).
There are no published results from large prospective studies that have assessed the role of fried food consumption in the development of hypertension. Therefore, the aim of the present study was to prospectively evaluate the potential association between the consumption of fried foods and the risk of hypertension in a Mediterranean cohort.
Subjects and methods
Study population
The SUN project is a Spanish, multi-purpose, dynamic and prospective cohort study that was designed to assess associations between diet and the occurrence of several diseases and chronic conditions including hypertension( Reference Segui-Gomez, de la Fuente and Vazquez Zenaida 20 ). All participants included in the study are university graduates. They are followed up every 2 years by mailed questionnaires. The recruitment of participants started in December 1999, and it is permanently open. Detailed information about the design and methods of the SUN project has been published elsewhere( Reference Segui-Gomez, de la Fuente and Vazquez Zenaida 20 ). Up to September 2009, 20 335 participants had been recruited. We excluded 2283 participants with prevalent hypertension; 1747 participants who reported values for total energy intake at baseline outside the predefined limits ( < 3347 kJ/d (800 kcal/d) in men and < 2092 kJ/d (500 kcal/d) in women or >16 736 kJ/d (4000 kcal/d) in men and >14 644 kJ/d (3500 kcal/d) in women)( Reference Willett, Stampfer and Willett 21 ); 1251 participants with chronic diseases at baseline (including cancer, diabetes or CVD); 1178 participants without any follow-up who were considered to be lost to follow-up (retention rate: 92 %); and 197 participants with missing values for variables of interest, leaving a total of 13 679 participants available for the final analysis (Fig. 1).

Fig. 1 Flowchart of participant recruitment: the SUN (Seguimiento Universidad de Navarra) project (1999–2012).
The Institutional Review Board of the University of Navarra approved the study. Voluntary completion of the first self-administered questionnaire was considered to indicate informed consent.
Dietary intake assessment
A previously validated 136-item semi-quantitative FFQ measuring participants' food intake in the previous year was included in the baseline questionnaire( Reference Martín-Moreno, Boyle and Gorgojo 22 ). Nutrient scores were calculated as frequency multiplied by the nutrient composition of specified portion sizes. For each food item, consumption frequencies were divided into nine categories (ranging from never/almost never, with almost never indicating that the specific item was consumed less than ‘once per month’, to >6 servings/d). The frequency of fried food consumption was evaluated by taking the following items into account: the consumption of fried foods at home and the consumption of fried foods away from home. The total consumption of fried foods per person was estimated using the sum of these two items. In addition, the total amount of fried foods consumed in grams was estimated by adding the proportion of fried foods consumed from the rest of the items in the FFQ. The proportion of consumption as a fried food according to typical Spanish culinary practices was multiplied by the frequency reported in the questionnaire (i.e. if the participant reported that he/she ate one portion of fried potatoes, the proportion of consumption was multiplied by one; on the other hand, if the participant reported that he/she ate one portion of meat, it was multiplied by 0·5 because we assumed that meat is consumed as a fried food half the time, taking into account the typical culinary practices in Spain). This approach has been used successfully in a previous study of the SUN cohort( Reference Sayon-Orea, Bes-Rastrollo and Basterra-Gortari 8 ). Finally, an additional question, ‘what kind of fat do you use at home to fry?’, was also included in the baseline questionnaire to determine whether the participants fried foods with olive oil or a different kind of oil. The nutrient databank was updated by a trained team of dietitians using the information available for food composition tables for Spain( Reference Moreiras, Carbajal, Cabrera, Moreiras, Carbajal, Cabrera and Cuadrado 23 ).
Assessment of non-dietary variables
Other questions (forty-six items for men and fifty-four items for women) were also included in the baseline questionnaire to assess participants' medical history, health-related habits, lifestyle, and sociodemographic variables, as well as anthropometric data (weight and height were validated previously in a subsample of the cohort)( Reference Bes-Rastrollo, Pérez-Valdivieso and Sanchez-Villegas 24 ). At baseline, the participants were queried about seventeen activities to quantify their physical activity levels, and from them a metabolic equivalent index (MET-h/week) was computed. Physical activity had also been validated previously in a subsample of the cohort( Reference Martinez-Gonzalez, López-Fontana and Varo 25 ).
Ascertainment of hypertension
The endpoint of the study was incident hypertension. The participants were asked whether they had received a medical diagnosis of hypertension at baseline and during the follow-up period and also about the date of diagnosis.
For the present analysis, the participants were considered to have prevalent hypertension at baseline if they reported a medical diagnosis of hypertension, systolic blood pressure ≥ 140 mmHg, diastolic blood pressure ≥ 90 mmHg, or use of any antihypertensive medication( Reference Chobanian, Bakris and Black 26 ). New cases of hypertension were defined as those participants who did not have hypertension at baseline and reported a new medical diagnosis of hypertension during the follow-up period. The validity of self-reported hypertension diagnosis was assessed in a subsample of the cohort. This validation study showed an adequate validity of the self-reported diagnosis of hypertension: among participants who reported a diagnosis of hypertension, 82·3 % (95 % CI 72·8, 92·8) were confirmed as hypertensive through conventional measurement of blood pressure, and among those who did not report a diagnosis of hypertension, 85·4 % (95 % CI 72·4, 89·1) were confirmed as non-hypertensive( Reference Alonso, Beunza and Delgado-Rodriguez 27 ). Moreover, in a recent study, we have validated each component of the metabolic syndrome (including high blood pressure) and found an intra-class correlation coefficient of 0·47 (0·36–0·57) for systolic blood pressure and of 0·46 (0·34–0·56) for diastolic blood pressure, using direct assessments by an experienced physician as the gold standard( Reference Fernandez-Montero, Beunza and Bes Rastrollo 28 ).
Statistical analyses
The participants were classified into three categories according to the distribution of their frequencies of fried food consumption: 0–2; >2–4; >4 times/week. The participants were also classified into tertiles of total fried food consumption (g/d) (details regarding food items and serving sizes of fried foods considered in the FFQ are given in an online supplemental table). The group with the lowest frequency of fried food consumption ( < 2 times/week) or in the lowest tertile was considered as the reference category. In an additional analysis, the participants were classified into the following four categories: 0–2; >2–4; >4– < 7; ≥ 7 times/week, considering the group with the lowest frequency of fried food consumption again as the reference category.
Nutrient intake was adjusted for total energy intake with the residuals methods, and separate regression models were used to obtain sex-specific residuals.
Person-time of follow-up was calculated for each participant, from the date of completion of the baseline questionnaire to the date of completion of the last follow-up questionnaire, the date of diagnosis of hypertension or death, whichever occurred first.
Cox regression models were used to assess the association between the consumption of fried foods at baseline and the subsequent risk of developing incident hypertension during the follow-up period. Tests of linear trend across increasing categories of fried food consumption were conducted by assigning medians for the frequency of fried food consumption within each category and treating this as a continuous variable.
The association between home and non-home fried food consumption separately and the risk of hypertension was also examined.
Interactions between age categories ( < 40 and ≥ 40 years), sex and the frequency of fried food consumption were calculated using likelihood ratio tests between the fully adjusted models and the same model, but by introducing the interaction product term. The interaction between the type of fat used for frying (olive oil or others) and the frequency of fried food consumption was also tested.
For all the analyses, a crude univariate model, an age- and sex-adjusted model, and two multivariable models were used after additional adjustment for the following potential confounders: model 1 – family history of hypertension (yes/no), self-reported history of hypercholesterolaemia (yes/no), physical activity (MET-h/week), smoking status (non-smoker, current smoker and former smoker), total energy intake (kcal/d), alcohol intake (g/d), and energy-adjusted Na (mg/d), K (mg/d), caffeine (mg/d), fibre (g/d), olive oil (g/d), fruit (g/d), vegetable (g/d), low-fat and high-fat dairy product, sugar-sweetened beverage (ml/d), fast food (g/d), and sweet (g/d) consumption, and time spent watching television (h/d) and model 2 – additionally adjusted for baseline BMI. For the selection of potential confounders in the multivariate model, and as currently recommended( Reference Hernán, Hernández-Díaz and Werler 29 ), the previously published scientific literature, including our own results based on the cohort regarding risk factors for hypertension, was taken into account, avoiding exclusively the statistical approach with the P value, the stepwise procedures or the changes in point estimates after adjusting for potential confounders.
To account for multicollinearity across independent variables, a statistical model was constructed and the variance inflation factor was calculated.
Sensitivity analyses were conducted, and all the models were used after (1) excluding early cases of incident hypertension (cases reported within the first 2 years of follow-up), (2) excluding late cases of hypertension (cases reported after ≥ 8 years of follow-up), (3) excluding participants who reported incident chronic diseases during the follow-up period, (4) excluding participants who were under the 5th percentile and over the 95th percentile of total energy intake, (5) excluding participants who did not answer nine or more items in the FFQ, and (6) including participants who reported systolic blood pressure ≥ 140 and/or diastolic blood pressure ≥ 90 at baseline. Finally, an additional analysis was conducted, adjusting for the calendar year of participant's inclusion in the cohort.
All P values presented are two-tailed; P< 0·05 was considered statistically significant. The analyses were carried out using Stata/SE version 12.0 (StataCorp).
Results
A total of 5059 men and 8620 women were included in the present study. The main baseline characteristics of the participants according to their frequency of fried food consumption are given in Table 1. The mean age of the participants was 36·5 (sd 10·8) years and the mean BMI was 23·2 (sd 3·3) kg/m2. Participants in the highest category of baseline fried food consumption (>4 times/week) compared with those in the lowest category ( ≤ 2 times/week) had a higher BMI, were less physically active, were more likely to have a history of hypercholesterolaemia, but less likely to have a family history of hypertension, had higher total energy and fat intake, lower protein and carbohydrate intake, higher Na, Mg and caffeine intake, but lower fibre, fruit, vegetable and low-fat dairy product intake, and had higher means of baseline systolic blood pressure and diastolic blood pressure.
Table 1 Baseline characteristics of the participants according to their frequency of fried food consumption (the SUN (Seguimiento Universidad de Navarra) cohort, 1999–2012) (Mean values, standard deviations and percentages)

BP, blood pressure; MET, metabolic equivalents; TV, television.
During the follow-up period (median of 6·3 years), we identified 1232 incident cases of hypertension. A higher frequency of fried food consumption was positively associated with a higher risk of developing hypertension. Participants consuming fried foods >2–4 and >4 times/week exhibited a significantly greater risk of developing hypertension compared with those consuming fried foods 0–2 times/week (hazard ratio (HR) = 1·18, 95 % CI 1·03, 1·36 and HR = 1·21, 95 % CI 1·04, 1·41, respectively; P for trend = 0·009), after adjusting for potential confounders (Table 2). When analysing total fried food consumption (g/d) in tertiles, we observed a HR of 1·04 (95 % CI 0·90, 1·20) for the second tertile and a HR of 1·18 (95 % CI 1·00, 1·38) for the third tertile v. the first tertile of consumption in the fully adjusted models (data not shown). The Pearson correlation coefficient between the frequency of fried food consumption and total fried food consumption in grams was r 0·912 (P< 0·001). When analysing the four categories of consumption, we also observed a greater risk in the highest category ( ≥ 7 times/week) in comparison with the lowest category (HR = 1·20, 95 % CI 1·00, 1·45; P for trend = 0·017) (data not shown).
Table 2 Cox proportional hazard ratios (HR) of incident hypertension according to the baseline frequency of fried food consumption in 13 679 participants of the SUN (Seguimiento Universidad de Navarra) project (1999–2012) (Hazard ratios and 95 % confidence intervals)
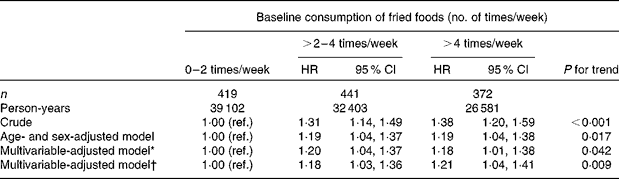
ref., Reference.
* Adjusted for sex, age, family history of hypertension, self-reported hypercholesterolaemia, physical activity, smoking status, total energy intake, alcohol intake, energy-adjusted Na, K, caffeine, fibre, olive oil, fruit, vegetable, low-fat and high-fat dairy product, sugar-sweetened beverage, fast food, and sweet consumption, and time spent watching television.
† Additionally adjusted for baseline BMI.
As we thought that the intake of this type of food might change over time and/or over the study period (i.e. early v. late entry into the dynamic cohort), we conducted an additional analysis adjusting for the calendar year of participant's inclusion in the cohort. We observed that the HR were attenuated, but remained statistically significant at 1·15 (95 % CI 1·00, 1·31) and 1·16 (95 % CI 1·01, 1·34) for those consuming fried foods >2–4 times/week and >4 v. < 2 times/week, respectively.
When analysing the frequency of fried food consumption at home and away from home, we obtained very similar results for both groups. We observed a HR of 1·16 for those consuming fried foods at home >2 times/week (95 % CI 1·03, 1·32) and a HR of 1·15 for those consuming fried foods away from home (95 % CI 0·97, 1·38) (Table 3).
Table 3 Cox proportional hazard ratios (HR) of incident hypertension according to the baseline frequency of fried food consumption, stratified according to fried food consumption at home or away from home (Hazard ratios and 95 % confidence intervals)
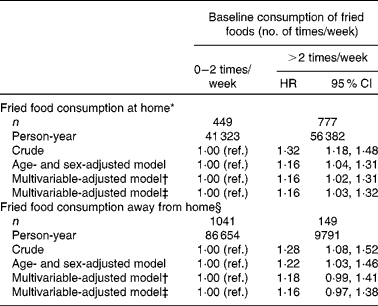
ref., Reference.
* We included 13 629 participants in this analysis (fifty participants excluded due to missing information for this variable) and we identified 1226 incident cases of hypertension.
† Adjusted for sex, age, family history of hypertension, self-reported hypercholesterolaemia, physical activity, smoking status, total energy intake, alcohol intake, energy-adjusted Na, K, caffeine, fibre, olive oil, fruit, vegetable, low-fat and high-fat dairy product, sugar-sweetened beverage, fast food, and sweet consumption, and time spent watching television.
‡ Additionally adjusted for baseline BMI.
§ We included 13 453 participants in this analysis (226 participants were excluded due to missing information for this variable) and we identified 1190 incident cases of hypertension.
The interactions between fried food consumption and age, sex and type of oil used for frying were not statistically significant (P for interaction = 0·711, 0·567 and 0·870, respectively).
We conducted multiple sensitivity analyses to account for the potential uncertainties of our assumptions regarding the induction period and also for possible sources of bias including measurement errors. In all these sensitivity analyses, the results were not meaningfully altered (Table 4).
Table 4 Cox model multivariate-adjusted hazard ratios (HR) of hypertension associated with the highest category (>4 times/week) of fried food consumption in sensitivity analyses, taking the group with the lowest frequency of fried food consumption as the reference category (<2 times/week) (Hazard ratios and 95 % confidence intervals)

SBP, systolic blood pressure; DBP, diastolic blood pressure.
* Adjusted for sex, age, baseline BMI, family history of hypertension, self-reported hypercholesterolaemia, total energy intake, smoking status, alcohol intake, energy-adjusted Na, K, caffeine, fibre, olive oil, fruit, vegetable, low-fat and high-fat dairy product consumption, sugar-sweetened beverage, fast food, and sweet consumption, and time spent watching television.
When testing for multicollinearity, we found variance inflation factor values to be satisfactory.
Discussion
Higher baseline consumption of fried foods was found to be significantly associated with a higher risk of incident hypertension in the Mediterranean cohort studied.
A previous cross-sectional study carried out in Spain including 538 participants( Reference Soriguer, Rojo-Martnez and Dobarganes 13 ) has evaluated the association between the consumption of fried foods and the prevalence of hypertension and found the risk of hypertension to be directly associated with the consumption of fried foods, especially on reusing vegetable oils such as sunflower oil ( Reference Soriguer, Rojo-Martnez and Dobarganes 13 ). Some studies have evaluated the association between the consumption of fried foods and the risk of CVD with inconsistent results( Reference Iqbal, Anand and Ounpuu 14 – Reference Kabagambe, Baylin and Siles 17 ). The Spanish EPIC cohort study, conducted in 40 757 adults aged 29–69 years, free of CHD at baseline, found that the consumption of fried foods was not associated with the risk of CHD with a HR of 1·08 (95 % CI 0·82, 1·43) for the fourth quartile of consumption in comparison with the first quartile( Reference Guallar-Castillon, Rodriguez-Artalejo and Lopez Garcia 16 ). Similarly, a case–control study carried out in Costa Rica found no association between the consumption of fried foods and the risk of myocardial infarction( Reference Kabagambe, Baylin and Siles 17 ). Conversely, the large INTERHEART case–control study observed a positive association between the consumption of fried foods and the risk of acute myocardial infarction( Reference Iqbal, Anand and Ounpuu 14 ). The Cardiovascular Heart Study found fried fish consumption to exhibit a non-significant trend towards a higher risk( Reference Mozaffarian, Lemaitre and Kuller 15 ).
The frying process involves many factors, some dependent on the process itself and others on the food and type of fat used( Reference Saguy and Pinthus 7 ). For example, during the frying process, the amount of trans-fatty acids in foods increases. The amount of trans-fatty acids generated depends on several aspects such as the frying technique (deep frying or pan frying), the type of oil and food used, and the degree of degradation of the oil( Reference Boskou, Salta and Chiou 6 ). In one large American cohort that included 28 100 women aged ≥ 39 years and free of CVD and cancer at baseline, Wang et al. ( Reference Wang, Manson and Forman 30 ) found a higher intake of trans-fatty acids to be associated with an increased risk of hypertension. Therefore, this mechanism may account for the association found in the present study. Another plausible mechanism involved in the association between fried food consumption and hypertension risk might be explained by the weight gained during the follow-up period due to fried food consumption. A previous study carried out in our cohort has shown a significant positive association between high frequency of fried food consumption and the risk of overweight/obesity( Reference Sayon-Orea, Bes-Rastrollo and Basterra-Gortari 8 ). The association between hypertension and obesity is widely known( Reference Landsberg, Aronne and Beilin 31 ). In this context, we conducted a secondary analysis, additionally adjusting for incident obesity (yes/no). We found the risk estimate to be attenuated and the association between fried food consumption (>4 v. ≤ 2 times/week) and hypertension risk to be non-significant (HR = 1·15, 95 % CI 0·97, 1·36). Similar results were obtained when we adjusted for yearly body weight change (HR = 1·14, 95 % CI, 0·96, 1·46). Therefore, incident obesity and yearly body weight change might be mediators in the causal chain, and this is likely to act as one of the potential mechanisms that might explain the association between the consumption of fried foods and the incidence of hypertension.
A potential limitation of the present study is the self-reported outcome. However, a self-reported diagnosis of hypertension has been validated previously in our cohort and a fairly adequate validity for the self-reported diagnosis of hypertension found( Reference Alonso, Beunza and Delgado-Rodriguez 27 , Reference Fernandez-Montero, Beunza and Bes Rastrollo 28 ).
Another limitation could be that the participants might have under-reported their fried food consumption because they perceived it as unhealthy (social desirability bias); however, this misclassification is expected to be non-differential and therefore could more likely bias the results of the present study to the null value( Reference Rothman, Greenland and Lash 32 ).
The present study also has important strengths, including its prospective design, which avoids the possibility of reverse causation bias. Other strengths are the use of a validated FFQ( Reference Martín-Moreno, Boyle and Gorgojo 22 ), the large sample size and the long follow-up period.
Inclusion of only university graduates might be a potential limitation of the present study, because it is not a representative sample. This might have affected the generalisability of our findings; therefore, we have to be cautious while extrapolating the results of the present study to the general population. Nevertheless, it could also have actually enhanced the internal validity of the present study because the high level of education and homogeneity of the cohort reduced the potential confounding related to socio-economic status. However, the generalisability of our findings, to some other important cohort, must be based on biological mechanisms and not on the representativeness of the study sample in the statistical sense of the term. In addition, the high educational level of the study participants helped us obtain better-quality information and increased the internal validity of the study.
In conclusion, more frequent consumption of fried foods at baseline was found to be associated with a higher risk of developing hypertension during the follow-up period in a Mediterranean cohort of university graduates.
Supplementary material
To view supplementary material for this article, please visit http://dx.doi.org/10.1017/S00071145140001755
Acknowledgements
The authors thank all the participants of the SUN project for their continued cooperation and participation. They also thank all the members of the SUN project for administrative, technical and material support.
The SUN study has received funding from the Spanish Government (grant nos. PI01/0619, PI030678, PI040233, PI042241, PI050976, PI070240, PI070312, PI081943, PI080819, PI1002658, PI1002293, RD06/0045, G03/140 and 87/2010), the Navarra Regional Government (36/2001, 43/2002, 41/2005, 36/2008, 45/2011), and the University of Navarra. A. G. is supported by a FPU fellowship of the ‘Ministerio de Educación, Cultura y Deporte’, from the Spanish Government.
The authors' contributions are as follows: M. A. M.-G. helped design the study and collected the data; M. B.-R. and C. S.-O. analysed the data and drafted the manuscript; A. G., I. Z., F. J. B.-G. edited and critically reviewed the manuscript.
None of the authors has any conflicts of interest to declare.









