13 results
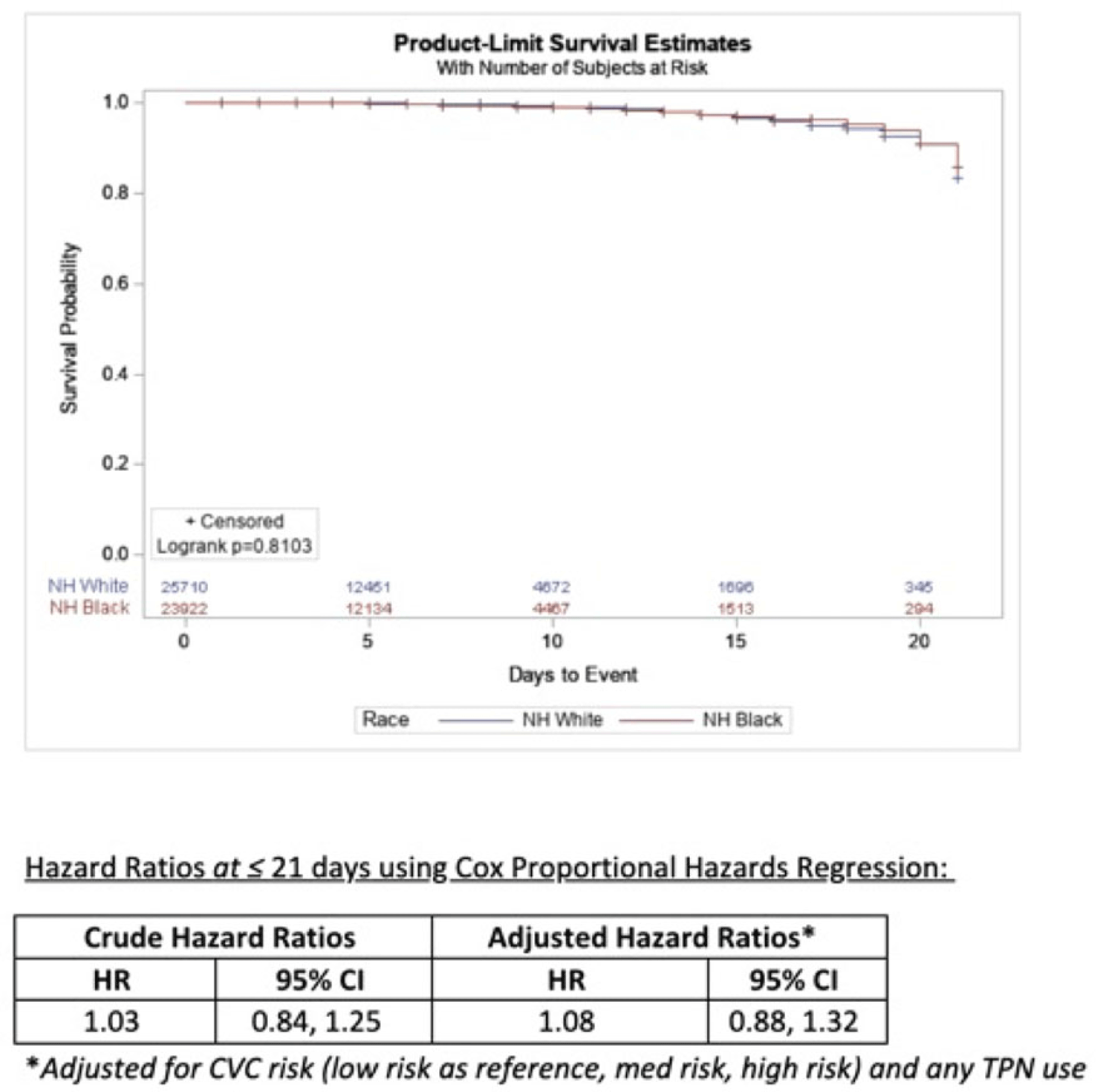
Estimating racial differences in risk for CLABSI in a large urban healthcare system
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s50-s51
-
- Article
-
- You have access
- Open access
- Export citation
Determinates of Clostridioides difficile infection (CDI) testing practices among inpatients with diarrhea at selected acute-care hospitals in Rochester, New York, and Atlanta, Georgia, 2020–2021
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 7 / July 2023
- Published online by Cambridge University Press:
- 14 September 2022, pp. 1085-1092
- Print publication:
- July 2023
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
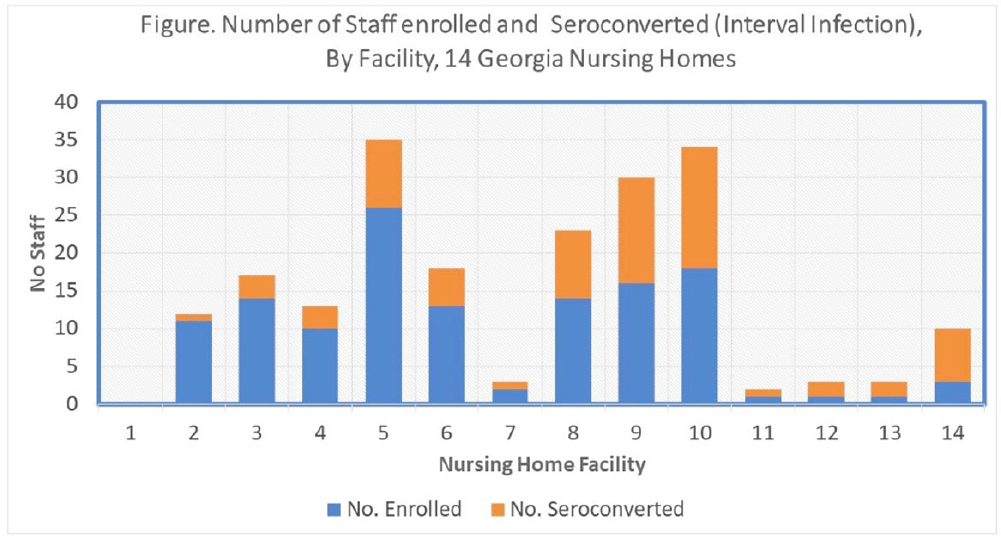
Which nursing home workers were at highest risk for SARS-CoV-2 infection during the November 2020–February 2021 winter surge of COVID-1?
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, p. s7
-
- Article
-
- You have access
- Open access
- Export citation
Occupational risk factors for severe acute respiratory coronavirus virus 2 (SARS-CoV-2) infection among healthcare personnel: A 6-month prospective analysis of the COVID-19 Prevention in Emory Healthcare Personnel (COPE) Study
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 43 / Issue 11 / November 2022
- Published online by Cambridge University Press:
- 14 February 2022, pp. 1664-1671
- Print publication:
- November 2022
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Risk factors for severe acute respiratory coronavirus virus 2 (SARS-CoV-2) seropositivity among nursing home staff
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue 1 / 2021
- Published online by Cambridge University Press:
- 28 October 2021, e35
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Occupational risk factors for severe acute respiratory coronavirus virus 2 (SARS-CoV-2) infection among healthcare personnel: A cross-sectional analysis of subjects enrolled in the COVID-19 Prevention in Emory Healthcare Personnel (COPE) study
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 43 / Issue 3 / March 2022
- Published online by Cambridge University Press:
- 09 February 2021, pp. 381-386
- Print publication:
- March 2022
-
- Article
-
- You have access
- HTML
- Export citation
A Portable, Easily Deployed Approach to Measure Healthcare Professional Contact Networks in Long-Term Care Settings
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, p. s455
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Evaluation of Care Interactions Between Healthcare Personnel and Residents in Nursing Homes Across the United States
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s36-s38
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
The Second Central Line Increases Central-Line–Associated Bloodstream Infection Risk by 80%: Implications for Inpatient Quality Reporting Programs
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s499-s500
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Variation in Measures of Antimicrobial Use Across Four Nursing Homes, Atlanta, Georgia, 2019
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, p. s510
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Variations in Concurrent Central-Line Use Among Central-Line–Associated Bloodstream Infection (CLABSI) Patients by National Healthcare Safety Network (NHSN) Location Type
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, p. s511
- Print publication:
- October 2020
-
- Article
-
- You have access
- Export citation
Behavioral momentum and multiple stimulus control topographies
-
- Journal:
- Behavioral and Brain Sciences / Volume 23 / Issue 1 / February 2000
- Published online by Cambridge University Press:
- 28 September 2001, p. 109
-
- Article
- Export citation
8 - Sex, Dating, Passionate Friendships, and Romance: Intimate Peer Relations Among Lesbian, Gay, and Bisexual Adolescents
-
-
- Book:
- The Development of Romantic Relationships in Adolescence
- Published online:
- 05 October 2014
- Print publication:
- 13 September 1999, pp 175-210
-
- Chapter
- Export citation