61 results
Diagnostic stewardship to improve patient outcomes and healthcare-associated infection (HAI) metrics
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 45 / Issue 4 / April 2024
- Published online by Cambridge University Press:
- 11 January 2024, pp. 405-411
- Print publication:
- April 2024
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Diagnostic stewardship and the coronavirus disease 2019 (COVID-19) pandemic: Lessons learned for prevention of emerging infectious diseases in acute-care settings
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 45 / Issue 3 / March 2024
- Published online by Cambridge University Press:
- 07 November 2023, pp. 277-283
- Print publication:
- March 2024
-
- Article
-
- You have access
- HTML
- Export citation
Introduction to A Compendium of Strategies to Prevent Healthcare-Associated Infections In Acute-Care Hospitals: 2022 Updates
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 10 / October 2023
- Published online by Cambridge University Press:
- 19 October 2023, pp. 1533-1539
- Print publication:
- October 2023
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Improving antimicrobial use through better diagnosis: The relationship between diagnostic stewardship and antimicrobial stewardship
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 12 / December 2023
- Published online by Cambridge University Press:
- 04 September 2023, pp. 1901-1908
- Print publication:
- December 2023
-
- Article
-
- You have access
- HTML
- Export citation
Impact of measurement and feedback on chlorhexidine gluconate bathing among intensive care unit patients: A multicenter study
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 9 / September 2023
- Published online by Cambridge University Press:
- 13 September 2023, pp. 1375-1380
- Print publication:
- September 2023
-
- Article
- Export citation
Executive Summary: A Compendium of Strategies to Prevent Healthcare-Associated Infections in Acute-Care Hospitals: 2022 Updates
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 10 / October 2023
- Published online by Cambridge University Press:
- 22 August 2023, pp. 1540-1554
- Print publication:
- October 2023
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Principles of diagnostic stewardship: A practical guide from the Society for Healthcare Epidemiology of America Diagnostic Stewardship Task Force
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 2 / February 2023
- Published online by Cambridge University Press:
- 14 February 2023, pp. 178-185
- Print publication:
- February 2023
-
- Article
-
- You have access
- HTML
- Export citation
Asymptomatic screening for severe acute respiratory coronavirus virus 2 (SARS-CoV-2) as an infection prevention measure in healthcare facilities: Challenges and considerations
- Part of
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 1 / January 2023
- Published online by Cambridge University Press:
- 21 December 2022, pp. 2-7
- Print publication:
- January 2023
-
- Article
-
- You have access
- HTML
- Export citation
Multicenter evaluation of contamination of the healthcare environment near patients with Candida auris skin colonization – ERRATUM
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue 1 / 2022
- Published online by Cambridge University Press:
- 07 October 2022, e166
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
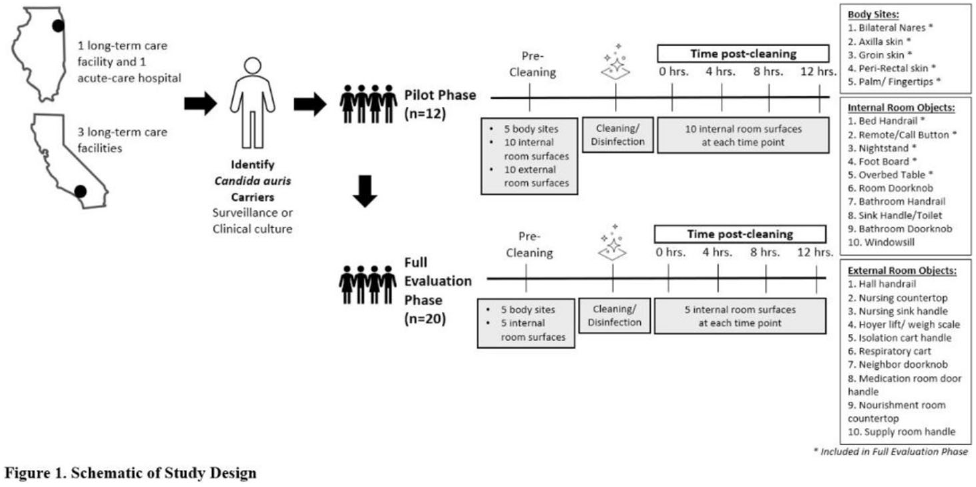
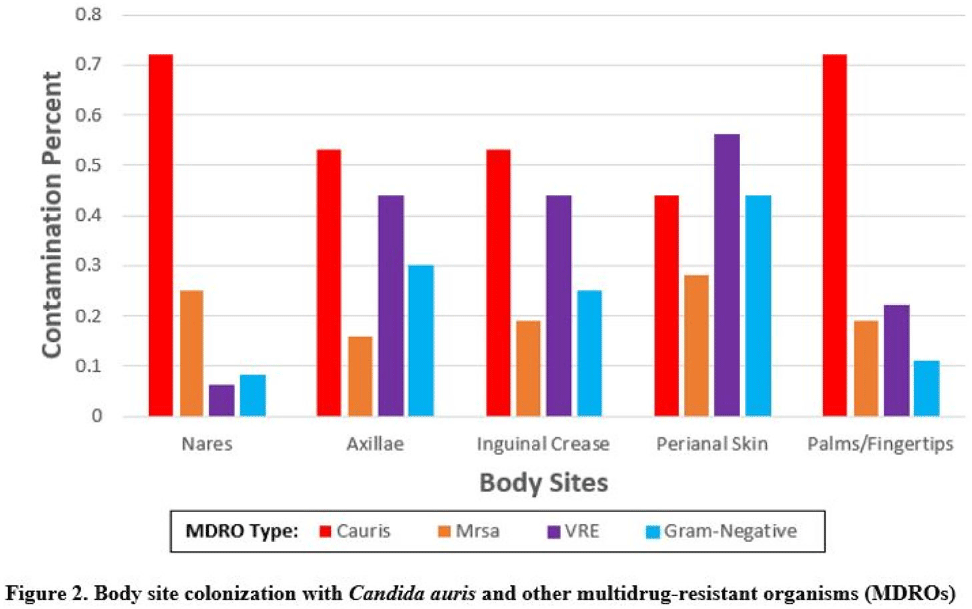
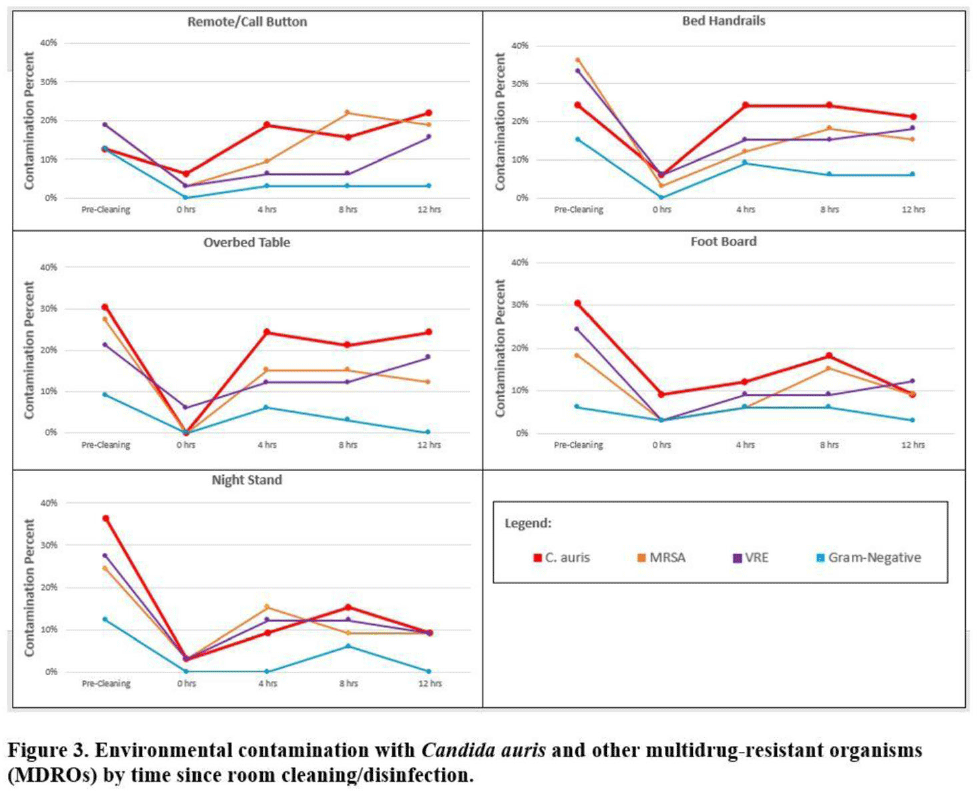
Multicenter evaluation of contamination of the healthcare environment near patients with Candida auris skin colonization
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, pp. s78-s79
-
- Article
-
- You have access
- Open access
- Export citation
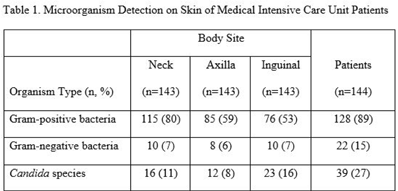
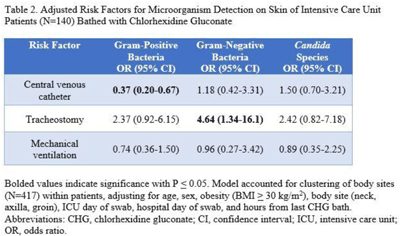
Indwelling medical devices and skin microorganisms on ICU patients bathed with chlorhexidine gluconate
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, pp. s43-s44
-
- Article
-
- You have access
- Open access
- Export citation
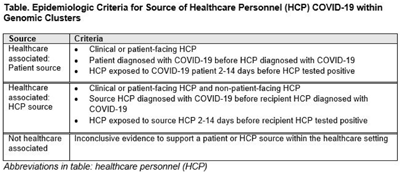
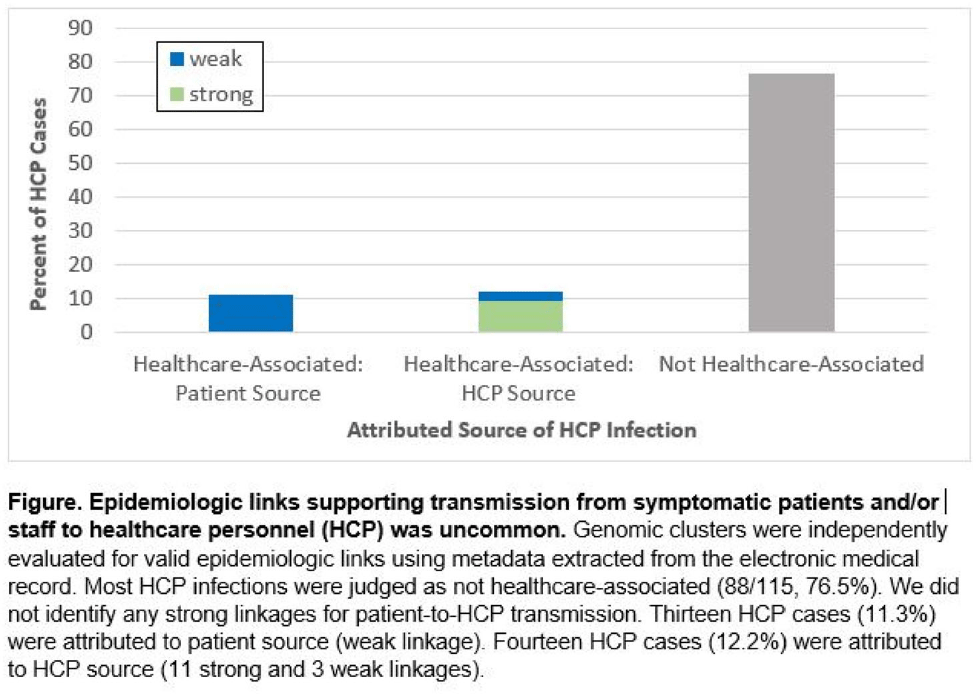
Genomic investigation to identify the source of SARS-CoV-2 infection among healthcare personnel
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, pp. s74-s75
-
- Article
-
- You have access
- Open access
- Export citation
Adapting and thriving, the Association for Professionals in Infection Control and Epidemiology (APIC) and the Society for Healthcare Epidemiology of America (SHEA) partnership
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 42 / Issue 12 / December 2021
- Published online by Cambridge University Press:
- 21 December 2021, p. 1421
- Print publication:
- December 2021
-
- Article
-
- You have access
- HTML
- Export citation
Whole-genome sequencing for neonatal intensive care unit outbreak investigations: Insights and lessons learned – ADDENDUM
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue 1 / 2021
- Published online by Cambridge University Press:
- 03 August 2021, e18
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
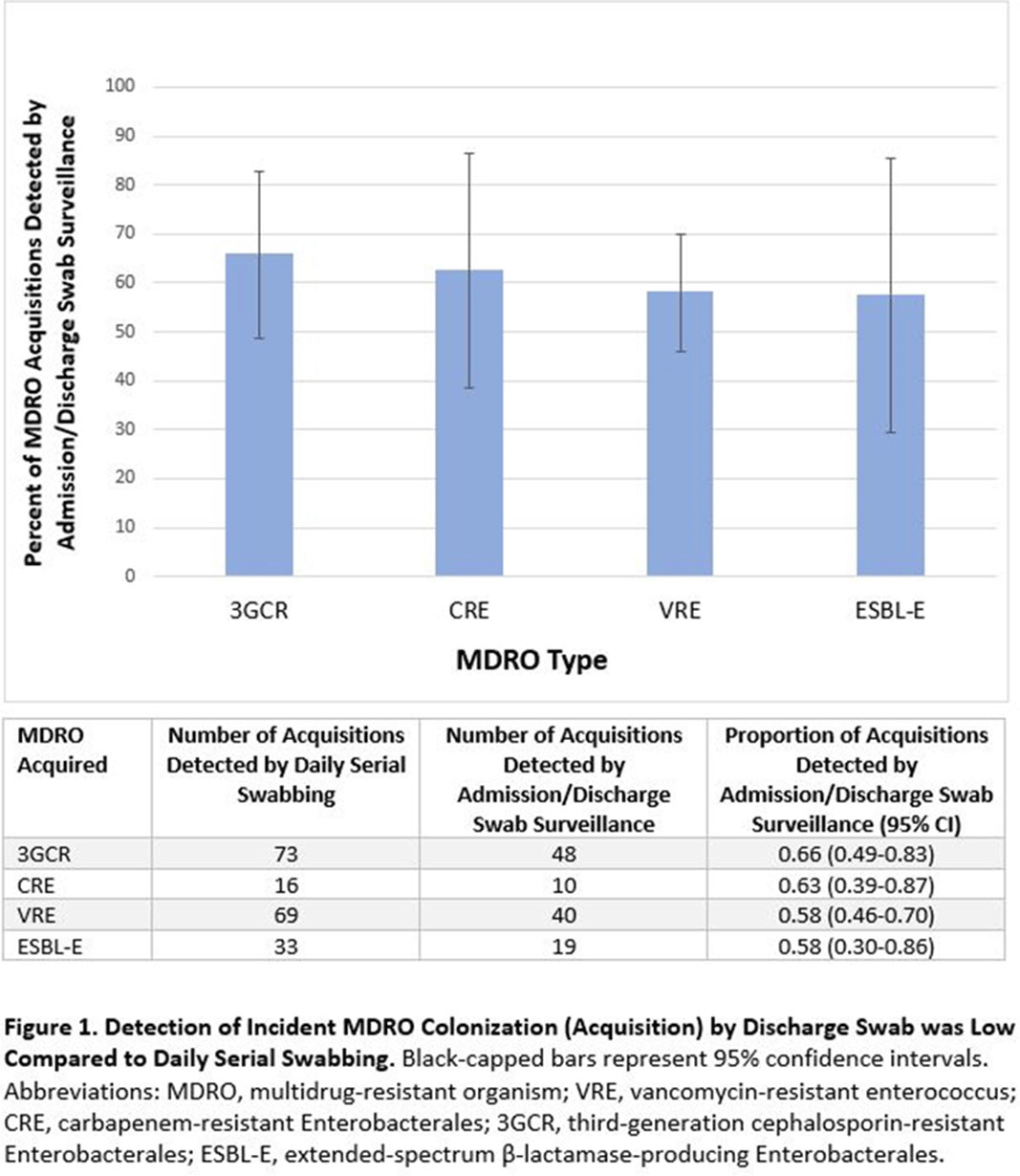
Admission and Discharge Sampling Underestimates Multidrug-Resistant Organism (MDRO) Acquisition in an Intensive Care Unit
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue S1 / July 2021
- Published online by Cambridge University Press:
- 29 July 2021, p. s28
-
- Article
-
- You have access
- Open access
- Export citation
Pediatric antimicrobial stewardship practices at discharge: A national survey
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 43 / Issue 11 / November 2022
- Published online by Cambridge University Press:
- 16 July 2021, pp. 1686-1688
- Print publication:
- November 2022
-
- Article
- Export citation
Whole-genome sequencing for neonatal intensive care unit outbreak investigations: Insights and lessons learned
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue 1 / 2021
- Published online by Cambridge University Press:
- 24 June 2021, e2
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Healthcare personnel experiences implementing carbapenem-resistant Enterobacterales infection control measures at a ventilator-capable skilled nursing facility—A qualitative analysis
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 43 / Issue 8 / August 2022
- Published online by Cambridge University Press:
- 21 June 2021, pp. 1010-1016
- Print publication:
- August 2022
-
- Article
- Export citation
Assessing the healthcare epidemiology environment—A roadmap for SHEA’s future
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 42 / Issue 9 / September 2021
- Published online by Cambridge University Press:
- 18 June 2021, pp. 1111-1114
- Print publication:
- September 2021
-
- Article
- Export citation
Local, state and federal face mask mandates during the COVID-19 pandemic
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 42 / Issue 4 / April 2021
- Published online by Cambridge University Press:
- 05 January 2021, pp. 455-456
- Print publication:
- April 2021
-
- Article
-
- You have access
- Open access
- HTML
- Export citation