70 results
Patterns, predictors, and patient-reported reasons for antidepressant discontinuation in the WHO World Mental Health Surveys
-
- Journal:
- Psychological Medicine / Volume 54 / Issue 1 / January 2024
- Published online by Cambridge University Press:
- 14 September 2023, pp. 67-78
-
- Article
- Export citation
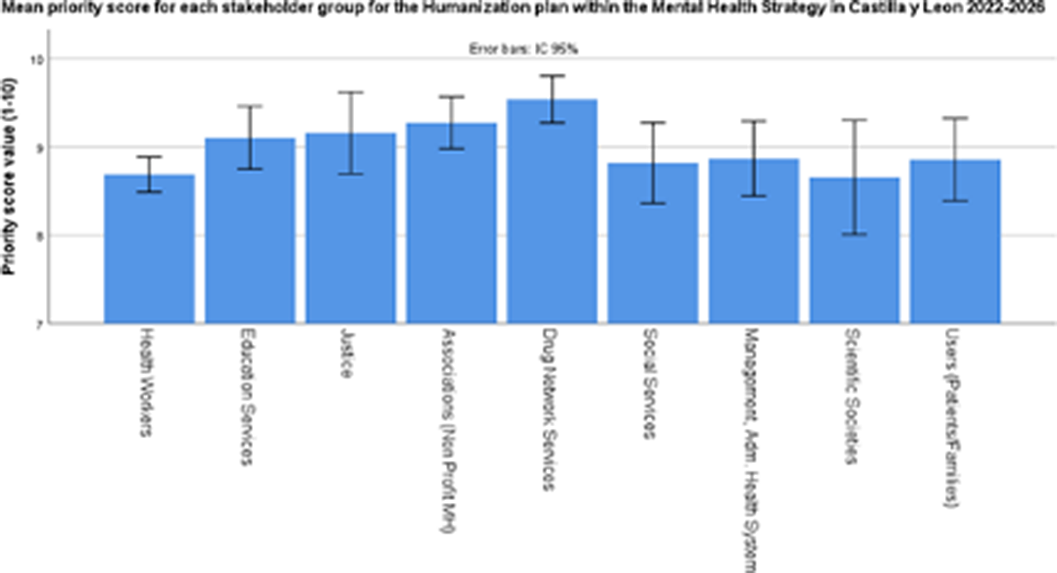
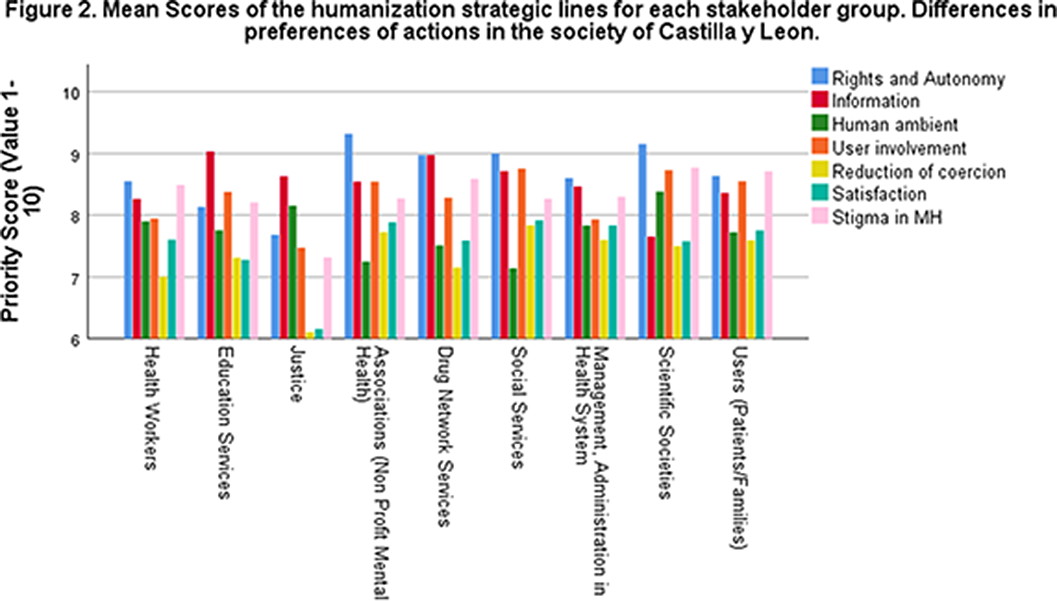
A social consensus to prioritize humanization strategies for Mental Health in Castilla y León
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S908-S909
-
- Article
-
- You have access
- Open access
- Export citation
218 Researcher and Stakeholder Partner Perspectives on Engaged Research During the COVID-19 Pandemic
- Part of
-
- Journal:
- Journal of Clinical and Translational Science / Volume 7 / Issue s1 / April 2023
- Published online by Cambridge University Press:
- 24 April 2023, pp. 66-67
-
- Article
-
- You have access
- Open access
- Export citation
A pilot study to develop an assessment tool for sheep welfare after long journey transport
-
- Journal:
- Animal Welfare / Volume 24 / Issue 4 / November 2015
- Published online by Cambridge University Press:
- 01 January 2023, pp. 407-416
-
- Article
- Export citation
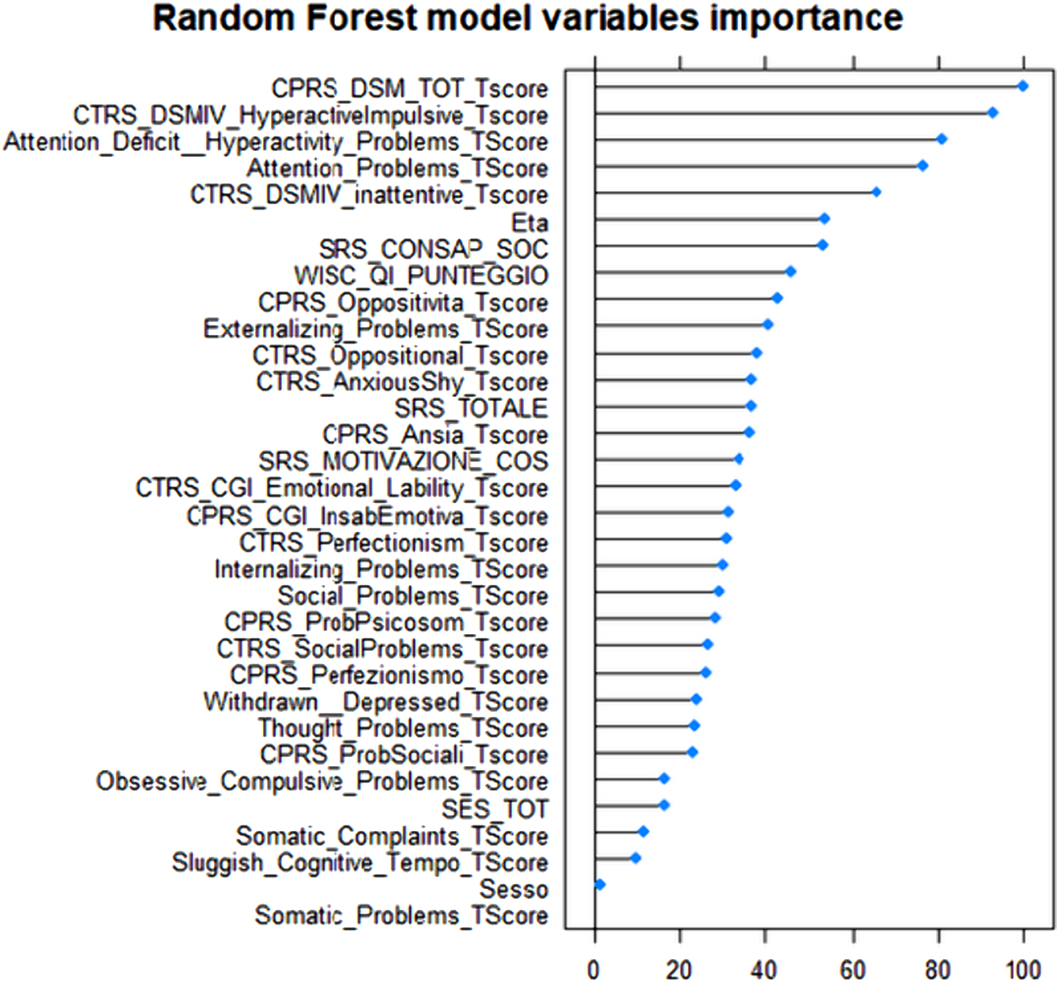
Use of machine learning on clinical questionnaires data to support the diagnostic classification of Attention DeficitHyperactivity Disorder: a personalized medicine approach
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S165-S166
-
- Article
-
- You have access
- Open access
- Export citation
NIRS Hemodynamic Response to Methylphenidate in Children with Attention Aeficit Hyperactivity Disorder: First Administration, Titration Phase and Associations with Clinical Severity
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S54
-
- Article
-
- You have access
- Open access
- Export citation
Obesity and loss of ambulation are associated with lower extremity oedema in Duchenne muscular dystrophy
-
- Journal:
- Cardiology in the Young / Volume 33 / Issue 4 / April 2023
- Published online by Cambridge University Press:
- 13 May 2022, pp. 597-602
-
- Article
- Export citation
Antidepressant use in low- middle- and high-income countries: a World Mental Health Surveys report
-
- Journal:
- Psychological Medicine / Volume 53 / Issue 4 / March 2023
- Published online by Cambridge University Press:
- 23 September 2021, pp. 1583-1591
-
- Article
- Export citation
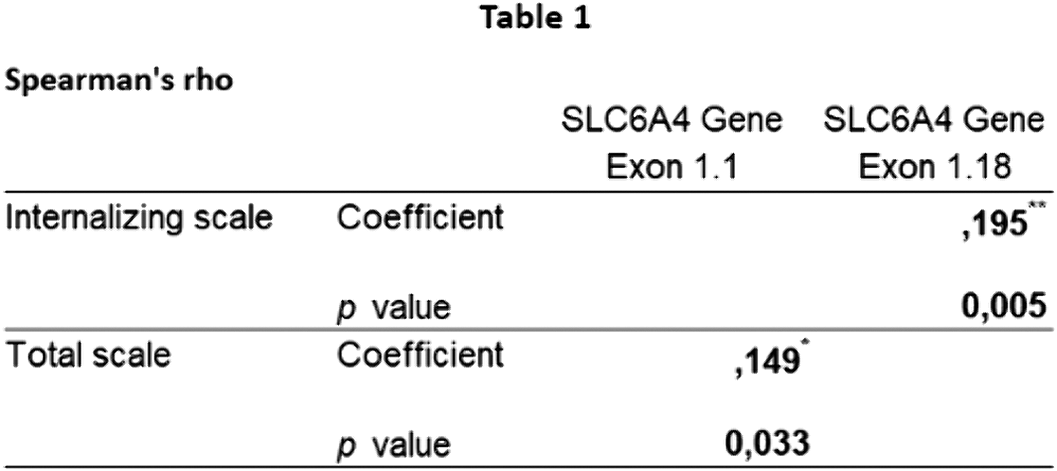
Associations between genes methylation, postnatal risk factors and psychiatric symptoms in a clinical sample of children and adolescents: Preliminar results from the remind longitudinal study
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, pp. S123-S124
-
- Article
-
- You have access
- Open access
- Export citation
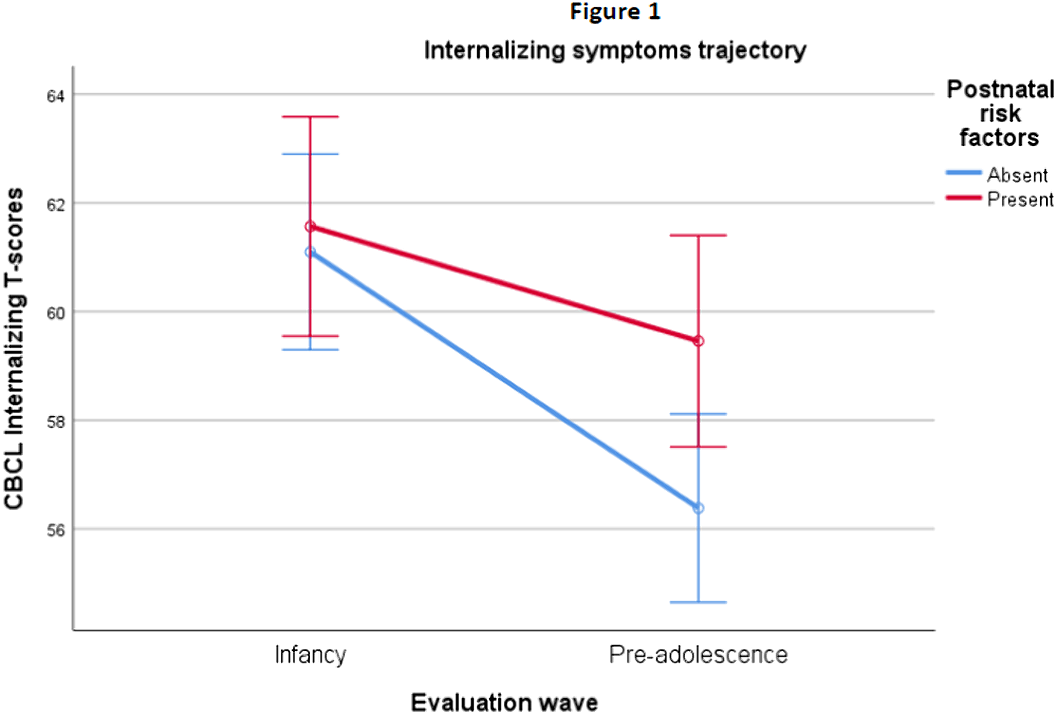
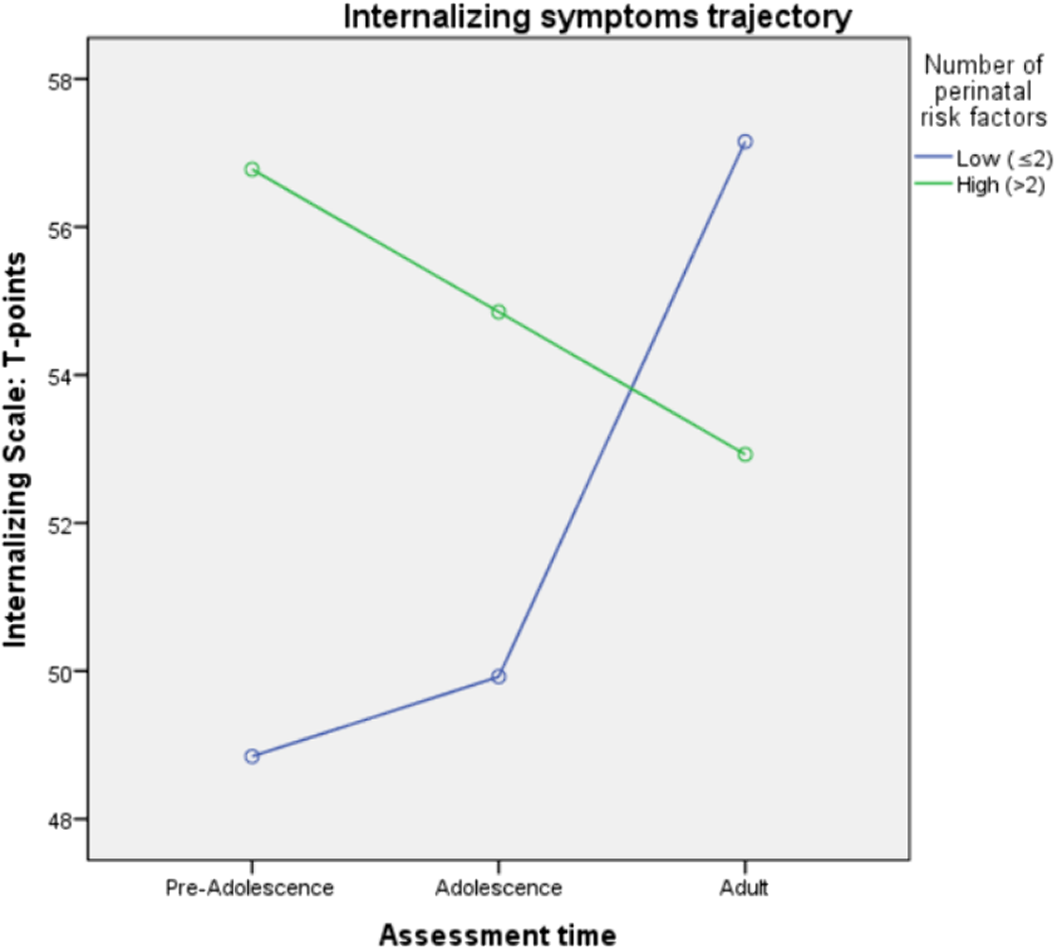
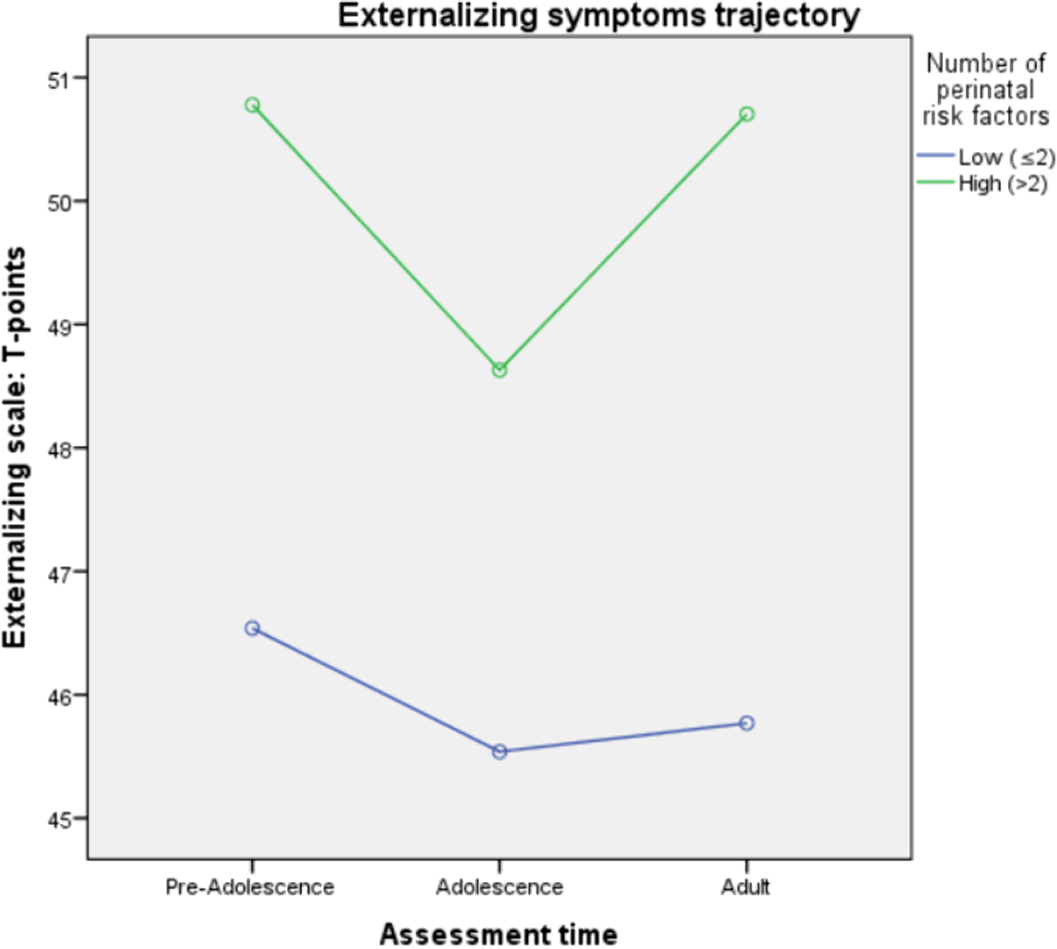
Relationship between internalizing and externalizing symptoms trajectories and perinatal risk factors in an epidemiological sample: Preliminary results from the remind project
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, pp. S148-S149
-
- Article
-
- You have access
- Open access
- Export citation
Development of an actuated corrugated laminate for morphing structures
- Part of
-
- Journal:
- The Aeronautical Journal / Volume 125 / Issue 1283 / January 2021
- Published online by Cambridge University Press:
- 17 August 2020, pp. 180-204
-
- Article
- Export citation
Comorbidity within mental disorders: a comprehensive analysis based on 145 990 survey respondents from 27 countries
-
- Journal:
- Epidemiology and Psychiatric Sciences / Volume 29 / 2020
- Published online by Cambridge University Press:
- 12 August 2020, e153
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Intermittent explosive disorder subtypes in the general population: association with comorbidity, impairment and suicidality
-
- Journal:
- Epidemiology and Psychiatric Sciences / Volume 29 / 2020
- Published online by Cambridge University Press:
- 23 June 2020, e138
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Patterns of care and dropout rates from outpatient mental healthcare in low-, middle- and high-income countries from the World Health Organization's World Mental Health Survey Initiative
-
- Journal:
- Psychological Medicine / Volume 51 / Issue 12 / September 2021
- Published online by Cambridge University Press:
- 28 April 2020, pp. 2104-2116
-
- Article
- Export citation
Hyperthyroidism and Psychotic Symptoms: a Case Report
-
- Journal:
- European Psychiatry / Volume 33 / Issue S1 / March 2016
- Published online by Cambridge University Press:
- 23 March 2020, pp. S440-S441
-
- Article
-
- You have access
- Export citation
Awareness of illness and psychosis
-
- Journal:
- European Psychiatry / Volume 33 / Issue S1 / March 2016
- Published online by Cambridge University Press:
- 23 March 2020, pp. S584-S585
-
- Article
-
- You have access
- Export citation
Structural Analysis of MoS2 Layers in a 3D Assembly
-
- Journal:
- Microscopy and Microanalysis / Volume 25 / Issue S2 / August 2019
- Published online by Cambridge University Press:
- 05 August 2019, pp. 2190-2191
- Print publication:
- August 2019
-
- Article
-
- You have access
- Export citation
Complementary and alternative medicine contacts by persons with mental disorders in 25 countries: results from the World Mental Health Surveys
-
- Journal:
- Epidemiology and Psychiatric Sciences / Volume 27 / Issue 6 / December 2018
- Published online by Cambridge University Press:
- 28 December 2017, pp. 552-567
-
- Article
-
- You have access
- HTML
- Export citation
Trauma and psychotic experiences: transnational data from the World Mental Health Survey
-
- Journal:
- The British Journal of Psychiatry / Volume 211 / Issue 6 / December 2017
- Published online by Cambridge University Press:
- 02 January 2018, pp. 373-380
- Print publication:
- December 2017
-
- Article
-
- You have access
- HTML
- Export citation
Feedback and Feeding in the Context of Galaxy Evolution with SPICA: Direct Characterisation of Molecular Outflows and Inflows
- Part of
-
- Journal:
- Publications of the Astronomical Society of Australia / Volume 34 / 2017
- Published online by Cambridge University Press:
- 10 November 2017, e054
-
- Article
-
- You have access
- HTML
- Export citation