Background
The Kumamoto earthquake that struck Japan in 2016 left 50 people dead and 2,804 injured, and led to the evacuation of 183,882. The Kumamoto earthquake actually involved two big earthquakes, the second being larger than the first, causing damage to many buildings and a fear of aftershocks, which led residents to want to stay at evacuation centers.
Numerous medical assistance teams, such as disaster medical assistance teams (DMATs), came from all parts of Japan and were coordinated by local health authorities, including the health center in Aso City. Humanitarian Medical Assistance (HuMA; Tokyo, Japan) is a medical, nongovernmental organization in Japan. The HuMA organization supported the Aso Health Center in managing the large number of assistance teams and starting a health cluster meeting.
Screening for Pregnant Women
Aso City, with a population of 27,018 based on figures from the national census in 2015, employs six midwives, each in charge of a different district. It was impossible to perform all of their duties immediately after the earthquake, as midwives are often over-burdened after a disaster. 1 After a disaster, the manual for midwives requires them to manage evacuation centers, visit homes in rural areas, re-start health check-ups for residents, and provide care to the most vulnerable among the population, such as older people, people with disabilities, children, and pregnant women. Two weeks after the earthquake, these midwives had still not managed to check on all pregnant women. It was reported that many pregnant women and families with children tended to avoid the evacuation centers because they were extremely congested and had limited or no private space, preferring instead to stay in their own cars. It was also reported that staying in a car was associated with a high-risk of developing deep venous thrombosis (DVT), especially among pregnant women and older people. Therefore, it was difficult to find pregnant women in evacuation centers.
Actually, the Japan Society of Obstetrics and Gynecology (Tokyo, Japan) dispatched a team of obstetricians to visit the evacuation centers in Kumamoto City, but they could not collect enough information about the pregnant women who required medical support because they could not find any. This led to the realization that people who stay in their car, especially pregnant women and families with children, cannot be reached to provide support.
The HuMA organization collaborated with the Advanced Life Support in Obstetrics (ALSO)-Japan team and considered how midwives could locate pregnant women in Aso City. It should be noted that mother and child health handbooks are distributed to all pregnant women when at approximately 10 weeks’ gestation by ward offices in Japan. The mother and child health handbook has vouchers for maternal health check-ups. The results of maternal health check-ups, infant vaccination records, and infant growth records can be documented in these handbooks. Information useful for child-rearing, such as that about the infant’s growth, growth curve, and appearance of stool, is also recorded in the handbook. When pregnant women receive this handbook, they have to declare their family makeup, address, and phone number to the ward office. Because Aso City has this information, we decided to call pregnant women directly to ask them a series of questions. We discussed the content of the questions with midwives and the ALSO-Japan team, and then classified the pregnant women according to risk. In total, we called 124 pregnant women and asked about their residential environment, their need for support, and so on, during a three-minute talk. The results are shown in Figure 1.

Figure 1. Stratification of the Risk of Pregnant Women.
We classified pregnant woman in Aso City according to risk as follows: those requiring immediate intervention by midwives or public health nurses were classified as Level 3; those requiring continuous care by midwives or public health nurses as Level 2; those requiring regular pregnancy health check-ups as Level 1; and those having no-risk as Level 0.
In total, seven pregnant women requiring immediate intervention were classified as Level 3. One of these women was considered to have a high-risk of DVT and therefore went to the hospital immediately after being examined by the ALSO-Japan team. Another pregnant woman classified as Level 3 was from a foreign country and could not understand Japanese language, while another had twins and was in her last month of pregnancy.
In addition, 19 pregnant women were classified as Level 2 and 68 as Level 1. None of the pregnant women had any life-threatening conditions. We explained the risks associated with staying in a car to the Aso City midwives, and suggested that the foreign pregnant woman be moved to a hotel as a post-disaster, publicly-funded rental accommodation; this woman agreed to go to the hotel and subsequently had a safe delivery. The pregnant woman with twins had planned to undergo a cesarean section, but it was performed earlier than scheduled because of early labor; however, the mother and both babies were healthy.
The HuMA organization and the ALSO-Japan team provided adequate interventions to the affected pregnant women in Aso City, and then handed them over to the midwives and public health nurses in Aso City for additional care. In this way, severe complications of pregnancy could be avoided. The HuMA organization and the ALSO-Japan team supported local midwives in providing care for pregnant women, which was the issue they had worried most about.
Trends in Hospital Access Among Pregnant Women
Medical assistance teams such as DMATs used a daily reporting system called J-SPEED to report the number of patients and diseases treated by medical assistance teams reported during the Kumamoto earthquake response. The original SPEED, which was developed in the Philippines, can be used to report the numbers of patients with some symptoms such as “fever,” “acute respiratory infection,” “watery diarrhea,” and so on. The use of this system can help visualize the number and distribution of patients after disaster and detecting early signs of outbreak of infectious diseases. Japan Disaster Relief medical teams used the SPEED system during the Haiyan typhoon disaster response in the Philippines, and then based on SPEED, developed the J-SPEED for use in Japan. These J-SPEED data from the Kumamoto earthquake are shown in Figure 2 as the patients’ ages and pregnancy status; in the figure, it can be seen that a limited number of pregnant women visited the medical assistance teams after the disaster, and the ratio of pregnant women who visited the medical assistance teams was significantly lower than that of other populations. The pregnant women who came to medical assistance teams were more severe than others (P <.01; Figure 2). However, the ratio of pregnant women who needed to be referred to a higher-level hospital was significantly higher (P <.01; Figure 3). This finding indicates that pregnant women have limited access to medical care, which highlights the importance of approaching pregnant women by medical staffs such as midwives and public health nurses.
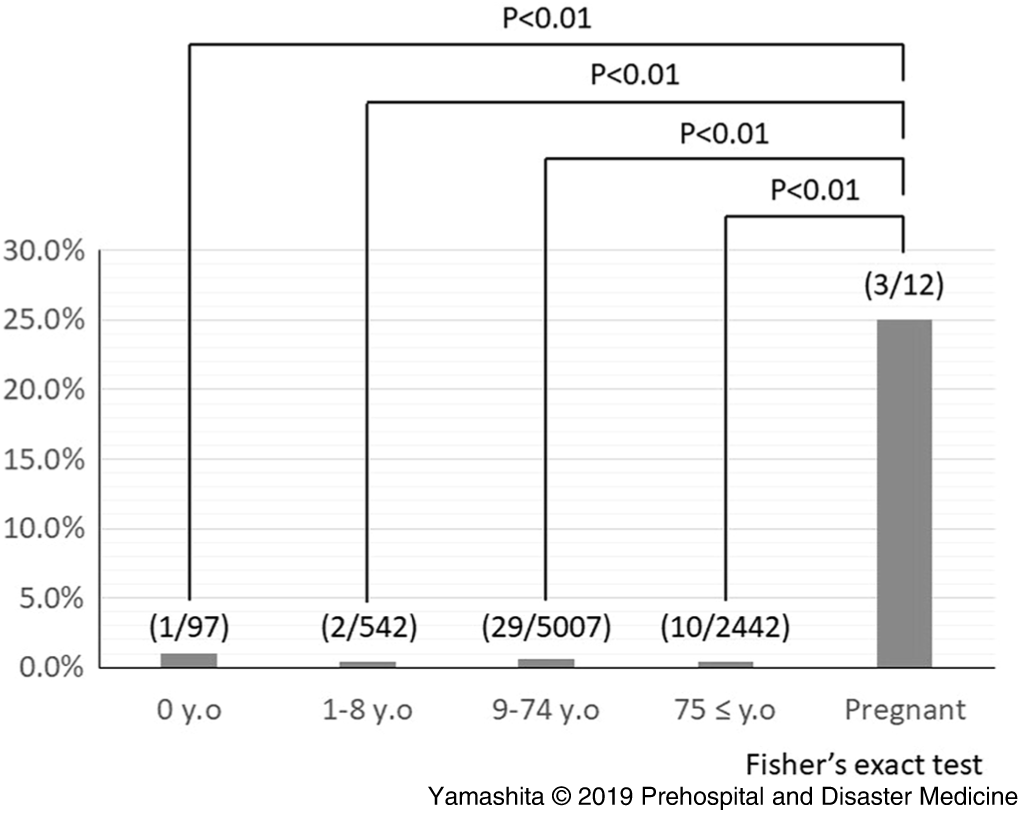
Figure 2. Prevalence of the Severe Patients.

Figure 3. Prevalence of the Patients to be Referred.
Considerations
In the present study, we discussed one method that is useful for providing obstetrical care to affected pregnant women that involves collaborating with specialists after a disaster, because care cannot always be provided by specialists in disaster medicine. It is also important for members of an obstetric team to foster good face-to-face relationships and conduct adequate drills and training.
The use of mother and child health handbooks is wide-spread in Japan, and this information is very helpful after a disaster. We consider that the government should maintain up-to-date information on pregnant women, such as addresses and phone numbers, because regardless of disasters, pregnant women can often be malnourished and are sometimes the victims of domestic violence. Japanese mother and child health handbooks contain a lot of useful information about perinatal care, and Japanese women are instructed to always carry this handbook. However, we believe that the Japanese government should add information regarding the contents of evacuation kits in the case of a disaster, as well as the locations evacuation centers where pregnant women can stay comfortably.
The most vulnerable people in a disaster situation who may need special support include older people, foreigners, people with disabilities, children, and pregnant women. The ratio of pregnant women in the Japanese population is only 0.8%,Reference Honami 2 but to support pregnant women means to support the fetus, which supports the future of Japan. Preparedness for providing care to pregnant women is relatively slow because of the common view that “pregnancy is not a disease” in Japan. By contrast, preparedness for providing care to older people, which can include cardboard beds and rehabilitation teams, tends to proceed smoothly. Pregnant women in Japan tend to avoid seeking assistance; rather, they often offer support to older people or those with disabilities because they also believe that “pregnancy is not a disease.” In fact, many pregnant women in Japan have the experience of not being offered a seat during busy commutes on public transport.
Although the concept of establishing evacuation centers in Japan especially for mothers, children, and pregnant women is becoming increasingly popular, it is still highly localized, and thus not sufficient to support all pregnant women in Japan. The findings of this study could be expected to promote efforts to support pregnant women and fetuses after a disaster in Japan, where the declining birth rate is a severe problem.
Acknowledgements
This study is supported by the World Health Organization Centre for Health Development (WHO Kobe Centre – WKC: K18003; Kobe, Japan). Study procedure of the J-SPEED data analysis was approved by the Ethics Committee for Medical Care and Research at the University of Occupational and Environmental Health, Kitakyusyu, Japan.
Conflicts of interest
none







