Introduction
In the USA, an estimated 2.5–4.7 million persons are living with chronic hepatitis C virus (HCV) infection, and approximately 50% of HCV-infected persons are unaware of their infection status [Reference Edlin1, Reference Yehia2]. Persons born during 1945–1965 (post-World War II baby boomer cohort) are estimated to account for >75% of chronic HCV infections in the USA; however, acute HCV infection is reported primarily among a younger population [Reference Denniston3–Reference Suryaprasad5]. Surveillance data of reported cases of HCV from Tennessee and other Appalachian states collected during 2006–2012 demonstrated a 364% increase in the number of reported acute HCV infections among persons aged ⩽30 years, with >70% of infected persons reporting injection drug use (IDU) [Reference Zibbell4].
During 2013–2016, in Tennessee, the rate of newly reported chronic HCV cases increased >400% (63 cases/100 000 persons in 2013 to 317 cases/100 000 persons in 2016) (unpublished TN surveillance data; TN NEDSS Based System, April 2017). Due to insufficient testing and a lack of resources to conduct thorough surveillance and comprehensive case investigations, reported HCV case counts are believed to underrepresent the true burden of chronic HCV. Despite uncertainty regarding the burden of chronic HCV infection in Tennessee, surveillance data have demonstrated that the eastern part of the state is affected disproportionately by chronic HCV. In 2016, the prevalence of newly reported chronic HCV in eastern Tennessee counties was 489.5 cases/100 000 persons, compared with 295.5 cases/100 000 persons in the rest of the state (unpublished TN surveillance data; TN NEDSS Based System, April 2017).
Despite these recent concerning trends in HCV incidence and prevalence in Tennessee and the USA, a recent assessment by the National Academies assessed the feasibility of HCV elimination in the USA. Their report concluded that control of HCV in the USA is attainable in the short term, and that the ultimate longer-term goal of HCV elimination is feasible, but will require a better understanding of the current epidemic and barriers to achieving these goals [6]. Therefore, we sought to better understand prevalence and risk factors for HCV infection in the region by conducting HCV testing with risk factor analysis among patients of three different local health department clinics in eastern Tennessee. Additionally, a nested case–control study was conducted among the identified persons who use drugs (injection and/or intranasal) to further explore associations between specific risk factors, drug use behaviours and HCV infection.
Methods
Sample population
Routine opt-out HCV testing was offered to patients attending sexually transmitted disease (STD) clinics and family planning (FP) clinics in Knox County (1 June 2016–31 October 2016) and Chattanooga-Hamilton County (6 July 2016–31 October 2016) Health Departments in Tennessee. Opt-in HCV testing was offered in STD clinics in the Sullivan County Regional Health Department, and testing was offered once-monthly at a Sullivan County addiction treatment facility (18 July 2016–31 October 2016). Patients ineligible for HCV testing included those with a documented positive HCV result within the last 6 months and persons aged ⩽13 years.
Data collection
Routine demographic and specific risk factor information was collected at the time of HCV testing (online Supplementary Appendix I). Pregnancy status, risk factor information and testing results for STDs (i.e. chlamydia, gonorrhoea, human immunodeficiency virus (HIV) and syphilis) that were collected on the same encounter date were linked and managed by using Research Electronic Data Capture (REDCap) [Reference Harris7]. Laboratory specimens underwent standard HCV testing (serum antibody testing coupled with reflex qualitative polymerase chain reaction (PCR)) at the Tennessee Department of Health (TDH) State Public Health Laboratory.
Nested case–control study
A nested case–control study was conducted among persons identified through HCV testing and risk factor assessment during 1 June–4 October 2016, who reported a history of intranasal or IDU and were aged ⩾18 years. All persons meeting these criteria were invited to participate in the nested case–control study; case-patients were HCV antibody positive and control subjects were HCV antibody negative. No incentives were provided for participation. Telephone interviews were conducted using a structured questionnaire to complete a detailed assessment of drug-using behaviours. Three attempts were made to contact potential participants unless they had an invalid phone number or declined participation. Participants were excluded from data analysis if they reported answers that were discrepant from their original risk factor assessment (e.g. reported a history of IDU during risk factor assessment at the time of HCV testing, but denied IDU during the telephone interview). This study was approved by the TDH Institutional Review Board and determined to be a public health problem evaluation/control by CDC.
Statistical analysis
Statistical analysis of data collected through routine HCV testing and risk factor assessment and the nested case–control study was conducted by using SAS® version 9.4 (SAS Institute, Incorporated, Cary, North Carolina, USA). T-tests were used to assess differences in continuous variables as appropriate, whereas Pearson's χ 2 and Fisher's exact tests were used to compare categorical variables. All P values were two-sided and considered statistically significant if P < 0.05. Multivariable logistic regression analysis, controlling for sex, race, health department testing location, clinic type and the assessed risk factors, was used to estimate adjusted odds ratios (aORs) for associations between reported risk factors and past or present HCV infection. Odds ratios (ORs) with corresponding 95% confidence intervals (CIs) were calculated for selected exposures in the case–control analysis; multivariable logistic regression was not conducted due to the small sample size.
Results
HCV testing and risk factor assessment
Of 4753 persons tested for HCV, 397 (8.4%) were HCV antibody positive (Ab+), indicating past or present HCV infection. Of Ab+ persons, 294 (74.1%) were PCR positive, representing current HCV infection. The mean age of Ab+ persons was 37.3 years (range 14–71 years) and 30.4 years (range: 10–79) (P < 0.0001) for antibody negative (Ab−) persons (Table 1). Among Ab+ persons, 19.4% (77/397) were born during 1945–1965 and 43.1% (171/397) were females of reproductive age (14–50 years old). Five (2.9%) Ab+ females of reproductive age were pregnant at the time of HCV testing (data not shown). Males were significantly more likely than females to be Ab+ (10.8% vs. 6.7%, P < 0.0001), and non-Hispanic white persons were significantly more likely to be Ab+ compared with all other races/ethnicities (14.8 vs. 3.6%, P < 0.0001). A higher proportion of patients tested at STD clinics (9.8%) and the addiction treatment facility (57.1%) were HCV Ab+, compared with those tested at FP clinics (3.4%, P < 0.0001).
Table 1. Characteristics of study population by hepatitis C virus antibody status (N = 4753)

HCV, hepatitis C virus; Ab, antibody; FRA, female of reproductive age (14–50 years old); STD, sexually transmitted disease; FP, family planning; SA, substance abuse.
* White, non-Hispanic race, compared with all other races/ethnicities.
† FP clinic, compared with other testing facility types.
Approximately 9.0% of the study population identified through HCV testing and risk factor assessment reported a history of IDU, and 20.0% reported a history of intranasal drug use (Table 2). Additionally, >25% of the overall study population and >75% of Ab+ persons reported a history of incarceration longer than 24 h. Compared with HCV Ab− persons, those testing HCV Ab+ were significantly (P-value <0.001) more likely to report IDU (69.5% vs. 3.4%), intranasal drug use (74.3% vs. 15.4%), tattoo or piercing (47.4% vs. 20.7%), incarceration (76.3% vs. 23.1%) and transfusion (3.3% vs. 1.1%). In multivariable regression analysis, history of IDU alone (aOR 52.7, 95% confidence interval (CI) 25.3–109.9), history of both intranasal and IDU (aOR 35.4, CI 24.1–51.9), history of intranasal drug use alone (aOR 2.6, CI 1.8–3.9) and history of incarceration (aOR 2.7, CI 2.0–3.8) were significantly associated with past or present HCV infection (Table 3). No significant associations with the previous history of transfusion, transplant or tattoo or piercing were demonstrated. Approximately 10% (39/397) of Ab+ persons reported no risk factors (Table 2).
Table 2. Univariate analysis of reported risk factors for hepatitis C virus (HCV) infection among study population (N = 4753), stratified by HCV antibody status
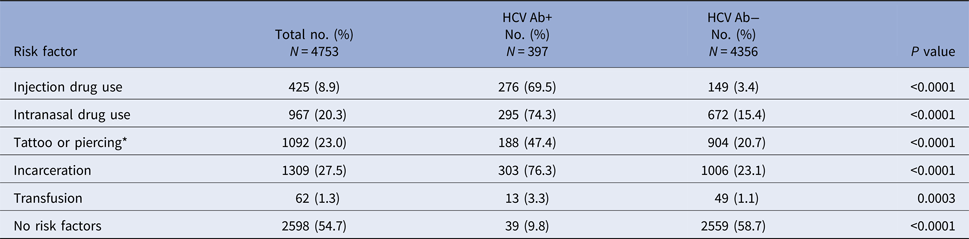
* Defined as piercing in a location other than ears.
Table 3. Multivariable logistic regression* estimated odds ratios for associations between risk factors and past or present hepatitis C virus infection (N = 4753)
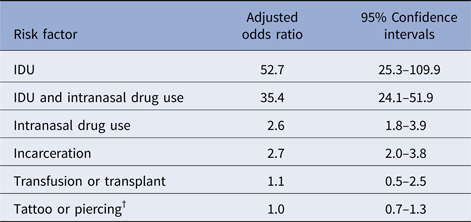
* Model controlled for sex, race, health department testing location, clinic type and the assessed risk factors.
† Defined as piercing in a location other than ears.
Approximately half (2777/4753; 58.4%) of all persons were tested for both HCV and HIV (data not shown). One person was newly diagnosed with HIV and HCV (Table 4). A higher proportion of gonococcal infections were identified among HCV Ab+ persons (11.6%), compared with HCV Ab− persons (6.0%, P = 0.06); conversely, a significantly higher proportion of chlamydial infections were identified among HCV Ab− persons (14.4%), compared with HCV Ab+ persons (8.1%, P = 0.02).
Table 4. Prevalence of bacterial and viral sexually transmitted pathogens by hepatitis C virus antibody status

HIV, human immunodeficiency virus; HCV Ab+, hepatitis C virus antibody-positive; HCV Ab−, hepatitis C virus antibody-negative.
* Gonorrhoea testing from any site: pharynx, cervix, penis, urethra, urine, vagina or rectum.
† Chlamydia testing from any site: pharynx, cervix, penis, urethra, urine, vagina or rectum.
Nested case–control study
Data from the HCV testing and risk factor assessment during 1 June–4 October 2016, identified 574 persons with a history of intranasal or IDU who were engaged for an interview for the case–control study (Fig. 1). Sixty-three (11.0%) interviews were completed from the 21 case-patients and 42 control subjects enrolled. Participants were aged 18–63 years (mean 35.9 years); 51% (32/63) were female; 78% (49/63) were non-Hispanic white; all reported a history of intranasal drug use, 49% with IDU and 70% with incarceration. Approximately half reported a high-school diploma or equivalent or less than a high-school level of education (35/63; 56%). These demographic frequencies are similar to those observed in the standard HCV testing and risk factor assessment sample (data not shown).

Fig. 1. Enrollment of participants in nested case–control study. Persons identified through hepatitis C virus testing and risk factor assessment during 1 June 2016–5 October 2016. Persons <18 years old and those who reported answers discrepant from their original risk factor assessment were excluded.
In the univariate analysis, history of IDU (OR 56.4, CI 6.8–470.9) and incarceration (OR 15.0, CI 1.8–122.4) were significantly associated with HCV infection. Because all 63 persons in the analysis used intranasal drugs, we were unable to measure a corresponding OR for this risk factor. Among 31 persons with a reported history of both intranasal and IDU, 84% reported previous intranasal drug use, occurring 1–18 years (median 5.5 years) before the first IDU. Compared with control subjects, a higher proportion of case-patients reported a history of reusing needles or syringes (94% vs. 45%, P < 0.01) and sharing snorting utensils, although this finding was not significant (81% vs. 62%, P = 0.24) (Table 5). The most frequently used intranasal drugs were cocaine (71%) and opioids (57%). A significantly higher proportion of case-patients than control subjects reported intranasal opioid drug use (76% vs. 48%, P = 0.03). The majority of commonly injected drugs reported were opioids (71%), cocaine (45%), heroin (42%) and methamphetamine (39%). Among those with a history of IDU, a significantly higher proportion of case-patients than control subjects reported injecting methamphetamine (55% vs. 9%, P = 0.02). Case-patients were significantly more likely to report a history of incarceration, compared with control subjects (95% vs. 57%, P < 0.01).
Table 5. Univariate analysis of risk factors among participants in a nested case–control study, stratified by case status
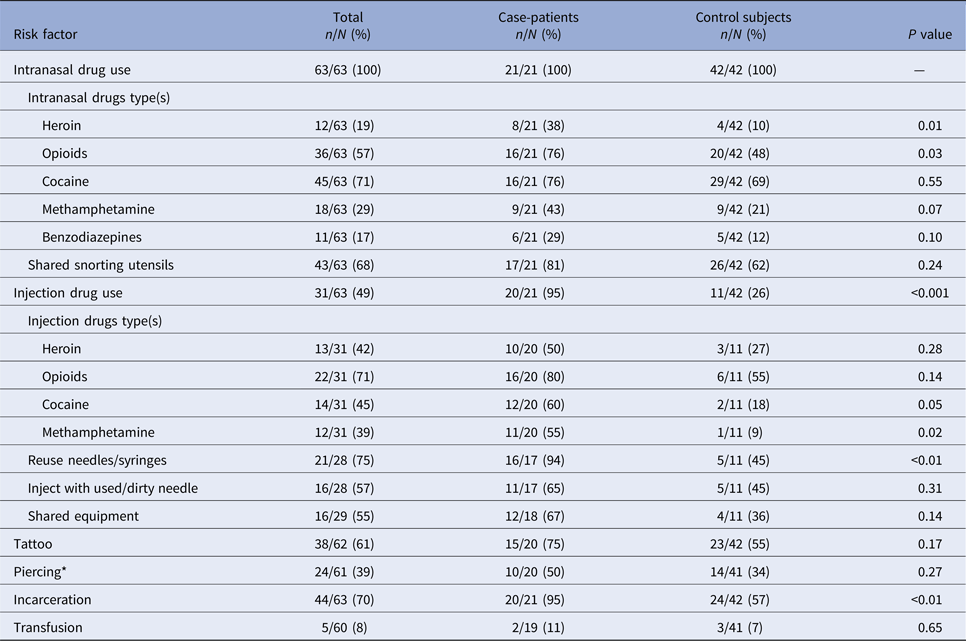
* Defined as piercing in a location other than ears.
Discussion
Our findings indicate that after adjusting for sex, race, testing location, clinic type and other risk factors, IDU, intranasal drug use and incarceration are independent indicators of risk for past or present HCV infection within the study population. Consistent with the United States Preventive Services Task Force (USPSTF) and the Centers for Disease Control and Prevention (CDC) guidelines, our analysis demonstrates that past or current IDU is the predominant risk factor for HCV infection among persons obtaining services from Tennessee STD and FP clinics, or from addiction treatment facilities [8–10]. While USPSTF considers intranasal drug use and incarceration to be indications for HCV testing, CDC does not. Current CDC recommendations state that HCV testing is of uncertain need for intranasal cocaine users and other persons who use non-injecting illegal drugs [8–10]. However, our findings demonstrate that incarceration and intranasal drug use might be independent indicators of risk for HCV infection, and that intranasal drug use is a potential indication of subsequent IDU.
Epidemiologic studies among asymptomatic blood donors, HIV-positive men who have sex with men and primary care patients have supported intranasal drug use as an HCV risk factor [Reference Conry-Cantilena11–Reference Drainoni14]. However, other studies have been inconclusive or indicated that intranasal drug use might reduce transmission of HCV infection among IDUs [Reference Galperim15–Reference Des Jarlais17]. Researchers have indicated intranasal drug use as a viable method of HCV transmission by demonstrating the presence of blood and HCV RNA in nasal secretions and intranasal drug-use equipment [Reference McMahon18, Reference Aaron19]. Although HCV testing and risk factor assessment in our analysis identified intranasal drug use as a significant independent predictor of risk for HCV infection, intranasal drug use could not be evaluated as an independent risk factor in the nested case–control analysis because all participants used intranasal drugs. However, a higher proportion of Ab+ persons in the nested case–control subgroup reported sharing snorting utensils, and the majority of persons with a history of IDU reported previous intranasal drug use occurring a median of 5.5 years before first IDU. This delay before the development of riskier drug use behaviours might be an opportunity for public health intervention that warrants exploration. If this is a common trend, it offers important information that may be applicable to public health prevention programmes. Our findings also highlight the ongoing opioid epidemic as a factor in the HCV epidemic, as opioids were commonly reported intranasal and injection drugs in our study population. We also must consider that some persons who admitted to only using intranasal drugs may, in fact, be persons who inject drugs. Regardless of whether it is an independent risk factor, or an indicator of higher HCV risk, persons who use intranasal drugs are an important group to target in HCV prevention and testing efforts.
Additionally, our analysis identified a history of incarceration as an independent indicator of risk for HCV infection. Although incarceration has been demonstrated to be a risk factor for HCV and is considered as such by USPSTF, some studies have demonstrated low rates of HCV testing among persons with a reported history of incarceration; in one primary care clinic study, only 9% of persons with an identified history of incarceration were tested for HCV, compared with 47% of those with a history of IDU [Reference Almario20]. Although a history of incarceration is associated with HCV in our analysis, separate from drug use risk, we believe that it is also a potential indicator of other high-risk behaviours and risk for acquisition of HCV. This premise has been explored in relation to HIV risk, and multiple studies have demonstrated that having an arrest history might serve as an indicator of HIV risk and substance abuse [Reference Weisbord21–Reference Wise24]. The validity of patients’ self-reported risk assessments might be lower for highly stigmatised or illegal activities like IDU or intranasal drug use. This concept has been explored in relation to drug use; reports of cocaine and heroin use were found to have particularly low sensitivity [Reference Fendrich25]. The low validity of self-reported risk factor screening for drug use might indicate that screening on the basis of other risk factors, like incarceration, might be a more accurate estimate of a patient's true risk. The role of incarceration, as both an independent risk factor and indicator of other high-risk behaviours, may be an important consideration in HCV risk stratification.
The prevalence of Ab+ persons among STD clinic patients was approximately 10%, suggesting there may be utility in incorporating HCV testing into routine STD assessment. HCV testing in STD clinics provides an opportunity to reach and test females of reproductive age before pregnancy. Several STD clinics throughout the country have successfully integrated risk-based HCV testing and counselling into their practice model, although supporting adequate follow-up and treatment for HCV-positive persons continues to present challenges [Reference Zimmerman26]. However, the presence of integrated hepatitis services within an STD clinic might attract persons who inject drugs for care, providing a valuable service for a highly vulnerable population [Reference Hennessy, Weisfuse and Schlanger27].
Females of reproductive age (14–50 years) represented 57.5% (2733/4753) of persons tested in this analysis and demonstrated an HCV antibody-positive rate of 6.3% (171/2733). Five of these women (5/171; 2.9%) were pregnant at the time of HCV testing and four (4/171; 2.3%) had chronic HCV infection. Three of the pregnant women (3/5; 60%) reported a history of IDU, 1 (1/5; 20%) reported a history of intranasal drug use only and 1 (1/5; 20%) reported no risk factors for HCV infection (data not shown). The American College of Obstetrics and Gynecology (ACOG) recommends that risk-based HCV screening per the CDC guidelines be applied to pregnant women; however, a substantial proportion of HCV-infected pregnant women and their high-risk children are undiagnosed [28–Reference Prasad and Honegger30]. Vertical transmission occurs in approximately 5% of births from HCV-infected mothers, and an estimated 85–95% of HCV-infected children in the USA have not been identified [Reference Benova31, Reference Prasad32]. A standardised public health case definition for perinatal HCV infection was just recently approved by the Council of State and Territorial Epidemiologist in June 2017; however, because no standardised case definition existed previously, it further complicated our ability to accurately quantify this problem [33]. Furthermore, there is evidence that maternal HCV infection is an independent risk factor for adverse perinatal outcomes [Reference Safir34]. A study among a cohort of HCV-infected pregnant women demonstrated that screening according to the ACOG and CDC guidelines would have missed 28% of those infected [Reference Benova31, Reference Fernandez35]. Routine prenatal screening for HCV is not recommended; however, expansion of risk-based prenatal testing for HCV beyond current guidelines may be an area for future consideration [Reference Patrick36].
This analysis has limitations. First, we were unable to perform routine opt-out HCV testing in all clinics in all health departments in Tennessee, making results more difficult to generalise geographically. Second, risk factor information collected at the time of HCV testing was self-reported and might be affected by response or recall bias; however, it is more likely that risk factors were underreported, biasing our results toward the null. Third, only 11% of identified intranasal or IDU could be interviewed for the nested case–control study, potentially leading to nonresponse bias. Finally, the limited sample size in the nested case–control study reduced our ability to detect statistical differences among groups for multiple potential risk factors.
These findings indicate intranasal drug use and incarceration as independent indicators of risk for HCV transmission. Our analysis adds to the body of evidence suggesting that persons who report a history of using intranasal drugs and persons with a history of incarceration are important populations to consider in HCV prevention and testing strategies [Reference Conry-Cantilena11, Reference Drainoni14, Reference Almario20]. In addition, expanded risk-factor testing aimed at higher-risk groups such as STD clinic populations, persons undergoing addiction treatment, persons with a history of incarceration and reproductive-aged females, may provide a diagnostic safety net for these vulnerable populations [Reference Patrick36, Reference Frimpong, D'Aunno and Jiang37]. With the advent of highly effective, well-tolerated, curative therapies for HCV, consideration may be given to implementing existing screening recommendations to ensure that thorough, risk-based testing is performed, especially among these vulnerable populations. Only by identifying and informing HCV-infected persons who are unaware of their status and linking them to established treatment and follow-up programmes, can we begin to work towards HCV elimination.
Supplementary material
The supplementary material for this article can be found at https://doi.org/10.1017/S0950268818000080.
Declaration of Interest
No known conflicts of interest exist.
Note: The findings and conclusions in this report are those of the authors and do not necessarily represent the official position of the Centers for Disease Control and Prevention.










