CLINICIAN'S CAPSULE
What is known about the topic?
Palliative medicine is increasingly encountered in an emergency medicine setting, and emergency medicine residents desire further training in this field.
What did this study ask?
How many postgraduate emergency medicine programs in Canada have an existing palliative medicine curriculum?
What did this study find?
A minority (38.5%) of emergency medicine programs report having a formal palliative medicine curriculum, and the contents are variable.
Why does this study matter to clinicians?
It will be important to define how trainees will achieve competence in palliative medicine in the emergency department.
INTRODUCTION
The emergency department (ED) may not be seen as the ideal place for initiation of palliative care and end-of-life care, yet up to 40% of patients with end-of-life concerns present to the ED in the last 2 weeks of life.Reference Barbera, Taylor and Dudgeon1, Reference Mierendorf and Gidvani2 Emergency medicine (EM) physicians play an important role in providing care at the end-of-life3 and identifying patients who may benefit from a palliative approach. Palliative care is relief of symptoms that restrict a patient's quality of lifeReference Mierendorf and Gidvani2 and thus it falls firmly within the realm of EM. This may include end-of-life care instituted when the patient is predictably in their final weeks of life and a cure is no longer considered achievable.Reference Quest, Asplin and Cairns4 Goals for ED patients near the end-of-life include pain management and management of other symptoms, including shortness of breath, nausea, fatigue, and depression. Even when established goals of care preclude hospital-based care, an ED visit may be sought due to family distress,Reference Mierendorf and Gidvani2 presenting the EM physician with a complex symptom management, disposition planning, and goals of care scenario. These patients and their families require straightforward and compassionate communication, empathy, reassurance, and solace.Reference Schears5
Nevertheless, the role and content of palliative care education for EM physicians remains ambiguous. Several groups have called for increased education around palliative care and end-of-life care in the ED.3, Reference Gisondi6–Reference Benenson and Pollack10 Ninety-four percent of EM physicians report a need for education in dealing with death and dying.Reference Schmidt, Norton and Tolle11 Several studies have shown that EM residents desire further training in palliative care,Reference Lamba, Pound, Rella and Compton8, Reference DeVader and Jeanmonod12, Reference Smith, Fisher and Schonberg13 and 54% of EM residents report never undergoing a rotation in palliative care.Reference Turner14 Completion of a fellowship in palliative medicine has been associated with increased comfort in managing terminally ill patients.Reference Turner14
At the time this study was designed, there was no consensus on competencies that a Canadian EM resident should possess in palliative and end-of-life care in the ED. In recent months, Canadian EM programs in the Royal College of Physicians and Surgeons of Canada (RCPSC-EM) stream have transitioned to the new Competence by Design curriculum.15 Under this model, training is broken down into stages, each of which has its own set of entrustable professional activities (EPAs) detailed by accompanying milestones. We will be discussing EPAs and competencies interchangeably. The list of EPAs for RCPSC-EM includes one that states: “Providing end-of-life care for a patient”16 (see Appendix 1). Within the Canadian College of Family Physicians Enhanced Training in Emergency Medicine, CCFP(EM), program, there are no listed competencies that pertain directly to palliative and end-of-life care.17 To our knowledge, there has been no evaluation of current curricular content or whether competencies are being addressed; furthermore, there is no standardized set of competencies that apply to both the RCPSC-EM and CCFP(EM) training streams. At the time of this study, the United States Accreditation Council for Graduate Medical Education's (ACGME) list of EM milestones for the evaluation of resident physicians did not include any milestones directly pertaining to palliative or end-of-life care.18 However, an expert, multidisciplinary panel created a curriculum called Education in Palliative and End-of-Life Care in Emergency Medicine (EPEC-EM) that contains a comprehensive list of learning objectives for palliative and end-of-life care in EM.19 Several educational models have been designed to educate residents in areas such as death notification,Reference Quest, Otsuki and Banja20 but this is a narrow aspect of palliative care. Many other resources are targeted primarily at the practising physician or registered nurse.Reference Lamba, DeSandre and Todd9, 21
We performed a national cross-sectional survey of EM program directors. Our objectives were to describe the number of Canadian postgraduate EM training programs with palliative and end-of-life care curricula and to describe what these curricula entailed. We hypothesized that if variability in training could be compared and contrasted, we could begin to establish and address required palliative and end-of-life care competencies for the modern EM physician and design curricula around these.
METHODS
From October to December 2016, a national cross-sectional survey was conducted to assess existing palliative and end-of-life care curricula in Canadian RCPSC-EM and CCFP(EM) programs. Our primary outcome was whether Canadian postgraduate EM training programs had structured palliative and end-of-life care curricula. The study was approved by the Interior Health Research Ethics Board and the University of British Columbia Clinical Research Ethics Board (2016-17-026-H).
Study population
All 36 Canadian EM program directors were surveyed, 19 RCPSC-EM and 17 CCFP(EM), including programs with sites distributed in geographical locations from the main centre.
Survey development
The survey was developed in consultation with the author group, including specialists in palliative medicine, EM (CCFP(EM) and RCPSC-EM), and medical education. It was pilot tested on two staff EM physicians at the University of British Columbia for comprehension and content validity. To our knowledge, there were no previously derived or validated survey tools for palliative and end-of-life care education in EM. An independent professional language translator translated the survey and recruitment materials from English to French.
The survey included dichotomous, Likert-type, and open-ended questions (see Appendix 2). Domains within the survey tool included clinical and non-clinical palliative and end-of-life care experiences, palliative and end-of-life care educational objectives, barriers to implementation of palliative and end-of-life care curricula, assessment of residents after curricular completion, and demographics. We defined the presence of a structured palliative care educational program as at least 3 hours of lecture and/or seminar based non-clinical education over the course of an academic year. Educational objectives were assessed with questions from the EPEC-EM19 objectives. The EPEC-EM objectives were used as a surrogate because, to our knowledge, at the time of this survey, there were no Canadian-based comprehensive palliative and end-of-life care curriculum objectives available that pertain specifically to EM.
Five-point Likert scales were used to assess each program's coverage of the EPEC-EM curriculum objectives in clinical and non-clinical domains. Responses were collated into Likert scores of 0–2 (not well addressed) and 3–5 (well addressed).
Survey administration
All potential participants received an information letter and provided informed consent prior to their enrolment in the study. A 15-question survey in English and French was sent by email to all program directors of both CCFP(EM) and RCPSC-EM postgraduate training programs countrywide using FluidSurveys™ with a modified Dillman approach.Reference Schaefer and Dillman22 Email addresses were obtained through the Canadian Resident Matching Service website. Program directors were emailed with a live link to the survey up to three times between October and December 2016. Participation was incentivized with a $20 CAD coffee card for the first 10 respondents and a draw for five remaining cards for any additional respondents. Finally, a follow-up phone call was made to program directors who had not yet responded 2 weeks prior to the survey closing.
Analysis
Contingency analysis was performed using the Fisher exact test for the primary outcome. Total annual hours of palliative and end-of-life care educational material were analysed using the median and interquartile range (IQR). A descriptive analysis was also performed. For all statistical analyses, p ≤ 0.05 (with 95% confidence intervals) was considered significant.
RESULTS
We received a total of 26 responses from the 36 (response rate = 72.2%) EM postgraduate training programs in Canada. Fourteen of 19 (73.7%) CCFP(EM) programs responded, and 12 out of 17 (70.6%) RCPSC-EM programs responded.
Regarding the primary outcome, 10 out of 26 (38.5%) programs reported having a structured educational program on palliative and end-of-life care. There was no significant difference between RCPSC-EM and CCFP(EM) programs in the primary outcome (p = 1). Educational coverage of the EPEC-EM objectives is displayed in Figure 1.
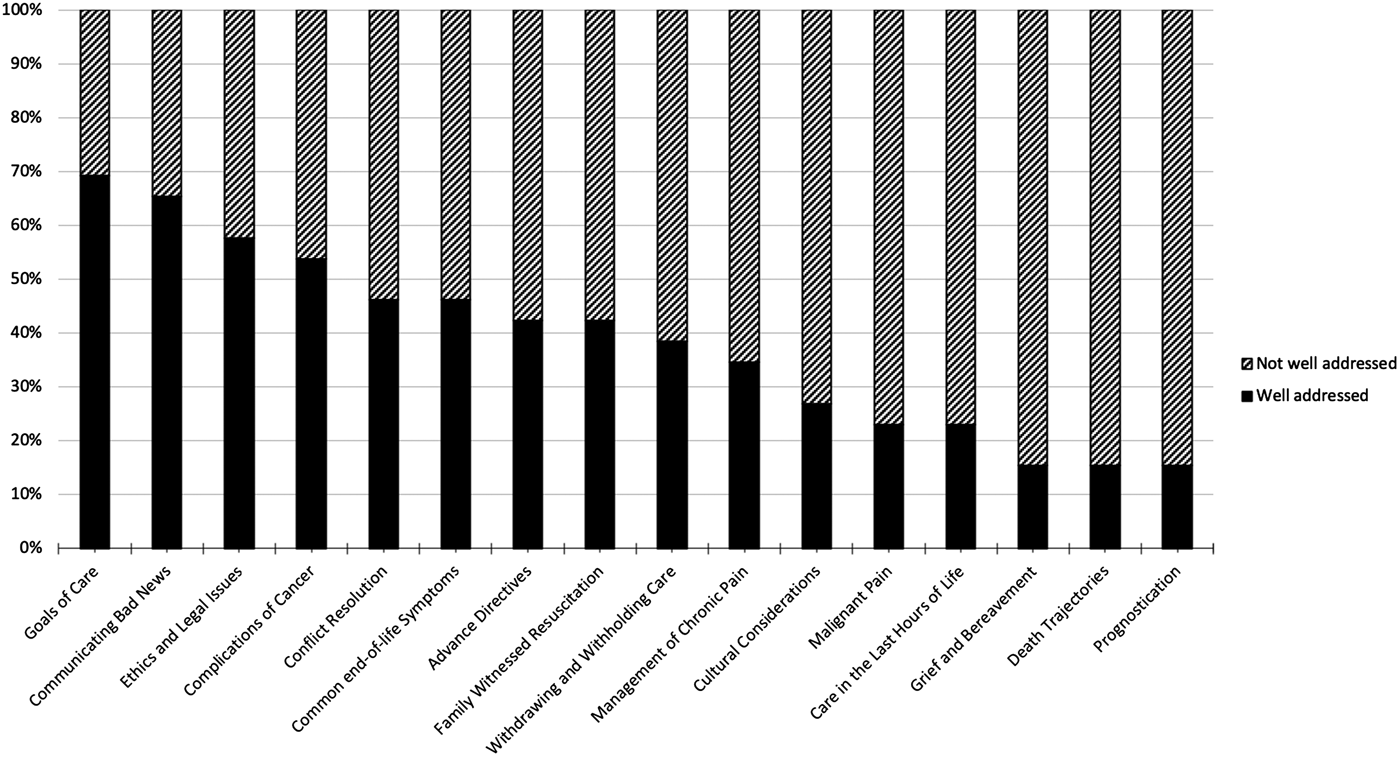
Figure 1. EM program coverage of palliative and end-of-life care objectives.
Of the 10 programs with a structured palliative and end-of-life care educational program, 100% were either lecture or seminar-based. For the entirety of residency, median total lecture hours were 4 (IQR = 4.75 hours). Median seminar hours were 4 (IQR = not applicable due to sample size). No programs used online modules, podcasts, videocasts, or handout materials.
Clinical palliative medicine rotations were mandatory in only one out of 26 (3.8%) programs. However, 4 out of 26 (15.4%) programs offer palliative medicine as a selective rotation out of a short list of options, and 13 out of 26 (50%) programs offer palliative medicine as an elective rotation.
Respondents identified many potential barriers to the implementation of palliative and end-of-life care curricula in EM (Table 1). The top two were a lack of time (84.6%) and curriculum development concerns (80.8%). These latter concerns were defined as an inability to keep content current and relevant.
Table 1. Identified barriers to implementation of curricula around palliative and end-of-life care

Only 4 out of 26 (15.4%) programs formally assessed residents in palliative or end-of-life knowledge or skills with some having multiple formal assessment modalities. Three (75%) of these programs had feedback after a patient encounter, one (25%) had an informal clinical evaluation, and one (25%) had a formal clinical evaluation such as an objective structured clinical examination (OSCE). One program did not specify how its residents were assessed. Seven out of 26 (26.9%) programs have had residents complete formal fellowships in palliative care. Three were RCPSC-EM and four were CCFP(EM).
Three CCFP(EM) programs remarked that there is insufficient time in a 1-year program to have a formal palliative and end-of-life care rotation or curriculum. However, two programs reported that incoming residents have completed training in palliative and end-of-life care during their family medicine training; this included one program that surveyed incoming CCFP(EM) residents over 2 years and found that all had previous formal training in palliative care prior to their EM year.
DISCUSSION
We found that only 38.5% of EM program directors reported having structured palliative and end-of-life curricula and that curricular content was highly variable. This is problematic in that it is difficult to educate trainees to achieve competence in palliative and end-of-life care when clinical or non-clinical experiences have not been defined. Furthermore, 100% of the curricula reported are lecture or seminar-based, which may not be the ideal way to teach these nuanced skills. To our knowledge, this study is the first of its kind in Canada and establishes a national landscape of current palliative and end-of-life care curricula in EM training programs.
In the United States, EPEC-EM provides a train-the-trainer, conference style curriculum for emergency providers.19 One of their specific goals is to collaborate with program directors in EM to ensure that their trainees receive education around core competencies in palliative and end-of-life care in the ED. In recent months, the American College of Emergency Physicians (ACEP) Palliative Medicine Section has developed a set of milestones, using the ACGME milestone framework, for hospice and palliative medicine for EM residents.Reference Shoenberger, Lamba and Goett23 Our results suggest that we do not currently have a similar educational landscape in Canada.
EPEC-EM was developed in the United States; however, a majority of the EPEC-EM objectives are similar to the milestones within the EPA for end-of-life care in the RCPSC-EM curriculum (see Appendix 1). The objectives of advance directives and ethics/legal concerns within EPEC-EM may differ in the Canadian setting. It is important to note that the EPA puts emphasis on end-of-life care and may inadvertently underemphasize other aspects of palliative medicine. Out of the EPEC-EM objectives, only goals of care, ethics and legal issues, communicating bad news, and complications of cancer were well addressed by a majority of EM programs. These pertain to 4 of the 10 milestones within the EPA for providing end-of-life care (see Appendix 1). The remainder of the milestones were either not assessed by this survey or not well addressed within current curricula. Establishing this baseline serves to provide areas of focus as EM residency programs consider starting or improving their palliative and end-of-life care curricula.
Assessment of trainee competency may prove challenging when EM physicians are reporting a need for further education on the topics covered within the EPA.Reference Schmidt, Norton and Tolle11, Reference Wright, Lowton and Robert24 In the future, assessment of competency may shift to the increasing number of EM physicians specializing in palliative medicine. As of 2018, there are 150 EM physicians in the United States with specialization in hospice and palliative medicine19 and both the ACEP and the Canadian Association of EM physicians have sections or committees for ED palliative medicine.
Time was noted to be a significant barrier to palliative and end-of-life care education in the ED in both RCPSC-EM and CCFP(EM) training streams. This is an interesting finding in that the RCPSC-EM program is 5 years in length, whereas the CCFP(EM) program is 1 year. CCFP(EM) programs appear to be assuming that their trainees have received palliative medicine training within their family medicine residency. On the other hand, RCPSC-EM trainees will not have had the same experience. It will be important for the RCPSC-EM program to prioritize time for addressing palliative and end-of-life care curricula to ensure that trainees achieve competencies in this important topic.
Simulation has been explored in nursing as an effective method through which to teach palliative medicine concepts.Reference Gillan, Jeong and van der Riet25 Methods used in Canadian oncology and palliative medicine postgraduate programs include role playing and simulation. When palliative and end-of-life care curricula are introduced to residents, they should match the needs of the current educational evidence and go beyond lecture/seminar formats.Reference Khan, Pattison and Sherwood26 In addition, postgraduate training programs should engage in bedside teaching and small group sessions, because these approaches are known to be preferred educational methods for palliative medicine in EM.Reference Turner14 Only four programs reported any assessment or evaluation of their trainees after palliative and end-of-life care education. In RCPSC-EM programs, this will likely involve direct observation using the end-of-life care EPA, which could occur in a simulation setting. However, in other EM programs, there will need to be a structured assessment and/or evaluation to determine whether competency has been achieved.
In discussing palliative and end-of-life care education for EM residents, it is important to recognize how the field is evolving. Due in part to demographic shifts, healthcare needs of Canadians are changing with seniors having a higher need for palliative care services.Reference Hawley27 Increasingly specialized care may lead patients to present to the ED with novel and unfamiliar medication regimens, or even complications of procedural management such as home paracentesis and thoracentesis catheters.
Another way in which palliative medicine is changing in Canada is with the introduction of medical assistance in dying (MAiD). Patients may present to the ED for symptom management concerns despite ongoing assessment for MAiD and even pending provision. EM learners will need to understand the legal framework around MAiD and their roles and responsibilities within it.
Limitations
We recognize several limitations in our study. Firstly, our survey was completed by program directors. Although program directors have an overall view of the curriculum of their residency program, they may not have the in-depth knowledge of the specific objectives of their program's palliative medicine curriculum. Program directors may also feel pressure to answer questions favorably to reflect well on their residency program, which can lead to a response bias. EPEC-EM is an American EM palliative medicine course that is designed to include residents. However, its applicability in the Canadian context may be a limitation. Our findings may underestimate the true number of hours of training in palliative care because we did not design our survey to capture experiences of residency training in family medicine prior to CCFP(EM) training. However, these experiences are in the context of family medicine, which may be distinctly different from the EM setting when it comes to palliative and end-of-life care. Furthermore, CCFP(EM) certificants virtually always practise full-time EM, further calling into question the relevance of family medicine based palliative and end-of-life care education in the EM context.19, 28
Next steps
Our study provides a starting point for further research and development of consensus among programs regarding which competencies are necessary for the modern EM physician regardless of training stream. Developing consensus should involve RCPSC-EM, CCFP(EM), and palliative medicine experts. Further research should also examine the patient perspective. Five areas have been identified by patients where quality of end-of-life care could be improved: adequate pain and symptom management, avoiding inappropriate prolongation of dying, achieving a sense of control, relieving the burden of death on family, and strengthening relationships with loved ones.Reference Singer, Martin and Kelner29 As suggested by the Improving Palliative Care in Emergency Medicine collaboration, it will be important that individual EM training programs identify a local palliative care championReference Lamba, DeSandre and Todd9 and use existing educational resources, such as the RCPSC-EM EPA for end-of-life care to structure educational curricula. These should include multiple clinical and non-clinical educational modalities, such as simulation and small groups.
CONCLUSION
Palliative and end-of-life care training within EM has been identified as an area of need for the preparation of a competent EM physician. This cross-sectional survey reveals high variability within current palliative and end-of-life care curricula in Canadian EM programs. There are currently developed milestones within the end-of-life care EPA for the RCPSC-EM curriculum. However, a minority of Canadian EM physicians are RCPSC-EM trained, and current curricula address a minority of the milestones within the EPA for providing end-of-life care. As such, it will be important for all EM training programs, RCPSC-EM and CCFP(EM), in Canada, to develop an agreed upon set of competencies and to structure their curricula around this. These curricula should include multimodal educational methods, including bedside teaching, small group sessions, and the development of robust simulation cases specific to patients with palliative needs in the ED.
SUPPLEMENTARY MATERIAL
The supplementary material for this article can be found at https://doi.org/10.1017/cem.2018.470.
Competing interests
CC reports personal fees from Pallium Canada, outside the submitted work.






