CLINICIAN'S CAPSULE
What is known about the topic?
Pain management provided by transport personnel is pivotal, yet most analgesia administration studies have been conducted in land ambulance services
What did this study ask?
What are the pain management practices of critical care paramedics when transferring trauma patients by air transport services in Ontario?
What did this study find?
Analgesia doses had minimal effect on pain ratings, due in part to inadequate dosing and a long time interval between doses
Why does this study matter to clinicians?
Reasons for oligoanalgesia remain unclear, so an opportunity exists to improve the management of acute pain in this patient population.
INTRODUCTION
Trauma systems are created based on the regionalization of care to improve patient outcomes in a cost-effective manner.Reference MacKenzie, Rivara and Jurkovich1,Reference MacKenzie, Weir and Rivara2 As a consequence, medical transport services are necessary for patient transfers to these designated regional trauma centres. Depending upon the proximity of the closest centre, air medical transport services are often required to cover large distances. Consequently, air medical personnel must, therefore, provide care to these trauma patients for a significant period of time.
A pivotal aspect of care provided by air medical personnel relates to pain management, as emphasized by previous position statements, reports, and guidelines.Reference McManus and Sallee3,Reference Turturro4,Reference Alonso-Serra and Wesley5 Pain is frequently undertreated during medical transport.Reference Jennings, Cameron and Bernard6,Reference McEachin, McDermott and Swor7,Reference Albrecht, Taffe and Yersin8,Reference Kosiński, Bryja, Wojtaszowicz and Górka9 Two studies noted that patients are more likely to receive pain relief in the context of chest pain or suspected acute myocardial infarction than after having suffered trauma.Reference Siriwardena, Shaw and Bouliotis10,Reference Bakkelund, Sundland and Moen11 Unfortunately, oligoanalgesia in trauma can have many long-term sequelae including chronic pain.Reference Clay, Watson, Newstead and McClure12,Reference Rivara, Mackenzie and Jurkovich13,Reference McGreevy, Bottros and Raja14 Identification of these types of shortcomings is important for the development and implementation of initiatives and guidelines to facilitate administration of adequate analgesia moving forward.Reference Gausche-Hill, Brown and Oliver15,Reference Brown, Hirshon and Alcorta16
The majority of studies involving an examination of the adequacy of analgesia administered have been conducted in land ambulance services. There is a gap in the literature with regards to evaluating pain management following trauma in the setting of air medical transport services, particularly those transported exclusively by paramedics.Reference Albrecht, Taffe and Yersin8,Reference Thomas, Rago, Harrison, Biddinger and Wedel17 Whether there is any difference from an analgesia perspective in patients transported by land or air or whether land and air medical personnel would act any differently during patient transportation is difficult to ascertain and has not yet been rigorously studied. Possible factors affecting analgesia in patients transported by air compared with those by land could be a longer transport duration and greater severity of the injury, as denoted by a higher injury severity score.Reference Buchanan, Coates and Sne18
The primary objective of this study was to evaluate the pain management practices of Ornge (Ontario's provincial air and land critical care transport service) during the transportation of trauma patients by air. Our aim was not to test any specific hypotheses or analyze for associative factors, but rather to describe current practices to guide future research projects on improving the adequacy of analgesia administration.
METHODS
Study design and time period
We conducted a 12-month health record review of Ornge electronic paramedic records. We screened cases from January 1, 2015, to December 31, 2015.
Study setting
Ontario is a large Canadian province (approximately 1.1 million km2 or 424,600 milesReference MacKenzie, Weir and Rivara2) with a mix of urban, suburban, rural, and remote areas. The health care system is publicly funded and serves a population of approximately 13.5 million people. Ornge Transport Medicine is the publicly funded air medical transport system providing all air medical patient transfers in Ontario. Ornge is Canada's single largest air medical transport provider, carrying out approximately 19,000 patient transports annually.
Ornge operates its own dedicated communication and dispatch centre and utilizes a dedicated medical decision algorithm to determine patient acuity and call priority. The centre also has a medical control physician, dedicated to providing full-time medical control without any other competing clinical duties. Medical control physicians are board certified in emergency medicine and have an extensive prehospital care or transport medicine background. Physicians also provide indirect medical control, providing medical oversight to the service's quality care, investigation, pharmacy and therapeutics, and education committees.
Ornge aircraft operate as either advanced or basic life support aircraft, with flight paramedics as the sole providers during transport. The scope of practice for the highest crew designation, critical care, is consistent with the National Occupational Competency Profile and includes management of patients who require intubation, mechanical ventilation, use of inotropes or vasopressors, administration of fibrinolytic agents, and maintenance of intra-aortic balloon-pump therapy without additional medical personnel. Flight paramedics provide care using standing orders and medical directives developed by the Ornge Medical Advisory Committee and contact medical control physicians when the care exceeds these orders or directives.
Population
The Ornge patient care record system was queried to identify potentially eligible patients. Patients were included if they were ≥18 years old, sustained multisystem traumatic injuries, and were undergoing air transport to a designated trauma centre by Ornge either directly from the scene or a primary receiving (non-trauma) hospital. Patients were excluded if they were <18 years old, had a Glasgow Coma Scale (GCS) score <14, required intubation, or were accompanied by a hospital-based staff (such as a nurse or physician).
The study was approved by the Research Ethics Board of Sunnybrook Research Institute and the Ottawa Health Science Network Research Ethics Board.
Data collection
Information was abstracted from the electronic patient care records of included patients in a standardized, piloted data collection form by a single trained data extractor. To confirm the accuracy of the data collection, a second reviewer abstracted data randomly from 10% of the selected records. Any differences were to be discussed to resolve data abstraction issues. All data abstracted using data collection forms were subsequently entered into a spreadsheet (Microsoft Excel; Microsoft Corporation, Redmond, WA, USA) to facilitate suitable data analyses.
Outcome measures
Patient demographic information collected included: age, sex, weight, medical comorbidities, medications, allergies, GCS score, and initial vital signs (heart rate, respiratory rate, blood pressure, and oxygen saturation).
Information collected regarding injury and transportation details included: type of trauma (blunt versus penetrating), mechanism of injury, injury location, pre-transportation analgesia, sending location, transfer duration, and general care received during transport (e.g., intravenous insertion, immobilization, etc.).
Outcomes measures that were selected included: medication administration (analgesia administered or not; time to first analgesia from departure of scene or receiving hospital; type of analgesia; analgesia dose and route; frequency of analgesia re-administration); pain management (comparison of initial and repeat pain assessments using a 11-point numerical rating scale related to administration of analgesia medication); and adverse events (rates of adverse events related to the total administration of analgesia medication).
Data analysis
We used descriptive statistics to report results as mean ± standard deviation, range, and percentage. Pain management, analyzed according to absolute differences in numerical rating scale pain assessments following administration of analgesia medication, was reported as the mean numerical rating scale differences between doses and also the number of patients experiencing numerical rating scale differences equal to zero (i.e., no change in numerical rating scale pain assessment from baseline to first dose of analgesia; from first dose to second dose; from second dose to third dose etc.).
Sample size
The sample size for this health record review was dictated by the number of patients eligible for inclusion over an entire consecutive calendar year. Use of a consecutive calendar year removed the potential for biases in seasonal variations present based on time of year.
RESULTS
During the one-year study period, 600 potential patients were identified, with a total of 372 patients meeting the eligibility criteria (Figure 1). No issues were identified between the two reviewers (i.e., 100% agreement) in relation to data abstraction. Patient characteristics for the included cases are presented in Table 1. Patients were 46.9 (range 19–92) years old, 262 (70.4%) were male, mean weight was 85.8 kg (range 40–242) kg, 11 (5.7%) had chronic pain, and 134 (36.0%) were taking any medications.

Figure 1. Study patient flow.
Table 1. Patient characteristics (N = 372)
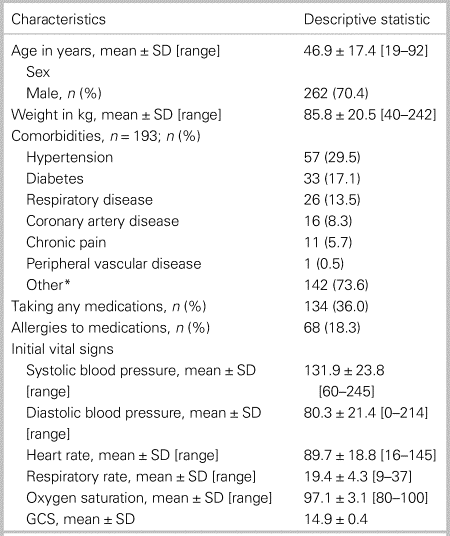
GCS = Glasgow Coma Scale; SD = standard deviation.
*“Other” represents a multitude of otherwise infrequent separate medical conditions.
Table 2 summarizes injury, patient care, and transportation details. There were 361 (97.0%) patients who sustained a blunt injury, and 11 (3.0%) sustained a penetrating injury. Motor vehicle collision was the most common mechanism of injury (34.1%), with extremities being the most affected injury location (68.3%), followed by the head (43.5%). Duration of transport was 82.4 ± 46.3 minutes. Approximately two-thirds of all patients underwent spinal immobilization (66.4%) or received intravenous fluids (62.6%) during transportation.
Table 2. Injury and transportation details
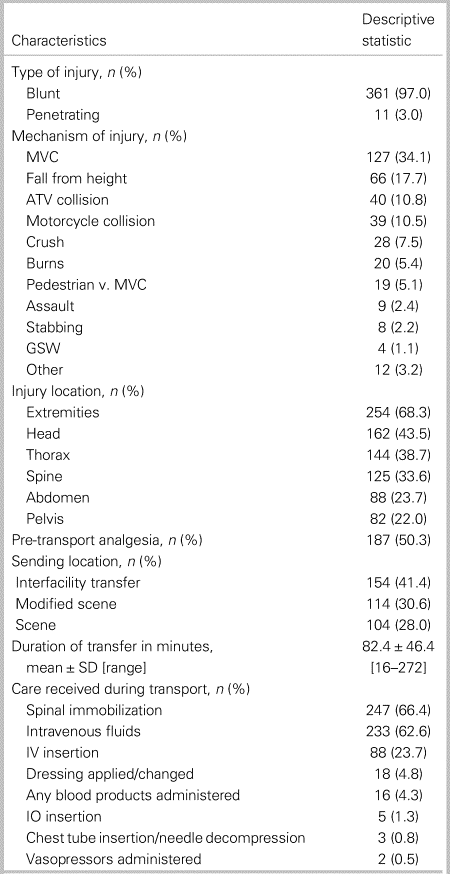
ATV = all-terrain vehicle; GSW = gun shot wound; IO = intraosseous; IV = intravenous; MVC = motor vehicle collision; SD = standard deviation.
*“Other” represents a multitude of otherwise infrequent separate mechanisms of injury.
The pain was initially assessed in 335 (90%) patients (Table 3). Overall, the numerical rating scale at baseline was 4.9 ± 2.8. For the 232 (62.4%) patients who received analgesia, the numerical rating scale at baseline was 5.9 ± 2.5, compared with 3.1 ± 2.5 in patients who did not receive analgesia. Fentanyl was the most commonly administered first dose of analgesia in 181 (78.5%) patients, with a mean dose of 44.3 (range 25–60) mcg. The numerical rating scale assessed in 81% of patients after the first dose of analgesia decreased by 1.1 ± 1.6 points (range −2 to 7). There were 44 (23.4%) patients who had no change in numerical rating scale from baseline after the first dose of analgesia.
Table 3. Pain and analgesia data for the first dose

IO = intraosseous; IV = intravenous; mcg = micrograms; mg = milligrams; NRS = numerical rating scale for pain assessment; SD = standard deviation.
A total of 171 (73.7%) patients received further analgesia, equal to 2.4 ± 2.0 (range 1–18) additional doses (Table 4). Fentanyl was again the most commonly administered analgesic across the second to nineteenth doses. Subsequent doses of analgesia resulted in no change in the numerical rating scale in over 65% of patients (range 65.4–71.3).
Table 4. Pain and analgesia data for the second, third, and fourth to nineteenth doses
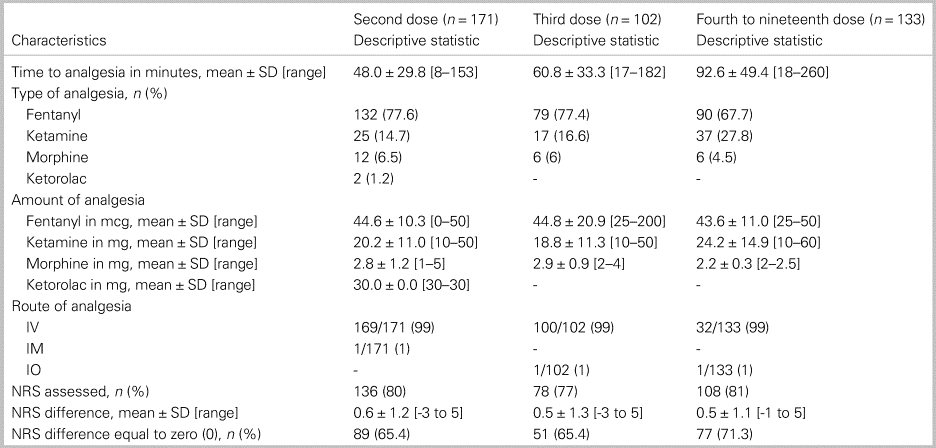
IO = intraosseous; IM = intramuscular; IV = intravenous; mcg: micrograms; mg: milligrams; NRS = numerical rating scale for pain assessment; SD = standard deviation.
Table 5 outlines the adverse events recorded. Thirty-two patients experienced a total of 43 adverse events after a total of 638 doses of analgesia. Nausea occurred most often (39.5%), and oxygen desaturation was the most common physiologic derangement (28.0%). Nearly one-half of all the adverse events recorded (48.8%) occurred after the first dose of analgesia.
Table 5. Adverse events following analgesia

AE = adverse event; BP = blood pressure; RR = respiratory rate.
DISCUSSION
Interpretation of findings
In this health record review, we evaluated the pain management practices of flight paramedics during transport of trauma patients by air. We found that the majority of patients were assessed for pain at baseline and, then, again after the first dose of analgesia. Pain at baseline was moderate on average. Although the first dose of analgesia had minimal effect on pain, it needs to be recognized that the average dose of fentanyl given was far less than the generally recommended 1–2 mcg/kg. Subsequent doses of analgesia appeared to have even less of an impact. Furthermore, with almost one-quarter of patients experiencing no pain relief after the first dose of analgesia, it reinforces that the dosing was inadequate. The prolonged time interval (up to 153 minutes) between the first and second dose of analgesia explains why some patients perceived worse pain after the first dose, in that they initially obtained some relief but were, then, allowed to re-experience pain as the initial dose wore off, and the analgesia was not titrated accordingly.
Postulating, more specifically, as to why this patient population received oligoanalgesia is challenging given the constraints of our study (e.g., retrospective review and qualitative analysis). Potential factors involved could be paramedic hesitation with medication side effects in treating unstable, critically ill patients; requirements of online medical direction for opioid administration and other analgesia; and a lack of weight-based dosing. Regardless, based on our results, it is our contention that there is an opportunity to improve the management of acute pain in this patient population.
Comparison to previous studies
Management of pain is a topic of continued interest because of the need for the provision of effective analgesia in prehospital settings.Reference Parker and Rodgers19 In a study of 1,156 patients with isolated limb injury rescued by air in Switzerland, Eidenbenz et al. found a similar percentage of patients received analgesia as in our study, although their cohort's baseline pain scores were higher.Reference Eidenbenz, Taffé, Hugli, Albrecht and Pasquier20 They also found fentanyl was their most commonly administered analgesic. In contrast, of 381 patients evacuated by US critical care air transport teams, fentanyl was only the third most popular analgesic behind morphine and hydromorphone.Reference Mora, Ganem, Ervin, Maddry and Bebarta21 In our study, morphine and ketamine were distant second and third choices behind fentanyl, and hydromorphone was used in less than 1% of patients.
Dijkstra et al. conducted a systematic review of pain management in trauma patients and showed that paracetamol and intravenous (IV) opioids (morphine and fentanyl) were effective, but non-steroidal anti-inflammatory drugs (NSAIDS) had mixed results.Reference Dijkstra, Berben, van Dongen and Schoonhoven22 They stressed that future studies should examine analgesic effectiveness and drug safety in prehospital emergency care. Our study addresses their suggestion, wherein we highlight that air medical crew members commonly administer morphine and fentanyl with minimal resultant drug-related adverse events. Smith et al. had similar results in 103 US trauma patients, showing no significant difference in analgesic effectiveness or incidence of adverse effects between morphine and fentanyl.Reference Smith, Wang and Cudnik23 However, a study involving intensive care helicopter paramedics in Australia established that a clinically significant pain reduction of ≥2 points was achieved by 87.0% of adult trauma patients while using ketamine in 18.5% of cases.Reference Andrew, de Wit and Meadley24 In contrast, our study showed that 23.4% of patients had no difference in numerical rating scale after the first analgesia dose. What these results seem to show is that a lack of evidence-based protocols or guidelinesReference Dijkstra, Berben, van Dongen and Schoonhoven22 can result in varying degrees of success in terms of pain management.
Strengths and limitations
Our study has several strengths compared with the existing literature in this field. We abstracted a greater number of variables that allowed us to ascertain trends regarding effectiveness. More importantly, we examined real-time concurrent assessments of pain and pain management during en route care in a generalizable population of trauma patients, as opposed to the only other previous study in 12 flights of 114 less severely ill and injured US military patients.Reference Bridges, Dukes and Serres25 We also followed a thorough health record review process that included a double-check on 10% of cases showing 100% correctness of data abstraction from the electronic paramedic records.
Our study was a health record review, making it impossible to control exposure or outcome assessment. We did not attempt to calculate any associations between not receiving a second dose and adverse events, comorbidities or vital signs, or type or site of injury. We were reliant on the accuracy of record-keeping in the Ornge electronic paramedic records. It was not possible to delineate whether the fact that 50.3% of patients received pre-transport analgesia impacted the analgesia delivered en route by the flight paramedics. We were also unable to procure accurate details on the pre-transport analgesic administration (e.g., type of medication and dosing). We may have encountered selection bias, given patients were excluded with a GCS score <14; however, this was deemed necessary from a patient perspective to obtain accurate and reliable numerical rating scale pain assessments. We were not able to rule out under-reporting of adverse events to account for the low number of adverse events observed following the total number of analgesia doses. Furthermore, it is unfeasible for us to be sure that the analgesia dose resulted in the adverse event; these are multisystem trauma patients, and it is difficult to resolve analgesic dose versus injury or blood loss as the reason for the adverse event. Finally, we were likely underpowered to contemplate formally testing statistical differences between various sub-groups and, therefore, were limited to descriptive statistics.
CONCLUSION
In the majority of patients, initial and subsequent dose(s) of analgesic dose had a minimal effect on pain as assessed using the numerical rating scale, due in part to inadequate dosing and a long time interval between doses. Future research is required to determine the reasons for oligoanalgesia and methods to improve the management of pain in this patient population.
Competing interests
None.










